The goal of aC3KTion Net was to recruit as many academic and community hospitals in Canada as possible into the network. Academic centres were recruited by identifying hospitals and ICUs affiliated with the Canadian Critical Care Trials Group (CCCTG 2015). A public list of hospitals, which included community hospitals, was used to identify other hospitals not affiliated with the CCCTG. Those with ICUs were identified by investigating hospital websites, and were then contacted by telephone for confirmation (CBC 2013). Identified ICUs were encouraged to register with aC3KTion Net via email, personal contacts and telephone solicitation. All units with self-identified ICUs were eligible for inclusion into aC3KTion Net and were encouraged to participate. A web-based registration platform (acktionnet.ca) was set up to enable registration.
To enable the function of the network and collect information on baseline practice, a modular data set was developed. It was designed to be used in all activities of the network and consisted of a Core Data Set (CDS) on to which modules could be added reflecting the data requirements of new initiatives as they were identified and implemented. The CDS was designed to be able to be used for any future research, knowledge translation or quality improvement initiatives depending on the add-on modules collected with the CDS. The CDS is comprised of admission, daily and outcome report forms. The Scientific and Steering Committees together defined the core data variables required for the CDS. The individual data elements in the CDS were explicitly defined to improve uniformity of the data collected. The definitions associated with each variable in the CDS were vetted through the Candian Critical Care Trials Research Coordinator group (CCCRCG 2015).
To assess the clarity of the definitions and time burden associated with data abstraction of the CDS, a Research Ethics Board-approved feasibility study was conducted in which data abstractors at five sites were asked to collect data on five patients each. Strict records of the time required to collect this data were kept. Source charts were then obtained and the data abstracted was compared with the source charts as a way to verify the utility of definitions and to determine variability in their interpretation.
Baseline Survey of Practices
In order to assess the penetration of research evidence into practice a baseline practice survey was conducted. A stepwise approach was used to determine which practices to survey. First the Steering committee identified nine potential ICU practices using the key requirement that current evidence-based practice guidelines existed. This was used as an indicator of the maturity of evidence and potential for knowledge translation (KT) activities. Moreover the presence of existing guidelines would allow for the determination of concordance to best evidence. The practices chosen included: Ventilator-Associated Pneumonia (VAP), Hypothermia after Cardiac Arrest, Nutrition for Critically Ill, Noninvasive Ventilation, Pain, Agitation and Delirium, Neurological prognostication after cardiac arrest, Thromboprophylaxis, Central Line infections and Sepsis. In addition the committees were asked to contemplate critical care practices for longer-term initiatives including surveys of practice and guideline development. Thirty-four initiatives were put forward as options for future initiatives. These included, but were not limited to: End-of-Life Care, Early Mobility, Mechanical Ventilation, Antimicrobial Stewardship, Staffing practices and Acute Kidney Injury. A modified Delphi process (RAND 1994) was then conducted using SurveyMonkey (SurveyMonkey 1999) involving all the members of the Steering and Scientific Committees. The respondents ranked each initiative using a Likert scale as “not very important” (1) to “very important” (9). The results for each initiative were then summed and ranked in order from highest to lowest score. The bottom four of both the current and future initiatives were removed after the first iteration. By the third round, stability had been reached; Ventilator-Associated Pneumonia (VAP) (Muscedere 2008a; 2008b), Sepsis (Dellinger 2008) and Nutrition (Dhaliwal 2014) were the three identified as being of highest priority. Among the practices where no guidelines are available, Endof-Life Care was identified as being the highest priority. Once the initiatives were identified, data modules were developed and added to the CDS. An electronic database REDCap (Vanderbilt University 2015) was used to collect data.
Registered sites who had agreed to participate in the baseline survey of practice collected patientlevel data for the CDS and practice modules as applicable. The number of participants requested from each site was predicated on the number of ICU beds at the site: ≥20 beds = 30 participants, ≤19 beds ≥ 10 beds =20 participants and ≤ 9 beds = 10 participants. As a quality improvement initiative, patient-level data was anonymised, and would only be presented in aggregate; Central Research Ethics Board approval, including a waiver of consent was sought and granted from Queen’s University.
Repository
Housed on the website, a restricted-to-member repository of Canadian critical care documents was established. The repository was primarily populated with documents shared on the Critical Care Google Group, an online discussion group affiliated with the Canadian Critical Care Society (CCCS). Each document conserved in the repository was protected by a caveat emptor disclaimer drafted to mitigate liability, and was only shared in the repository after permission was granted by the original Google Group poster.
Undertaking Knowledge Translation
Due to the widespread nature of the network, KT primarily consisted of passive KT, dissemination of material via the distribution lists, or by posting on the website. Webinars were hosted, including those on VAP guidelines and Sepsis. aC3KTion Net also hosted a six-month long Accelerated Collaborative in conjunction with the Canadian ICU Collaborative (Northway 2008) targeting sepsis, VAP and nutritional support in the ICU.
