ICU Management & Practice, Volume 22 - Issue 5, 2022
Critical care ultrasound examination should be considered in specific situations in the intensive care unit. It has become increasingly important to understand and master all the possible applications and future innovations of ultrasonography in the critical care setting.
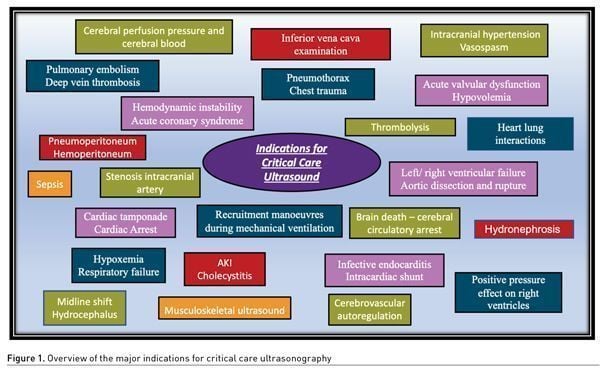
Point of care application of ultrasound has been widely validated as an essential imaging technique in the management of critical care patients (Lou and See 2022). Bedside ultrasonography consents real-time evaluation of the anatomy and function of several organs, allowing a rapid recognition and diagnosis of the major cause of haemodynamic instability in intensive care patients (i.e., hypovolaemia, acute cardiac tamponade, pneumothorax, cardiogenic shock, haemoperitoneum). Even more, as part of acute management of critically ill patients, critical care ultrasound examination should be considered for the study of specific situations encountered in intensive care unit; heart and lung interaction, the effects of mechanical ventilation on central haemodynamic, multiorgan consequences of septic shock, severe multisystem trauma, and intensive care unit-acquired weakness (Guevarra and Greenstein 2020; Vieillard-Baron et al. 2008; Soliman-Aboumarie et al. 2021; Mongodi et al. 2021). In addition to clinical examination, ultrasound can provide intensivists with useful information for quick decision-making and set or change therapeutic strategy, allowing a direct evaluation of the response of a specific treatment. Beside its diagnostic potential, ultrasonography also represents a real-time guidance for several invasive procedures (e.g., tracheostomy, central line insertion, local anaesthesia, intercostal drain insertion) (Saugel et al. 2017; Wong et al. 2020). Consequently, it is essential for intensivists to gain specific training and competence in ultrasonography, following internationally validated curricula (Wong et al. 2020; Expert Round Table on Echocardiography in ICU 2014). An overview of possible indications of ultrasonography in ICU is provided in Figure 1.
Lung Ultrasonography
Lung Ultrasonography (LUS) is a radiation-free, low-cost, rapid, and portable imaging technique, that allows real-time examination of pulmonary structures. LUS is a key component of critical care; it can be used to evaluate patients with acute respiratory failure, titrate mechanical ventilation, guide interventional procedures, and monitor outcomes (Corradi et al. 2014; Luecke et al. 2012; Schmidt et al. 2019; Corradi et al. 2022a; Vezzani et al. 2017). LUS has also played an important role in the management of patients with COVID-19-associated lung injury through the study of the lung parenchyma and the diaphragm (Hussain et al. 2020; Volpicelli et al. 2021; Corradi et al. 2021a; Corradi et al. 2021b).
LUS has recently gained consideration as a useful tool for the assessment of lung pathophysiology. Compared with chest radiography, LUS has shown higher sensitivity and similar specificity for the detection of pleural effusion, pneumonia, pneumothorax, and pulmonary oedema (Vezzani et al. 2014). However, although recognition of B-lines and differentiation between A- and B-pattern are simple tasks also for beginners, the quantification of B-lines and their distance can be challenging (Corradi et al. 2022b). Thus, automatic methods for the detection and quantification of B-lines have been recently proposed to have an objective, operator-independent, automated, and quantitative classification of the severity of pulmonary interstitial syndrome (Weitzel et al. 2015; Brattain et al. 2013; Anantrasirichai et al. 2017).
