New molecular imaging technologies can make it easier to diagnose, monitor and treat cancers, and finding a way to use these noninvasive techniques more widely in clinical settings should be a top priority, according to experts from the Abramson Cancer Center and the Perelman School of Medicine at the University of Pennsylvania.
See Also: Multimodality Imaging in Cancer Management
In a review published in JAMA Oncology, the Penn team says use of molecular imaging provides added benefits to biopsies, especially when multiple examinations are needed. In a biopsy, tissue is removed from the patient so doctors can examine it.
Precision cancer care focuses on identifying the specific biomarkers of a patient’s cancer, which can help doctors make decisions about the best treatment options. The research team cites four main areas where molecular imaging can have a major impact:
• First, it can help identify patients most likely to benefit from targeted therapy. “Once we start treatment, it can also help us plan radiotherapy treatment and help define the boundaries of the active tumour,” says lead author Dr. David A. Mankoff.
• Second, it can monitor the movement of drugs throughout the body to guide drug dosing and minimise side effects.
• It can also monitor whether those drugs are having an effect.
• Finally, all of this data can be combined to predict patient outcomes including overall survival.
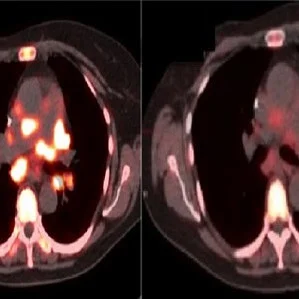
Molecular imaging uses special imaging “probe” compounds (injected into the patient) to highlight a desired molecular target in a tissue of interest. FDG-PET, one of the only molecular imaging techniques routinely used in oncology, employs a glucose-like probe, FDG, with a radioactive isotope of fluorine attached as a beacon. Upon injection into the bloodstream, the FDG probe quickly accumulates in tumours, which tend to make heavy use of glucose. Thus, it “lights up” those tumours on a PET (positron emission tomography) scan.
FDG-PET has been used for more than two decades to detect tumours and determine the extent to which cancer has spread. According to the Penn team, the newer PET probes now in development and testing are meant for many other applications in cancer medicine. For example, two new classes of probe are designed to bind to estrogen and HER2 receptors. Breast, uterine, and ovarian tumours often use these receptors to boost their growth, and many cancer drugs target them.
Detecting the presence of tumour estrogen or HER2 receptors with PET scans allows oncologists to examine all sites of cancer for each patient, choose the appropriate drug treatment more quickly, monitor the tumour for changes that may necessitate a switch to another treatment, and even evaluate how well a drug is hitting its receptor targets.
In addition, imaging with the new PET probes can reveal receptors or other tumour-related markers at sites where the cancer may have spread, including bone, which is much harder to biopsy, the researchers explained.
Although many of these new methods are already being studied in clinical trials, "the path from clinical trials to routine clinical use is seldom easy,” notes Dr. Mankoff, PhD, the Gerd Muehllehner Professor of Radiology and director of the PET Center at the Perelman School of Medicine at the University of Pennsylvania. “And molecular imaging methods face some particularly challenging hurdles such as the need to deliver the short-lived imaging probes to centres performing the imaging.”
Dr. Mankoff and his colleagues argue that making a strong clinical case for these new imaging techniques will mean demonstrating their ability to improve traditional treatment outcomes such as progression-free survival and quality of life.
Source: Perelman School of Medicine at the University of Pennsylvania
Image Credit: Penn Medicine
References:
Mankoff DA, Farwell MD, Clark AS (2016) Making molecular imaging a clinical tool for precision oncology: a review. JAMA Oncol, 2016 Dec 29. doi: 10.1001/jamaoncol.2016.5084.
Latest Articles
Molecular Imaging, Cancer Care, targeted therapy, radiotherapy, patient outcomes
New molecular imaging technologies can make it easier to diagnose, monitor and treat cancers, and finding a way to use these noninvasive techniques more widely in clinical settings should be a top priority, according to experts.