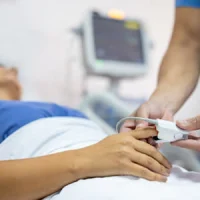
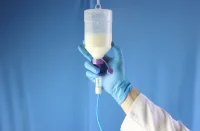
Nutrition in critical illness has become a significant area of focus in recent decades. Initially, early and adequate feeding was believed to enhance outcomes by promptly ensuring the patient reaches full energy target. However, this perspective was challenged after the release of the EPaNIC trial in 2011.
The EPaNIC trial observed worse outcomes in patients who received early supplemental parenteral nutrition (PN), leading to the belief that PN was the cause. As a result, there was a sudden decrease in the use of PN in clinical practice and guidelines recommended against its use. However, subsequent evidence has accumulated, indicating that providing nutrition to reach the full energy target, regardless of the delivery route, is harmful rather than beneficial. This suggests that either the energy needs of patients are being overestimated the energy or there is a biological advantage associated with underfeeding.
Several studies have investigated potential biological mechanisms to explain this finding. These mechanisms include increased endogenous energy supply independent of exogenous energy provision and suppressing autophagy with nutrition. In addition, numerous large clinical studies and meta-analyses have been conducted in recent years, exploring nutrition through different routes and at various doses, challenging previous understanding of nutrition provision in early critical illness.
This narrative review summarises the latest research on the route and dosage of nutrition and studies on explanatory mechanisms. It offers an interpretation of the available evidence from the perspectives of basic scientists, dietitians, and intensivists. Moreover, the review provides collective suggestions for clinical practice and highlights the need for future research in this field.
The review discusses several key findings from recent randomised controlled trials. One trial found that patients receiving a lower calorie intake of 6 kcal/kg/day compared to 25 kcal/kg/day achieved readiness for ICU discharge earlier and experienced fewer gastrointestinal complications. Another trial indicated that high protein dosage might harm patients with pre-existing acute kidney injury and more severe illness. Lastly, a prospective observational study suggested that early full feeding, particularly through enteral means, is associated with higher 28-day mortality compared to delayed feeding.
The viewpoints of basic scientists, critical care dietitians, and intensivists converge on the agreement that early full feeding is likely detrimental in critically ill patients. However, several important questions remain unanswered, including the mechanisms of harm and the optimal timing and dosage of nutrition for individual patients. Future studies are needed to address these gaps. In the meantime, it is suggested to provide a low dose of energy and protein during the initial days in the ICU, followed by an individualised approach based on the assumed metabolic state determined by the trajectory of the illness. Additionally, there is a need for research to develop improved tools for accurately and continuously monitoring the metabolism and the nutritional requirements of individual patients.
Source: Critical Care
Image Credit: iStock