In 2013, Corradi and co-workers first studied isolated bovine lung to test the hypothesis that extravascular lung water (EVLW) could be reliably quantified by a first order computer-assisted grey-scale LUS analysis, using gravitometry as a gold standard (Corradi et al. 2013). The results showed that quantitative LUS by video grey-scale analysis was more accurate in the estimation of EVLW than visual scoring or quantitative chest Computed Tomography (CT). Most importantly, the study provided further insight into the relationship between B-lines and EVLW, underlining differences between quantitative LUS and quantitative CT as diagnostic tools. The authors observed that mean LUS intensity was strongly correlated with EVLW but weakly with physical density; CT analysis showed opposite results. These data suggest that comparison of quantitative LUS and quantitative CT has the potential to distinguish increased water content from increased tissue content in lung disorders where pulmonary oedema and parenchymal abnormalities may co-exist. Moreover, quantitative LUS was clearly superior to visual scoring in detecting the presence of EVLW; even in case of amounts as small as 16% of initial lung weight. Furthermore, multi-frame video-based was superior to single-frame method, due to the fact that single-frame methods are not sufficient to evaluate the total respiratory cycle.
In patients mechanically ventilated after cardiac surgery (Corradi et al. 2016), the same group of authors also showed that mean echo-intensities were significantly better correlated with the degree of EVLW content than the 28-region-based aeration score. This study also showed that quantitative LUS was superior to visual scoring in the assessment of EVLW with moderate-to-high positive end-expiratory pressure. Indeed, visual scores (progression or regression of abnormal patterns, spaced B-lines, coalescent B-lines, and consolidation) seemed effective in determining large changes in lung aeration (i.e., >600 ml), as those caused by positive end-expiratory pressure used for recruitment manoeuvres in ARDS; however, the accuracy diminished dramatically with milder changes of lung aeration (Bouhemad et al. 2011).
In adults, computer-assisted LUS has been used in a wide array of pulmonary diagnoses. Raso et al. (2015) graded pulmonary fibrosis and lung oedema by computer analysis in two sets of pre-selected patients. Corradi et al. (2015) found that the mean grey-scale intensity, determined by computer-aided grey-scale analysis, was considerably more accurate than either chest x-ray or visual LUS in the diagnosis of community-acquired pneumonia confirmed by CT. This was independent of size and distance from pleural line, presumably owing to more hyper-echogenic images resulting from hypo-aerated lung parenchyma around consolidations. In children, quantitative LUS was used to assess the severity of neonatal respiratory distress, to evaluate foetal lungs for predicting neonatal respiratory morbidity, and to detect pneumonia (Raimondi et al. 2018; Cisneros-Velarde et al. 2016; Bonet-Carne et al. 2015). Finally, an algorithmic approach allowed to clinically validate the most valuable semiquantitative ultrasound score by demonstrating that only the calculation of the percentage of the pleural line, inferred by a transversal approach within the intercostal spaces, correlates with EVLW (Brusasco et al. 2019).
There are still technical advancements that are necessary to make quantitative LUS widely applicable in clinical practice: the inclusion of radio frequency signal data in addition to B-mode image data to provide more detailed ultrasound information and the validation of second order statistics, based on a set of textural features extracted from the grey-level co-occurrence matrix, to make results independent of ultrasound device, parameters, and settings (Brusasco et al. 2022).
Furthermore, there is emerging evidence that local lung strain can be estimated by LUS, thus possibly providing a method for assessing local lung ventilation. Although lung sliding is affected by a variety of lung pathologies, the magnitude of this change was never quantified. It has been suggested that speckle-tracking technology applied in the lung will be able to provide speckle displacement during inspiration and expiration (Dori and Jakobson 2016). This would represent the final step towards the development of an ultrasound protocol suitable as a global ventilatory monitoring tool, also allowing the quantification of pulmonary over-distension.
Critical Care Echocardiography
Critical care echocardiography (CCE) has to be considered something parallel to conventional echocardiography performed by cardiologists, requiring specific knowledge of critical care medicine peculiarities. Ultrasonography in critical care setting requires to be quickly available on 24h basis and to respond to specific clinical questions, not only addressing the heart and great vessel anatomy and physiopathology but also evaluating the tight interaction between heart and lung, the potential consequences of mechanical ventilation on right heart and the possible causes of haemodynamic instability (Soliman-Aboumorie et al. 2021). Consequently, critical care echocardiography demands specific training and competence, following internationally validated curricula (Expert Round Table on Echocardiography in ICU 2014).
