COVID-19 associated ARDS is associated with high mortality risk. Many patients with COVID-19 have been admitted with pneumonia and arterial hypoxaemia, increased work of breathing or impending fatigue. It is a common clinical practice to intubate patients with severe hypoxaemia. However, during the pandemic, there was a high demand for ICU beds. Therefore, some experts recommended a more conservative approach and promoted the use of high flow nasal cannula (HFNC) or non-invasive ventilation while the patient is in an awake prone position.
A study was conducted to determine whether time-to-intubation was associated with higher ICU mortality in patients with COVID-19 on mechanical ventilation due to respiratory insufficiency. The researchers hypothesised that later intubation was associated with worse outcomes than early intubation in patients with COVID-19.
One hundred and eighty-three patients with confirmed SARS-CoV-2 infection and hospitalised with moderate to severe ARDS and on mechanical ventilation were included in the study. Time to intubation was defined as the time from admission to the hospital to endotracheal intubation.
The primary outcome of the study was ICU death. Secondary outcomes included duration of mechanical ventilation, length of stay in hospital and ICU, and mortality on day 28 and on discharge from the ICU.
Time of intubation was classified as early (<48 hours) or late (≥48 hours). 48% of the patients were intubated before 48 hours, and 52% were intubated after.
The main finding of the study was that among hospitalised patients with COVID-19, intubation after 48 hours of hospital admission and PaO2/FiO2 ratio on admission <100 mmHg was associated with increased mortality. In particular, COVID-19 patients over the age of 60 and admitted with a PaO2/FiO2 ratio <100 mmHg may have a higher risk of ICU mortality when intubated after 48 hours. Also, patients admitted with PaO2/FiO2<100 mmHg and intubated after 48 hours may have worse lung mechanics than patients intubated before 48 hours.
Overall, findings from this study show that the time to intubation may be associated with an increase in mortality in hypoxaemic patients with COVID-19. Late intubation, older age, and previous use of ACE inhibitors were associated with increased ICU mortality.
Source: Journal of Critical Care
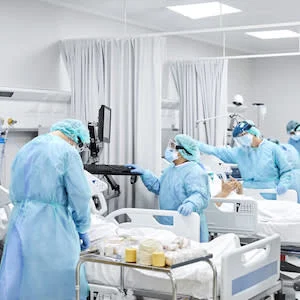
Image Credit: iStock
References:
Vera M et al. (2021) Intubation timing as determinant of outcome in patients with acute respiratory distress syndrome by SARS-CoV-2 infection. Journal of Critical Care. 65:164-169. doi.org/10.1016/j.jcrc.2021.06.008