HealthManagement, Volume 20 - Issue 10, 2020
An overview of a developmental model the authors have been working on for the past two years with a focus on chronic disease management and support for patients who are labile or highly reactive to changes in their
environmental conditions.
Key Points
- Global healthcare systems are struggling to manage the growth in chronic diseases.
- Several countries have identified that as many as half their populations may now be living with a long-term health condition for which there is no current cure.
- Respiratory conditions, such as COPD, have a significant impact on individuals including both their physical and psychological health status
- AI applications can play a role in supporting patients with chronic disease.
Introduction
Health systems globally are struggling to manage the growth in chronic diseases. Many low to middle income countries, in addition to wealthier countries, are now dealing with rising prevalence rates for heart, lung, cancers and metabolic disorders (Aikens et al. 2010; Bowry et al. 2015). Indeed, several countries have identified that as many as half of their populations may now be living with a long-term health condition for which there is no current cure. The impact of COVID-19 in 2020 also indicates that not only are such people at greater risk of death but also that COVID-19 survivors may experience long-term health impacts that complicate their lifetime health trajectories. This intersectional epidemiology indicates that health system responses will need to be highly adaptable in the coming decades if all of these complicated factors are to be managed appropriately and sustainably.
Recent developments have indicated that such flexibilities in healthcare are viable but the evidence base for longer term success remains limited. One of the emergent domains offering some evidence for sustainable response includes the growth in ‘virtual’ healthcare associated with expanded telehealth models for health monitoring and response in the community. The expansion in virtual health options has been greatly enhanced by the growth in digital technologies more generally (including the potential of 5G) and in digital health-specific technologies in particular. One of these domains is growth in the development and application of Artificial Intelligence (AI) options. This is a complicated area of practice with advances in some sectors, such as scanning analysis with Machine Learning (ML) moving faster than others. However, the indicators are that as AI options continue to prove their value in some specific clinical domains, that more general applications will be increasingly introduced to deal with emerging complexities and to enhance systemic capabilities.
In this piece we explore a developmental model the authors have been working on for the past two years with a focus on chronic disease management and support for patients who are labile or highly reactive to changes in their environmental conditions. The reason for this is that labile patients may deteriorate faster and require more immediate care and support than those whose conditions are stable and more manageable by conventional models of care. The role that various AI applications can potentially play in supporting these patients, and their associated health system touch points is the focus of this piece.
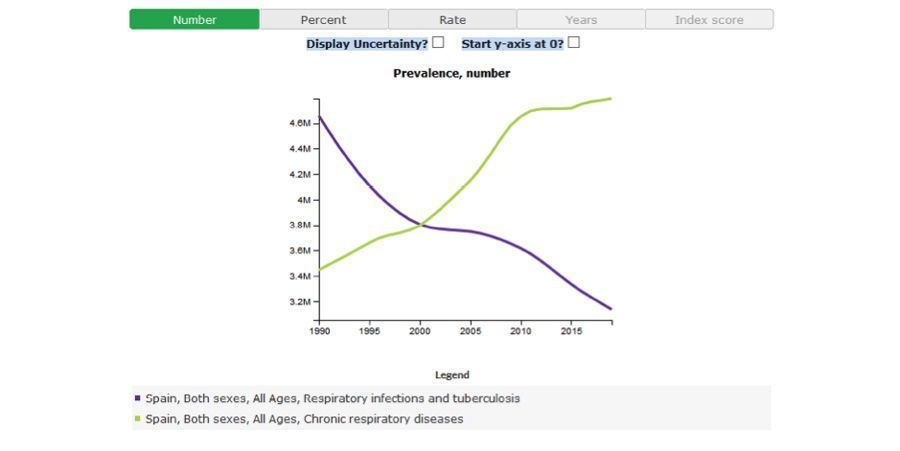
Chronic Diseases in Europe
The WHO has for some time now identified the growing problem presented by chronic diseases associated not only with factors like population ageing but also ambient and domestic air pollution and other urban-intensive health risks (Busse et al. 2010). This is an increasingly global concern but here we focus on the general European context and then on Spain in particular. This is because Europe’s population, including Spain’s, is ageing and infectious disease rates have been declining, with chronic conditions representing the major burden of disease.
