ICU Management & Practice, Volume 16 - Issue 2, 2016
The transport of critically ill patients for diagnostic or therapeutic procedures carries a particular risk and requires therefore a careful risk-benefit assessment. Transport-related risks can be reduced by increased awareness and education, adequate staffing, proper choice and handling of equipment and the use of error-preventive tools like checklists.
Intensive Care Units (ICUs) have been developed to provide a safe environment staffed with highly educated and competent physicians and nurses using the most advanced medical technology and therapies for the critically ill patients. Even if this ideal of an ICU were perfectly realised it would be necessary for many if not most ICU patients to temporarily leave this paradigmatic world. The reason is simply the common need to perform a diagnostic or therapeutic procedure outside the ICU or the need to transfer a patient to another hospital with higher-level or more specialised critical care, or other medical service (e.g. heart surgery). These transports expose critically ill patients to an increased risk for errors and adverse events. ICU teams must aim to reduce this risk and related consequences as much as possible, or in other words to increase patient safety in this particular vulnerable situation.
What is a Safe Transport?
In an abstract perspective a safe transport would be defined by the absence of error with the potential for patient harm and ultimately by the absence of adverse events. In a more pragmatic approach a safe transport could be described by several aims like “patient arrives at least in the same condition as at departure”, “no transport-related physiological deterioriation”, “absence of critical events”, “no equipment failure” and so on. Indeed, the opportunities for transport-related errors and events are numerous. To illustrate a few, a pathophysiological deterioriation might arise from the displacement of lines or drains, the loss of airway in a ventilated patient, a less sophisticated monitoring or treatment during transport (e.g. a more simple mode of ventilation), additional movements (e.g. lifting of a patient) or exposure to altered environmental conditions (temperature, altitude, acceleration), as well as limited diagnostic and therapeutic resources during transport frequently characterised by the lack of senior staff.
Risk Assessment and Safety Status of Transports
Although the number of publications in this field is increasing it remains difficult to come up with representative numbers. The reasons for this difficulty consist of different definitions of error, different types of transport (e.g. intrahospital and interhospital), and very frequently the missing information about the number of opportunities for error and the actual error (numerator and denominator). In a study on 184 mechanically ventilated ICU patients requiring 262 transports for CT, 26% of transports were associated with an adverse event affecting the patient (Parmentier-Decrucq et al. 2013). Interhospital transports carry a particular risk regarding the safe functioning of transport equipment. In a Dutch study involving 353 interhospital transports, 55 technical problems were encountered, ranging from problems with the gas supply and electricity to problems with the medical equipment and the trolleys, as well as with some functions of the ambulance car. Although there was only little impact on patient status, these problems led to delays or even cancellation of patient transports. In any case this study highlights the particular dependence on technical equipment during a period when the relatively safe environment of a hospital is left with a critically ill patient on board (Droogh et al. 2012).
Patient safety is not only a matter for the transport period; a transport might impact the patient status beyond arrival on or return to the ICU. In a French study it was shown that intrahospital transport increases the risk for complications in ventilated critically ill patients. Patients exposed to a transport had a higher risk for various complications including pneumothorax, atelectasis, ventilator-associated pneumonia, hypoglycaemia, hyperglycaemia, and hypernatraemia (Schwebel et al. 2013). The latter findings illustrate that the interruption of critical care processes like the continuous administration of medication might lead to pathophysiological derangements if no proper and time-sensitive adaption is performed.
An important question concerns the composition of the transport team. While it seems intuitively most likely that a dedicated transport team should be advantageous there are few data supporting this assumption. In a Scottish study on interhospital transfers of acutely ill patients the incidence of unsecured medical equipment and equipment failures in ventilated patients was significantly lower in dedicated transport teams (Fried et al. 2010). Obviously ventilated patients are to be considered as a group with increased risk during any kind of transport and a clear demand for skilled accompanying medical staff. To illustrate this point an example of a patient with decreasing oxygen saturation might be helpful. The causes for a decreasing oxygen saturation might be trivial like the loss of the signal due to the displacement of the oxygen sensor, but could also be attributed to a life-threatening event like airway obstruction or pneumothorax, as well as technical problems like the breakdown of gas supply or defect hoses and valves, just to mention a few. It goes without saying that the fast and accurate workup and solution of this event will be much more challenging with a patient on the move, either on the street or in the air.
How to Minimise Transport-Associated Risks for Patients?