Bedside echocardiography allows the assessment of global left ventricular (LV) size and function, the identification of regional wall motions abnormalities, the evaluation of right ventricular (RV) size and function, the estimation of pulmonary pressure, the presence of pericardial effusion, the study of valvular dysfunction and to evaluate hypovolaemic status with dynamics parameter (Longobardo et al. 2018). Consequently, several usual disorders encountered in ICU can be quickly diagnosed and treated. Critical care echocardiography is a fundamental tool for the primary evaluation and differential diagnosis in case of circulatory and respiratory failure, especially when combined with LUS evaluation, and to identify life-threatening causes of shock and cardiac arrest (Long et al. 2018; Price et al. 2010; Chou et al. 2020). Noteworthy, ultrasonography may help in the differential diagnosis of the cause of shock in haemodynamic unstable patients, detecting pericardial tamponade, aortic dissection, hypovolaemia, and regional or global LV dysfunction (Yamamoto 2014). Even more, echography findings of right ventricles overload and dysfunction may be also looked at carefully in this setting. Indeed, right ventricular dysfunction can be due to a concomitant cardiac or respiratory disease. However, the findings of right heart overload or dysfunction in a haemodynamic unstable patient always raises suspicions of possible pulmonary embolism (Daley et al. 2019). In this group of patients, CT angiography is generally not feasible, consequently, ultrasound can provide important diagnostic information in order to carry out the diagnosis. The combination of several echography findings such as the 60/60 sign and the McConnell’s sign in addition to right ventricle dilatation/dysfunction, septal flattening and RV/LV ratio alteration is highly suggestive of a diagnosis of pulmonary embolism (Konstantinides et al. 2020). Other important findings are represented by the direct visualisation of free-floating right heart thrombus or direct visualisation of deep venous thrombus during compression ultrasonography.
Echocardiography plays an interesting role also in the evaluation of septic patients (Vallabhajosyula et al. 2020). Common features of these patients are represented by potentially reversible myocardial depression, hypovolaemia, and altered vascular tone. Critical care echocardiography, evaluating central haemodynamic and heart, consents to guide management and directly evaluate the effect of therapy. The ultrasonographic evaluation must focus on evaluating cardiac output, cardiac contractility, and fluid responsiveness. Indeed, echocardiographic methods may help intensivists to determine the need for inotrope and fluid infusion (Shrestha and Srinivasan 2018; Guérin and Vieillard-Baron 2016). Dynamic parameters are used to predict a positive response to fluid. In mechanically ventilated patients and in sinus rhythm, distensibility index of IVC and the respiratory of aortic blood flow are generally preferred.
With CCE, it is also possible to evaluate the diastolic function, although it requires a more advanced use. This is particularly important to define the tolerance to fluid administration: identifying ventricles that display a restrictive pattern (the most advanced form of diastolic dysfunction) may alert clinicians about the risk of pulmonary oedema/congestion with generous fluid resuscitation. Similarly, by analysing the doppler pattern of the hepatic, portal and renal veins (VeXUS score), it is possible to identify various degree of venous congestion.