Average Spanish Life Expectancy (LE) was recently ranked as number three in the world (WHO 2018). In addition, non-communicable diseases now represent the greatest burden of morbidity and mortality (Sorianao et al. 2016).
The sub-set of respiratory conditions including chronic obstructive pulmonary disease (COPD) and upper and lower respiratory tract infections are a significant contributor to the Spanish burden of disease.
The Global Burden of Disease (GBD) Study data indicates that respiratory disease remains a significant health issue in Spain. While respiratory infections have declined significantly since 1990, nonetheless more than 3 million in a population of 47 million (2020 estimate) are affected. In contrast, chronic respiratory diseases are continuing to climb over the same period with almost 4.8 million people estimated to be living with these conditions (GBD 2020).
The Concept
GeoAI refers to the intersection of conventional AI methods and the vast array of spatially enabled technologies available, including both software and hardware, such as geographic information systems (GIS), LIDAR, GPS, RFID, digital sensor systems and so on. The rise of digitisation has seen a growing integration of spatial technology with other forms of digital technologies such that most handheld devices can now generate and utilise spatial data including mobile phones, tablets, laptops and specialist devices.
When we consider the growth in personal health technologies (wearables) that monitor one or more physical and physiological factors (blood pressure etc.), then we can see how conventional AI and emerging spatial technologies have the capability of greatly improving care in the community and also care between specialist services and patients living in their own homes. This is because all digital data can be effectively spatialised and personalised to allow the geographic location of labile patients and the monitoring and reporting of environmental risk factors (e.g. pollution spikes, forest/bush fires, and even allergens such as grain shipments).
A next step in this integrated domain is the application of AI applications like chatbots which, as they become increasingly sophisticated, can help individuals not only manage their own health but work collaboratively with health service providers and people with the same health condition to maximise their safety and wellbeing. The addition of chatbot data, which patients provide to healthcare providers and even each other as a form of mutual support, can be collected and integrated to model risk factors in real-time, inform systemic responses and support patients in situ. This data integration concept sits at the centre of this discussion because we believe this is where some key value lies in the AI equation, and especially so in a spatially enabled or GeoAI strategy.

The target audience for this concept is respiratory patients whose conditions are labile, or especially responsive to environmental changes rather than those with clinically stable conditions. This is important because there is evidence for natural events having a sudden and significant effects on community-dwelling patients which then lead to sudden demand spikes at hospitals and potential impacts on surge capabilities, workforce availability and even patient and community communication outcomes. The 2016 Melbourne, Australia thunderstorm asthma event created unprecedented havoc and associated communication failures which a subsequent inquiry showed could have been much better managed (Lee et al. 2017; Thien et al. 2018).
Contemporary research indicates that chatbots and associated techniques have substantial potential in, for example, self-management healthcare scenarios (Fernández-Avelino et al. 2021). A key issue here is that AI-based conversational technologies, such as chatbots, can be integrated with spatial technologies to provide an ongoing monitoring process that not only supports patients but also helps connect healthcare service providers likely to be impacted by changes in patient acuity and, therefore, service demand. This could include unplanned calls to specialists, to general practitioners/family doctors, to pharmacists supplying their medications, allied health service providers and, ultimately, emergency services who might be called out to take acutely unwell patients to hospital. The better informed these various services are about the status of such labile patients, the greater their capacity to plan ahead and anticipate spikes in demand by patient type, location, condition and acuity.
The Aqurate Model
Our Aqurate model aims to apply these new conversational technologies, integrated into a GIS platform, as a potential source of patients’ information to simulate what could happen from the development of an integrated AI-GIS-provider-patient platform and the potential impact it can have on patients living with respiratory diseases in urban agglomerations. This integration includes the analysis of natural language data collected via chatbot conversational technologies to build a responsive system that accommodates both conventional quantitative data measures (e.g. in-home sensors and monitors) and the subjective experiences of individual patients whose conditions are labile or highly reactive to changes in environmental conditions. In other words, the individual patient’s self-assessment is readily integrated into the diagnostic and response scenario. This can be especially important for patients living with multiple chronic health conditions since, as we know, co-morbidity and multi-morbidity rates are rising globally (King et al. 2018; Singer et al. 2019).
