Key requisites for the interventional radiology practice was the subject of Dr. Iain Robertson’s presentation at the CIRSE congress today.
Interventional radiologists need to understand the scope of their services. be more proactive about the services they intend to provide. and also what they do not provide. IR services should be a
conduit towards services even if they do not provide them. IN hours and out of hours services will not be identical and also need to be considered. He emphasised the importance of understanding outcomes. At his own institution, they took the two most common procedures and looked at deaths after the procedure. Their analysis showed about 40% die from other causes - interventional radiologists can’t make assumptions about the success of their procedures without analysing the data.
The physical set up should included:
- a fixed fluoroscopy facility
- clean/theatre air and piped gases
- local regulatory estates guidance
- follow specific guidance e.g. in the Uk the MHRA guidance on EVAR for example
- Ultrasound in room
- Access to CT/MR/PF
Outpatient clinics are essential, and need to be a clinic with support, a referral focus , pre-intervention assessment, follow-up and the ability to undertake research. Robertson noted a survey that the British Society of Interventional Radiology undertook in 2012. They found that only 52% of the reponsdents had outpatient clinics.
Services need bed access - more in day beds than inpatient beds. This widens the referral base and lowers the cost per case. Beds need to be in a purpose-built area not an ad hoc single bed. Each service should decide whether it is an IR only unit or more general. If it is IR only then they need to be staffed from the team. If they general then the IR service needs to educate team. He added that in his experience general units have faster throughput.
When it comes to staffing requirements, knowing the scope of services helps you and applicants know whether they fit. How many staff depends on your services - if it’s 24/7 probably a minimum of 1:6 is appropriate. If the population is greater than a million then 1:8. looks to cirses development of european guidelines. The UK has its own standards for providing access to IR services 24/7 published by the NHS Improving Quality.
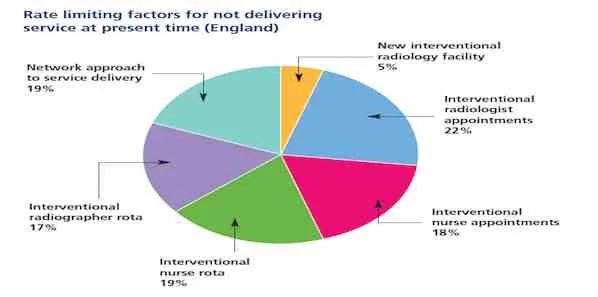
the British Society for Interventional Radiology asked its members what the limiting factors were in providing a comprehensive IR service. These mainly related to staff rotas [see image].
Robertson emphasies the important roles of IR nurses and radiographers. Nurses are vital to a safe on-call system. The UK college has published guidelines for nursing care in interventional radiology. He noted that there are issues with rotational staff when it comes to leadership. He ended with a call to focus on the role of extended care practitioners. They are massively underused, he said, and are key to coping with future demands.
Communication with Patients
Robertson emphasised the two main goals - to create a good interpersonal relationship and facilitate the exchange of information. Including patients in decision making leads to better information, compliance and recovery. It sounds simple, but he believes that doctors always overestimate their communication skills. He quoted Terry Canale: “The patient will never how much you know until they know how much your care.” In summary, doctors should stop (looking at the computer screen), look at the patient and think about what they are trying to tell you, and listen. Repeat key facts in a summary plan, give contact details for more information and seek feedback.
When it comes to communicating with colleagues, teamwork hinges on communication and respect. It is important record decisions to gain respect. Radiologists should consider structured communication. In addition, try to summarise what has been done, and don’t just refer them to the ehealth record. Interventional radiologists should seek and use multi-source feedback.
Interventional radiologists need to understand the scope of their services. be more proactive about the services they intend to provide. and also what they do not provide. IR services should be a
conduit towards services even if they do not provide them. IN hours and out of hours services will not be identical and also need to be considered. He emphasised the importance of understanding outcomes. At his own institution, they took the two most common procedures and looked at deaths after the procedure. Their analysis showed about 40% die from other causes - interventional radiologists can’t make assumptions about the success of their procedures without analysing the data.
The physical set up should included:
- a fixed fluoroscopy facility
- clean/theatre air and piped gases
- local regulatory estates guidance
- follow specific guidance e.g. in the Uk the MHRA guidance on EVAR for example
- Ultrasound in room
- Access to CT/MR/PF
Outpatient clinics are essential, and need to be a clinic with support, a referral focus , pre-intervention assessment, follow-up and the ability to undertake research. Robertson noted a survey that the British Society of Interventional Radiology undertook in 2012. They found that only 52% of the reponsdents had outpatient clinics.
Services need bed access - more in day beds than inpatient beds. This widens the referral base and lowers the cost per case. Beds need to be in a purpose-built area not an ad hoc single bed. Each service should decide whether it is an IR only unit or more general. If it is IR only then they need to be staffed from the team. If they general then the IR service needs to educate team. He added that in his experience general units have faster throughput.
When it comes to staffing requirements, knowing the scope of services helps you and applicants know whether they fit. How many staff depends on your services - if it’s 24/7 probably a minimum of 1:6 is appropriate. If the population is greater than a million then 1:8. looks to cirses development of european guidelines. The UK has its own standards for providing access to IR services 24/7 published by the NHS Improving Quality.
the British Society for Interventional Radiology asked its members what the limiting factors were in providing a comprehensive IR service. These mainly related to staff rotas [see image].
Robertson emphasies the important roles of IR nurses and radiographers. Nurses are vital to a safe on-call system. The UK college has published guidelines for nursing care in interventional radiology. He noted that there are issues with rotational staff when it comes to leadership. He ended with a call to focus on the role of extended care practitioners. They are massively underused, he said, and are key to coping with future demands.
Communication with Patients
Robertson emphasised the two main goals - to create a good interpersonal relationship and facilitate the exchange of information. Including patients in decision making leads to better information, compliance and recovery. It sounds simple, but he believes that doctors always overestimate their communication skills. He quoted Terry Canale: “The patient will never how much you know until they know how much your care.” In summary, doctors should stop (looking at the computer screen), look at the patient and think about what they are trying to tell you, and listen. Repeat key facts in a summary plan, give contact details for more information and seek feedback.
When it comes to communicating with colleagues, teamwork hinges on communication and respect. It is important record decisions to gain respect. Radiologists should consider structured communication. In addition, try to summarise what has been done, and don’t just refer them to the ehealth record. Interventional radiologists should seek and use multi-source feedback.
Latest Articles
CIRSE 2014, interventional radiology, Service delivery
Key requisites for the interventional radiology practice was the subject of Dr. Iain Robertson’s presentation at the CIRSE congress today. Intervention...