HealthManagement, Volume 13 - Issue 3, 2013
Author
Dr. Daniel Boxer
West Hertfordshire Hospitals NHS Trust
Watford, UK
Key Point
· Delivery of radiology for acute care within a dedicated unit may be beneficial for patient outcomes and lengths of stay. · Radiology is becoming an extended hour 7-day service. · Separating acute and elective care has organisational benefits for radiology departments. · Radiology working practices can be modernised and this can be facilitated by IT solutions. |
“the challenge of balancing the need for a radiologist to have a wide range of skills against the quality issue of developing subspeciality interest remains the biggest challenge to implementing and developing a service model such as ours”
Introduction
West Hertfordshire Hospitals NHS Trust (WHHT) provides predominantly secondary care acute hospital services to a population of about 500,000 people in Southern England. Emergency in-patient care is based around an (initially) 120 bedded, purpose built, Acute Admissions Unit (AAU), which opened in 2009. A new model of acute care was developed with intensive investigation and treatment of acute admissions and greatly increased consultant level input into management decisions. Ward rounds are performed on an extended hours 7-day model. To complement this, radiology is also provided in this manner with consultant radiologists being on-site 7 days per week and for extended working hours. This service is also based within the AAU in a dedicated radiology suite. Over the intervening years, with experience and changes (mainly increases) within the workload, the radiology model has developed in a dynamic manner, which will be discussed in this article.
