Over the past several decades there have been significant and important improvements in the care of patients diagnosed with cancer, and there are currently an estimated 14.5 million survivors of cancer in the U.S., or approximately 4.5% of the total population (DeSantis et al. 2014). One unintended consequence of this success is a growing population of patients with cancer treatment-related cardiovascular toxicity (CTCT). Survivors are at increased risk for cardiovascular complications, including heart failure, myocardial ischaemia, valvular disease, pericardial disease, hypertension, arrhythmias and thromboembolism (Yeh and Bickford 2009; Mulrooney et al. 2009), with up to 50% of disease being asymptomatic (Carver et al. 2013). The leading cause of both morbidity and mortality in survivors of many cancers is cardiovascular disease; for example, childhood and young adult cancer survivors are 5-6 times more likely than sibling controls to develop cardiovascular sequelae (Mulrooney et al. 2009).
To meet the growing needs of the population of cancer survivors with CTCT, a number of cardio-oncology (or onco-cardiology) programmes have emerged at tertiary and quaternary hospitals in the U.S. and Europe. In addition, national and international organisations have established dedicated groups to address all facets of cardio-oncology, one of the most recent being the Cardio-Oncology Member Section of the
American College of Cardiology (ACC), intended as a home for healthcare providers and researchers interested in cardio-oncology within one of the leading cardiology organising bodies worldwide. The overarching goal of these various programmes and organisations is to advance patient care in cardio-oncology by meeting the professional need in clinical guidance and training, advancing education, research and advocacy (Barac et al. 2015).
Comprehensive Cardiac Care Throughout Treatment
The first evidence for CTCT became apparent shortly after introduction of anthracycline chemotherapy in the late 1960s, with invasive and noninvasive evidence for cardiac injury and dysfunction clearly demonstrated in the mid-1970s (Rinehart et al. 1974; Bristow et al. 1978). Early efforts focused on management of symptomatic heart failure in survivors, but that shortly shifted to prevention. The current model for comprehensive cardio-oncology care begins with cancer and cardiovascular screening before any diagnosis is made, and continues through long-term survivorship (see Figure 1).
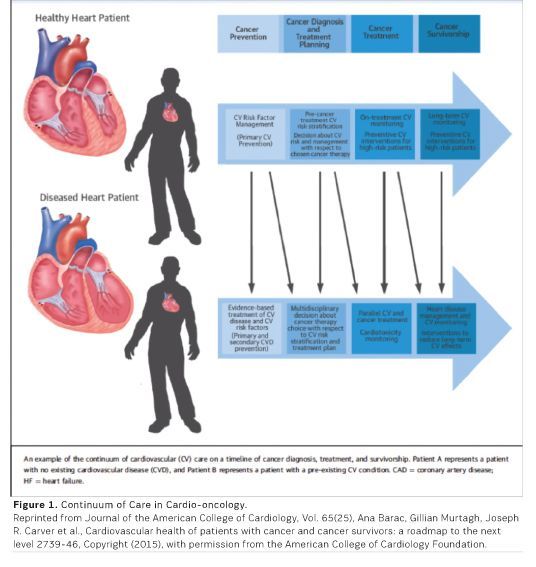
Once on treatment, appropriate surveillance for development of CTCT is necessary. guidelines for this surveillance are scarce and vary widely across different cancer types and patient populations. Recent data demonstrate the importance of early diagnosis and treatment of cardiac injury that may prevent development of clinical cardiovascular toxicity and improve patient outcomes, thus highlighting the need for investigations of standards of cardiac monitoring and prevention strategies during the cancer treatment period (Cardinale et al. 2015; 2010). The application of specialised imaging techniques (eg myocardial strain) and serum biomarkers (eg troponin, brain natriuretic peptide) have proven useful in tracking the degree of injury and stress during treatment, and in some cases are useful in predicting patients at greater risk to develop CTCT (Thavendiranathan et al. 2014; Ky et al. 2014). Beyond the risk to develop longterm CTCT, patients undergoing treatment, particularly with anthracyclines, are also at risk to develop acute CTCT, which can be life-threatening. A close working relationship between oncologists and cardiologists allows quick recognition of this development, and appropriate management to bridge the patient through what is often a recoverable process.
