ICU Management & Practice, Volume 19 - Issue 2, 2019
An overview of the 'PICU Up!' mobility programme at Johns Hopkins Children's Center, which integrates sleep promotion, delirium prevention, and sedation optimisation to increase mobilisation in critically ill children.
What is the PICU Up! Programme?
Paediatric intensive units traditionally have had a culture where critically ill children are intubated and mechanically ventilated, immobilised, and highly sedated. This practice is primarily driven by a focus on safety and keeping children comfortable, along with the perception that bed rest provides greater haemodynamic stability. There is also the feeling that keeping children deeply sedated may ensure that the child does not remember their ICU stay, thus promoting the creation of a culture of immobility, which could have negative short and long-term implications for critically ill children.
You might also like:Implementation of early and structured rehabilitation in ICU
The Paediatric Intensive Care Unit at Johns Hopkins is a 40-bed, tertiary care medical surgical unit that cares for children between the ages of 0 to 22 years. In 2011, our PICU team at Johns Hopkins began to think about how we were using the terms “sleep” and “sedation” interchangeably. For example, if a child already on an opioid and a benzodiazepine was agitated, we were giving them more medicine so that they would “sleep better.” We know that sleep and sedation are very different states and can have an impact on the child’s developing brain, but we weren’t addressing the issue of restorative sleep in our patients whose brains are actively developing of children. A common misperception is that children in the PICU are older, but data from a recent multicentre study has demonstrated that more than half of our longer stay patients are under the age of two (park.web.jhu.edu). Therefore, we have an opportunity to positively impact neurocognitive development during a time that is most critical in a child’s brain maturation.
When the PICU Up! Programme was being developed for Johns Hopkins, we decided to first address sleep as the “low-hanging fruit” because sleep is very disrupted for a number of reasons in the ICU, with modifiable risk factors. There is a great deal of discussion related to delirium in the adult literature, but we were only just starting to recognise it in paediatrics. Sleep disruption can be a risk factor for delirium.
Over the years, the mortality rate in PICUs has declined quite significantly. The focus now has become not just survival, but survivorship. How does the child’s stay in the PICU affect their life? For most children, their lives are very different when they go home then they were before they came to the PICU. They are weak, and their mobility is impaired. The quality of life they knew before PICU was different from the one after hospitalisation. PICU Up! was born out of all of those different issues.
When designing the core elements of PICU Up!, we had to create an overhaul in PICU culture. Our theory was that bed rest is bad and that mobilising children during the daytime and optimising their sleep at night was the best way to minimise exposure to opioids and sedative drugs and facilitate their functional recovery. These factors grounded the foundation of our PICU Up! programme strategy.
PICU Up! Champions
PICU Up was born out of engagement from a huge multidisciplinary group of champions from nursing, physical therapy (PT), occupational therapy (OT), respiratory therapy, child life specialists, nurse practitioners, and physicians. No additional staff was hired for this programme. We worked as a team to change our PICU culture to a culture of mobility instead of a culture of immobility. We outlined strategies to decrease sedation while keeping kids still safe and comfortable. And while we did this, we also addressed other issues that impact mobility, such as sleep hygiene and delirium. Together, we were able to create a structured programme to address each child’s unique mobility needs, and championed setting a mobility goal for “Every kid, Every day.” A major goal of our PICU Up! initiative was to get children and their families back into a routine as close to what they had at home.

Image Credit: Johns Hopkins Children's Center
PICU Up! Tiered System
PICU Up! is a three-level system - PICU up! Level 1, 2, and 3. There are objective clinical criteria for levelling the patients based on how sick they are, and where each level is connected with a set of interventions based on the needs of those children. The most critically ill patients would be considered Level 1, patients who are intubated with a high oxygen requirement, for example. As they start to get better or their clinical status improves, they move to Level 2. Level 2 generally includes patients who are on non-invasive mechanical ventilation or are intubated and getting close to extubation. Finally, Level 3 patients are on the launching pad for discharge to home or the inpatient floor, but still have critical care needs- these patients have the highest potential for mobilisation.
