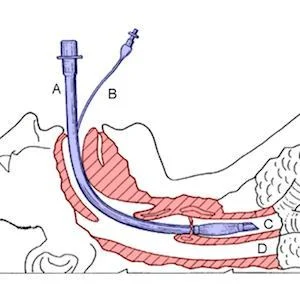
Endotracheal mechanical ventilation (MV) is a major treatment of life-threatening conditions, but weaning from MV remains a great challenge, and time of extubation a critical issue in the ICU management, says an Editorial published in the journal Annals of Translational Medicine. Extubation failure can occur in 10-20% of cases with a higher ICU mortality rate in reintubated patients ranging from 25% to 50%, the article notes.
It's important for ICU physicians to "consider the potential issue of the weaning/extubation process as early as possible according to the underlying status for optimising the weaning/extubation conditions, limit the risk of reintubation and eventually propose alternative techniques for post-extubation management," write article authors Drs. Christophe Girault, Gaëtan Béduneau, Dorothée Carpentier and Benoît Misset, all from the Department of Medical Intensive Care, Rouen University Hospital (France).
In addition to standard oxygen therapy (O2), two other non-invasive techniques have been proposed for the weaning/post-extubation management: non-invasive ventilation (NIV) and high-flow nasal oxygen therapy (HFNO). The authors explain how these techniques are applied and their benefits to patients:
- Apart from NIV used as a
weaning strategy, preventive post-extubation NIV appears to be of clinical
benefit mainly in medical population considered at risk for extubation failure,
whereas curative post-extubation NIV seems more beneficial in surgical
(post-operative) than in non-selected medical population.
- HFNO has been shown to be beneficial on clinical outcome in severe hypoxaemic ARF patients; it has also been recently assessed as a preventive post-extubation ventilatory support.
While HFNO has been demonstrated to improve oxygenation and respiratory comfort, decrease the need for reintubation and post-extubation NIV in a general ICU population, the authors note that no study has applied post-extubation HFNO in high-risk patients for extubation failure nor compared HFNO with NIV in this setting.
The two trials recently conducted by Hernández et al. have suggested a potential benefit of HFNO compared to standard O2 in the post-extubation management, particularly in high-risk patients for reintubation.
"Using preventive HFNO in all low-risk patients for extubation failure could be, however, unreasonable since HFNO is more expansive than standard O2 and can be still unavailable in all adults ICU. Furthermore, weaning from HFNO being not well established, such a strategy could unnecessarily increase the ICU stay in low-risk patients, the use of HFNO being not recommended on general wards because of its potential risk to mask undertreated ARF," according to the Editorial.
Image credit: Wikimedia Commons
References:
Girault C1, Béduneau G, Carpentier D, Misset B (2017) Preventive post-extubation high-flow nasal oxygen therapy versus non-invasive ventilation: a substitutive or a complementary ventilatory strategy? Ann Transl Med, 5(6): 146. doi: 10.21037/atm.2017.01.23 |