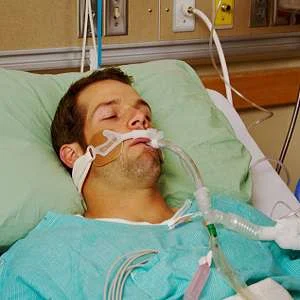
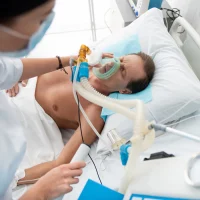
Ventilator-induced lung injury is a multifaceted problem that has progressively become a preoccupation for intensivists and anaesthesiologists. Interestingly, it has taken many years to realise that mechanical ventilation, a life-saving technique, could also induce harm, according to an Editorial article published online in the journal Anesthesiology.
The editorial cites pioneering experimental work — from Webb and Tierney and later from Dreyfuss and Saumon — that progressively demonstrated the potential of large volumes and pressures to cause injury either in previously healthy or already injured lungs.
Further, recommendations in the early 1990s introduced the concept of pressure limitation in the alveoli, as measured by the plateau pressure. An early clinical report by Hickling et al. also suggested, in 1990, a marked improvement in patient survival resulting from deliberately limiting pressures and volumes.
The editorial, penned by Dr. Laurent Brochard (Interdepartmental Division of Critical Care Medicine, University of Toronto) and Dr. Andrew Bersten (Intensive and Critical Care Unit, Flinders Medical Centre), commends a new study by Collino et al. for addressing these two important questions: Which positive end-expiratory pressure (PEEP) level is optimal for protecting the lung of mechanically ventilated patients? How can we determine when mechanical ventilation is harming the lung and/or is inducing systemic inflammation deleterious for other organs (before it is too late)?
In their study, Collino et al. applied the concept of mechanical power as a unifying determinant of injury that describes the energy transfer to the lung to predict the potential harm generated by mechanical insufflations at increasing pressures. The mechanical power takes into account the energy delivered to the lung, popularised by the driving pressure, the dynamic changes in pressure, the energy related to the increase in lung volume induced by PEEP, and the respiratory rate.
"The study well illustrates the complexity of the so-called ventilator-induced lung injury, including both atelectrauma (insufficient reopening of the lung at end expiration and/or repeated opening and closing of this atelectatic lung) and volutrauma inducing distension and major haemodynamic effects," Drs. Brochard and Bersten note. "Interestingly, they found that PEEP — at 'low' values — is an important component of lung protection, a key finding shown for many years, even if its mechanisms are not completely understood."
The experimental model used in the study by Collino et al. represents the effects of potentially injurious “standard” ventilation (8 to 10ml/kg of tidal volume) at different baseline pressures (PEEP) in the presence of general anaesthesia with healthy lungs. However, the chosen model, piglets, makes it difficult to completely infer from these data what would be the equivalent in patients, according to the editorialists.
"We need to see data using a relevant lung injury model where the competing issues of recruitment and overinflation may well influence the data and suggest a different safe power," Drs. Brochard and Bersten say.
Source: Anesthesiology
Image Credit: iStock