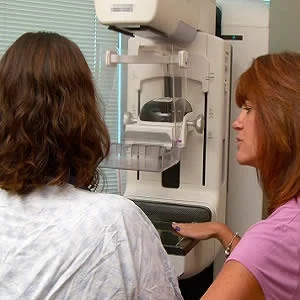
A Harvard-led study indicates that digital breast tomosynthesis (DBT) improves breast cancer detection at screening mammography. The study compared the diagnostic performance of DBT to that of full-field digital mammography (FFDM) in a mixed DBT and FFDM imaging environment. Based on the results, FFDM and DBT recall rates were not significantly different in a mixed FFDM and DBT breast imaging practice. However, the positive predictive value 1 (PPV1) of recalled cases and the cancer detection rate (the primary screening objective) were significantly higher with DBT compared with FFDM.
"Although the effects on overall recall rate may be lower with DBT than previously reported, the improvement in PPV1 suggests a reduction in unnecessary recalls," the authors write. "Future studies are needed to assess whether quality improvement interventions, such as focused interventions to lower individual and group recall rates, can enhance screening performance with DBT."
DBT is a technologic advance in breast imaging that acquires multiple images of the compressed breast in conjunction with a standard 2D mammogram acquired immediately after DBT acquisition during the same breast compression or, alternatively, a 2D image synthesised from the DBT acquisition. Studies of DBT in the screening setting have reported decreased recall rates (improved specificity) or increased cancer detection rates (improved sensitivity) or both, compared with standard 2D FFDM. Reported disadvantages of DBT include cost of the equipment, increased storage for much larger amounts of data, increased interpretation times, and increase in radiation dose when DBT is added to standard FFDM.
This retrospective observational study consisted of all female patients undergoing screening DBT or FFDM at an academic medical centre and outpatient imaging facility between October 2012 and May 2015. Patient demographics and personal history of breast cancer were collected from the electronic medical records. A natural language processing algorithm extracted patients' breast density, current or prior imaging findings, and BI-RADS category from their most recent prior imaging examinations.
To control for differential selection of FFDM versus DBT, researchers applied propensity score matching based on patient age, imaging site, and prior imaging findings. An institutional breast cancer registry identified cancer diagnoses. Primary outcomes of recall rate, cancer detection rate, and PPV1 were compared between matched FFDM and DBT groups.
Among 68,794 screening examinations, the researchers matched 16,264 FFDM with 21,074 DBT examinations (total, 37,338 exams) using nearest neighbour propensity score matching. Recall rates were 10.3% (1,683/16,264) for FFDM and 10.7% (2254/21,074) for DBT (p = 0.26). Cancer detection rates (number of cancers/1,000 exams) were 1.8/1,000 for FFDM and 3.8/1000 for DBT (p = 0.005). The PPV1 (number of cancers/number of recalls) was 1.8% (26/1,478) for FFDM and 3.6% (37/1,036) for DBT (p = 0.006).
"Our findings of reduced recall rates for baseline screening for DBT compared with FFDM are similar to others. Because baseline studies typically have a higher recall rate compared with studies with available comparison studies, practices with a hybrid imaging environment may wish to preferentially offer DBT to patients undergoing baseline screening," the authors said.
In addition, they found no significant difference in cancer detection rate and PPV1 in baseline examinations of patients who underwent DBT compared with FFDM. However, as the authors noted, the subgroup analysis was likely underpowered to reach statistical significance because of the small number of cancers in this subgroup.
Iphigenia Papaioanou
Editorial Project Director
HealthManagement
Latest Articles
Mammography, breast cancer, digital breast tomosynthesis, full-field digital mammography
A Harvard-led study indicates that digital breast tomosynthesis (DBT) improves breast cancer detection at screening mammography. The study compared the diagnostic performance of DBT to that of full-field digital mammography (FFDM) in a mixed DBT and FFDM