ICU Management & Practice, Volume 19 - Issue 2, 2019
Quality improvement provides tools that help the transformation of an intensive care unit into a highly reliable and safe environment, that nurtures continuous learning and delivery of high-quality care that improves patient experience and outcomes.
Despite advances in healthcare and dramatic improvements in survival across the spectrum of disease states, there exists a chasm between ideal care and actual healthcare delivery globally (NASEM 2018). In the U.S., consistent high-quality health care remains elusive in the increasingly complex and subspecialised healthcare system (IOM 2001). Quality improvement (QI) has emerged as a strategy to address the defects in the healthcare system, to achieve the best care that improves patient experience and outcomes. We will discuss some of the concepts of the QI process, with particular emphasis on the paediatric intensive care unit (PICU) environment.
Definition
High-quality care is consistent with evidence base and professional knowledge, and it is characterised by an increased likelihood of achieving desired outcomes (IOM 2001). The IOM report outlined six dimensions of quality in healthcare: i) safety (avoiding patient harm), ii) effectiveness (avoiding overuse and underuse), iii) patient-centredness (focused on patient needs), iv) timeliness (avoiding harmful delays), v) efficiency (avoiding waste, affordability to system), and vi) equity (IOM 2001; NASEM 2008). Avedis Donabedian described a model with three main areas for assessment of quality; structure, process, and outcome – the SPO framework – this model guides the practical application of QI concepts. The patient perspective is central to this framework, and QI efforts must be focused on the patient experience and outcomes during illness.
You might also like:Data-driven management for intensive care units
Challenges to quality improvement in the PICU
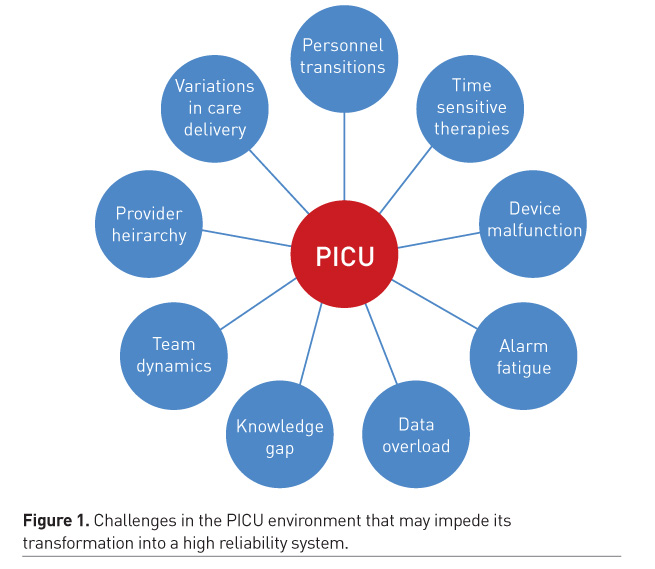
The PICU environment is characterised by complexity of care, therapeutic choices, time sensitivity for interventions, constantly changing workflow, competing priorities and a complicated interaction between the provider, patient and the healthcare environment (Figure 1). Large amounts of visual real-time data that need to be interpreted in the context of changing patient status and the interface with devices, create opportunities for unpredictable errors and harm. Healthcare-associated infections, medication errors, device-related safety issues, and failure to provide timely therapies are some of the events seen in this environment. Human behavioural factors, such as knowledge gap, fixation, alarm fatigue and failure to effectively communicate and collaborate are often deemed as causal factors for errors. In addition, lack of engagement from the frontline providers, disruption of autonomy and competing priorities in the unit result in a perception of QI efforts as a burden, time constraint and top-down mandates that are not deemed worthwhile. Lack of leadership buy-in can be a major factor in the failure to sustain QI efforts in the PICU. The PICU environment (structure, devices, workflow) and its interaction with providers is a critical factor in preventable harm, with faulty systems design often the root cause. A highly reliable ICU must incorporate a thoughtful and intelligent design and structure that facilitates the delivery of high-quality care.
