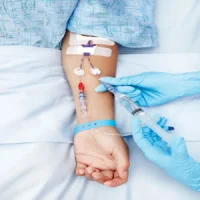
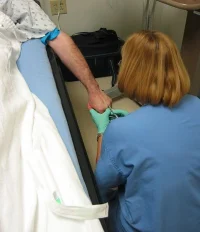
The intensive care unit (ICU) is an ethically charged environment: life and death decisions are made daily. Particularly when medical criteria alone are insufficient in deciding what is the right thing to do, healthcare professionals can be faced with an ethical dilemma. For example, deciding whether to discharge a patient not quite ready for the general ward to create bed space for a gravely ill patient in need of intensive care.
To provide insight into ethical problems that influence the ICU admission and discharge process, this study aimed to identify and explore ethical dilemmas healthcare professionals are faced with.
"What became clear from our study was the difference between the ICU and the general ward, and its role in the emergence and mitigation of ethical problems. Care in the ICU is more highly technological and more intensive than in the general ward – ICU personnel are more technically skilled than nurses in the general ward," according to Anke Oerlemans and colleagues at Radboud University Medical Center (the Netherlands).
The findings, published in BMC Medical Ethics, indicate that when professionals of different wards feel there is a collective effort to solve a problem and a shared responsibility towards achieving the best possible care for the patient(s) in question, this helps to prevent or alleviate moral distress.
Methodology
This was an explorative, descriptive study using qualitative methods (individual and focus group interviews). The researchers conducted 19 individual interviews and 4 focus group interviews with nurses and physicians working in the ICU or the general ward (regularly admitting post-ICU patients) of 10 Dutch hospitals.
Audio of the interviews was recorded and subsequently transcribed verbatim. The interview and focus group transcripts were coded using ATLAS.ti 6.2. The analysis was conducted using a grounded theory approach, in which the codes and codebook emerge from the data (as opposed to previously formulated hypotheses which are “tested” against qualitative data).
Results and Discussion
The ethical problems in the context of ICU admission and discharge can be divided into problems concerning full bed occupancy and problems related to treatment decisions. Ethical problems connected to full bed occupancy have in common the weighing of interests (and risks and benefits) of two (or more) patients against each other: delay of ICU care for patient A means that patient B benefits from the care he needs, or a transport risk and the inconvenience of a different hospital for patient C mean that patient D can benefit from timely and adequate care.
The second cluster of ethical problems is related to treatment decisions, more specifically the decision whether to start or to stop ICU treatment. In these dilemmas the central question is what is best for an individual patient — ie, weighing of the risks and benefits of different alternatives for the patient in question.
The different nature of the role of nurses and physicians in the patient’s care leads to differences in how they perceive and deal with ethical problems. Where physicians predominantly act in a cure role and carry decision-making responsibility when it comes to admitting and discharging patients, nurses work from a care perspective and do not have this responsibility.
The gap between the high level of care the ICU can provide and the lower care level in the general ward sometimes leads to mutual misunderstandings: for instance, the ICU staff overestimates the nursing care the general ward can provide, and prematurely discharges patients, substantially increasing the care burden at the general ward.
ICU patients’ wishes are often unknown, causing healthcare professionals to err on the side of more treatment. Additionally, the highly technological nature of intensive care appears to encourage over-treatment.
Conclusions
The nature of the ICU environment makes it important for healthcare professionals to be aware of the risk of over-treatment, reflect on why they do what they do, and be mindful of a possible negative impact of over-treatment on their patients. Early discussion of a patient’s wishes with regard to treatment options is important in preventing over-treatment.
It is important for ICUs and general wards to cooperate well, since there is a mutual dependency for optimal patient flow between the different departments. Interventions that improve the understanding and cooperation between these wards may help mitigate ethical problems.
Image Credit: NHS (Wales) UK
To provide insight into ethical problems that influence the ICU admission and discharge process, this study aimed to identify and explore ethical dilemmas healthcare professionals are faced with.
"What became clear from our study was the difference between the ICU and the general ward, and its role in the emergence and mitigation of ethical problems. Care in the ICU is more highly technological and more intensive than in the general ward – ICU personnel are more technically skilled than nurses in the general ward," according to Anke Oerlemans and colleagues at Radboud University Medical Center (the Netherlands).
The findings, published in BMC Medical Ethics, indicate that when professionals of different wards feel there is a collective effort to solve a problem and a shared responsibility towards achieving the best possible care for the patient(s) in question, this helps to prevent or alleviate moral distress.
Methodology
This was an explorative, descriptive study using qualitative methods (individual and focus group interviews). The researchers conducted 19 individual interviews and 4 focus group interviews with nurses and physicians working in the ICU or the general ward (regularly admitting post-ICU patients) of 10 Dutch hospitals.
Audio of the interviews was recorded and subsequently transcribed verbatim. The interview and focus group transcripts were coded using ATLAS.ti 6.2. The analysis was conducted using a grounded theory approach, in which the codes and codebook emerge from the data (as opposed to previously formulated hypotheses which are “tested” against qualitative data).
Results and Discussion
The ethical problems in the context of ICU admission and discharge can be divided into problems concerning full bed occupancy and problems related to treatment decisions. Ethical problems connected to full bed occupancy have in common the weighing of interests (and risks and benefits) of two (or more) patients against each other: delay of ICU care for patient A means that patient B benefits from the care he needs, or a transport risk and the inconvenience of a different hospital for patient C mean that patient D can benefit from timely and adequate care.
The second cluster of ethical problems is related to treatment decisions, more specifically the decision whether to start or to stop ICU treatment. In these dilemmas the central question is what is best for an individual patient — ie, weighing of the risks and benefits of different alternatives for the patient in question.
The different nature of the role of nurses and physicians in the patient’s care leads to differences in how they perceive and deal with ethical problems. Where physicians predominantly act in a cure role and carry decision-making responsibility when it comes to admitting and discharging patients, nurses work from a care perspective and do not have this responsibility.
The gap between the high level of care the ICU can provide and the lower care level in the general ward sometimes leads to mutual misunderstandings: for instance, the ICU staff overestimates the nursing care the general ward can provide, and prematurely discharges patients, substantially increasing the care burden at the general ward.
ICU patients’ wishes are often unknown, causing healthcare professionals to err on the side of more treatment. Additionally, the highly technological nature of intensive care appears to encourage over-treatment.
Conclusions
The nature of the ICU environment makes it important for healthcare professionals to be aware of the risk of over-treatment, reflect on why they do what they do, and be mindful of a possible negative impact of over-treatment on their patients. Early discussion of a patient’s wishes with regard to treatment options is important in preventing over-treatment.
It is important for ICUs and general wards to cooperate well, since there is a mutual dependency for optimal patient flow between the different departments. Interventions that improve the understanding and cooperation between these wards may help mitigate ethical problems.
Image Credit: NHS (Wales) UK
References:
Oerlemans AJM, Van Sluisveld N et al. (2015) Ethical problems in intensive care unit admission and discharge decisions: a qualitative study among physicians and nurses in the Netherlands. BMC Medical Ethics
2015, 16:9 doi:10.1186/s12910-015-0001-4
Latest Articles
ICU, admission, Discharge, ethical problems, general ward, over-treatment
The intensive care unit (ICU) is an ethically charged environment: life and death decisions are made daily. Particularly when medical criteria alone are in...