HealthManagement, Volume 16 - Issue 3, 2016
The Radiologist’s View
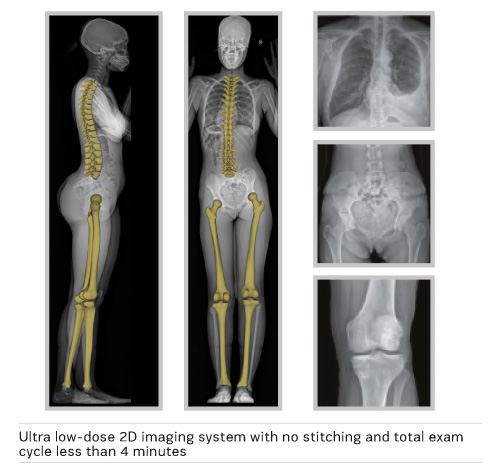
The Hospital for Special Surgery (HSS) acquired the EOS ® imaging system because the technology gives us biplanar capability with a single exam, with no distortion in the image and most importantly, it is low-dose. Our orthopaedic surgeons wanted to reduce radiation dose for their patients, particularly the pediatric patients who need repeated x-rays for limb-length discrepancies or for scoliosis. Previously, in order to get a long field of view of the patient, such as the pelvis to the ankles or from the skull to the pelvis, you would have to take two different exposures from the anteroposterior (AP) or frontal view, and another two from the lateral or side view. Both images of each view then had to be digitally stitched together. Sometimes there was poor stitching so you would not get an accurate image length. EOS ® vertically scans the desired length and has the ability to image from head to toe in one exam. Moreover, the system has two detectors and two tubes so you can get both the frontal and lateral views in one shot, greatly reducing the time required for a full exam.
We have a lot of potential users wanting access to this technology
With EOS ®, in addition to getting a longer field of view and simultaneous frontal and lateral acquisitions, we have the ability to image patients in functional positions either standing or sitting. With this, we can see how a patient’s lower limbs (hips, knees) are positioned and aligned when standing and how this changes when seated. We acquired this technology originally for our pediatric patients. It quickly became very popular with orthopaedic surgeons, because they realized how important it was for all patient groups – adults with scoliosis, limb length discrepancies, etc. We have a lot of potential users wanting access to this technology.
3D Modelling
Once the biplanar images, frontal and lateral, are acquired simultaneously, and since the system is pre-calibrated, the sterEOS workstation can be used to build a personalized 3D model of the patient’s lower limbs or spine. These models are accompanied by automatically calculated 3D measurements of the patient’s anatomy, all from a single pair of lowdose radiographs.
Joint Replacement Research
We are using this technology for research with Dr. David Mayman on total hip and knee replacements (Carroll et al. 2016; Esposito et al. 2016a; 2016b). For example, we want to find out what the anatomy is beforehand, and discover why some patients dislocate following hip surgery. That may be a function of how the pelvis orientation changes between sitting and standing, and EOS ® lets us see this. The relationship of the patient’s spine to their pelvis is something people have been looking at for years, but it’s been difficult to research, especially in 3D, until now with EOS ®. This system gives us that ability to look at the entire spine and the lower extremities from front and side in a single exposure. It allows us to see the relationship between the spine and pelvis changes between standing and sitting, and that’s very important. We were not able to do this very well with conventional x-rays. EOS ® opens up a whole new area not just for patient care, but research as well.
Conclusion
EOS ® is a tool that is especially adapted to long-axis imaging in weight-bearing, functional positions (standing, sitting), for children (scoliosis, leg lengths) as much as for adults (scoliosis, leg lengths, joint replacement). Scans with EOS ® are quicker and more accurate than doing the traditional radiograph stitching, and the fact that you get a frontal and a lateral view with a single exposure also gives a considerable time advantage. It has improved our patient care and opened up an important area of research.