High-reliability organisations/systems
In order to successfully mobilise change and ensure high-quality care delivery, the PICU must embrace the culture of high reliability (Hines AHRQ 2008). Highly reliable organisations (HRO) are characterised by extended periods without catastrophic accidents or serious failures, despite operating in a highly complex and hazardous domain. A highly reliable PICU nurtures a culture of continuous quality improvement, has strong, engaged and motivating leaders who cultivate resilience in the system by prioritising safety over other performance demands. The five characteristics of an HRO are: i) preoccupation with failure; ii) reluctance to simplify explanations for operations, successes, and failures; iii) sensitivity to operations (situational awareness); iv) deference to frontline expertise, and v) commitment to resilience.
Smart PICU design
Preferably conceived at its inception, a strategic PICU design creates an environment (workspace and workflow) that is suitable for safe and effective care provision by committed providers, while also optimising patient and provider experiences. Patient rooms are designed to promote infection control procedures, early mobility, and patient comfort. A smart ICU room may also monitor and track changes in light, noise and other environmental hazards. Intelligent summarisation of data, smart alarm management, and patient privacy are other key aspects of the ICU design (Halpern 2014).
Optimising PICU workflow
Thoughtfully developed and standardised key processes such as patient rounds, handoffs during admission, transfers and discharges, medication reconciliation and safety huddles have become an integral part of daily workflow in the PICU. The use of a checklist or a more robust decision support tool that integrates patient data in real time facilitates some of these processes during rounds in many PICUs. Protected space for undisturbed performance of high-risk tasks, such as medication check, structured assessment tools for sedation and pain, tracking the evolution of illness severity using early warning scores are examples of nursing QI and safety processes aimed at improving patient safety in the PICU. In a highly reliable PICU, providers continue to explore the environment for potential disasters, are willing to speak up for safety, and strive for prevention or early detection and mitigation of harm.
Culture of continuous QI and Learning healthcare systems
A highly reliable PICU invests in data gathering. Patient level data are analysed in the context of existing knowledge base to develop best practices using the concepts of implementation science, an important tool that completes the cycle of a Learning healthcare system, depicted in Figure 2. The commitment to learn from every event or data stream is at the core of this cycle. The lessons learnt from this interpretation and past experience, are immediately made available for clinical decision support (Friedman 2014).

A just culture is critical to promoting a learning environment in which the providers report hazards, errors, and defects in care, without fear of blame or punishment. At our institution, providers are encouraged to check each other, be attentive to details and look for latent defects, speak up if concerned for safety, communicate clearly, escalate concerns along the chain of command if necessary, and maintain a questioning attitude. Such a culture breaks barriers such as hierarchy, interdisciplinary team dynamics, and fear of blame in the PICU. A just culture does not absolve individuals of any accountability but ensures that individuals are not blamed for systemic flaws that make it more likely for highly trained and dedicated providers to fail.
ICU informatics and quality improvement
Figure 3 illustrates a smart ICU model, where patient level data at the bedside are integrated and intelligently displayed, transforming them into actionable data for decision support. Modern informatics concepts must aim to utilise patient level data to ensure high quality care, continuous learning and quality improvement to impact patient outcomes. Such continuous bedside data allow learning from invaluable dynamic trends during illness course in the ICU, in context to therapies being applied. Automatic aggregation of data from a large number of patients, from multiple sites and via a variety of data sources has allowed the creation of large ICU databases such as the Multiparameter Intelligent Monitoring in Intensive Care II (MIMIC-II) research database (Saeed 2011). Examples of group learning using automatic or manually submitted data in small or large registries in the PICU population include the Virtual PICU systems (VPS), Pediatric Research Database (PRD Pivot) with rich de-identified data elements from the electronic health record, Pediatric Heart Network (PHN) collaborative learning model, Pediatric Cardiac Critical Care Consortium (PC4) clinical registry for infants and children in North American cardiac ICUs, Pediatric International Nutrition Study (PINS, I, II & III) database of nutritional intake and outcomes in mechanically ventilated children, Collaborative Pediatric Critical Care Research Network (CPCCRN) and Pediatric Emergency Care Applied Research Network (PECARN) databases, Society of Thoracic Surgeons Congenital Heart Surgery Database (STS-CHSD), Extracorporeal Life Support Organization (ELSO), Australia New Zealand Pediatric Intensive Care (ANZPIC) registry and the PICU International Collaborative Learning through Outcomes Data sharing (PICU-CLOUD) network.
