ICU Management & Practice, Volume 17 - Issue 4, 2017
This article highlights the key current challenges of intensive care training and education. We share our experience of utilising modern educational techniques through the BASIC Collaboration to facilitate global critical care training.
Critical care is a young and rapidly expanding specialty. This brings particular challenges in training staff. Survey data demonstrate that many medical schools do not teach critical care, and studies consistently show a failure by junior medical staff to recognise and appropriately manage critically ill patients (Shen et al. 2003; McQuillan et al. 1998). Thus doctors entering training in intensive care have very rudimentary knowledge of and skills in critical care. In parts of the world the problem is exacerbated by shorter working hours, which raise concerns that training will be impaired (Moonesinghe et al. 2011).
You might also like:Adult education for ICU management: a better way
Training in medicine has traditionally followed a master and apprentice model, which is well suited to established specialties that are not undergoing rapid growth. However, this is not the case in critical care where a significant imbalance between masters and apprentices is common.
Technological advances have also expanded the scope of practice of critical care practitioners. Ultrasound machines are now widely available at affordable cost, and with that availability has come the expectation that critical care practitioners will acquire the expertise to use these devices (Mayo 2011). Non-medical technological advances also mean that our traditional approach to training may require re-thinking. Traditional approaches to medical education have emphasised acquisition and retention of knowledge, with an emphasis on memory. However, the widespread availability of mobile devices incorporating Internet connectivity and high memory capacity should prompt a greater emphasis on training doctors to apply knowledge rather than memorise facts (Mobasheri et al. 2015). Furthermore, patient safety discourages reliance on memory in favour of checking reference sources (Nolan 2000).
As a result it is necessary to devise training programmes that use the time of the available masters in the most efficient manner, emphasise development of skills and allow training of large numbers of healthcare workers. Furthermore the rapid growth of critical care research, in particular the strength of collaborative investigator-led trials groups, has led to the need to frequently update the content of training programmes (Marshall 2017).
The herculean task of providing suitable training to sufficient numbers of critical care healthcare workers is well illustrated by the example of China. It has previously been estimated that, even with a relatively low Intensive Care Unit (ICU) bed provision of 1-2% of hospital beds, the total number of ICU beds in China was approximately 52,000. Assuming a low ratio of 4 nurses per bed and 1 doctor for 5 beds, this equates to a need for training for approximately 200,000 nurses and 10,000 doctors. At that time there was no formal training programme in either intensive care medicine or nursing in China (Du et al. 2010).
However, by concentrating on critical care as a geographical location this illustration underestimates the magnitude of the task. There is an increasing awareness that our specialty involves care of critically ill patients, regardless of their location, not just the care of patients in ICUs (Adhikari et al. 2010).
Solutions
Our belief is that the solution lies in a collaborative approach to education. This allows a pooling of efforts to develop and provide high-quality education that is responsive to changing needs, practice and technology. One of the best early examples of this approach was the development and dissemination of the Fundamentals of Critical Care Support (FCCS) course by the Society of Critical Care Medicine. This course consists of pre-course reading, short lectures and small group teaching (Joynt et al. 2011). The material is written and updated by a small group of intensivists with an interest in education, but the course is delivered at a local level by a large number of intensivists in multiple locations across the globe. A similar approach has been taken by our group and we describe our experience below.
Apart from the gain in efficiency resulting from avoiding repeated re-invention of the wheel, this approach has the advantage of making more efficient use of masters’ time by minimising the need to spend time on simple knowledge transfer. Instead, candidates are expected to acquire the relevant knowledge by reading the course manual before attending the course, so that the course can be devoted to reinforcing important points and acquisition of skills (both practical and cognitive). This is the underlying principle of the ‘flipped classroom’ approach, which is gaining favour in education. In its purest form students acquire all the necessary knowledge before attending face-to-face teaching, which then concentrates on application of that knowledge to problems. This is the reverse of traditional classroom teaching, in which didactic teaching occurs face to face and problem solving is carried out unsupervised, in the form of homework.
The BASIC Collaboration
The
BASIC Collaboration was founded in 2004, with a logistic and administrative
base in the Department of Anaesthesia & Intensive Care, The Chinese
University of Hong Kong. While inspired by the FCCS course and the Society of
Critical Care Medicine, the Collaboration differs in a number of aspects.
