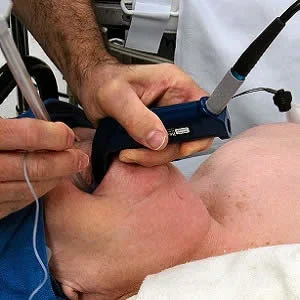
The optimal timing of endotracheal intubation in critically ill patients requiring invasive mechanical ventilation remains undefined. A new analysis of the large, prospective Intensive Care Over Nations (ICON) database compares patients who underwent intubation early – within two days of ICU admission – to those who underwent intubation later. Results show that later intubation (after two days) was associated with a greater hazard of death after 10 days of ICU stay than early intubation.
Whether or not delaying intubation could impact outcome in critically ill patients is not well defined. Delayed intubation can contribute to acute hypoxemic respiratory failure (ARF) in case of aspiration. Failure of non-invasive ventilation is predictable, especially in patients with ARF combined with shock, marked metabolic acidosis, high illness severity scores, and greater degrees of hypoxemia.
Notwithstanding the risk of intubation itself, which may include cardiac arrest, tracheal injury, ventilator-associated complications and the need for sedation, early intubation may exert a protective effect by controlling tidal volume, plateau pressure, loaded breathing and by supporting myocardial function (decreased left ventricular afterload and better oxygen supply), while influencing body position, and limiting or preventing compression atelectasis especially in obese patients.
Researchers analysed data of 4,729 patients, of whom 4,074 never underwent intubation. Of the remaining 655 patients, 449 underwent intubation early and 206 later. Despite similar severity scores on ICU admission, unadjusted ICU and hospital mortality rates were higher in patients intubated later than in those intubated earlier, as were ICU and hospital lengths-of-stay. After adjustment, the hazard for ICU and hospital death was significantly greater 10 days after ICU admission for patients intubated late.
"Mechanistically, our results suggest that the timing of intubation in patients worldwide is apposite to clinical requirements. When factors related to the use of early intubation were accounted for, the hazard for death was higher >10 days after ICU admission in those intubated late. The reason for this difference is not clear. Both groups, early and late intubation, were similar at admission, including in terms of severity and organ failure, with the exception that patients who underwent intubation late were more often admitted from the floor and less often from the emergency room than patients intubated early," the authors write.
In addition, the findings suggest that the timing of intubation may itself be a prognostic factor and close monitoring of critically ill patients with frequent reassessment for the need for intubation may be warranted, especially after the first 48 hours of ICU admission, according to the authors.
The study has several limitations, including its observational nature. Also, the precision of the timing of intubation was limited to calendar days and a more refined distribution of the timeframe of intubation could not be established.
Source: Journal of Critical Care
Image Credit: DiverDave
References:
Bauer, Philippe R. et al. (2017) Association between timing of intubation and outcome in critically ill patients: A secondary analysis of the ICON audit. Journal of Critical Care. doi.org/10.1016/j.jcrc.2017.06.010
Latest Articles
ICU, Delayed Intubation, early intubation, endotracheal intubation
A new analysis of the large, prospective Intensive Care Over Nations (ICON) database compares patients who underwent intubation early – within two days of ICU admission – to those who underwent intubation later. Results show that later intubation (after t