Results
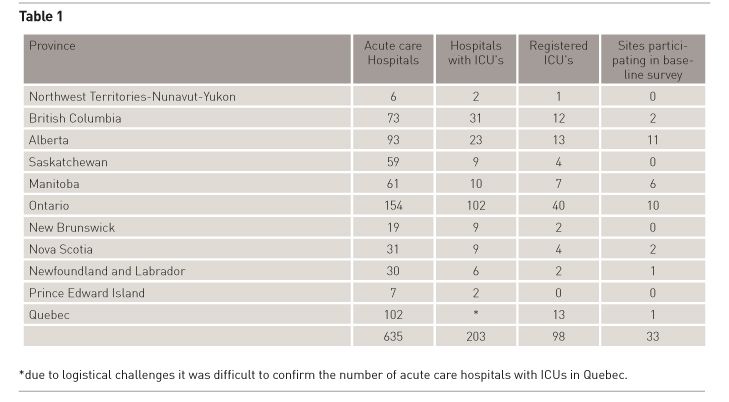
The number of acute care hospitals, those with an ICU, the number of sites registered with aC3KTion Net and the number of sites that participated in the baseline survey of practice is outlined in Table 1. A total of 98 ICUs across Canada enrolled in aC3KTion Net with 33 of them agreeing to collect data on baseline practices.
Data Collection Metrics
Based on the feasibility study, the time to abstract the CDS for a patient with an average length of stay (LOS) of eight days was a mean of 50.9 minutes (± 24.9 minutes) with a range of 26.0 minutes to 1.3 hrs. For the same average LOS, abstracting 30 patients would take a mean 25.5 hours (±12.5 hours).
Survey of Practice and Repository
Approximately 900 participants have been entered into the REDCap database. Analysis is pending the receipt of additional data from some of the sites. The repository of critical care documents was organised according to Organ Systems, Trauma, Pharmacology in the ICU, End-of-Life Care and Advanced Care Planning, Diagnostic Modalities, Rehabilitation, Nursing Management, ICU design and Laboratory medicine. This repository houses over 500 documents from across Canada and the database is searchable by keyword. In spite of aggressive recruitment efforts, only four sites registered for the collaborative with a total of seven projects. Passive KT efforts continue.
Discussion
We have developed a national network of ICUs which is inclusive of both academic and community centres. The creation of a standardised CDS, element data dictionary and scalable modular data system, which can be utilised for quality improvement or research will enable any future initiatives in this regard. We have amassed a repository of practice documents from across the country in a searchable, retrievable manner, which is and will continue to be a resource into the future for any clinician wishing to adapt them to their practice environment. This repository will continue to grow over time. We will continue to build the relationships within the network and with external organisations as we go forward, including the Choosing Wisely campaign (Choosing Wisely Campaign Canada 2015). In spite of these successes, aC3KTion Net encountered many challenges and was not able to carry out many of the activities envisioned at its initiation.
The nature of healthcare in Canada is that it is rendered regionally. Without federal oversight each province or territory is responsible for overseeing its own healthcare, resulting in thirteen systematically different healthcare systems, presenting a challenge when creating a national network. Further compounding this is the lack of public availability of a catalogue of acute care resources on either a federal or provincial basis, which made it difficult to identify all the acute care hospitals in Canada. In addition, determining which hospitals had critical care units was even more challenging. This necessitated a long labour-intensive process to identify ICUs, contact them and recruit them into the network. Although some provinces maintain up-to-date registries of critical care units, a registry of ICUs at the national level would facilitate initiatives such as ours, critical care resource management, human resource management and would be of importance during crises such as pandemics. This initiative has reinforced the need for the development of such a resource.
Despite broad support and enthusiasm for the baseline survey of practice, by June 2015 only one-third of registered ICUs had contributed data to the survey or approximately 900 participants nationwide. The lack of financial incentives from aC3KTion Net and lack of local resources at the site level were anecdotally identified as being responsible for not being able to contribute data at all or in a timely manner. Although the average time to abstract the CDS was significant, it was less than one hour per patient and we estimate that data collection per patient was less than two hours when the modules were included with the CDS. Although most ICUs maintain that quality improvement is a priority, in reality, dedicating resources to its conduct in the busy environment of the ICU remains challenging. This was a common refrain from our participating sites. Other factors which may have led to the poor response of baseline practice included the launch of multiple initiatives at once and perceived lack of return for the time spent on data collection. Financial incentives were not available for the collection of the data, and it is possible that the offer of standardised comparative reports of performance, ability to participate in our KT activities and access to the repository of practices was perceived to be insufficient. This will require further investigation.
The purpose of the baseline survey of practice was to ascertain penetration of research evidence into current practice and thereby target our knowledge translation efforts to the largest gaps. Since the baseline survey is incomplete, we have not been able to do this on a large scale. To this end, we offered the collaborative opportunity to ICUs which would or had completed the baseline survey. In spite of aggressive recruitment for the collaborative and expressed interest, participation was very limited with the expressed barriers being lack of availability of staff and the time commitment required. For the hospitals that participated in the collaborative, it was well received, and garnered positive feedback. Again, the ability to commit resources to external quality improvement initiatives appears to be limited. We are unable to comment on internal quality improvement.
Conclusion
We have developed a platform for KT activities that is nationally inclusive of both academic and community centres. Once complete, the analysis of the baseline practice data will provide insights and directionality forward. Many resource challenges and barriers to the conduct of KT and quality improvement in Canadian critical care units are present and provided challenges for the operation of the network as it was originally envisioned. More efforts are required to overcome these challenges and these are ongoing.