ICU Management & Practice, Volume 17 - Issue 2, 2017
Patient-centered care is becoming a major topic in healthcare. Many initiatives have begun focusing their care around patients and their medical conditions. This requires focusing on patient value (Porter and Teisberg 2006). When focusing on value for patients, a few challenges may arise. Firstly, the meaning of value for patients varies widely among stakeholders in healthcare. Secondly, not all patients receive the same treatment for the same illness. Patients (and their families) want to be treated differently based on their preferences. Thirdly, the quality of care delivery in terms of patient relevant outcomes differs among hospitals. The diversity in measurements makes it difficult to compare.
I. Patient Value: A Common Definition
Doctors would base the meaning of patient value on the skills of a doctor, an improved medical lab result, or a well-performed surgery. These measurements are mainly based on the treatment or intervention perspective. On the other hand, a patient may base patient value on aspects such as the length of waiting lists, how kind the doctor was or perhaps how good the coffee or breakfast tasted. "Most people would agree that both sets of measurements do not truly reflect the quality of care from a medical perspective. Patients' perception: "They were so kind to me when performing the surgery seven times.
II. A Singular Language
Value-based healthcare provides a singular language that is comprehended by doctors, medical teams, patients and their families. Patient value is defined by an equation whereby patient-relevant outcome measurements are the numerator, and costs per patient in delivering those outcomes are the denominator. Patient value is defined for a specific medical condition over the full cycle of care (Figure 1).

Meetbaar Beter (winner of the VBHC Prize 2014) is a great example that transparently reports patient relevant outcome measurements for specific medical conditions. They include coronary artery disease, atrial fibrillation, aortic valve disease and combined aortic valve disease and coronary artery disease (Meetbaar Beter 2012-2016). It is important to note that outcome measurements should be defined around a medical condition and should be manageable and actionable. Doctors and their teams are then intrinsically motivated to improve the quality of care they deliver to patients. All they need are the tools to measure and the ability to visualise accurate and valuable outcomes.
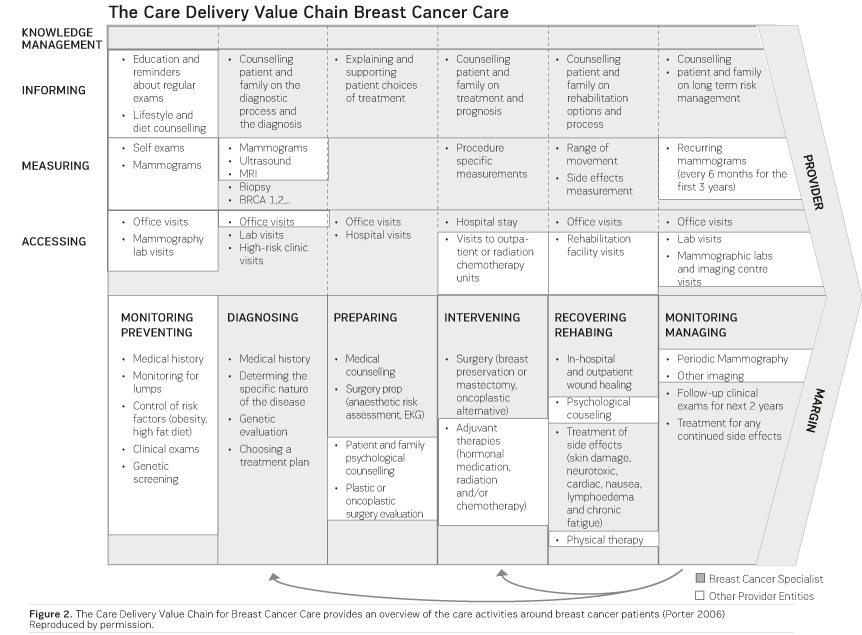
III. Focused on Measurable Health Outcomes To Facilitate Improvement
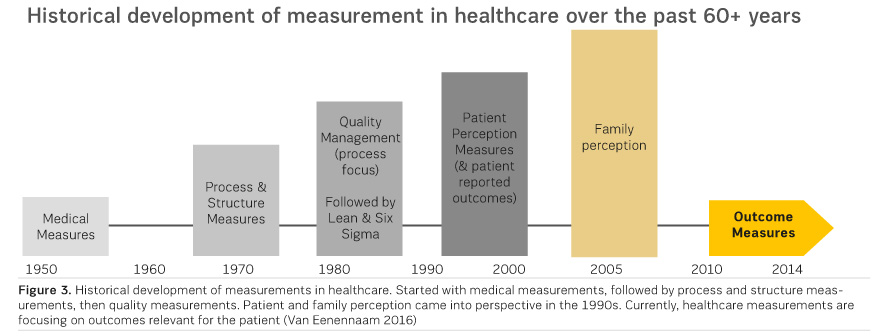
Measuring outcomes in healthcare began in the 1950s (Figure 3), followed by a strong trend towards process and structure measurements. Some of the measurements focused on at that time were the length of waiting lists and the number of (certified) staff. This led to quality management based on the optimisation of processes, including Lean. All of these measurements are important in improving the internal process of care delivery. Patient and family perception only became important from a measurement perspective in the 1990s. Surprisingly, the healthcare sector took quite some time in realising the significance of patients in healthcare delivery. Luckily, healthcare providers are now able to present true patient-relevant outcome measurements to their colleagues and patients.
