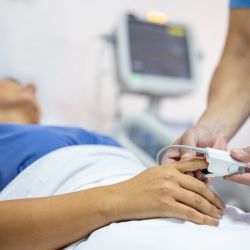
ICU Management & Practice, ICU Volume 15 - Issue 4 - 2015
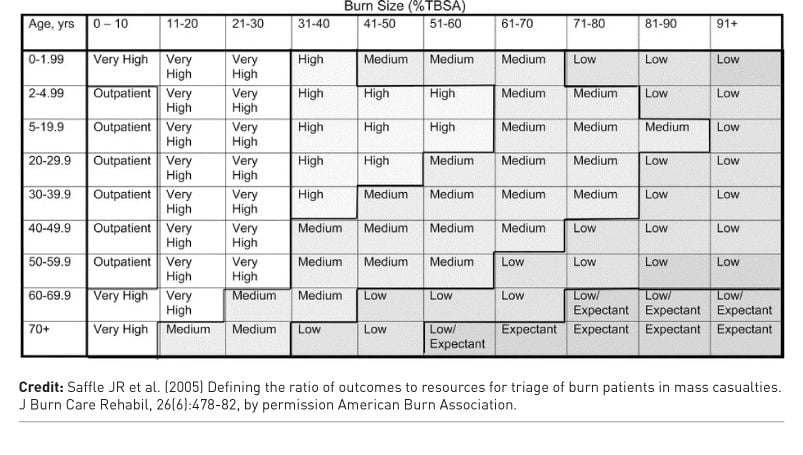
- Outpatient: Patients that will have greater than 95% survival and will not need to be hospitalised.
- Very High: Survival greater than or equal to 90%, length of stay (LOS) less than or equal to 14-21 days, 1 to 2 operations needed.
- High: Survival greater than or equal to 90%, LOS 14-21 days, multiple operations necessary, prolonged rehabilitation.
- Medium: Survival greater than 50% but less than 90% even with full treatment.
- Low: Survival greater than 10% but less than 50% despite full treatment.
- Expectant: Survival less than or equal to 10% despite full treatment.
References:
ABA Board of Trustees, the Committee on Organization and Delivery of Burn Care (2005) Disaster management and the ABA plan. Journal Burn Care Rehabil, 26(2): 102-6.
American Burn Association (2015) National burn repository benchmark report. [Accessed: 3 November 2015] Available from ameriburn.org
American Burn Association (2014) Consultation/verification program for burn centers. [Accessed: 3 November 2015] Available from ameriburn.org
American College of Surgeons, Committee on Trauma (2006) Resources for optimal care of the injured patient. Chicago, IL: ACS.
Barillo DJ, Hallock GG, Mastropieri CJ et al. (1989) Utilization of the burn unit for nonburn patients: the “wound intensive care unit”. Ann Plast Surg, 23(5): 426-9.
Baxter CR, Marvin J, Curreri PW (1973) Fluid and electrolyte therapy of burn shock. Heart Lung, 2(5): 707-13.
Bell N, Simons R, Hameed SM et al. (2012) Does direct transport to provincial burn centres improve outcomes? A spatial epidemiology of severe burn injury in British Columbia, 2001-2006. Can J Surg, 55(2): 110-6.
Birkmeyer JD (2000) Should we regionalize major surgery? Potential benefits and policy considerations. J Am Coll Surg, 190(3): 341-9.
Birkmeyer JD, Siewers AE, Finlayson EV et al. (2002) Hospital volume and surgical mortality in the United States. N Engl J Med, 346(15): 1128-37.
Brigham PA, Dimick AR (2008) The evolution of burn care facilities in the United States. J Burn Care Res, 29(1): 248-56.
Curreri PW, Richmond D, Marvin J et al. (1974) Dietary requirements of patients with major burns. J Am Diet Assoc, 65(4): 415-7.
Demling RH, DeSanti L (2003) Oxandrolone induced lean mass gain during recovery from severe burns is maintained after discontinuation of the anabolic steroid. Burns, 29(8): 793-7.
Desai MH, Herndon DN, Broemeling L et al. (1990) Early burn wound excision significantly reduces blood loss. Ann Surg, 211(6): 753-9.
Endorf FW, Supple KG, Gamelli RL (2005) The evolving characteristics and care of necrotizing soft-tissue infections. Burns, 31(3): 269-73.
Faucher LD, Morris SE, Edelman LS et al. (2001) Burn center management of necrotizing soft-tissue surgical infections in unburned patients. Am J Surg, 182(6): 563-9.
