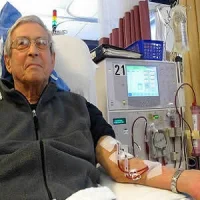
A clear answer for the optimal timing of RRT in critical illness remains elusive, say the authors of a systematic review published in Critical Care. They recommend that clinicians refrain from lowering their clinical thresholds for implementing RRT in critical care patients with acute renal injury.
Studies on the timing of renal replacement therapy (RRT) for acute kidney injury (AKI) and effect on mortality at 1 month and hospital and ICU length of stay (LOS) were analysed by Benjamin T. Wierstra, Division of Internal Medicine, Department of Medicine, University of Calgary, and colleagues. Nine studies (1024) patients were judged to be of sufficient quality from a literature search of research published between January 1985 and November 2015. The authors explain that they excluded data from cohort trials where there were methodological shortcomings that predisposed them to find an effect misattributed to the intervention. Their analysis used ‘early’ as defined by the authors of the studies included.
No survival advantage was found with “early” RRT among high-quality studies with an OR of 0.665 (95 % CI 0.384–1.153, p = 0.146). The authors explain that they found that most of the data that support "early" RRT was in the pooled low-quality studies. Subgroup analysis by reason for ICU admission (surgical/medical) or definition of “early” (time/biochemical) showed no evidence of survival advantage. No significant differences were observed in ICU or hospital LOS in the high-quality studies. They conclude that on the basis of the research evaluated the optimal timing for initiation of RRT is not clarified.
This analysis did not concur with the conclusions of previous meta-analyses, write the authors, who add that their conclusions build on the concerns raised by previous meta-analyses that the results of cohort trials that favoured “early” RRT were not reproduced in randomised controlled trials. They explain that prior meta-analyses relied heavily on retrospective cohort study data that possessed incomplete preintervention data or preexisting significant differences in groups which predisposed the investigators to identify a survival difference attributed to “early” RRT that may have been accounted for by the preintervention population differences.
Image credit: freeimages.com
Studies on the timing of renal replacement therapy (RRT) for acute kidney injury (AKI) and effect on mortality at 1 month and hospital and ICU length of stay (LOS) were analysed by Benjamin T. Wierstra, Division of Internal Medicine, Department of Medicine, University of Calgary, and colleagues. Nine studies (1024) patients were judged to be of sufficient quality from a literature search of research published between January 1985 and November 2015. The authors explain that they excluded data from cohort trials where there were methodological shortcomings that predisposed them to find an effect misattributed to the intervention. Their analysis used ‘early’ as defined by the authors of the studies included.
Findings
No survival advantage was found with “early” RRT among high-quality studies with an OR of 0.665 (95 % CI 0.384–1.153, p = 0.146). The authors explain that they found that most of the data that support "early" RRT was in the pooled low-quality studies. Subgroup analysis by reason for ICU admission (surgical/medical) or definition of “early” (time/biochemical) showed no evidence of survival advantage. No significant differences were observed in ICU or hospital LOS in the high-quality studies. They conclude that on the basis of the research evaluated the optimal timing for initiation of RRT is not clarified.
This analysis did not concur with the conclusions of previous meta-analyses, write the authors, who add that their conclusions build on the concerns raised by previous meta-analyses that the results of cohort trials that favoured “early” RRT were not reproduced in randomised controlled trials. They explain that prior meta-analyses relied heavily on retrospective cohort study data that possessed incomplete preintervention data or preexisting significant differences in groups which predisposed the investigators to identify a survival difference attributed to “early” RRT that may have been accounted for by the preintervention population differences.
Image credit: freeimages.com
References:
Wierstra BT, Kadri S, Alomar S, Burbano X, Barrisford GW, Kao RL
(2016) The impact of "early" versus "late" initiation of renal replacement therapy in critical care patients with acute kidney injury: a systematic review and evidence synthesis. Crit Care, 20(1): 122. doi:
10.1186/s13054-016-1291-8.
Latest Articles
renal replacement therapy, timing, acute kidney injury
A clear answer for the optimal timing of RRT in critical illness remains elusive, say the authors of a systematic review published in Critical Care. They recommend that clinicians refrain from lowering their clinical thresholds for implementing RRT in cri