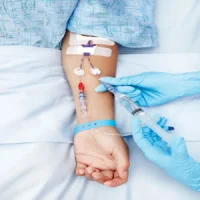
Post-traumatic stress disorder — often thought of as a symptom of warfare, major catastrophes and assault — can also affect patients who survive a critical illness and stay in the intensive care unit (ICU). A Johns Hopkins study has found that nearly one-quarter of ICU survivors suffer from PTSD. Researchers also identified possible causes of PTSD and indicated a potential preventive strategy: having patients keep ICU diaries. The findings will be published in the May issue of Critical Care Medicine.
Through a systematic literature review, the researchers looked at 40 studies of 36 unique patient cohorts with a total of more than 3,000 patients who survived a critical illness and ICU stay. The analysis excluded patients who had suffered a trauma, such as a car crash, or brain injury, because those patients' cognitive and psychological outcomes can be affected by the injury itself, rather than the critical illness/ICU stay. Data revealed that the prevalence of PTSD in the studies ranged from 10 to 60 percent.
The research team also performed a meta-analysis of a subset of the 40 studies to obtain a more definitive estimate of PTSD prevalence. They selected six studies, with a total of about 450 patients, that used a PTSD measurement tool called the Impact of Event Scale between one and six months after ICU discharge. The data indicated that one in four patients had symptoms of PTSD. The researchers also reviewed studies that looked at patients seven to 12 months after an ICU stay and found that one in five patients had PTSD.
"These rates are as high as you might see in combat soldiers or rape victims," says Dale Needham, MD, a professor of medicine and of physical medicine and rehabilitation at Johns Hopkins University School of Medicine. "Our clinicians and patients should know that the high risk of PTSD exists among patients surviving critical illness."
The research team identified these common risk factors for PTSD: being diagnosed with a psychological problem (eg, anxiety or depression) before coming to the ICU; receiving large amounts of sedation medication while in the ICU; and having frightening memories of being in the ICU.
These symptoms occur across a wide variety of patients, regardless of their age, diagnosis, severity of illness or length of stay. "This tells us that if we focus on factors traditionally associated with worse physical outcomes, such as a patient's age, we may miss individuals with psychiatric symptoms," says Joe Bienvenu, MD, associate professor of psychiatry and behavioural sciences at Johns Hopkins.
The researchers also looked at the best ways to prevent PTSD. The solution that seemed most effective was an ICU diary, a notebook that allows clinicians and family members to write daily messages about what is happening to the patient.
At The Johns Hopkins Hospital, the medical ICU team will be implementing a quality improvement project that will include using an ICU diary as a tool to prevent PTSD and improve recovery. Relatively few institutions in the US utilise ICU diaries, but these are commonly used in Europe. Johns Hopkins plans to use them for patients entering the medical ICU and will further evaluate their effectiveness as a therapeutic tool.
Each year, more than 5 million people require ICU-level care in the United States and more than 750,000 Americans need mechanical ventilators. "It's clear that those who care for ICU patients need to be aware that there could be long-term consequences of critical illness and lifesaving treatments, including PTSD, which can significantly limit a patient's quality of life well after discharge," according to Ann Parker, a fellow in the Johns Hopkins Medicine Division of Pulmonary and Critical Care Medicine.
Source: Johns Hopkins Medicine
Image Credit: Flickr.com
Through a systematic literature review, the researchers looked at 40 studies of 36 unique patient cohorts with a total of more than 3,000 patients who survived a critical illness and ICU stay. The analysis excluded patients who had suffered a trauma, such as a car crash, or brain injury, because those patients' cognitive and psychological outcomes can be affected by the injury itself, rather than the critical illness/ICU stay. Data revealed that the prevalence of PTSD in the studies ranged from 10 to 60 percent.
The research team also performed a meta-analysis of a subset of the 40 studies to obtain a more definitive estimate of PTSD prevalence. They selected six studies, with a total of about 450 patients, that used a PTSD measurement tool called the Impact of Event Scale between one and six months after ICU discharge. The data indicated that one in four patients had symptoms of PTSD. The researchers also reviewed studies that looked at patients seven to 12 months after an ICU stay and found that one in five patients had PTSD.
"These rates are as high as you might see in combat soldiers or rape victims," says Dale Needham, MD, a professor of medicine and of physical medicine and rehabilitation at Johns Hopkins University School of Medicine. "Our clinicians and patients should know that the high risk of PTSD exists among patients surviving critical illness."
The research team identified these common risk factors for PTSD: being diagnosed with a psychological problem (eg, anxiety or depression) before coming to the ICU; receiving large amounts of sedation medication while in the ICU; and having frightening memories of being in the ICU.
These symptoms occur across a wide variety of patients, regardless of their age, diagnosis, severity of illness or length of stay. "This tells us that if we focus on factors traditionally associated with worse physical outcomes, such as a patient's age, we may miss individuals with psychiatric symptoms," says Joe Bienvenu, MD, associate professor of psychiatry and behavioural sciences at Johns Hopkins.
The researchers also looked at the best ways to prevent PTSD. The solution that seemed most effective was an ICU diary, a notebook that allows clinicians and family members to write daily messages about what is happening to the patient.
At The Johns Hopkins Hospital, the medical ICU team will be implementing a quality improvement project that will include using an ICU diary as a tool to prevent PTSD and improve recovery. Relatively few institutions in the US utilise ICU diaries, but these are commonly used in Europe. Johns Hopkins plans to use them for patients entering the medical ICU and will further evaluate their effectiveness as a therapeutic tool.
Each year, more than 5 million people require ICU-level care in the United States and more than 750,000 Americans need mechanical ventilators. "It's clear that those who care for ICU patients need to be aware that there could be long-term consequences of critical illness and lifesaving treatments, including PTSD, which can significantly limit a patient's quality of life well after discharge," according to Ann Parker, a fellow in the Johns Hopkins Medicine Division of Pulmonary and Critical Care Medicine.
Source: Johns Hopkins Medicine
Image Credit: Flickr.com
Latest Articles
PTSD, ICU, Depression, anxiety, critical illness, traumatic
Post-traumatic stress disorder — often thought of as a symptom of warfare, major catastrophes and assault — can also affect patients who survive a crit...