Gamelli RL et al. (2007) ABA/ACS Verification review committee [PowerPoint presentation]. [Accessed: 6 November 2015] Available from: ameriburn.org/VerificationPresentation.pdf
Gibran NS, Klein MB, Engrav LH et al. (2005) UW Burn Centre. A model for regional delivery of burn care. Burns, Suppl 1: S36-9.
Healthcare Cost and Utilization Project (2010) National inpatient sample (HCUP-NIS: 2010 data); National hospital discharge survey (2010 data). [Accessed: 3 November 2015] Available from hcup-us.ahrq.gov/db/nation/nis/NISIntroduction2010.pdf
Holmes JH 4th, Carter JE, Neff LP et al. (2011) The effectiveness of regionalized burn care: an analysis of 6,873 burn admissions in North Carolina from 2000 to 2007. J Am Coll Surg, 212(4): 487-95.
Hussain A, Choukairi F, Dunn K (2013) Predicting survival in thermal injury: a systematic review of methodology of composite prediction models. Burns, 39(5): 835-50.
Jeschke MG, Finnerty CC, Shahrokshi S et al. (2013) Wound coverage technologies in burn care: novel techniques. J Burn Care Res, 34(6): 612-20.
Kastenmeier A, Faraklas I, Cochran A et al. (2010) The evolution of resource utilization in regional burn centres. J Burn Care Res, 31(1): 130-6.
Klein MB, Mack CD, Kramer CB et al. (2008) Influence of injury characteristics and payer status on burn treatment location in Washington state. J Burn Care Res, 29(3): 435-40.
Klein MB, Nathens AB, Emerson D et al. (2007) An analysis of the long-distance transport of burn patients to a regional burn centre. J Burn Care Res, 28(1): 49-55.
Klein MB, Nathens AB, Heimbach DM et al. (2006) An outcome analysis of patients transferred to a regional burn center: transfer status does not impact survival. Burns, 32(8): 940-5.
MacKenzie EJ, Rivara FP, Jurkovich GJ et al. (2006) A national evaluation of the effect of trauma-centre care on mortality. N Engl J Med, 354(4): 366-78.
Luft HS, Bunker JP, Enthoven AC (2007) Should operations be regionalized? The empirical relation between surgical volume and mortality. Clin Orthop Relat Res, 457: 3-9.
Pacella SJ, Butz DA, Comstock MC et al. (2006) Hospital volume outcome and discharge disposition of burn patients. Plas Reconstr Surg, 117(4): 1296-305.
Palmieri TL, London JA, O’Mara MS et al. (2008) Analysis of admissions and outcomes in verified and nonverified burn centers. J Burn Care Res, 29(1): 208-12.
Palmieri TL, Greenhalgh DG, Saffle JR et al. (2002) A multicentre review of toxic epidermal necrolysis treated in U.S. burn centers at the end of the twentieth century. J Burn Care Rehabil, 23(2): 87-96.
Patel NP, Brandt CP, Yowler CJ (2006) A prospective study of the impact of a critical care pharmacist assigned as a member of the multidisciplinary burn care team. J Burn Care, 27(3): 310-3.
Praiss IL, Feller I, James MH (1980) The planning and organization of a regionalized burn care system. Med Care, 18(2): 202-10.
Saffle JR, Gibran N, Jordan M (2005) Defining the ratio of outcomes to resources for triage of burn patients in mass casualties. J Burn Care Rehabil, 26(6): 478-82.
Sheridan RL, Hinson MI, Liang MH et al. (2000) Long-term outcome of children surviving massive burns. JAMA, 283(1): 69-73.
Sheridan RL (2003) Burn care: results of technical and organizational progress. JAMA, 290(6): 719-22.
Sheridan R, Weber J, Prelack K et al. (1999) Early burn centre transfer shortens the length of hospitalization and reduces complications in children with serious burn injuries. J Burn Care Rehabil, 20(5): 347-50.
Taylor S, Jeng J, Saffle JR, et al. (2014) Redefining the outcomes to resources ratio for burn patient triage in a mass casualty. J Burn Care Res, 35(1): 41-5.
Warden GD, Heimbach D (2003) Regionalization of burn care – a concept whose time has come. J Burn Care Rehabil, 24(3): 173-4.
Wolf SE, Rose JK, Desai MH et al. (1997) Mortality determinants in massive pediatric burns. Ann Surg, 225(5): 554-69.
Zonies D, Mack C, Kramer B et al. (2010) Verified centers, nonverified centers, or other facilities: a national analysis of burn patient treatment location. J Am Coll Surg, 210(3): 299-305.