ICU Management & Practice, Volume 16 - Issue 3, 2016
A New Model for ICU Rehabilitation
It is now well established that many patients and caregivers suffer physical, psychological and social problems in the years and months following critical care discharge (Herridge et al. 2011). Similar to many centres, our intensive care unit (ICU) had no follow-up service available to support patients through this difficult recovery period (Griffiths et al. 2006). To understand how best to create a service that was safe, effective and person-centred, two members of our multidisciplinary team (MDT) undertook research programmes to help identify the problems that patients faced after ICU and to help understand the context for change (Quasim et al. 2015; McPeake et al. 2016).
From this work, four main challenges were identified:
- There is minimal evidence of
how and when rehabilitation services should be delivered (Mehlhorn et al.
2010), despite an abundance of literature describing the issues for ICU
survivors and their families.
- The hardships facing ICU
patients are often not apparent to hospital management. Readmissions to
hospital, increased general practitioner (family physician) visitations and
the increased reliance on welfare benefits are distributed amongst a variety
of budgets, which do not necessarily appear related to an ICU admission.
- Finding staff with the time
and ability to do something new that is different from their traditional ICU
role can be problematic.
- Finding physical space with a
suitable area to hold a rehabilitation programme can be difficult.
Patient-Focused Solutions
Simultaneously the team set up a Patient and Family Council (PFAC). The PFAC was a group of 10-12 previous patients and caregivers who met bimonthly for approximately two hours. This group, which was chaired by a patient or caregiver, helped create potential solutions to the problems encountered by ICU patients and their loved ones.
Utilising peer support as a central component for rehabilitation is gaining momentum within the ICU community (Mikkelsen et al. 2016). By bringing together a heterogeneous group of ICU survivors as part of our PFAC, the positive effect of peer support was obvious. Without exception, it was the first time that they had spoken to someone with a shared experience of the ICU.
What was also clear from this feedback was that their desire to get home did not live up to expectations. At around a month after hospital discharge, patients realised that their individual recovery was not what had been expected. It was also very clear that both patients and caregivers were frustrated that healthcare professionals and indeed the general public did not understand the difficulties in overcoming a critical illness. In attempting to move forward, the team were faced with the harsh reality that there is limited funding to establish a new service. Not unreasonably, most healthcare managers require evidence of benefit before there is financial investment.
In 2014 the Health Foundation, a UK charity, advertised a series of innovation grants, the Shine Awards. The team successfully applied for one of these awards. The advantage of this opportunity was that the MDT did not have to have the finished, polished intervention and thus were not limited to undertaking traditional research methodologies. This was a ‘learning’ grant, which allowed the team to develop a new service and change things after learning what worked and what didn’t.
See Also: PTSD Common in ICU Survivors
InS:PIRE
Utilising the first hand experience of our Patient and Family Council, the MDT co-created and developed the concept of InS:PIRE (Intensive Care Syndrome: Promoting Independence and Return to Employment). InS:PIRE is a five-week, peer-supported, self-management programme aimed at empowering patients and relatives to take control of their own health and wellbeing by finding community resources to help them. To ensure that we did not create a population of ‘chronic’ ICU patients, the course was kept deliberately short.
Every week there was a group exercise class to stimulate peer support. To encourage peer support further within the programme, InS:PIRE adopted patient and carer volunteer roles. These roles were undertaken by ICU survivors further along the recovery trajectory, who could offer hope and support to patients who were still struggling. To help encourage cross-communication we set up a café area; this allowed patients, staff and volunteers to intermingle in a relaxed setting.
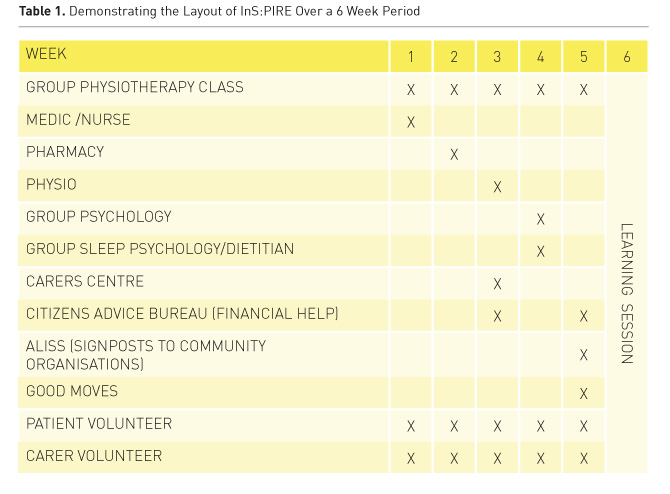
As well as the weekly physiotherapy class, patients and caregivers had individual and group sessions (Table 1). These included a physiotherapy consultation to discuss pain, musculoskeletal and balance issues. Patients were then given an individualised programme for their specific needs.
A pharmacy appointment was also provided to ensure that an appropriate medicines reconciliation had been undertaken. This was also the opportunity for the pharmacist to educate patients on what they were taking their medicines for and how to take them properly. If there were any issues, the pharmacist would write to the GP or use the National Patient Safety Foundation Framework Ask Me 3 (npsf. org/?page=askme3) document to empower patients to discuss their medication queries independently.
At a nursing and medical session, the patient was provided with a lay summary of their ICU stay if they wanted it and offered the opportunity to revisit the ICU. Personal goals were set with the patient and caregiver by asking simple questions such as “What can’t you do now that you could do before ICU?” or “What would you like to be doing in six months’ time?” Personal outcomes were often centred on issues such as driving, walking and using public transport independently. We would break these challenges into smaller tasks to make them more achievable.