The purpose of creating the tiered system was to define the minimum requirements for children at each of those levels. We needed to make it clear to everyone that the goal was NOT to get every intubated kid up and out of bed and walking, but that there is an individualised spectrum of mobility for every child. We wanted every kid, every day to do the most that was possible, both safely and without overwhelming available resources. It was also important to change the way we thought about patients who were traditionally considered to be “too sick for therapy.” Regardless of a child’s severity of illness, almost always a therapy evaluation can offer something beneficial, even if those therapies don’t start immediately. No patient is too sick for a physical or occupational therapy consultation, and our rehabilitation team appreciates being in the loop from the very beginning.
All patients at Johns Hopkins PICU get a PT or OT consult by day 3 of admission, and all of our patients have their sleep hygiene addressed and their routine set so that we're ideally not giving baths at 2am and not scheduling routine x-rays at 5 a.m. As patients progress, we start increasing their mobility, with an individualised mobility goal set for the day. The PICU Up! programme was implemented over a three-month period to demonstrate safety and feasibility. We collected a year of baseline pre-implementation data, implemented the programme over three months, and then looked at one year of post-implementation data. Our findings showed that the implementation of PICU Up! resulted in an increase in occupational therapy consultations and physical therapy consultations by day 3. The median number of mobilisations per patient by day 3 doubled, and more children were able to engage in mobilisation activities because of this intervention (Wieczorek et al. 2016). Twenty-seven percent of children ambulated by day 3, which was an increase of 15% pre-implementation. Among children 3 years or older, 20% ambulated prior to the implementation of the programme while 39% ambulated after implementation (Weiczorek et al. 2016).
Incorporating rehabilitation team consultation by day 3 made a huge difference, creating a culture where our nurses and our therapists were partnering together early in a child’s course. The therapist isn't at the bedside 24 hours a day, but the bedside nurse is. Therefore, it is really important for nurses to feel educated and empowered to facilitate mobility activities. Previous adult rehabilitation point-prevalence studies and emerging paediatric data are demonstrating just how crucial nursing engagement is for facilitating mobility.
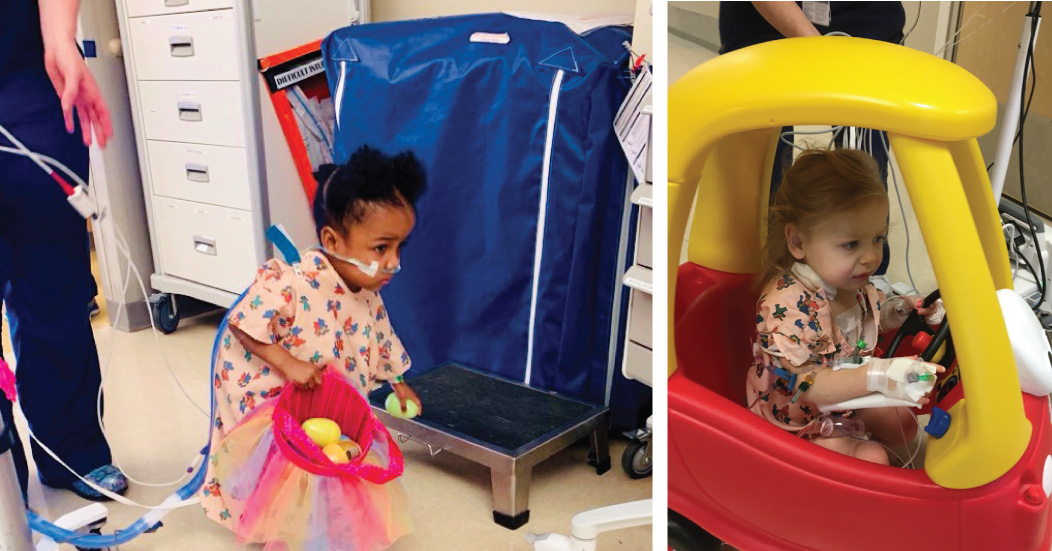

It was also really important to involve family members in mobility because they obviously play a huge role in
engaging their child. Since most of our patients are infants and toddlers, a major part of our mobility goals is to get children out of bed and to let them be held by their parents – I call it “therapeutic cuddles.” That in itself is the daily mobility goal for many of our patients. PICU Up! has enabled us to completely change the culture of the unit to a unit of mobility and to ask questions that we've never thought to ask before. For example, there are infants in the PICU that have never been outside because they've lived in the hospital since they were born. We ask if a child can safely go outside with their parents and nurse. And if they can, our staff comes together to make it happen. Natural sunlight and outdoor time can also work wonders for older children and their families, not just physically but emotionally.