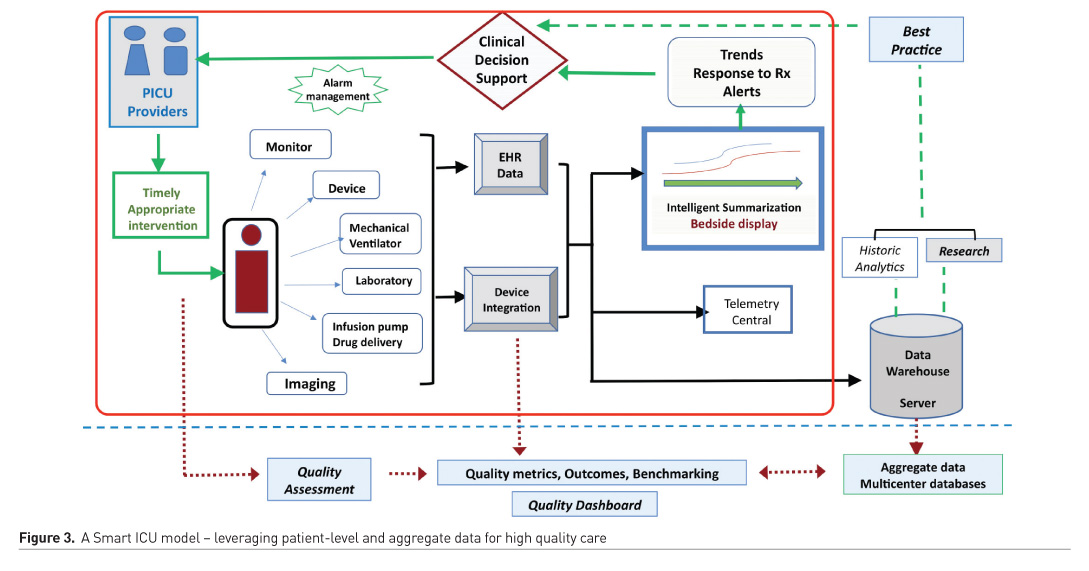
Large patient-level datasets that can be leveraged for hypothesis generation, comparative effectiveness research, tracking, trending and benchmarking of ICU quality metrics, and a novel approach of collaborative learning. Attention to the accuracy, quality, and rigorous analyses of these data must be ensured, and data privacy, security, management, and governance are important considerations when sharing data across institutions on these digital platforms. Optimisation of electronic note writing, data input by nurses, alarm management to prevent fatigue, efficient storage, and analyses of data for research, intelligent data summarisation to provide decision support, are some of the benefits of healthcare IT advances. In order to benefit from these platforms, their development must take into account the unintended data overload, documentation burden, human behaviour expertise, and user interface in the PICU.
Collaborative learning
Best practices at the institutional level can be rapidly disseminated for wider adoption leading to improved patient outcomes. This concept is the central theme of collaborative learning, in which participating centres in a network share data and benchmark performances along key metrics. Potential target areas are explored for best practices using a collaborative multistep approach that involves site visits. Best practices are translated into clinical practice guidelines that are systematically applied across the network to examine their impact on clinical outcomes (Wolf 2016). The Pediatric Heart Network used a stepwise collaborative model that included data sharing, site visits to identify best practice, developing standards by consensus, and implementation of practice change across the network. They successfully decreased the time to extubation after paediatric cardiac surgery (Mahle 2016). Other examples of successful networks that leverage data for collaborative learning include the Children’s Oncology Group, Cystic Fibrosis Foundation, and the Vermont-Oxford Collaborative.