After treatment is complete, the period of survivorship begins. Paediatric literature, where survivorship of childhood and young adulthood cancers has seen a steady increase over years, provides invaluable amounts of cardiovascular data stemming from long-term survivorship cohorts that housed the bulk of efforts for research and clinical care. Awareness of cardiovascular disease risk among adult cancer survivors has seen an impressive surge, paralleling recent advances in cancer treatments that offer long survivorship, particularly for some cancers such as breast. Providers need to understand that symptomatic heart failure is not the only CTCT of concern. Increased occurrence of myocardial infarction, valvular disease, pericardial disease, hypertension, vascular disease, arrhythmias and obesity has also been reported. According to American Heart Association (AHA)/ ACC heart failure guidelines, patients who have received potentially cardiotoxic therapy would be classified within at a minimum, the stage A heart failure category (see Table 1), with the goal of surveillance and therapy being to prevent progression to stages B-D (Carver et al. 2013). While it may not be necessary for all survivors, certainly some should have lifelong follow-up with a cardiologist who understands the issues at hand. Approaching cancer therapy as an additional risk factor may have a profound influence on how a patient is followed, and what kind of surveillance may be needed relative to someone without this risk factor.

Special Considerations: Paediatrics and Advanced Cardiac Therapies
Paediatric and adolescent patients have been an important part of the story in defining CTCT, and many of the data regarding long-term survivors are from this population (Lipshultz et al. 2013). The Children’s Oncology group has detailed guidelines regarding screening for CTC in survivors, based on age at treatment, dose of anthracycline and concomitant radiation therapy (
survivorshipguidelines.org). Individual chemotherapy protocols also generally include some level of screening during treatment. However, involvement of a cardiologist is often reserved for a time when ventricular dysfunction or clinical heart failure is apparent. This approach may miss the opportunity to intervene with early changes or to be involved in risk assessment and treatment planning. The low incidence of existing cardiovascular disease in children going into therapy when compared to adults, and/or the desire not to introduce the spectre of additional poor outcomes, may be the explanation of the current strategies. However, early introduction could help identify additional risk factors not previously appreciated, open avenues for collaborative research in early prevention strategies, and establish a relationship that would ease introduction of a new care team if needed.
When patients with CTCT become refractory to standard medical therapy they may be considered for advanced therapies such as heart transplantation or mechanical circulatory support. Traditional recommendations have been for a patient to be off chemotherapy and in remission for 1-5 years, depending on the malignancy and prognosis, before being considered for transplantation. In general reported transplant outcomes have not significantly differed from those in patients without CTCT (Oliveira et al. 2012). For those patients not outside of the window of observation, mechanical circulatory support in the form of a ventricular assist device may allow recovery of function or serve as a bridge to the time at which evaluation would be appropriate. In cases that a patient is not expected to be eligible for transplantation, device therapy as a destination may be appropriate. Indeed, introduction of targeted therapy and significant improvement of expected survival in some forms of stage IV cancers is challenging our practice of excluding patients with cancer from advanced heart failure therapies. For example, in patients with metastatic HER2-positive breast cancer, where expected survival is measured in years, mechanical support devices may have the potential of meaningfully extending and improving quality of life. Active collaboration between the oncology, cardiology and advanced heart failure teams, with considerations of the risk for bleeding, thrombus, and infection, will be critically needed in this decision process.