During cardiopulmonary resuscitation, current guidelines recommend performing CCE, due to the important information that can be gained from this imaging technique. CCE allows to exclude treatable and reversible causes of cardiac arrest without interfering advanced life support protocols (i.e., cardiac tamponade, pulmonary embolism, tension pneumothorax, and hypovolaemia) and to guide consequent invasive procedures (i.e., pericardiocentesis, decompression of tension pneumothorax) improving the safety and efficacy of these interventions (Price et al. 2010; Balderston et al. 2021). Even more, CCE allows the evaluation of the quality of compression (direct and real-time evaluation of compression and relaxation of ventricles) and permits to discriminate true asystole from fine ventricular fibrillation; conditions with different therapeutic approaches. Echocardiography can permit to differentiate patients with pulseless electrical activity (PEA) without cardiac contractile activity (True-PEA) from patients in PEA but who still have cardiac contractile activity (False-PEA); an important prognostic data. Indeed, patients with false-PEA were more likely to have a Return of Spontaneous Circulation (ROSC) (Wu et al. 2018; Gaspari et al. 2021). Moreover, critical care echocardiography, both transthoracic (TTE) and transoesophageal approach (TEE), are fundamental for the management of veno-arterial ECMO in extracorporeal life support (ECLS) programme; from cannula insertion, maintenance, to weaning (Donker et al. 2018). Echocardiography represents a dominant bedside tool allowing disorder valuation, treatment optimisation, and weaning of extracorporeal treatment (Douflé and Ferguson 2016). Possible benefits of CCE during V-A ECMO are represented but not limited to evaluation of arterial and venous puncture size, the choice of peripheral or central ECLS, the presence of thrombus and the evaluation of vessel size, the correct placement of the cannula, the evaluation of the underlying cardiac condition and to evaluate optimal unloading of ventricles (Platts et al. 2012).
It is also worth highlighting the use of TEE in critical care settings. TEE represents another ultrasonography cardiovascular imaging modality (Prager et al. 2022). It requires the insertion of a flexible probe down into the oesophagus; consequently, the transducer’s proximity to the heart and great vessel provides a good ultrasonic window (Peterson et al. 2003). TEE is generally performed when transthoracic approach is not diagnostic or feasible. Indeed, transthoracic ultrasound transmission can be altered by several confounding factors resulting in scarce image quality; hyperinflation, emphysema, pneumothorax, chronic obstructive pulmonary disease, obesity, chest wall injuries, or dressing tubing. Even more, TEE can allow the evaluation of structures typically difficult to evaluate with TTE such as the aorta, and left atrial appendage, and provide a superior evaluation of prosthetic heart valves and paravalvular leak and regurgitation, the evaluation of paravalvular abscesses and valvular endocarditis (Lengyel 1997; Michelena et al. 2010). TEE is generally performed during cardiac surgery, with precise procedural indications; evaluation of cardiac structure and function before cardiopulmonary bypass (CPB), monitoring of weaning from CPB, evaluation of surgical repairs and possible complications after CPB. Additionally, TEE finds indications during several haemodynamic and interventional procedures (e.g., percutaneous aortic valve implant, left atrial appendage closure, percutaneous closure of permeable oval foramen, and septal defect closure) (Hahn et al. 2014). Unfortunately, TEE is not widely available in the general intensive care unit.
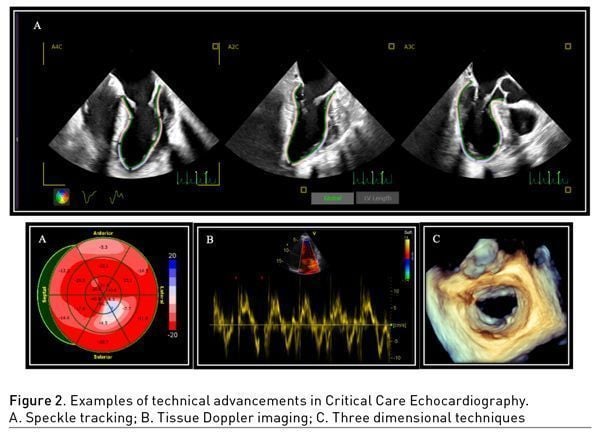
There are attractive future technical advancements in CCE (e.g., three-dimensional techniques, speckle tracking, tissue Doppler imaging, intracardiac echo (Figure 2) (Cinotti et al. 2015; Orde et al. 2018; Poelaert and Roosens 2007). Speckle tracking is a relatively new and very interesting technique for the evaluation of myocardial motion wall abnormalities and dyssynchrony. It requires specific software able to track frame to frame the motion through the cardiac cycle in multiple directions. Speckle tracking measurements are extremely useful in the assessment of myocardial contractility, left ventricular dysfunction, and filling pressures, allowing a two-dimensional non-Doppler angle-independent objective analysis of myocardial deformation. Consequently, deformation imaging analysis allows quantifying the thickening, the longitudinal and circumferential shortening of cardiac cycle. Finally, 3D echocardiography represents a useful diagnostic analysis for quantifying complex geometric shape volumes in multiplanes mode, allowing an accurate evaluation of cardiac chamber volumes and valvular anatomy. Unfortunately, 3D echocardiography requires significant offline data processing, and it is, at the present time, not commonly available in general intensive care units (unlike cardiovascular anaesthesia and cardiothoracic ICU).