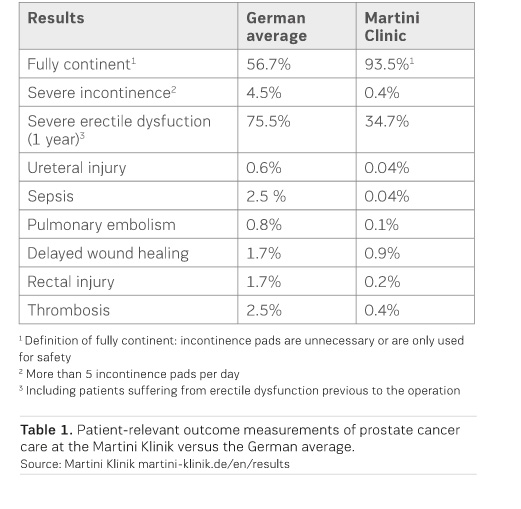
One of the most inspiring examples of improving measurable health outcomes is the Martini Klinik at the University Hospital Hamburg-Eppendorf (UKE) in Germany. Since the founding of the clinic in 2005, the Martini Klinik has focused on improving long-term health outcomes for patients with prostate cancer. The Martini Klinik massively improved their care by measuring patient-relevant outcomes (Table 1). The improved outcomes led to growth in volume and the Martini Klinik became the world’s largest prostate cancer care clinic by 2013. It later received the VBHC European Inspirational Award in 2016 based on these inspiring results.
A second example is Meetbaar Beter. Meetbaar Beter has helped doctors learn from one another and improve care delivery based on reported outcomes. Over the last few years, impressive effects on patient-relevant outcomes have been achieved by looking at and learning from fellow cardiologists and cardiovascular surgeons.
See Also: Vulnerability Leading to Improvement: Hospitals Start Comparing Outcomes Internationally
IV. Protocols Do Not Fit Every Patient, But Patients Benefit From Protocols
Every patient is unique but they each walk a different path through the cycle of care. Protocols are very useful as they provide care delivery guidelines for patients with common medical conditions. In the St. Antonius hospital (winner of ‘VBHC Cost-Effectiveness Award’ 2016), elderly patients with end-stage renal failure are guided towards their choice of treatment. Previously, protocols stated that patients with this medical condition should primarily be treated with dialysis. Dialysis is highly invasive (and costly) for elderly patients and it requires them to remain in hospital for long periods of time. Research made by Dr. Willem Jan Bos and his team found that conservative treatment is much better than dialysis (Verberne et al. 2016). By having discussions with patients, protocols can be changed and care delivery can be opitmised and adjusted to fit every individual.
V. Become a Patient-Centred, Fast-Learning Team
Value-based healthcare is centred around learning. Doctors who have a drive to show medical leadership and create a learning culture are key for the implementation of VBHC. Learning to improve value for patients provides satisfaction. This motivates doctors and their teams and also cuts costs. VBHC empowers doctors and their teams to do what they do best—provide excellent patient-value by using clinically relevant and evidence based insights.
Creating Excellent Patient Value
- Patient-centred care is on the rise;
- VBHC provides a common definition for patient-value and a common language for all stakeholders in healthcare;
- VBHC puts the patients, their families, doctors and their teams at focus;
- Patients with similar medical conditions have different preferences and they each follow roughly similar care-paths;
- Care quality improves by measuring the right patient relevant outcome measures. This creates compelling learning cycles for the medical team.
Working towards excellent patient-value has never been more optimistic than it is today!
Value-Based Health Care Center Europe is the European platform for VBHC implementation since 2012. With over 1000 members in the community, VBHC Center Europe facilitates people with an interest in VBHC to connect, create and share VBHC best practices. Additionally, since 2014, VBHC Center Europe annually awards the VBHC Prize. More information: www.vbhc.eu.
References:
Martini Klinik (2014) Facts count: unique data on the success of our therapies. [Accessed: 24 January 2017] Available from martini-klinik.de/en/results
Meetbaar Beter Boek (2012-2016) [Accessed: 6 February 2017] Available from: meetbaarbeter.com/documents/meetbaar-beter-boeken
Porter ME, Teisberg EO (2006) Redefining health care, 2006. Boston, MA: Harvard Business School Press.
Porter ME (2006) Value based competition in health care [presentation]. [Accessed 24 January 2017] Available from
hbs.edu/faculty/Publication%20Files/20061020_MayoPresentation_e10acf3c-846b-4d39-9c8b-88f01c1be0f1.pdf
Porter ME (2010) What is value in health care? N Engl J Med, 363(26): 2477-81.
Value-Based Health Care Europe (2016) Harvard Prof. Porter on value-based health care in the Netherlands. [Accessed: 10 February 2017] Available from youtube.com/watch?v=36ZH1gxq8XQ
Van Eenennaam F (2016) Value-based health care in Europe. What’s next? [presentation]. Leadership and Management in Cardiovascular Medicine Forum, 16-18 June, Vienna. [Accessed: 6 February 2017] Available from lmcforum.org/wp-content/uploads/2016/09/VanEenennaam-Fred_Value_based-healthcare-in-europe_what-is-next.pdf
Verberne WR, Geers AB, Jellema WT et al. (2016) Comparative survival among older adults with advanced kidney disease managed conservatively versus with dialysis, Clin J Am Soc Nephrol, 11(4): 633-40.