Research and the Road to Reducing Cardiovascular Toxicity
As with all clinical advances, research holds the key to making improvements in clinical care for patients with CTCT. Identifying patients at risk, treatment factors involved, improved methods of surveillance, protective strategies and appropriate treatment once disease is discovered are all top priorities for the field of cardio-oncology (Shelburne et al. 2014). Some of the key challenges include lack of precise cardiovascular phenotypes, as well as unavailability of prospectively defined and collected cardiovascular outcomes in a broad population of patients who are receiving or have received cancer therapies. Creation of cardiovascular registries specific for these patients and cancer-treatment type would inform clinical practice and direct research. Close collaboration between cardiology and oncology professional organisations offers an opportunity for implementation of tools and resources already existing in cardiology clinical practice and rapidly advancing this field. For example, the ACC’s National Cardiovascular Data Registry (NCDR®) has been used in diverse areas of cardiovascular care, representing a standard for data collection and performance measures in cardiovascular medical therapies, procedures and devices. Expansion of this registry model to identify and follow cardiovascular outcomes in patients receiving cancer treatment would provide a powerful platform for advancement of cardio-oncology.
Establishing a Dedicated Cardio-oncology Programme
The team approach is key in establishing clinical and research programmes to care for cardio-oncology patients. Beside the obvious need for interested and invested cardiologists and oncologists, other key elements are institutional support, dedicated clinical staff, and appropriate education of ancillary services such as cardiovascular imaging, pharmacy and laboratory capabilities. The role of professional societies in this arena is to develop competency statements and provide training opportunities for all team members. Continuous education programmes for trainees and hospital staff, patient education and advocacy, and dissemination of information through local, regional, and national forums are all vital to a successful programme (Okwuosa and Barac 2015).
Moving Forward
The field of cardio-oncology is at the beginning of what promises to be an exciting and productive period that will benefit patient care for years to come. While established cardiology programmes nested within tertiary institutions with a primary cancer focus represented cardiooncology for years, the new era is marked by cardio-oncology clinics emerging in small and medium-size hospitals and community health offices. This is a reflection of the oncology care pattern, and has created a critical need for training of cardiovascular health care practitioners in this field. A recent ACC member survey showed that >70% of the respondents perceived cardiovascular effects of cancer treatment were very important, and 65% felt that access to specialised consultants would provide an advantage to caring for such patients. However, nearly 30% of respondents reported that they had to rely on a single provider with expertise or had no cardio-oncology services available (Barac et al. 2015). There is clearly a need to provide not only clinical training and services, but also educational opportunities for interested providers. Professional organisations offer unique resources to provide a framework for such efforts through development of clinical content standards and competencies, creation of clinical training curricula for cardiovascular trainees, and distribution of education and knowledge through workshops and conferences. The dynamic nature of this field will continue to be influenced by developments in the fields of oncology and cardiology. Ongoing collaboration at the level of providers, divisions, institutions and professional organisations will be critical, with each enhancing the ability of the other to care for this complex and potentially fragile patient population.
Key Points- Cancer therapy-related cardiovascular toxicity is a limitation of treatment.
- Patients need screening before, and surveillance during and after treatment.
- Cardio-oncology programmes are emerging to meet clinical and research needs.
- Support for cardio-oncology efforts from professional organisations is vital to their success.
Barac A, Murtagh G, Carver JR et al. (2015) Cardiovascular
health of patients with cancer and cancer survivors: a roadmap to the next
level. J Am Coll Cardiol, 65(25): 2739-46.
Bristow MR, Mason JW, Billingham ME et al. (1978)
Doxorubicin cardiomyopathy: evaluation by phonocardiography, endomyocardial
biopsy, and cardiac catheterization. Ann Intern Med, 88(2): 168-75.
Cardinale D, Colombo A, Bacchiani G et al. (2015) Early
detection of anthracycline cardiotoxicity and improvement with heart failure
therapy. Circulation, 131(22): 1981-8.
Cardinale D, Colombo A,
Lamantia G et al. (2010) Anthracycline-induced cardiomyopathy: clinical
relevance and response to pharmacologic therapy. J Am Coll Cardiol, 55(3):
213-20.