Firstly, it is entirely focused on medical education. Secondly, a deliberate
decision was made not to charge licence fees for running courses. Thirdly, the
Collaboration is deliberately international. Since its inception and the
development of its first course, Basic Assessment and Support in Intensive Care
(BASIC) (Joynt et al. 2011; Douglas et al. 2010), the Collaboration courses
have been run in over 50 countries (Figure 1), the number of different courses
has grown (Table 1) and the number of healthcare workers trained each year
has grown steadily (Figure 2). An estimated 40,000 healthcare workers have been
taught in total. In keeping with our belief in collaboration, courses have been
developed with the European Society of Intensive Care Medicine (Intensive Care
Nephrology – beyond BASIC) and Médecins Sans Frontières (BASIC for Developing
Healthcare Systems and BASIC DHS for Nurses). In keeping with our belief that
our specialty encompasses care of critically ill patients wherever they may be,
our portfolio of courses includes acute care in high-resource non-ICU settings
(Very BASIC) and in low-resource settings (BASIC DHS and BASIC DHS for Nurses).
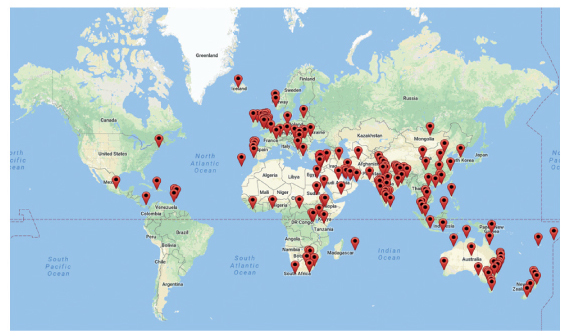
Figure 1. BASIC Collaboration course venues since 2004. Reproduced from https://multiplottr.com/?map_id=125266
Table 1. Currently running BASIC courses and their development origins
| Course | Subject | Target audience | Country base of development team | Launch year |
| Basic Assessment & Support in Intensive Care (BASIC) | Introduction to adult intensive care | Intensive care novices (physicians) | AU, HK, UK, NZ | 2004 |
| Paediatric BASIC | Introduction to paediatric intensive care | Intensive care novices (physicians) | AU, CA, HK, ZA | 2012 |
| BASIC for Nurses | Acute care of critically ill patients outside ICU | Intensive care novices (nurses) | AU, HK | 2013 |
| Very BASIC | Acute care of critically ill patients | Final year medical students and junior doctors in high-resource settings | AU, HK, NZ, UK | 2005 |
| BASIC for nurses on the ward | Acute care of critically ill patients | General ward nurses | HK, NZ | 2007 |
| BASIC for Developing Healthcare Systems (BASIC DHS)* | Acute care of critically ill patients | Doctors and medical students in low-resource settings | FR, HK | 2011 |
| BASIC DHS for Nurses* | Acute care of critically ill patients | Nurses in low-resource settings | AU, FR, HK | 2015 |
| BASIC Science | Basic sciences relevant to intensive care | Junior intensive care trainees | AU, HK, NZ | In progress |
| BASIC Patient Safety | Patient safety for clinicians | Clinical healthcare professionals | HK, NO, UK | 2010 |
| BASIC Clinical Research | Introduction to clinical research | Clinical research novices | AU, CA, HK, NZ | 2016 |
| BASIC Transthoracic echocardiography | Echocardiography in critically ill patients | Intermediate Intensive Care trainees | HK | 2017 |
| Mechanical Ventilation: beyond BASIC | Mechanical ventilation | Intermediate-senior intensive care trainees and as a refresher for intensive care specialists | HK, NO, NZ | 2009 |
| Intensive Care Nephrology: beyond BASIC# | Nephrology relevant to intensive care | Intermediate-senior intensive care trainees and as a refresher for intensive care specialists | HK, IN, NO, NZ, PT, UK | 2011 |
| Airway Management: beyond BASIC | Airway management relevant to Intensive Care | Intermediate-senior intensive care trainees and as a refresher for intensive care specialists | AU, HK | 2013 |
| Cardiothoracic Intensive Care: beyond BASIC | Post operative cardiac intensive care | Intermediate-senior intensive care trainees and as a refresher for intensive care specialists | HK, NO, UK | 2016 |
| Cardiocerebral Resuscitation: beyond BASIC | In-hospital cardiocerebral resuscitation | Hospital doctors | HK, IN, NO | 2014 |
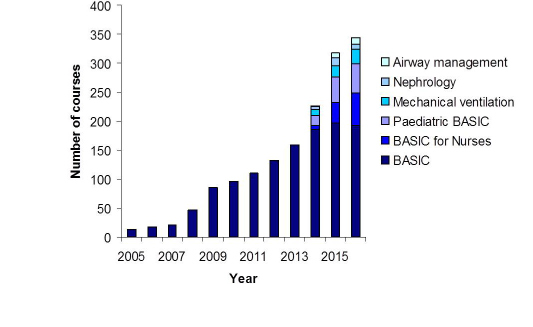
Figure 2. Selected BASIC Collaboration courses since 2005 – number of courses. Data for BASIC for Nurses, Paediatric BASIC and Beyond BASIC Mechanical Ventilation, Nephrology and Airway Management courses were only collected from 2014.