The new paradigm in our unit is to have patients who are minimally sedated and comfortable while avoiding continuous benzodiazepine infusions which have been shown to be an independent risk factor for delirium. Most of our patients receive a low dose of opioid to keep them comfortable with the noxious stimuli of the endotracheal tube, with a low-dose sedative as needed, usually dexmedetomidine. Some of our older patients do beautifully with patient-controlled analgesia, which gives them a feeling of control over their own pain management. Many of our patients participate in their care and communicate with their families and our staff, telling us what their needs are. Are there patients who still receive deep sedation? Yes- there will always be patients who must be deeply sedated to facilitate physiologic stability, but the major difference is that deep sedation is no longer the default.
Primary goals of PICU Up!
Ultimately, what we want to do is to use standardised, evidence-based interventions to increase each child’s activity level in the PICU and to promote a culture of mobility. Our big picture goal is to normalise the child's routine as much as possible and optimise their functional outcome so they can go home to the best quality of life possible. Mobility, sleep hygiene, delirium prevention, and management, family engagement, and goal-directed sedation are all key components of PICU Up! and the Society of Critical Care Medicine’s ICU Liberation ‘ABCDEF’ bundle. A recent multicenter study of 15,000 adults showed that ABCDEF bundle compliance was associated with a decrease in the duration of mechanical ventilation, mortality, and delirium (Pun et al. 2019).
In the PICU, all five of these issues are intricately interrelated. If you're not sleeping at night, you're less likely to mobilise during the day. If you're not sleeping well, you're more likely to be delirious. If you're not mobilising, you're less likely to sleep well at night. If you're delirious and agitated, you're going to receive more sedation. If you're getting more sedation, you’re more likely to be delirious. If your family is not engaged, you are less likely to mobilise. It's a vicious cycle, and all of these issues feed into each other. Therefore, the levels and the activities associated with each level incorporate all four of those things: sleep hygiene, delirium screening, early rehab, and goal-directed sedation. The multi-component bundled intervention is bringing it all together so that people think of it as a PICU liberation approach as opposed to the sedation, delirium, and rehabilitation silos.
Types of activities for children in the PICU
Early mobilisation activities include in-bed activities such as passive range of motion, passive bed positioning, splinting, active range of motion, and active bed positioning. As patients progress, activities include motivating patients to sit on the edge of the bed, sit to stand, transfer, ambulate, and play (Wieczorek et al. 2016). Play is a key part of this programme. For babies, there's developmental play that is facilitated by our occupational therapists and child life specialists who bring in all sorts of unique items for the babies to play and engage with. The older children who can leave the unit can go to the rehab kitchen and bake cookies and brownies. They may not always be able to eat their baked goods, but they can always come back and distribute them to our staff! We also have riding and stationary bikes and portable treadmills for older children. Video games are an excellent way to facilitate dexterity for some of our older patients who aren’t ready to get out of bed but can still use their hands.
Video Credit: Johns Hopkins Children's Center
Another key part of our rehabilitation initiative is our Augmented and Assistive Communication (AAC) programme. With more PICU patients awake and alert while intubated, we quickly realised we needed to give them more ways to communicate. Our child life specialists, occupational therapists, speech language pathologists, and nurses work together to identify a child’s needs and create a communications plan with low-tech and high-tech devices. It may be as simple as a whiteboard or a board with pictures for them to point to; many of our older patients are writing, and can also use other devices like an iPad, and their families can also communicate with them. Several of our patients have texted with their friends, done homework to keep up at school, and use video chat to communicate with family when they are not at the bedside. Even for children who do not survive their PICU stay, facilitating communication can be priceless for patients and families at the end of life.