Musculoskeletal Ultrasound
Intensive care unit-acquired weakness (ICUAW) represents a severe complication encountered in the intensive care unit (ICU). Muscular weakness is the direct consequence of critical illness polyneuropathy (CIP) and/or critical illness myopathy (CIM). The pathophysiological mechanisms are complex and not entirely understood; however, it seems that the synergism of metabolism, inflammation and immunity play a crucial role. Even more, weakness is also associated with medications (e.g., glucocorticoids), nutritional status, and prolonged muscular immobilisation (De Jonghe et al. 2022). Diagnosis is reached with clinical examination and electrophysiological tests (rarely with muscle biopsies). Muscle ultrasound can potentially play an interesting role to investigate muscle changes over time after admission in ICU. Long-term outcomes in heterogeneous ICUAW populations include transient disability in 30% of patients and persistent disabilities that may occur even in patients with nearly complete functional recovery (Formenti et al. 2019).
Muscular ultrasonography allows visualisation and classification of muscle characteristics by cross-sectional area, muscle layer thickness, echointensity by greyscale and the pennation angle. Healthy muscle tissue has a distinctive appearance by ultrasound: in axial images, muscle consists of primarily echolucent (dark) areas interspersed with small, bright, curved echoes of seemingly random orientations. In the sagittal plane, however, these bright echoes are seen to be the fibrous tissue that surrounds muscle fibres and fascicles and is recognisable as striations. Bipennate muscles present a central area of thickened fibrous tissue (central aponeurosis). If followed distally, this structure becomes the tendon. Except for visible arterial pulsations, healthy muscle is static at rest. However, with slow contraction, the central portion of the muscle can be seen to bulge with thinning of its more distal ends (Walker 2004).
Ultrasound may potentially detect the presence of chronic pathologic changes in muscle and measure its dimensions. Common features of critical illness myopathy and critical illness polyneuropathy include symmetric, flaccid limb weakness and ventilatory muscle weakness. Tendon reflexes are often reduced, especially with CIP.
Four main findings distinguish diseased muscle from healthy muscle: increased echogenicity, atrophy, increased homogeneity, and loss of bone shadow (Turton et al. 2016). Ultrasound parameters used to evaluate muscle architecture are:
- Cross-sectional area (CSA): Determined by the number and size of individual fibres within a muscle. The term ‘muscle architecture’ (parallel or pennate) refers to the physical arrangement of muscle fibres at the macroscopic level and determines the muscle’s mechanical function. In a parallel muscle, the two CSAs coincide, as the fibres are parallel to the longitudinal axis; in pennate muscles, both areas may be used to describe the contraction properties. Muscle atrophy mainly affects type II fibres rather than a relatively equal loss of slow and fast fibres, resulting in the denervation/re-innervation process.
- Muscle layer thickness: Easily identifiable with ultrasound, it has been shown that muscle loss in ICU patients could be monitored by thickness measurements, and it significantly correlates with CSA; however, its predictivity has not been proven in intensive care patients.
- Echointensity: Measure of the image greyscale, reflects the muscle’s composition. Increased echogenicity indicates more homogenous muscle. Ultrasonic echogenicity can be graded according to a score that classifies ultrasonic echogenicity semi-quantitatively into four levels, with higher grades corresponding to increased severity of muscle impairment.
- Pennation angle: The angle of insertion of muscle fibres into the aponeurosis. This angle provides information about muscle strength. A higher pennation angle correlates with a muscle’s capacity to generate force (Formenti et al. 2019).
