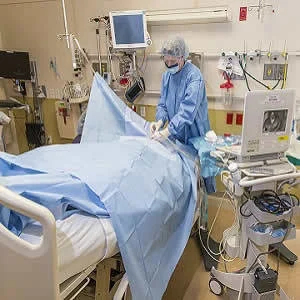
Critical care researchers from Intermountain Medical Center in Salt Lake City conducted a study with 616 patients treated for Acute Respiratory Distress Syndrome (ARDS), a progressive condition that often occurs in patients who are critically ill or who have significant trauma injuries . The aim of the study was to determine factors that played a significant role in their quality of life six months following discharge from the hospital. Results of the study are published in the online issue of Thorax.
Findings of the study showed that patient's acuity, or level of illness, was not a significant marker in their subsequent quality of life. It was actually lifestyle factors, specifically obesity and smoking that were associated with a worse quality of life rating.
A major complication often associated with ARDS is that fluid leaks into the lungs making it difficult for the patients to breathe. A large majority of people with ARDS are already hospitalised for trauma or illness and are unable to breathe on their own without a ventilator. Thus, improving the quality of life outcomes in such patients is a clinical and research priority, explains the study's principal investigator Samuel M. Brown, MD, MS, FASE, director of the Center for Humanizing Critical Care at Intermountain Medical Center.
"The ICU and the critical care environment are so focused on life-and-death issues, and we're so busy as clinicians, that we often don't have time to think about lifestyle factors, such as obesity and smoking and the role they play in our patient's long-term quality of life. Our study emphasises the need for us to do more of that," said Dr. Brown.
See also: ARDS Still Under-Recognised, Under-Treated
Study findings also suggest that smoking cessation education should be incorporated into the critical care setting and support for patients who survive ARDS should be improved.
In an email to ICU Management and Practice, Dr. Brown points out that many ARDS patients lose substantial weight, especially muscle, as part of their critical illness. Often, survivors are trying to recover their lean muscle mass. Dieting may not have the expected effect in ARDS survivors. It may be, however, that careful weight loss approaches a year after ARDS in patients with continued obesity could be of benefit. Those will need specific new research to know for sure.
When asked to describe the specific interventions that the research team planned to study for ARDS patients at risk of poor quality of life after discharge, Dr. Brown explained that their current interest was in trying to understand how to develop Aftercare and Recovery Clinics that improve outcomes for patients and families. Such clinics should likely include smoking cessation, psychological and social work support, medication reconciliation, monitoring for new complications, and physical rehabilitation. How best to build these clinics and what to include in them is an open research question. What’s already well proved is that many ARDS survivors suffer from Post Intensive Care Syndrome and substantial disability and frustration. Their needs are urgent.
Source: Intermountain Medical Center
Image Credit: Intermountain Medical Center
References:
Brown SM, Wilson E, Presson AP, Zhang C, Dinglas VD, Greene T, Hopkins RO, Needham DM; with the National Institutes of Health NHLBI ARDS Network (2016) Predictors of 6-month health utility outcomes in survivors of acute respiratory distress syndrome. Thorax, Jul 20. pii: thoraxjnl-2016-208560. doi: 10.1136/thoraxjnl-2016-208560.
Latest Articles
Acute Respiratory Distress Syndrome, ARDS, Quality of Life, lifestyle factors
Researchers from Intermountain Medical Center found that lifestyle factors, specifically obesity and smoking, were associated with a worse quality of life rating in patients treated for ARDS.