Assessment of the Patient & Decision for Transport
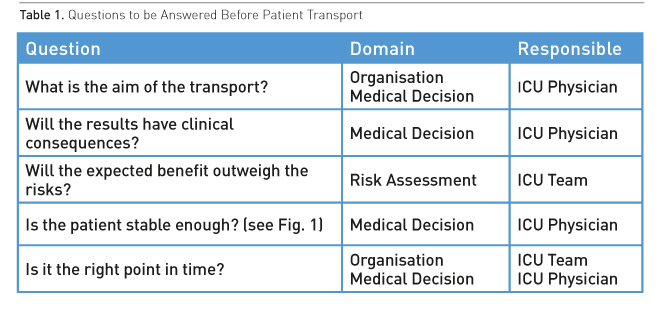
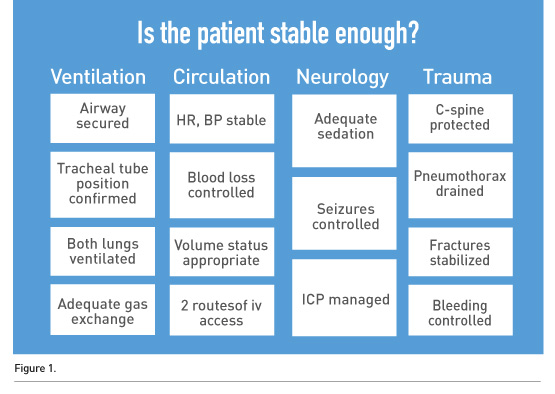
Considering the risks associated with the transport of critically ill patients the first principle must be “avoid any unnecessary transport” and ask the question “will this transport likely result in findings or procedures that will ultimately benefit this patient?”. Table 1 summarises the questions to be answered before any transport. Most importantly a careful assessment of the patient status must be performed before a final decision is reached to transport the patient (Fig. 1).
Setting & Equipment
As elaborated above the choice, maintenance and proper handling of equipment is a crucial factor in preventing critical events during transport. One of the paradigms in safety research is about system design and the risk of an environment and equipment that might rather promote than prevent the occurrence of error. It is therefore of uppermost importance to choose transport equipment that is built with a user-friendly and error-mitigating design. The user-machine interface makes a difference, as has been shown in a study on different types of transport ventilators (Templier et al. 2007). For intrahospital transports the ICU equipment already in use in a particular patient should be used as much as possible for the transport as well. There are many ICU ventilators available that will be applicable during transport, for example. Alternatively some transport ventilators will provide the exact similar ventilator mode as used with a particular ICU ventilator.
The placement of equipment during a transport should allow unhindered access to the patient, while at the same time patient safety must not be compromised by an insecurely stowed monitor, ventilator, perfusion pump etc. In most cases equipment is best mounted at or below the level of the patient, but the display of the monitor, ventilator and other devices must be visible and alarms should be as audible as possible.
At least for gas supply and power supply redundancy must be a principle. Calculations must consider unplanned delays during a transport and other scenarios like a higher demand for oxygen in a deteriorating patient.
Staffing
If we agree with the principle that the safety profile of a transport of a critically ill patient should resemble the conditions of an ICU as closely as possible then an intensive care physician or an emergency physician and at least one intensive care trained nurse are required for this transport. Depending on the character of the transport and the number of medical staff additional personnel like porters might be necessary.
Route & Means of Transport
The choice of route and the means of transports depend on several criteria like geographic circumstances and weather conditions (interhospital) or local structures (intrahospital). But first of all the patient’s status of urgency and stability is the determining factor. Of note, the fastest route and means of transport will not always provide the best risk to benefit ratio for a patient.
Handover
Information transfer and the loss of significant information during medical processes are a major challenge in healthcare. This is particularly true for critically ill patients undergoing interhospital transports. A comprehensive medical report from the transferring ICU and a report from the transport team are essential tools to ensure continuity of care and avoid loss of relevant clinical information.
Checklists
Many of the issues elaborated above can be in part addressed by the use of checklists. The assessment of a patient before transport and the review of transport equipment are good examples. It has been shown that the use of checklists is associated with a reduction of incidents during the transport of critically ill patients (Bérubé et al. 2013). Other authors have published very useful checklists for the preparation and realisation of transports that can be considered as part of a programme to enhance patient safety (Fanara et al. 2010; Brunsveld-Reinders et al. 2015).
Conflict of Interest
Andreas Valentin confirms that he has no affiliations or involvement in any organisation or entity with any financial interest in the subject matter or materials discussed in this manuscript.
References:
Bérubé M, Bernard F, Marion H et al. (2013) Impact of a preventive programme on the occurrence of incidents during the transport of critically ill patients. Intensive Crit Care Nurs, 29(1): 9-19. PubMed ↗
Brunsveld-Reinders AH, Arbous MS, Kuiper SG et al. (2015) A comprehensive method to develop a checklist to increase safety of intra-hospital transport of critically ill patients. Crit Care, 19: 214. PubMed ↗
Droogh JM, Smit M, Hut J et al. (2012) Inter-hospital transport of critically ill patients; expect surprises. Crit Care, 16(1): R26. PubMed ↗
Fanara B, Manzon C, Barbot O. et al. (2010) Recommendations for the intra-hospital transport of critically ill patients. Crit Care, 14(3): R87. PubMed ↗
Fried MJ, Bruce J, Colquhoun R et al. (2010) Inter-hospital transfers of acutely ill adults in Scotland. Anaesthesia, 65(2): 136-44. PubMed ↗
Parmentier-Decrucq E, Poissy J, Favory R et al. (2013) Adverse events during intrahospital transport of critically ill patients: incidence and risk factors. Ann Intensive Care, 3(1): 10. PubMed ↗
Schwebel C, Clec'h C, Magne S et al. (2013) Safety of intrahospital transport in ventilated critically ill patients: a multicenter cohort study*. Crit Care Med, 41(8): 1919-28. PubMed ↗
Templier F, Miroux P, Dolveck F et al. (2007) Evaluation of the ventilator-user interface of 2 new advanced compact transport ventilators. Respir Care, 52(12): 1701-9.
PubMed ↗