Background
Following a strategic review of acute hospital care within West Hertfordshire, governmental approval was given to merge the acute hospitals services provided by two District General Hospitals on to one of the pre-existing sites. The major organisational drivers for this were to improve financial stability and allow for junior doctor rotas to comply with the European Working Times Directive. There would be a net significant reduction in the bed pool. To offset this, a 120 bed purpose-built freestanding acute admissions unit with integrated diagnostic suite was developed together with new, more efficient, ways of working. The aim was to reduce patient length of stay and improve the quality of care by increased consultant input, early use of high level imaging to improve diagnosis and extended hours working. The radiology department took this opportunity to substantially reorganise in-patient care, separating acute and elective work. This was facilitated by the coincidental development of radiology management software (Wizrad) and substantial modernisation of radiologists’ working practices.
The Acute Admissions Unit
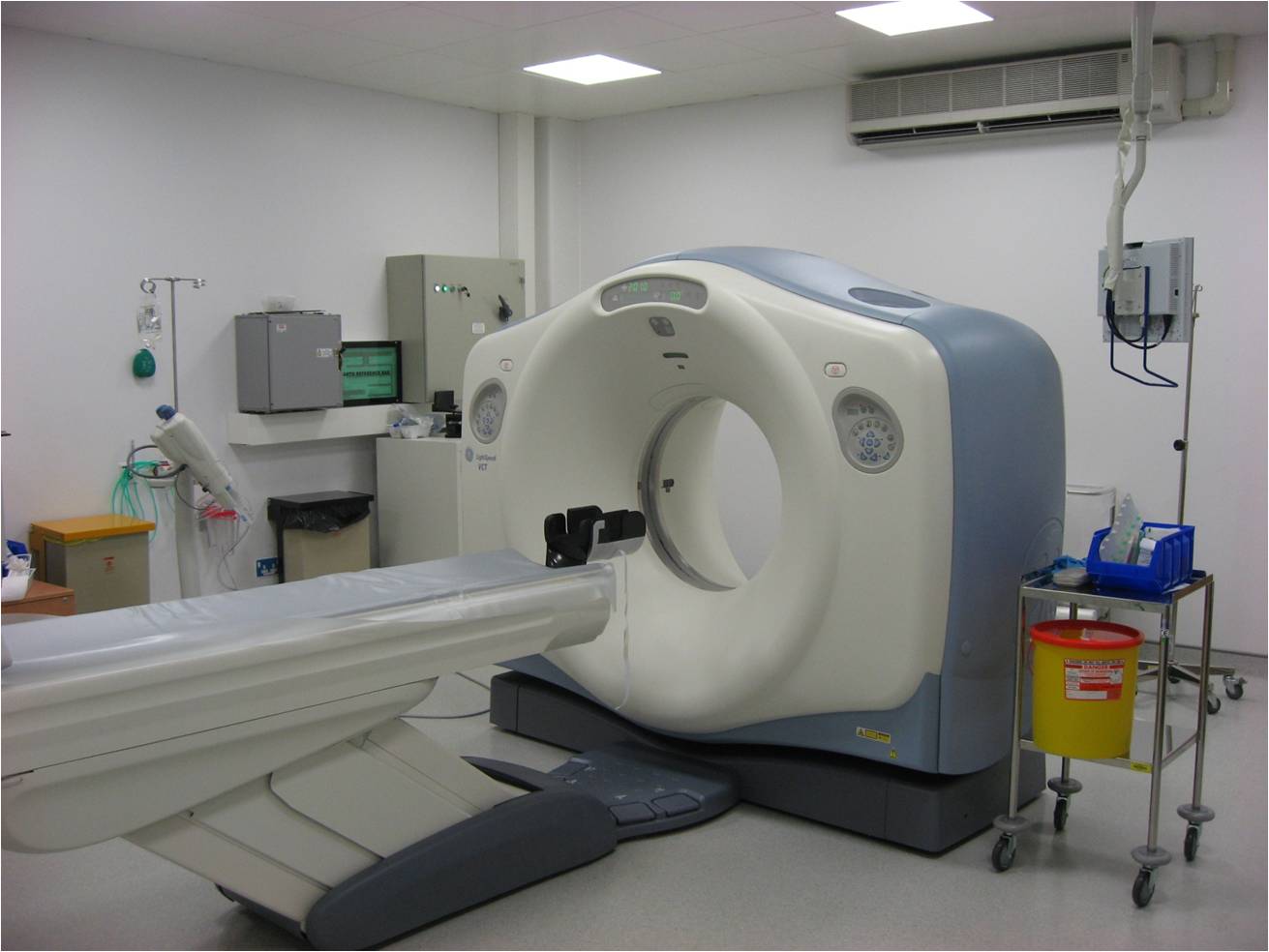
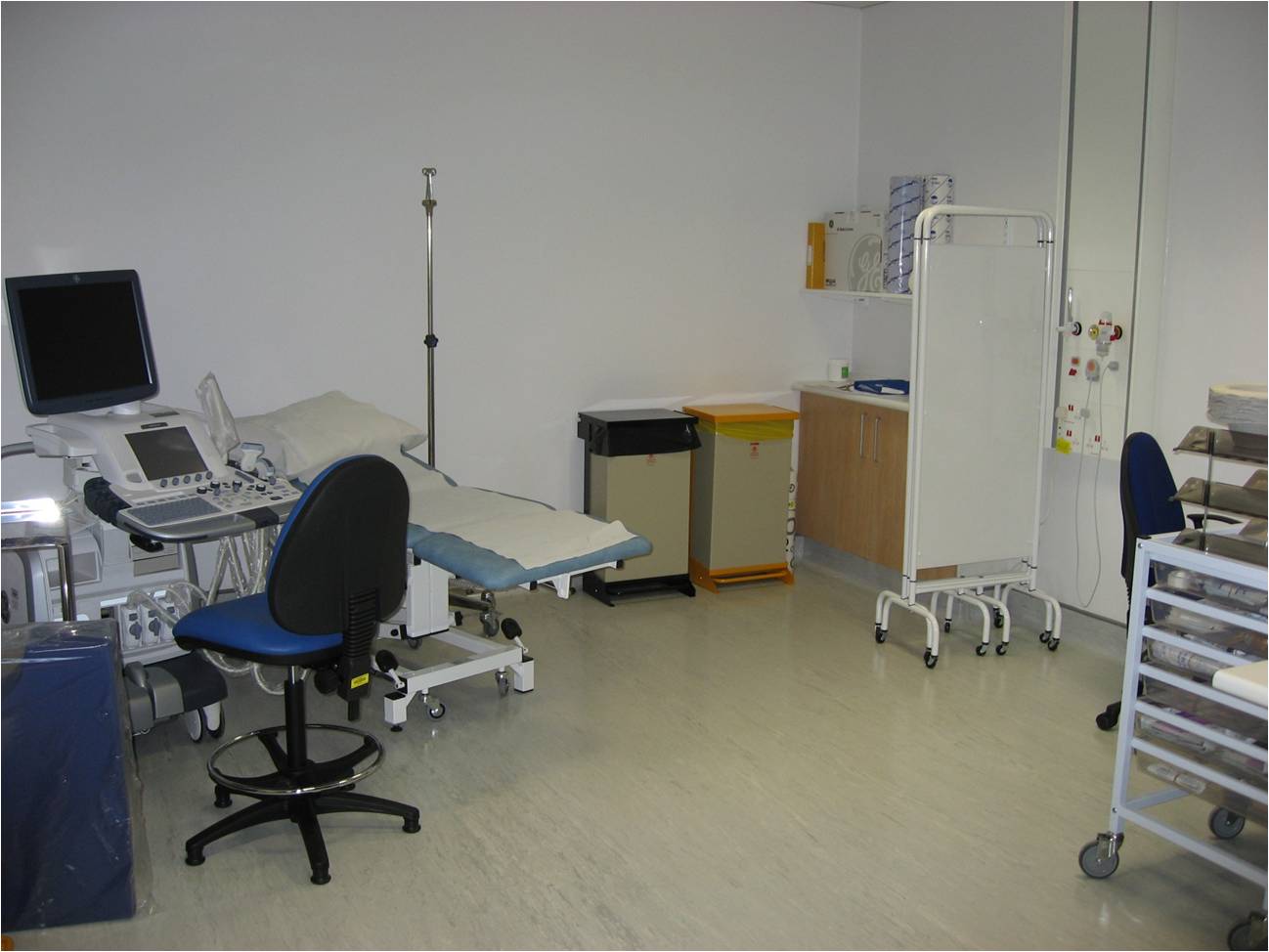