A group psychology session explored ‘coping’ strategies. We also provided patients with information on how to seek further psychological support in the community if they felt this was necessary. We separated the patients from relatives during the psychology sessions as our PFAC felt this was important. This is also reflected within the literature, which demonstrates the challenges which caregivers face during critical care recovery (Haines et al. 2015). During the psychology session, patients were able to ‘normalise’ their feelings and express their concerns without causing more anxiety for their relatives. For the carers, it was a chance for them to offload exhaustion, anger and frustration without feeling guilty. This process appeared to offer this group an enormous sense of relief.
The fifth and final week of InS:PIRE was named the social prescription week. This session signposted participants to community organisations which might help their recovery. For example, we looked at volunteering options as a platform to return to work, community physiotherapy classes or places that can help with welfare issues. A fundamental aim of InS:PIRE was to provide patients with the tools to take control of their own health by using existing community resources. Unless absolutely necessary, patients were not referred back into the hospital setting.
A vital part of this initial pilot of InS:PIRE was the ‘learning week’, which included a meeting of the entire health and social care team involved in the delivery of InS:PIRE. From this we could find out from patients, staff and the volunteers what worked, what didn’t and what we needed to change. An example of this learning was in our first cohort where attendance was initially low. We had phoned patients a few days in advance to ask if they were attending the clinic, but then often they didn’t attend. When they were contacted to ask why, it was because they didn’t realise what day of the week it was. This is consistent with many of the well-documented ongoing cognitive problems which patients encounter following critical care discharge (Iwashyna et al. 2010). By contacting patients on the morning of the clinic, attendance doubled. We also realised that there was a risk of patients becoming dependent on individual members of the team. As a result of this learning, a generic email account and phone number was created and utilised for all patient interactions.
Learning from InS:PIRE
The positive difference in
patients that the team witnessed between the first and final week of InS:PIRE
was overwhelming. What was unexpected was the effect InS:PIRE had on the staff
attending the clinic. Staff who had been in the same job for decades were
expanding their role and working in a different way; they weren’t defined by
the role they had trained in.
For patients the biggest issues which were identified
and supported during the programme were social: housing; finances;
relationships and employment. The skills needed to support these issues were
very different from the traditional skill base of critical care practitioners.
Cross-boundary working became essential as well as developing new skills for
the team involved.

A strong theme which continued
over the year from the patients who attended InS:PIRE was “Why does no-one
know how difficult it is for ICU patients who survive?” The term ‘Post Intensive
Care Syndrome (PICS) may appear to be labelling patients. However, in our
experience patients and caregivers valued this terminology. Many patients
felt it ‘legitimised’ their feelings and experiences after ICU and helped validate
their concerns.
The Future
The team recognised that to help patients have their voice heard and to highlight InS:PIRE in the hope of securing further funding, we had to publicise and disseminate learning as widely as possible. We were extremely proud and indeed grateful to have been awarded the BMJ 2016 ‘Innovation into Practice’ award. It allowed InS:PIRE to be in the public domain at a very early stage.
InS:PIRE was co-produced with patients for patients. Whilst the programme works in one population, it needs to be evaluated in other sites to understand if this model is safe and effective at a larger scale. The InS:PIRE team has recently been successful in obtaining further funding from the Health Foundation to ‘Scale and Spread’ the InS:PIRE model of care. Over the next six months, InS:PIRE will be implemented in four other health boards in Scotland. The aim of this programme of research will be to understand the impact of InS:PIRE for patients on a larger scale. It will also seek to understand how this complex intervention can be implemented more widely.
A five-week cohort of InS:PIRE (including a funded learning session) for 12 patients and their carers costs approximately £9000. Our aim is for InS:PIRE to become an established clinical service. This will not be without challenges. We have funding for the life of the aforementioned Health Foundation grant and we will be engaging with our executive board to secure future finance. We are currently developing a full economic evaluation of the project to examine cost-effectiveness and help build a strong business case.
Conclusion
Patients and caregivers face many challenges in the months and years following critical care discharge. The peer-supported model of InS:PIRE appears to have some utility in supporting this patient group. Future evaluation on a larger scale is imminent and will hopefully support the development of reliable evidence to support this group of patients.

Abbreviations
EN enteral nutrition
ICU intensive care unit
ICU-AW ICU-acquired weakness
MPB muscle protein breakdown
MPS muscle protein synthesis
PN parenteral nutrition
References:
Griffiths JA, Barber VS, Cutherbertson BH et al. (2006) A national survey of intensive care follow up clinics. Anesthesia, 61(10): 950-5.
PubMed ↗
Haines KJ, Denehy L, Skinner EH et al. (2015) Psychosocial outcomes in informal caregivers of the critically ill: A systematic review. Crit Care Med, 43(5):1112-20.
PubMed ↗
Iwashyna TJ, Ely EW, Smith DM et al. (2010) Long term cognitive impairment and functional disability among survivors of severe sepsis. JAMA, 304(16):1787-1794.
PubMed ↗
McPeake JM, Forrest E, Quasim T et al. (2015) The health and social consequences of an alcohol related admission to critical care: a qualitative study. BMJ Open, 6: e009944.
Article ↗
Mehlhorn J, Freytag A, Schmidt K et al. (2014) Rehabilitation interventions for post intensive care syndrome: a systematic review. Crit Care Med, 2(5): 1263-71.
PubMed ↗
Mikkelsen ME, Jackson C, Hopkins RO et al. (2016) Peer support as a novel strategy to mitigate post intensive care syndrome. AACN Adv Crit Care, 27(2): 221-9.
PubMed ↗
Quasim T, Brown J, Kinsella J (2015) Employment, social dependency and return to work after intensive care. JICS, 16(1): 31-6.
Article ↗