Many studies, examining the association between muscle weakness and clinical outcomes have shown muscle weakness as an independent predictor of mortality, increased ventilator-dependent time, and prolonged ICU length of stay (De Jonghe et al. 2002; Sharshar et al. 2009; Ali et al. 2008).
Ideally, within the first 48h after admission to the ICU, the first muscular ultrasound assessment should be performed to define a baseline picture of the quadriceps muscle. At the same time, strength evaluation, using validated tools such as the Medical Research Council (MRC) scale should be also performed as soon as cognitive impairment allows. However, impaired mental status or a low MRC score dictates the need for additional examination for ICUAW, with the aim of preventing muscle weakness; in this case, serial revaluations by muscular ultrasound may represent a valuable aid. In this regard, reductions of 20% in muscle thickness, 10% of CSA, 5% in pennation angle, and an increment in echointensity of at least 8% seem reasonable indicators of ICUAW (Formenti et al. 2019).
Conclusion
Due to the complexity of critical care patients and the often difficult and limited possibility of clinical examination, imaging is playing an increasingly important role to help clinicians diagnose and monitor treatment at the bedside. Among all the different imaging techniques available nowadays, ultrasound can provide intensivists with a round-the-clock assessment of critically ill patients. Understandably, the medical history, clinical setting and therapies must be integrated into the medical assessment. However, it is important to highlight that specific training and a well-defined curriculum to achieve professional competence are warranted. Consequently, it has become increasingly important to understand and master all the possible applications and future innovations of ultrasonography in the critical care setting.
Conflict of Interest
None.
References:
Ali NA, O'Brien JM Jr., Hoffmann SP et al. (2008) Acquired weakness, handgrip strength, and mortality in critically ill patients. Am J Respir Crit Care Med. 178(3):261-8.
Anantrasirichai N, Hayes W, Allinovi M et al. (2017) Line Detection as an Inverse Problem: Application to Lung Ultrasound Imaging. IEEE Trans Med Imaging. 36(10):2045-56.
Balderston JR, You AX, Evans DP et al. (2021) Feasibility of focused cardiac ultrasound during cardiac arrest in the emergency department. Cardiovasc Ultrasound. 19(1):19.
Bonet-Carne E, Palacio M, Cobo T et al. (2015) Quantitative ultrasound texture analysis of fetal lungs to predict neonatal respiratory morbidity. Ultrasound Obstet Gynecol. 45(4):427-33.
Bouhemad B, Brisson H, Le-Guen M et al. (2011) Bedside ultrasound assessment of positive end-expiratory pressure-induced lung recruitment. Am J Respir Crit Care Med. 183(3):341-7.
Brattain LJ, Telfer BA, Liteplo AS, Noble VE (2013) Automated B-line scoring on thoracic sonography. J Ultrasound Med. 32(12):2185-90.
Brusasco C, Santori G, Bruzzo E et al. (2019) Quantitative lung ultrasonography: a putative new algorithm for automatic detection and quantification of B-lines. Crit Care. 23(1):288.
Brusasco C, Santori G, Tavazzi G et al. (2022) Second-order grey-scale texture analysis of pleural ultrasound images to differentiate acute respiratory distress syndrome and cardiogenic pulmonary edema. J Clin Monit Comput. 36(1):131-40.
Chou EH, Wang CH, Monfort R et al. (2020) Association of ultrasound-related interruption during cardiopulmonary resuscitation with adult cardiac arrest outcomes: A video-reviewed retrospective study. Resuscitation. 149:74-80.c
Cinotti R, Delater A, Fortuit C et al. (2015) Speckle-Tracking analysis of left ventricular systolic function in the intensive care unit. Anaesthesiol Intensive Ther. 47(5):482-6.
Cisneros-Velarde P, Correa M, Mayta H et al. (2016) Automatic pneumonia detection based on ultrasound video analysis. Annu Int Conf IEEE Eng Med Biol Soc. 4117-20.
Corradi F, Ball L, Brusasco C, Riccio AM et al. (2013) Assessment of extravascular lung water by quantitative ultrasound and CT in isolated bovine lung. Respir Physiol Neurobiol. 187(3):244-9.