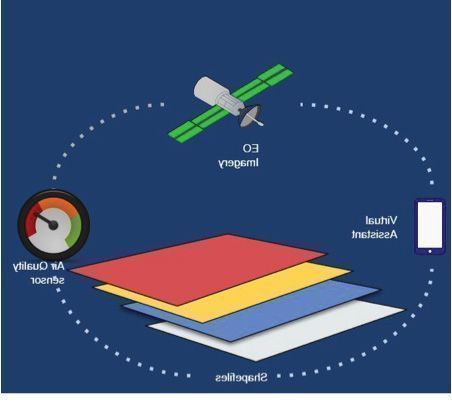
The illustrations outline the basic concept we have developed. This includes the capacity for patients to self-report their situation, including changing symptoms experienced over time, and the integration of that data from remote sensing technologies (such as satellites monitoring weather or wildfires), environmental sensors (such as traffic related air pollution in urban areas), landscape data (altitude, vegetation cover etc.), and relevant infrastructure data including traffic monitoring and health service locations (hospitals, pharmacies, ambulance stations etc.).
The key issue here is that all of this data is fully digital and hence it can be automatically geocoded using the geographic information system (GIS) software and integrated with any associated analytics and visual dashboards. With patient approvals in place, individuals and their reported data could be either shown directly on the dashboard maps or key data anonymised but stamped with date, time and small area geography to illustrate trends in factors affecting the clinical status of the patients. This would help to track the degree of localisation of a patient or patients’ situation or identify trends across larger geographic areas.
Industry Applications
The synergies that could be generated between the academic, corporate and medical-scientific world, The University of Technology Sydney and the Clínica de Navarra will generate potentially positive feedback at all levels, from commercial and corporate, to research and CSR strategies.
In addition, another important aspect is the design, development and integration of the platform in a 5G network. Speed, capacity and flexibility of a 5G network will be especially important for the development of the tool.
Aspects such as the integration and optimisation of the tool in a 5G network will be a key factor for the project’s development.
Therefore, the project will ultimately aim to create a tool optimised for a 5G network that synthesises, standardises and ultimately simplifies the analysis process in which they may be interested from corporate sectors linked to academia and research, the healthcare industry, and finally the public sector.
The applications derived from the development of the tool and in order to optimise its output to the market will focus on three different areas of development depending on their applications.
Hence, we are proposing our partners the development of an agreement focused on a longer-term strategy with financial benefits to come at a later date. A concern/goal would make sense at this initial stage.
The purpose would ultimately be to focus on an innovation that can be implemented in the medium-long term, with the necessary resources and always focused on developing a prototype in a flexible and collaborative framework by all parties in relation to patents and IPRs.
Applications
Healthcare sector:
• Hospitals and patient services.
Spatial distribution of pollutants and risk areas for patients.
• Warning information system for patients as well as for practitioners who want to be informed of the evolution and scope of any pollution event
• Study of distribution of patients by specialty.
Sports-Outdoors:
• Mapping Outdoor Sports Suitability:
Development of an alert system on the suitability of locations for performing outdoor sports (Running/Cycling).
• As the topographic profile of the race, an information system based on isolines that inform the max recommended time of exposure to pollutants while running or cycling could be valuable in terms of practical information to the users.
Defence:
• Spatial distribution modelling of chemical-warfare agents from unconventional weapons.
• Perimeter protection system of chemical-warfare attacks in temporary mission military settlements.
Public Government:
Development of applications to support public health services in different areas from patient care through a system that allows access to relevant information e.g. pollution data, to information and control service for a hospital network. The objective is to facilitate the management of information for patients of public services as well as the connection with the network of hospital services.
