More than half the patients admitted to a Los Angeles ICU could have been cared for in more appropriate settings, according to a research letter published today in JAMA Internal Medicine. Corresponding author, Dong W. Chang, MD, told ICU Management & Practice in an email that while these results are likely to vary among hospitals, the issue of ICU over-utilisation will resonate with most ICU practitioners.
Chang and colleagues conducted the study based on the overall impression that ICU care is often delivered to patients who are unlikely to derive long-term benefit. They were surprised by the magnitude of the problem, however. Equally concerning was that a substantial percentage of patients were admitted to the ICU for aggressive care even in the setting of progressive irreversible medical conditions, like advanced cancer or dementia.
See Also: High ICU Usage Increases Invasive Procedures, Costs
For 808 admissions to the ICU at Harbor-UCLA Medical Center between 1 July 2015 until 15 Jun 2016, the researchers totalled the number of days each patient spent in the ICU and found that nearly 65% of the total number of days those patients spent in ICU were allocated to care that was considered discretionary monitoring, had a low likelihood of benefit despite critical illness or would have been manageable in non-ICU settings. They categorised admissions according to the latest Society of Critical Care Medicine (SCCM) admission, discharge and triage guidelines.
Results
- 46.9% were categorised as priority 1 (critically ill, needing intensive treatment and monitoring that cannot be provided outside of ICUs)
- 23.4% required close monitoring but not ICU-level care (priority 2)
- 20.9% of the patients were critically ill but unlikely to recover because they had underlying illnesses or severity of acute illness (priority 3)
- 8% were dying or the same outcomes were expected in non-ICU care (priority 4)
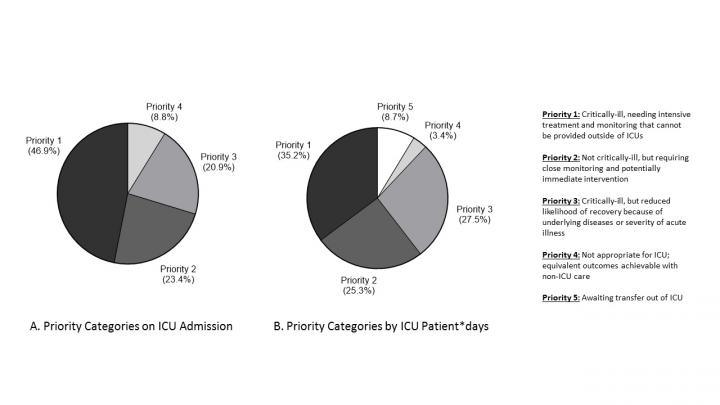
Of the priority 3 patients, the researchers found that 26% had advanced cancer and 27.2% had advanced dementia, suggesting that many patients in this priority group were at risk for receiving inappropriate, aggressive ICU care.
The researchers acknowledge that evaluating appropriateness of ICU care is complex, as it also needs to take into account patient and family preferences, ICU resource availability and type of monitoring available in non-ICU settings.
Next Steps
Chang commented that for many physicians it is reflexive to admit patients who are very ill to the ICU. “However, as a medical community we have to recognise that for some patients this results in no substantial long-term clinical benefit at best, and invasive treatments that can be harmful at worst. We need to identify such patients, discuss options carefully with patients and their families, and show clinical restraint regarding invasive ICU care when appropriate. Hopefully, our study will facilitate other institutions’ efforts to examine their ICU use and develop interventions to improve utilisation.Chang added that they plan to focus efforts on improving ICU utilisation among those patients with advanced medical conditions who are unlikely to benefit from ICU care (priority 3 in the study).
“We are examining why patients with such advanced medical illnesses are receiving invasive treatments and identifying interventions to optimise this element of ICU care. As an example, we are exploring ways to improve communications between patients/surrogate decision-makers and care providers to make sure that the care we deliver aligns with patients' preferences and to unify goals and expectations for ICU care.”
Source: LA Biomed
Image credits: top image - Pixabay, middle image - LA Biomed
References:
Chang DW, Dacosta D, Shapiro MJ (2016) Priority levels in medical intensive care in an academic public hospital. JAMA Intern Med,
published online Dec 27. E1-2.
Latest Articles
ICU, admissions, triage, severity of illness
More than half the patients admitted to a Los Angeles ICU could have been cared for in more appropriate settings, according to a research letter published today in JAMA Internal Medicine. Corresponding author, Dong W. Chang, MD, told ICU Management & Pra