Corradi F, Brusasco C, Vezzani A et al. (2016) Computer-Aided Quantitative Ultrasonography for Detection of Pulmonary Edema in Mechanically Ventilated Cardiac Surgery Patients. Chest. 150(3):640-51.
Corradi F, Brusasco C, Garlaschi A et al. (2015) Quantitative analysis of lung ultrasonography for the detection of community-acquired pneumonia: a pilot study. Biomed Res Int. 868707.
Corradi F, Brusasco C, Pelosi P et al. (2014) Chest ultrasound in acute respiratory distress syndrome. Curr Opin Crit Care. 20(1):98-103.
Corradi F, Guarracino F, Santori G et al. (2022a) Ultrasound localization of central vein catheter tip by contrast-enhanced transthoracic ultrasonography: a comparison study with trans-esophageal echocardiography. Crit Care. 26(1):113.
Corradi F, Isirdi A, Malacarne P et al. (2021a) Low diaphragm muscle mass predicts adverse outcome in patients hospitalized for COVID-19 pneumonia: an exploratory pilot study. Minerva Anestesiol. 87(4):432-8.
Corradi F, Vetrugno L, Orso D et al. (2021b) Diaphragmatic thickening fraction as a potential predictor of response to continuous positive airway pressure ventilation in COVID-19 pneumonia: A single-center pilot study. Respir Physiol Neurobiol. 284:103585.
Corradi F, Vetrugno L, Isirdi A et al. (2022b) Ten conditions where lung ultrasonography may fail: limits, pitfalls and lessons learned from a computer-aided algorithmic approach. Minerva Anestesiol. 88(4):308-13.
Daley JI, Dwyer KH, Grunwald Z et al. (2019) Increased Sensitivity of Focused Cardiac Ultrasound for Pulmonary Embolism in Emergency Department Patients With Abnormal Vital Signs. Acad Emerg Med. 26(11):1211-20.
De Jonghe B, Sharshar T, Lefaucheur JP et al. (2002) Paresis acquired in the intensive care unit: a prospective multicenter study. JAMA. 288(22):2859-67.
Donker DW, Meuwese CL, Braithwaite SA et al. (2018) Echocardiography in extracorporeal life support: A key player in procedural guidance, tailoring and monitoring. Perfusion. 33(1_suppl):31-41.
Dori G, Jakobson DJ (2016) Speckle tracking technology for quantifying lung sliding. Med Hypotheses. 91:81-3.
Douflé G, Ferguson ND (2016) Monitoring during extracorporeal membrane oxygenation. Curr Opin Crit Care. 22(3):230-8.
Gaspari R, Weekes A, Adhikari S et al. (2021) Comparison of outcomes between pulseless electrical activity by electrocardiography and pulseless myocardial activity by echocardiography in out-of-hospital cardiac arrest; secondary analysis from a large, prospective study. Resuscitation. 169:167-72.
Formenti P, Umbrello M, Coppola S et al. (2019) Clinical review: peripheral muscular ultrasound in the ICU. Ann Intensive Care. 9(1):57.
Guérin L, Vieillard-Baron A (2016) The Use of Ultrasound in Caring for Patients with Sepsis. Clin Chest Med. 37(2):299-307.
Guevarra K, Greenstein Y (2020) Ultrasonography in the Critical Care Unit. Curr Cardiol Rep. 22(11):145.
Hahn RT, Abraham T, Adams MS et al. (2014) Guidelines for performing a comprehensive transesophageal echocardiographic examination: recommendations from the American Society of Echocardiography and the Society of Cardiovascular Anesthesiologists. Anesth Analg. 118(1):21-68.
Hussain A, Via G, Melniker L et al. (2020) Multi-organ point-of-care ultrasound for COVID-19 (PoCUS4COVID): international expert consensus. Crit Care. 24(1):702.
International consensus statement on training standards for advanced critical care echocardiography. (2014) Intensive Care Med. 40(5):654-66.
Konstantinides SV, Meyer G, Becattini C et al. (2020) 2019 ESC Guidelines for the diagnosis and management of acute pulmonary embolism developed in collaboration with the European Respiratory Society (ERS). Eur Heart J. 41(4):543-603.