As originally constructed this was a freestanding modular built structure on three levels containing 120 beds. The ward accommodation comprises eight suites of 15 beds each, 12 in bays and three side rooms, on levels 1 and 3. Level 2 accommodates radiology, two cardiac catheter laboratories with 12 recovery beds and a robotic pharmacy. The radiology suite is furnished with a 64-slice CT scanner (pictured below), ultrasound (pictured below), three PACS workstations, offices and ancillary spaces. There is a plain film room on level 1.
 (Im
(Im
Image 1 - The AAU as originally configured
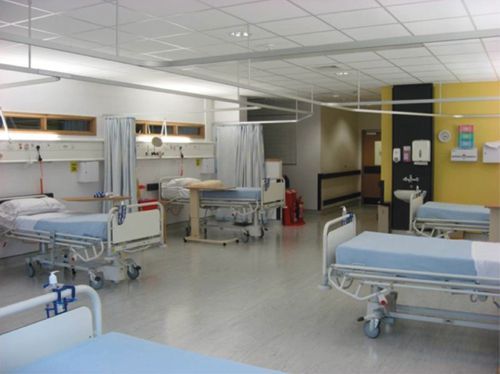 Image 2)
Image 2)
Image 2 - AAU ward bay
 Most acute medical, surgical and orthopaedic patients are
admitted to the AAU, either directly by family doctors, ambulance paramedics or
via Accident and Emergency. Patients are seen by senior clinicians with
multiple daily ward rounds. These are supported by a similar level of daily
sub-speciality ward rounds (e.g. chest medicine, cardiology, and
gastroenterology). Requesting of complex imaging is generally at this level or
by speciality registrars. As the radiologists are based within the unit and
dedicated to the in-patient service direct multidisciplinary discussion of
cases is straightforward. We have recently moved to digital order
communications. A side effect of this has been to reduce the
clinic-radiological interactions. The radiologists see this as being
detrimental to the service, but it has proven popular with the clinical staff,
in particular the junior medical staff. The impact on workload has yet to be
appreciated.
