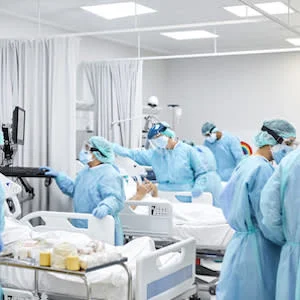
Sedation management is a critical component when managing mechanically ventilated patients. It is important to use a protocol-driven approach, which favours paired spontaneous awakening (SAT) and breathing (SBT) trials, along with light levels of sedation. The initial period of respiratory failure in the emergency department and the first 48 hours in the ICU are critical to ensure reduced overall time the patient spends under deep sedation and coma.
During the COVID-19 pandemic, mechanically ventilated patients have experienced longer periods of deep sedation. Studies from the pre-COVID era suggest that early deep sedation is associated with worse outcomes. However, there is still a lack of data on the depth of sedation and its impact on outcomes in mechanically ventilated COVID-19 patients.
Early sedation depth is an important contributor to outcomes in mechanically ventilated patients. Several studies demonstrate that deep sedation during the first 48 hours of mechanical ventilation is associated with increased duration of mechanical ventilation, higher mortality, greater incidence of delirium and longer length of stay.
In the COVID-SED study, researchers characterise the emergency department and ICU sedation practices during the pandemic to determine if early deep sedation is associated with worse clinical outcomes. The study included 391 mechanically ventilated patients. Sedation-related data was collected during the first 48 hours. Deep sedation was defined as a median RASS of − 3 to − 5; or median SAS of 1–3. The primary outcome of the study was hospital mortality. Secondary outcomes included ventilator-, ICU-, and hospital-free days. The deeply sedated patient group had a higher proportion of patients with COVID-19 and lower partial pressure of arterial oxygenation to fraction of inspired oxygen ratio.
72.4% of patients experienced early deep sedation. They received higher doses of fentanyl, propofol, midazolam, and ketamine than those who received light sedation. Early deep sedation persisted throughout the first week of mechanical ventilation and was negatively associated with outcome.
Results show that deep sedation patients experienced fewer ventilator-, ICU-and hospital-free days and greater mortality (30.4% versus 11.1%) compared to light sedation. Early deep sedation was significantly associated with higher mortality. These results were stable in the subgroup of patients with COVID-19.
These findings show that early deep sedation is independently associated with worse clinical outcomes. It is thus important to use a protocol-driven approach to sedation, targeting light sedation as early as possible, regardless of COVID-19 status.
Source: Critical Care
Image Credit: iStock