QI Toolkit
A variety of tools have been developed to undertake systematic QI studies. Paediatric intensivists must become familiar with the methodologies and interpretation of the essential QI tools such as the i) Cause and effect (fishbone) diagram – to determine root causes of the event, ii) Failure Modes and Effects Analysis – to identify potential risks and their impact, iii) Flowcharts, Pareto charts, Run Charts and Control Charts – help visualisation of variation in performance over time, iv) Plan-Do-Study-Act rapid-cycle testing sheet to assess the impact of short iterative interventions. Details of these and other such tools are well described in the Institute for Healthcare Improvement (IHI) website (ihi.org/resources/Pages/Tools/Quality-Improvement-Essentials-Toolkit.aspx).
Quality metrics
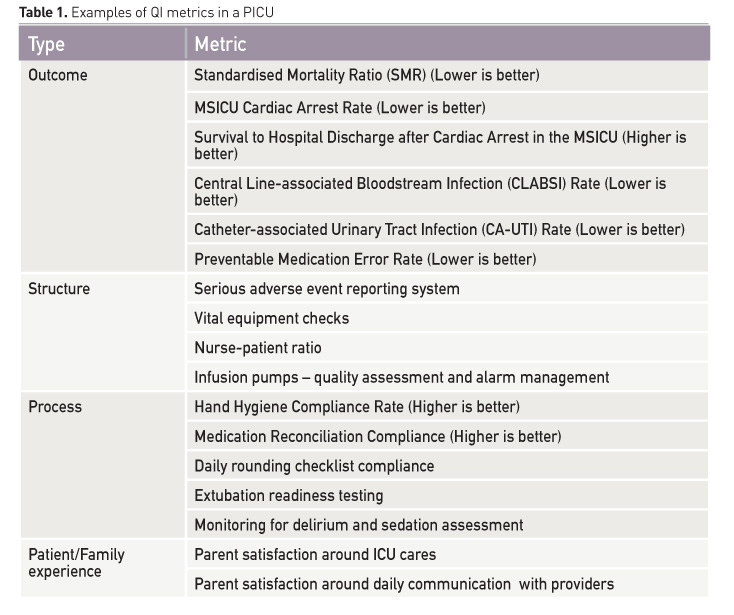
Measurement is an important component of the healthcare transformation journey. Quality metrics are indicators that help measure PICU performance along agreed areas of importance to patient outcomes. These metrics allow serial examination of the unit performance over time, in the context of interventions, and are compared to internal goals or external (other PICU or group) benchmarks. QI metrics can be process variables, outcome metrics or structural indicators. Characteristics of an ideal QI metric include a clear definition, measurable, show a degree of variability across sites such that good and poor performers can be differentiated, preferably an outcome measure or have a plausible link to the outcome of interest, not sensitive to severity of illness and reflect provider or unit performance. Table 1 shows some examples of QI metrics in a PICU
Safety culture in the ICU
The Michigan Keystone Project is a landmark effort that demonstrated the benefits of a collaborative QI approach to improve ICU outcomes. Over a 10-year period, sustained reductions in the rate of central line-associated bloodstream infections (CLABSI) were observed in over 100 ICUs across Michigan (Pronovost 2016). In addition to incorporating simplified best practices proven to reduce CLABSI, the investigators launched a systematic QI framework for preventing harm in the unit, embraced a strong safety culture, including checklists for safe central line insertion bundles, workflow re-design and empowering of providers to speak up for compliance to best practices. PICU leaders must encourage reporting of near misses and latent defect in the system without fear of reprisal. Near misses must be viewed as opportunities to learn about systems issues and potential improvements, rather than as evidence of safety. Vigilance for and anticipation of potential failures is a hallmark of a high reliability organisation.