Most acute medical, surgical and orthopaedic patients are
admitted to the AAU, either directly by family doctors, ambulance paramedics or
via Accident and Emergency. Patients are seen by senior clinicians with
multiple daily ward rounds. These are supported by a similar level of daily
sub-speciality ward rounds (e.g. chest medicine, cardiology, and
gastroenterology). Requesting of complex imaging is generally at this level or
by speciality registrars. As the radiologists are based within the unit and
dedicated to the in-patient service direct multidisciplinary discussion of
cases is straightforward. We have recently moved to digital order
communications. A side effect of this has been to reduce the
clinic-radiological interactions. The radiologists see this as being
detrimental to the service, but it has proven popular with the clinical staff,
in particular the junior medical staff. The impact on workload has yet to be
appreciated.
The original intention was that patients would spend a maximum of 48 hours within the AAU and either be discharged or transferred to speciality wards within the main hospital. Unfortunately this model has not been consistently sustainable due to bed blockages further down the line and delays organising discharge care packages and so on. Consequently some patients are spending longer within the AAU. Additionally there has been a dramatic increase in demand for acute care, particularly of the elderly frail. It has been necessary to increase the capacity of the AAU, which now has 156 beds, having been enlarged by additional linear positioned units. Some of these are dedicated to ambulatory care, and the AAU radiology department also provides imaging for these patients.

Image 3 - Current expanded configuration of the AAU
Radiology Staffing for the AAU
As well as fully funding the accommodation and equipment for the radiology suite the business case provided for two additional radiologists and two radiographers. It was agreed that a consultant-level radiologist (our department is staffed essentially entirely at this level) would be on-site 08:00-20:00 Monday-Friday and 09:00-13:00 on weekends and public holidays. Departmental analysis (a Wizrad function) suggested that a typical day’s in-patient activity, excluding complex interventional procedures, equates to 20 hours of radiologist time. All in-patient CT and ultrasound scanning was to be performed in the AAU, MRI in the main department but reported via PACS by the AAU radiologist.
In order to staff this service a series of interlocking radiologist rotas was developed: AAU1 08:00-16:00, AAU2 10:00-18:00, evening 17:00-20:00, weekend and public holidays 09:00-13:00. The radiologists would do a week alternating as either AAU1 or 2 approximately once a month. Averaged over the year one evening and weekend session is performed per month. If a radiologist is not available to perform a session (typically half a day) because they are not contracted to be present or for other reasons (such as high priority clinical commitment, e.g. one stop clinics), another radiologist acts as a filler, compensated for by a reduction in their weekly workload. This is easily calculated because of the workload programming function within Wizrad used to allocate work in the weeks when not assigned to the AAU.
The disparity between providing 20 hours of radiology time during the week and four hours at weekends was originally due to a combination of funding and the radiologist’s willingness to sacrifice the work/life balance. Currently we are trialling extension of the service until 18:00 on these days.
Outside of the extended hours scheme above a ‘traditional’ type on-call service is provided, largely via telemedicine.
The AAU radiologists are responsible for most of the imaging of inpatient and emergency patients. Vetting is now largely by order communications and reporting is increasingly via voice recognition. Imaging is entirely via PACS. The largest reporting load is of CT scanning, but they also report MRI scans, and perform ultrasound scans and simple interventional procedures (mainly biopsies and drainages). The radiologists thus have to have a wide range of skills. Individually they may not be able to cover all aspects of clinical care (for instance paediatrics, gynaecology and higher level musculoskeletal). However, there tend to be complementary skills available between the personnel on the different overlapping rotas. Alternatively it is usually possible to find a radiologist working outside the AAU able to absorb these occasional cases. The challenge of balancing the need for a radiologist to have a wide range of skills against the quality issue of developing subspeciality interest remains the biggest challenge to implementing and developing a service model such as ours.