Carver JR, Szalda D,
Ky B (2013) Asymptomatic cardiac toxicity in long-term cancer survivors:
defining the population and recommendations for surveillance. Semin Oncol,
40(2): 229-38.
Desantis CE, Lin CC, Mariotto AB et al. (2014) Cancer
treatment and survivorship statistics, 2014. CA Cancer J Clin, 64(4): 252-71.
Hunt SA, Abraham WT,
Chin MH et al. (2005) ACC/AHA 2005 guideline update for the diagnosis and
management of chronic heart failure in the adult: a report of the American
College of Cardiology/American Heart Association Task Force on Practice
Guidelines (Writing Committee to Update the 2001 Guidelines for the Evaluation
and Management of Heart Failure): developed in collaboration with the American
College of Chest Physicians and the International Society for Heart and Lung
Transplantation: endorsed by the Heart Rhythm Society. Circulation, 112(12):
e154-235.
Ky B, Putt M, Sawaya H et al. (2014) Early increases in
multiple biomarkers predict subsequent cardiotoxicity in patients with breast
cancer treated with doxorubicin, taxanes, and trastuzumab. J Am Coll Cardiol,
63(8): 809-16.
Lipshultz SE, Adams MJ, Colan SD et al. (2013) Long-term
cardiovascular toxicity in children, adolescents, and young adults who receive
cancer therapy: pathophysiology, course, monitoring, management, prevention,
and research directions: a scientific statement from the American Heart Association.
Circulation, 128(17): 1927-95.
Mulrooney DA, Yeazel MW, Kawashima T et al. (2009) Cardiac
outcomes in a cohort of adult survivors of childhood and adolescent cancer:
retrospective analysis of the Childhood Cancer Survivor Study cohort. BMJ, 339:
b4606.
Okwuosa TM, Barac A (2015) Burgeoning CardioOncology
Programs: Challenges and Opportunities for Early Career Cardiologists/Faculty
Directors. J Am Coll Cardiol, 66(10): 1193-7.
Oliveira GH, Hardaway BW, Kucheryavaya AY et al. (2012)
Characteristics and survival of patients with chemotherapy-induced
cardiomyopathy undergoing heart transplantation. J Heart Lung Transplant,
31(8): 805-10.
Rinehart JJ, Lewis RP, Balcerzak SP (1974) Adriamycin
cardiotoxicity in man. Ann Intern Med, 81(4): 475-8.
Shelburne N, Adhikari B, Brell J et al. (2014) Cancer
treatment-related cardiotoxicity: current state of knowledge and future
research priorities. J Natl Cancer Inst, 106(9). pii: dju232. doi: 10.1093/
jnci/dju232.
Thavendiranathan P,
Poulin F, Lim KD et al. (2014) Use of myocardial strain imaging by
echocardiography for the early detection of cardiotoxicity in patients during
and after cancer chemotherapy: a systematic review. J Am Coll Cardiol, 63(25 Pt
A): 2751-68.
van Dalen EC, Caron
HN, Dickinson HO et al. (2011) Cardioprotective interventions for cancer
patients receiving anthracyclines. Cochrane Database Syst Rev, (6): CD003917.
van Dalen EC, Michiels EM, Caron HN et al. (2010) Different
anthracycline derivates for reducing cardiotoxicity in cancer patients.
Cochrane Database Syst Rev, (5): CD005006.
van Dalen EC, van Der Pal HJ, Caron HN et al. (2009)
Different dosage schedules for reducing cardiotoxicity in cancer patients
receiving anthracycline chemotherapy. Cochrane Database Syst Rev, (4):
CD005008. Yeh ET, Bickford CL (2009) Cardiovascular complications of cancer
therapy: incidence, pathogenesis, diagnosis, and management. J Am Coll Cardiol,
53(24): 2231-47.