• Transport:
• Infrastructure management in extreme climatic events and natural disasters (e.g. Volcanic Ash, Smoke Plumes, Mineral Dust).
• Harbours and Ports management (e.g. Soybean unloading and incidence of asthma cases).
• Public Healthcare system:
• Optimisation of public hospitals and patient services costs.
• Risk zone mapping for urban outdoor activities and sports.
• Aerosols: Particulate matter spatial distribution.
Conclusion
Respiratory conditions, such as COPD, have a significant impact on individuals including both their physical and psychological health status (e.g. Smith et al. 2014). There is evidence that they are also at higher risk of some other health conditions and, since the advent of the COVID-19 pandemic, these risks have only increased (Leung et al, 2020). Maintaining the health and safety of people with chronic disease is more important than never and this model identifies an approach with considerable potential in this space. Indeed, the upswing in telehealth and related virtual initiatives under COVID-19 only reinforces the basic concept presented here. An additional benefit may be the further customisation of services and support for particular patients (respiratory and others) becomes increasingly viable through the Aqurate modelling approach.
This article outlines a model for improving patient and health using an integrated set of digital technologies. The case study scenario of respiratory disease is illustrative of the complexities associated with chronic disease more generally and, more specifically, the growing problem of multimorbidity. The growing demand for patient self-monitoring and management relies on an expanded and better integrated use of digital technologies that link patients and providers more effectively. Lastly, patients and providers inhabit particular places where conditions may vary across space and over time. This model shows how both the general problems associated with rising chronic disease and the specific problems of distinct urban areas can be effectively managed within the one conceptual and technological framework.
References:
Aikins ADG, Unwin N, Agyemang C, Allotey P, Campbell C, Arhinful D (2010) Tackling Africa’s chronic disease burden: from the local to the global. Globalization and health, 6(1), 1-7.
Bowry AD, Lewey J, Dugani SB, Choudhry NK (2015) The burden of cardiovascular disease in low-and middle-income countries: epidemiology and management. Canadian Journal of Cardiology, 31(9), 1151-1159.
Busse R, Blümel M, Scheller-Kreinsen D, Zentner A (2010) Tackling Chronic Disease in Europe: strategies, interventions and challenges (No. 20). WHO Regional Office Europe.
Fernández-Avelino J, Alor-Hernández G, Paredes-Valverde MA, Sánchez-Morales LN (2021) Developing Chatbots for Supporting Health Self-Management. In Handbook of Research on Natural Language Processing and Smart Service Systems (pp. 135-156). IGI Global.
King DE, Xiang J, Pilkerton CS (2018) Multimorbidity trends in United States adults, 1988–2014. The Journal of the American Board of Family Medicine, 31(4), 503-513.
Lee J, Kronborg C, O’Hehir RE, Hew M (2017) Who’s at risk of thunderstorm asthma? The ryegrass pollen trifecta and lessons learnt from the Melbourne thunderstorm epidemic. Respiratory medicine, 132, 146-148.
Leung JM, Niikura M, Yang CWT, Sin DD (2020) COVID-19 and COPD. European Respiratory Journal, 56(2).
Singer L, Green M, Rowe F, Ben-Shlomo Y, Kulu H, Morrissey K (2019) Trends in multimorbidity, complex multimorbidity and multiple functional limitations in the ageing population of England, 2002–2015. Journal of comorbidity, 9, 2235042X19872030.
Smith MC, Wrobel JP (2014) Epidemiology and clinical impact of major comorbidities in patients with COPD. International journal of chronic obstructive pulmonary disease, 9, 871.
Soriano JB, Rojas-Rueda D, Alonso J, Antó JM, Cardona PJ, Fernández E, Lazarus JV (2018) The burden of disease in Spain: Results from the Global Burden of Disease 2016. Medicina Clínica (English Edition), 151(5), 171-190.
Thien F, Beggs PJ, Csutoros D et al. (2018) The Melbourne epidemic thunderstorm asthma event 2016: an investigation of environmental triggers, effect on health services, and patient risk factors. The Lancet Planetary Health, 2(6), e255-e263.