Vascular and complex interventional work remains the province of the interventional radiologists, who have an allocation within their general reporting (via Wizrad) to allow for this.
Most radiologists find working in the AAU to be intense and stressful although the work is interesting and generally rewarding. The workload has however increased significantly (see Table 1), in parallel with the increasing demand. Further resources for radiology are clearly needed although difficult to fund under the current economic climate.
Removing most of the acute radiology from our pre-existing department has had significant benefits for the elective service. Unbooked spaces no longer need to be kept in lists in case they are needed for in-patients. There are far fewer interruptions whilst reporting or performing investigations. This improves productivity; indeed, since the introduction of Wizrad the reporting output of the radiologists has increased by approximately 25%. It is also beneficial to the clinical teams, as they no longer have to search for and negotiate with a radiologist involved in other activities.
Wizrad and Allocated Workloads
Radiologists no longer have dedicated lists in modalities such as CT, MRI and nuclear medicine or dedicated reporting sessions. Instead they are allocated reporting of these modalities based on the amount of non-committed time they have in their timetable during that week. This is orchestrated by an information technology solution, Wizrad, which is an in-house authored spreadsheet driven programme, shortly to be replaced by a proprietary web-based programme. From the radiologist’s number of contracted hours committed time is removed. This would include hands on radiology procedures (e.g. ultrasound, interventional and screening procedures) as well as multidisciplinary meetings, teaching, management and medical supporting activities, such as clinical governance. The remaining time is used for generic reporting. Wizrad converts this time into number of examinations to be reported based on a time tariff, which was agreed by the radiologists as a body, and individual modality preferences and subspecialty interest. If the radiologist loses reporting time to attend AAU as a filler this undergoes a pro-rata reduction. The radiographic modality leads receive a list of how many examinations each radiologist is to report that week, which are then placed on their individual work lists on the Radiology Information System. This system has great advantages for the radiologists, as they know exactly how much reporting they will receive that week, there is flexibility in when the reporting can be done and it is seen to be transparent and equable (Boxer, 2012). As a management tool it provides accurate reporting capacity data, as well as being a powerful departmental scheduler and leave manager.
Conclusion
There is increasing evidence that providing extended hours radiology services improves patient outcomes, reduces length of stay and overall costs of hospital-based acute patient care (Department of Health, 2012). We have been able to provide the radiology support to a very large acute admission unit on this basis. We have found separating acute from elective work streams has had organisational benefits to our radiology department. This has been enabled by innovative working practices utilising a novel IT solution. Our model has proven successful within our organisation. However, other units would have different challenges implementing such a system. A particular issue is that of subspecialisation and the skill set required to provide an acute service. An increasingly recognised medical subspecialty is that of acute care physician (Temple 2012), it may be that a similar practitioner is required in radiology with appropriate skill levels and experience.
Table 1. Total
radiologist work load by parts imaged in financial years
| CT | MRI | Ultrasound |
2009 | 9867 | 866 | 3257 |
2010 | 10960 | 1446 | 3304 |
2011 | 11542 | 1663 | 3651 |
2012 | 12197 | 1767 | 4214 |
References:
Boxer D (2012) Radiology session scheduling - an IT based flexible reporting system. Imaging Management, 12(1):35-6.
National Imaging Clinical Advisory Group (2012). Implementing 7 Day working in radiology departments: good practice guidance. London: Department of Health. Available at: <https://www.gov.uk/government/publications/implementing-7-day-working-in-imaging-department-good-practice-guidance> [Accessed: 1 August 2013]
Temple RM, Kirthi V, Patterson LJ (2012) Is it time for a new kind of hospital physician? BMJ, 344: e2240.