The Orthopaedic Surgeon’s View
The EOS ® orthopaedic imaging device uses lowdose, biplanar radiographs to capture full body, lower extremity or spine images without stitching or vertical distortion. Furthermore, it provides images in functional positions.
EOS ® replaces standard preoperative radiographs, and at the Hospital for Special Surgery (HSS), we have found EOS ® to be extremely accurate in predicting component positioning when compared to computed tomography (CT).
I have been using EOS ® for the past two and a half years. I use it for all preoperative templating for total hip and total knee arthroplasty to predict intraoperative implant sizes and component positions. The corrected image magnification results in more accurate templating than traditional radiographs. In the case of total hip arthroplasty, EOS ® is very userfriendly and accurate with excellent inter-observer agreement.
EOS® should become the preoperative imaging standard of care for arthroplasty patients
The ability to use hipEOS, the 3D pre-operative surgical planning software, for patients with increased native version has been very helpful. In certain cases, after preoperative planning with hipEOS , I have changed my plan and used different components. The 3D models allow us to gain more knowledge preoperatively to save intraoperative time. This has enabled me to be more efficient in the operating room and decrease the time spent requesting different implant sizes.
The technology has changed my practice. I have been able to decrease radiation exposure to my patients and decrease the number of radiographs that are required for surgery.
Value of 3D
Especially when combined with hipEOS ,3D models can be used to create a patient-specific plan where the surgeon is able to visualize and manipulate various implants. This is not possible with standard radiographs or even 2D EOS images. The 3D models allow us to see rotation of the femur and to identify patients with varying offset and neck anteversion that may change our preoperative planning. Most commonly, patients with arthritic hips stand with their femur externally rotated, which makes it very difficult to template. However, the 3D capabilities of hipEOS takes this into account.
We can now accurately measure component position in two planes such that we can consider flexion contractures at the knee or pelvic tilt at the hip. Additionally, this allows us to measure implant position in functional positions such as standing and sitting. The ability to evaluate standing/sitting and spine radiographs with one low-dose 2D-3D system provides additional information that will help us determine which patients may be at high risk for dislocation. Absence of variation in pelvic tilt between standing and sitting positions reduces posterior acetabular coverage, which may put patients at higher risk of dislocation in the sitting position. The ability to identify these patients and plan accordingly will provide better patient outcomes.
Benefits for Pediatric, Arthroplasty, and Spine Patients
The HSS acquired the EOS ® system originally for pediatrics. However, we found it to be extremely useful in arthroplasty, and we acquired two additional units for adult and spine patients.
EOS ® has been a valuable tool for our surgical cases and for the patient, it provides an alternative to standard imaging with less radiation exposure. In difficult cases, the 3D model EOS provides us to plan specifics such as leg-length and version that radiographs are unable to do.
EOS ® should become the preoperative imaging standard of care for arthroplasty patients to decrease radiation exposure and provide a patient-specific, 3D model of each patient so that their surgery is planned based on their individual anatomy.

References:
Carroll K, Esposito C, Miller T, Lipman J, Padgett DE, Jerabek SA, Mayman DJ (2016) Accuracy of measuring combined anteversion in total hip arthroplasty using EOS(r) Imaging. Orthopaedic Proceedings, 98-B (Suppl 7): 129.
Esposito CI, Miller TT, Kim HJ, Barlow BT, Wright TM, Padgett DE, Jerabek SA, Mayman DJ (2016a) Does degenerative lumbar spine disease influence femoroacetabular flexion in patients undergoing total hip arthroplasty? Clin Orthop Relat Res, 474(8): 1788-97. doi: 10.1007/s11999-016-4787-2.
Epub 2016 Mar 28. Esposito C, Miller T, Kim HJ, Mayman DJ, Jerabek SA (2016b) Functional acetabular component position in total hip replacement patients during standing and sitting using EOS Imaging. Orthopaedic Proceedings, 98-B (Suppl 1): 126..