What have we learned from the BASIC Collaboration?
Collaboration is better
While the benefits are seemingly self-evident, international collaboration in education lags behind collaboration in research. Each BASIC Collaboration course is written by a small group of authors, but each course benefits from continual informal peer review by multiple course instructors across the world. Instructors are encouraged to submit criticisms and comments, and rapid and recurrent review of the material is facilitated by distribution of course material in an electronic format. Furthermore the material is continually revised to maximise understanding and skill development, based on feedback from both instructors and participants. This is an essential but time-consuming part of the development of high-quality material, which is only possible through collaborative efforts. The process of quality improvement is made worthwhile by the large number of people who are trained. We believe our policy of not charging licence fees improves collaboration by removing any suspicion of financial conflicts of interest.
Flipped classrooms
Over the past 12 years our Very BASIC course has transformed from a partial to a fully flipped classroom format (Gruber et al. 2007). Students are expected to not only read the course manual but also to complete e-learning material, in the form of short narrated lectures, interactive lessons and formative assessment, before attending faceto- face small group teaching (Gomersall et al. 2010). The premise underlying this approach is that valuable teacher time is better spent on high-value small group teaching than on low-value lecturing (Schwartzstein and Roberts 2017). The saving in teacher time, as a result of the abolition of face-to-face lectures has allowed us to maintain small group teaching despite a 75% increase in class size—with only a minimal increase in resources. Surprisingly, student feedback indicates a preference for e-learning lectures over face to face. Students like the ability to listen to a lecture at a time that suits them and to replay segments of the lecture. While we believe that e-learning is essential in preparing students so that they achieve maximal benefit from small group teaching, e-learning alone may not have a significant effect on students’ ability to manage clinical situations. We have shown that interactive electronic learning alone was not associated with improved medical student performance responding to scenario-based questions on managing mechanical ventilation, but the addition of just one hour of small group face-to-face teaching designed to reinforce application of knowledge was associated with a marked improvement (Leung et al. 2017).
Mobile apps
The Very BASIC course is supported by a free mobile app which facilitates quick retrieval of key information and also contains an electronic version of the course manual. The premise of the app is that medical students may not be able to rapidly recall information they have learned after they qualify but, if familiar with the app, will be able to find it rapidly when it is required. Once installed, the app can be used entirely offline, except to receive updates. This circumvents concerns regarding use in close proximity to key medical equipment and allows use of the app in clinical situations. Usage data from the app indicates that 30% of final year medical students continued to use the app following qualification (Leung et al. 2015; 2017). A free mobile app to support the BASIC course has just been introduced and we plan to develop mobile apps for all of our courses. Developing a mobile app for BASIC for Developing Healthcare Systems is a high priority. Costs of printing course manuals in low-income countries are high and may even match the disproportionately high cost of air freight to these countries. However, anecdotal evidence suggests that a high proportion of doctors in some lowincome countries possess a smartphone or tablet, opening the possibility of using an app as an alternative to printed course manuals.
Conclusion
Training sufficient healthcare workers to provide high-quality care to critically ill patients across the globe is a major challenge. We believe that a collaborative approach utilising modern educational techniques and advances in mobile technology will facilitate attempts to meet that challenge.
Conflict of interest
Charles
David Gomersall is the chair of the BASIC steering committee. Wai Tat Wong and
Lowell Ling are instructors for the BASIC courses.









