A recent study, presented at the meeting of the American College of Cardiology (ACC) in Washington and published by the New England Journal of Medicine, has cast a doubt over therapy used in more than 80 countries and prescribed to treat hypertension that does not respond to drugs.
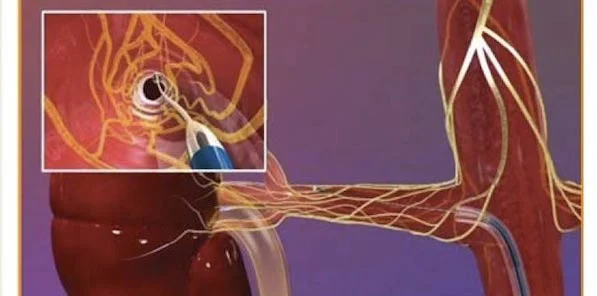
Renal artery denervation is an intervention in which nerve connections between the heart and kidney are disrupted in an effort to lower blood pressure by threading a catheter into the arteries feeding the kidney and using radiotherapy to destroy some of the nerves believed to control blood pressure.
This new major clinical trial was considered a key test for the procedure, as prior trials did not include a blinded control group for efficacy comparison. In this study, patients who were treated by renal artery denervation were no more likely to see their blood pressure decline than those who received a fake therapy.
Commenting in a Journal editorial, Dr. Fran Messerli and Dr. Sripal Bangalore saw this study bringing a stop to the “renal-denervation train”. Due to the fact that earlier tests of this technique did not involve treating some patients with sham therapy, they suggest that the placebo effect may well explain all or most of the blood pressure differences noted in two key trials, entitled SYMPLICITY HTM-1 and HTN-2.
SYMPLICITY HTN-3, the new blinded test, was financed by Medtronic Inc, makers of the equipment used in the study. Boston Scientific Corp and St. Jude Medical Inc are also renal denervation equipment manufacturers.
Chief investigator Dr. Deepak Bhatt of Brigham and Women's Hospital in Boston explained the team’s aim was to explore whether this would improve further on what the best medical therapy could do, adding that the findings should now at least “give doctors pause to what the are doing”.
While renal denervation is still regarded as experimental in the United States, countries such as South America, Canada, Australia and parts of Europe have approved the therapy. Roughly 10 percent of high blood pressure sufferers are resistant to conventional therapy, making them candidates for the treatment.
Since previous trials had yielded positive findings, Dr. Anthony DeMaria, who did not participate in the trial but discussed the study at an ACC news conference, expressed how surprised all involved were about the negative results. He added that further evidence was required to ascertain that the procedure was indeed accomplishing effective denervation. Until this was achieved, DeMaria, director of the Cardiovascular Center at U.C. San Diego School of Medicine, suggested limiting this treatment to "patients who had no alternative," said DeMaria.
All of the 364 patients enrolled in the study were already taking a minimum of three blood pressure medicines at maximum tolerated doses, however this had failed to bring the condition down to target levels.
Among those whose arteries were treated, systolic blood pressure was 14 mm Hg lower six months following the treatment, versus 12 mm HG lower among the 171 who had a renal angiogram but not the denervation procedure. Furthermore, no major difference in the drop in 24-hour ambulatory systolic blood pressure was noted. It declined 7 mm Hg with treatment and 5 mm Hg in the sham group.
Nina Goodheart, head of renal denervation for Medtronic, declared the company remained convinced that so far, resistant hypertension was a large medical un-met need and that renal denervation provided a promising opportunity. Planning to collaborate with the US Food and Drug Administration in order to establish its Symplicity system, Medtronic intends to carry on providing access to it in countries where it is approved.
While saying further clinical investigation was warranted, the company will halt a follow-up study that had been suspended, and consult with local regulators to decide the future of trials in Japan and India.
Bhatt believed that this type of randomized, blinded trial done with sham controls for medical devices questioned a lot of things previously thought of as effective, and he added that the researchers still hoped a variant of the technique might be useful. Their plans include following the patients for up to five years to see if the treatment shows a delayed benefit.
Acknowledging the negative outcome of this clinical trial, Bhatt expressed his concern that this could signal an end to the field of renal denervation, noting that previously used animal studies, clinical data and surgery showed the disruption of nerves between the kidney and the heart leading to lower blood pressure.
Due to the consequence of drastic side effects in earlier surgeries it was abandoned. Bhatt expressed hope it would one day be possible to identify the ideal point between those two extremes which would potentially allow the delivery of enough energy to denervate without negative surgery side effects, producing a clinically meaningful effect on blood pressure.
Source: Reuters
Image source: Google Images
4 April 2014
Latest Articles
kidney, Surgery, Patient, Renal, high blood pressure, renal therapies, antiplatelet therapy, artery, blood pressure
A recent study, presented at the meeting of the American College of Cardiology (ACC) in Washington and published by the New England Journal of Medicine, ha...