Conclusions
Quality improvement in the ICU includes a spectrum of efforts aimed at improving individual patient experience and outcomes, leveraging smart technology and informatics to provide bedside decision support to deliver high-quality care, and the use of specialised tools to examine the impact of QI interventions on process and outcomes. PICU leaders must strive to transform their unit into a high reliability system by embracing a culture of safety, promoting continuous improvement, and investing in engineering a safer environemnt for patients and providers. A strategic quality management plan with broad stakeholder buy-in allows QI efforts in the PICU to be focused. Measurement, benchmarking and dissemination of performance metrics are essential to maintain provider engagement and sustain the improvements in processes and patient outcomes.
Key points
- Paediatric intensive care unit is a highly complex environment with likelihood of for unintended patient harm.
- Quality improvement strategies aimed at improving patient outcomes must be firmly embedded in the PICU culture.
- PICU leaders must embrace the culture of high reliability and continuous quality improvement where every event or data point is considered an opportunity for learning. Providers in such units are preoccupied with failure, looking for defects in the system to prevent or mitigate harm
- Smart PICU designs allow providers to work in a safe and efficient environment, minimising harmful events and optimising patient comfort and experience
- Data management and intelligent summarisation facilitate bedside decision support in such units.
- Quality improvement tools allow gathering and intepretation of data, highlight opportunities for improvement, and facilitate collaborative learning that promotes high quality and value care in the ICU.
Conflicts of interest
None
References:
Friedman C (2014) Toward Complete and Sustainable Learning Systems. Available from medicine.umich.edu/sites/default/files/2014_12_08-Friedman-IOM%20LHS.pdf.
Halpern NA (2014) Innovative designs for the smart ICU. Chest, 145(3):646-658
Hines S, Luna, K, Lofthus J, et al. (2008) Becoming a High Reliability Organization: Operational Advice for Hospital Leaders. (Prepared by the Lewin Group under Contract No. 290-04-0011.) AHRQ Publication No. 08-0022. Rockville, MD: Agency for Healthcare Research and Quality.
Institute of Medicine (2001) Crossing the Quality Chasm: A New Health System for the 21st Century. Washington, DC: The National Academies Press.
Mahle WT, Nicolson SC, Hollenbeck-Pringle D, Gaies MG, Witte MK, Lee EK, Goldsworthy M, Stark PC, Burns KM, Scheurer MA, Cooper DS, Thiagarajan R, Sivarajan VB, Colan SD, Schamberger MS, Shekerdemian LS (2016) Pediatric Heart Network Investigators. Utilizing a Collaborative Learning Model to Promote Early Extubation Following Infant Heart Surgery. Pediatr Crit Care Med, 17(10):939-947.
National Academies of Sciences, Engineering, and Medicine (2018) Crossing the global quality chasm: Improving health care worldwide. Washington, DC: The National Academies Press.
Pronovost PJ, Watson SR, Goeschel CA, Hyzy RC, Berenholtz SM (2016) Sustaining Reductions in Central Line-Associated Bloodstream Infections in Michigan Intensive Care Units: A 10-Year Analysis. Am J Med Qual, 31(3):197-202.
Saeed M, Villarroel M, Reisner AT, Clifford G, Lehman LW, Moody G, Heldt T, Kyaw TH, Moody B, Mark RG (2011) Multiparameter Intelligent Monitoring in Intensive Care II: a public-access intensive care unit database. Crit Care Med, 39(5):952-960.
Wolf MJ, Lee EK, Nicolson SC, Pearson GD, Witte MK, Huckaby J, Gaies M, Shekerdemian LS, Mahle WT (2016) Pediatric Heart Network Investigators. Rationale and methodology of a collaborative learning project in congenital cardiac care. Am Heart J. 174:129-137.