Video Credit: Johns Hopkins Children's Center
Mobility and the sedated child
For children who require deep sedation, we get our rehabilitation team to the bedside as soon as possible and make sure that we're doing as much as possible while they're sedated to prevent morbidity. For other patients, we optimise active engagement in mobility which has changed how much sedation they need. Increased activity during the day means less delirium and improved circadian rhythms. There's no question that the PICU Up! programme has helped decrease sedative and opioid use among PICU patients, and we are actively studying these outcomes.
Wider implementation of PICU Up!
We want to facilitate the implementation of multicomponent mobility programmes as widely as possible to decrease the need for PICUs to “reinvent the wheel.” PICU Up! is already being implemented in several other PICUs in the United States including the Cincinnati Children’s Hospital, Northwestern Lurie Children's Hospital, University of Virginia, Vidant Hospital in North Carolina and St. Jude Children's Hospital. Every year we host about 150 multidisciplinary team members who come to learn specifically about paediatric critical care rehabilitation implementation at the Annual Johns Hopkins Critical Care Rehabilitation Conference (bit.ly/icurehab). If a PICU wants to license our programme, we can make that happen. Or if they want to create and implement their own programme, we are here to help. The goal is to ensure that a culture of mobility is disseminated safely and effectively. We have six other ICUs that are set to implement the programme within the next year as part of a multicentre, randomised controlled trial (clinicaltrials.gov/ct2/show/NCT03860168).
Future Plans
First, we need to demonstrate that programmes like PICU Up! have an impact on both short and long-term patient outcomes. The natural next step is then to start to hone in more on the mechanisms by which our interventions are working and to determine the appropriate dose, frequency, and duration of rehabilitation for critically ill children. We also want to determine what activities are the most beneficial for which patients, and how often should we be doing them moving forward. It’s important for children to be able to get back to the lives they had before their critical illness as quickly as possible. We need to ask if these children, once discharged from the PICU, are sleeping differently when they go home? Are we making a difference in their long-term sleep patterns and sleep trajectory? What are the underlying mechanisms by which all of these interventions are working so that we can continue to understand more on a patient-based level and can optimise outcomes for every child in the PICU? There is much work to do.
Key points
- The primary goals of the PICU Up! programme include increasing mobility, normalising the child's routine, optimising their functional outcome, optimising sleep hygiene, and decreasing exposure to sedative and interventions with medications.
- PICU Up! was made possible by engagement from a huge multidisciplinary group of champions.
- PICU Up! is a tiered system that uses objective clinical criteria for levelling patients based on their severity of illness.
References:
PARK-PICU. Prevalence of acute rehab for kids in the PICU. Available from park.web.jhu.edu/
PICU Up!: Trial of a Multicomponent Early Mobility Intervention for Critically Ill Children (PICU Up!). Available from clinicaltrials.gov/ct2/show/NCT03860168
Pun BT, Balas MC, Barnes-Daly MA, Thompson JL, Aldrich JM, Barr J, Byrum D, Carson SS, Devlin JW, Engel HJ, Esbrook CL, Hargett KD, Harmon L, Hielsberg C, Jackson JC, Kelly TL, Kumar V, Millner L, Morse A, Perme CS, Posa PJ, Puntillo KA, Schweickert WD, Stollings JL, Tan A, D'Agostino McGowan L, Ely EW (2019) Caring for Critically Ill Patients with the ABCDEF Bundle: Results of the ICU Liberation Collaborative in Over 15,000 Adults. Critical Care Medicine, 47(1):3-14.
Wieczorek B, Ascenzi J, Kim Y, Lenker H, Potter C, Shata NJ, Mitchell L, Haut C, Berkowitz I, Pidcock F, Hoch J, Malamed C, Kravitz T, Kudchadkar SR (2016) PICU Up!: Impact of a Quality Improvement Intervention to Promote Early Mobilization in Critically Ill Children. Pediatr Crit Care Med, 17(12):e559–e566.







