Across Europe, the growing number of radioembolisation procedures may reflect that radioembolisation is increasingly recognised as a valuable treatment option in European cancer guidelines. Furthermore, there seems to be a trend towards less coil-embolisation of non-target vessels, according to a new study published online in the journal CardioVascular and Interventional Radiology.
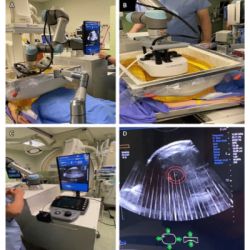
Radioembolisation requires close collaboration of a multidisciplinary team, in which intervention-radiologists and nuclear physicians take the lead together. It is a complex image-guided procedure and can be performed in a large variety of ways. Operators have to make choices ranging from the type of microspheres, type of catheters, use of imaging modalities to methods for calculating the activity.
A survey from 2011 (published in 2012) showed that there are many differences in how radioembolisation is performed across 28 centres in Europe. Today, the radioembolisation community has grown and there have been technical and strategic changes in the field. For example, cone-beam CT (also known as C-arm CT) is introduced as a tool in the radioembolisation procedure and a significant increase in the use of SPECT–CT is seen.
To investigate how these changes have impacted daily practice in European centres and what differences exist between centres, an online questionnaire was distributed amongst all members of the Cardiovascular and Interventional Radiological Society of Europe (CIRSE). The 25 questions from the 2011 study (Powerski et al.) were updated, and new questions were added.
The survey was completed by 60 centres. Based on the survey data, there seems to be a steady rise in number of centres performing radioembolisation. Cumulatively, 60 centres in Europe perform radioembolisation, with the majority of centres (80%) performing between 1 and 50 radioembolisation procedures in 2016. The number of centres performing more than 25 treatments per year has increased over the last three years from 20 centres in 2014 to 25 centres in 2016.
Hepatocellular carcinoma (HCC) and colorectal carcinoma metastases (mCRC) were the most frequent tumour types treated with radioembolisation as 15 centres treat more than 25 patients per year with these tumour types. Also, there were a few centres that use radioembolisation for pancreas cancer and (ocular) melanoma amongst other tumour types. Other key findings from the survey include:
- 40% of the centres use resin microspheres only, whereas 27% only use glass microspheres and approximately 33% use both resin and glass microspheres.
- In most cases, a combination of imaging modalities is used for pretreatment staging of disease. CT (75%) was most commonly used, closely followed by MRI (70%) and lastly PET–CT (50%).
- Tumour burden > 70% is a dominant contraindication in the majority of centres. Lung shunting is the main reason to exclude patients from treatment (82%).
- The degree of coil-embolisation of non-target vessels is highly variable between centres: the right gastric artery is coil-embolised most often (79%), followed by the gastroduodenal artery (75%). The vast majority of centres (92%) do not coil the cystic artery.
In addition, 7% of all centres do not use post-treatment imaging to evaluate microsphere distribution. The other centres often use multiple imaging modalities: Bremsstrahlung SPECT–CT (53%), PET–CT (34%), and Bremsstrahlung SPECT (19%). CT (72%) and MRI (72%) were mostly used for follow-up of tumour status, followed by PET–CT (35%) and PET (2%).
The main complications reported after radioembolisation are: radiation pneumonitis, gastrointestinal complications, pancreatic complications, bile duct complications, cholecystitis and abscess, with the centre peak incidences at 0–1% of patients.
"In general, the results of this survey show a discrepancy between the techniques that are recommended in the literature and the techniques used in daily practice. Examples are the relatively infrequent use of the partition model, scarce use of Y90-PET–CT and cone-beam CT and the high frequency of coil-embolisation. We believe that research initiatives should be aimed at reducing these discrepancies and improving techniques in a way that they can be used by any centre and not only by experts," the study authors conclude.
Image Credit: Health.mil
References:
Reinders MTM et al. (2018) Radioembolisation in Europe: A Survey Amongst CIRSE Members. Cardiovasc Intervent Radiol. Published online: 08 May 2018 https://doi.org/10.1007/s00270-018-1982-4
Latest Articles
radioembolisation, coil-embolisation, SPECT–CT
Across Europe, the growing number of radioembolisation procedures may reflect that radioembolisation is increasingly recognised as a valuable treatment option in European cancer guidelines. Furthermore, there seems to be a trend towards less coil-embolisa