Lau YH, See KC (2022) Point-of-care ultrasound for critically ill patients: A mini-review of key diagnostic features and protocols. World J Crit Care Med. 11(2):70-84.
Lengyel M (1997) The impact of transesophageal echocardiography on the management of prosthetic valve endocarditis: experience of 31 cases and review of the literature. J Heart Valve Dis. 6(2):204-11.
Longobardo L, Zito C, Carerj S et al. (2018) Role of Echocardiography in the Intensive Care Unit: Overview of the Most Common Clinical Scenarios. J Patient Cent Res Rev. 30;5(3):239-243.
Long B, Alerhand S, Maliel K, Koyfman A (2018) Echocardiography in cardiac arrest: An emergency medicine review. Am J Emerg Med. 36(3):488-93.
Luecke T, Corradi F, Pelosi P (2012) Lung imaging for titration of mechanical ventilation. Curr Opin Anaesthesiol. 25(2):131-40.
Michelena HI, Abel MD, Suri RM et al. (2010) Intraoperative Echocardiography in Valvular Heart Disease: An Evidence-Based Appraisal. Mayo Clin Proc. 85(7):646-55.
Mongodi S, De Luca D, Colombo A et al. (2021) Quantitative Lung Ultrasound: Technical Aspects and Clinical Applications. Anesthesiology. 134(6):949-65.
Orde S, Slama M, Stanley N et al. (2018) Feasibility of biventricular 3D transthoracic echocardiography in the critically ill and comparison with conventional parameters. Crit Care. 22(1):198.
Peterson GE, Brickner ME, Reimold SC (2003) Transesophageal echocardiography: clinical indications and applications. Circulation. 107(19):2398-402.
Plata P, Gaszyński T (2019) Ultrasound-guided percutaneous tracheostomy. Anaesthesiol Intensive Ther. 51(2):126-32.
Platts DG, Sedgwick JF, Burstow DJ et al. (2012) The role of echocardiography in the management of patients supported by extracorporeal membrane oxygenation. J Am Soc Echocardiogr. 25(2):131-41.
Poelaert J, Roosens C (2007) Is tissue Doppler echocardiography the Holy Grail for the intensivist? Crit Care. 11(3):135.
Prager R, Bowdridge J, Pratte M et al. (2022) Indications, Clinical Impact, and Complications of Critical Care Transesophageal Echocardiography: A Scoping Review. J Intensive Care Med. 8850666221115348.
Price S, Uddin S, Quinn T (2010) Echocardiography in cardiac arrest. Curr Opin Crit Care. 16(3):211-5.
Raimondi F, Migliaro F, Verdoliva L et al. (2018) Visual assessment versus computer-assisted gray scale analysis in the ultrasound evaluation of neonatal respiratory status. PLoS One. 13(10):e0202397.
Raso R, Tartarisco G, Matucci Cerinic M et al. (2015) A soft computing-based B-line analysis for objective classification of severity of pulmonary edema and fibrosis. JACC Cardiovasc Imaging. 8(4):495-6.
Saugel B, Scheeren TWL, Teboul JL et al. (2017) Ultrasound-guided central venous catheter placement: a structured review and recommendations for clinical practice. Crit Care. 21(1):225.
Schmidt GA, Blaivas M, Conrad SA et al. (2019) Ultrasound-guided vascular access in critical illness. Intensive Care Med. 45(4):434-46.
Sharshar T, Bastuji-Garin S, Stevens RD et al. (2009) Presence and severity of intensive care unit-acquired paresis at time of awakening are associated with increased intensive care unit and hospital mortality. Crit Care Med. 37(12):3047-53.
Shrestha GS, Srinivasan S (2018) Role of Point-of-Care Ultrasonography for the Management of Sepsis and Septic Shock. Rev Recent Clin Trials. 13(4):243-51.
Soliman-Aboumarie H, Pastore MC, Galiatsou E et al. (2021) Echocardiography in the intensive care unit: An essential tool for diagnosis, monitoring and guiding clinical decision-making. Physiol Int.
Turton P, Hay R, Taylor J et al. (2016) Human limb skeletal muscle wasting and architectural remodeling during five to ten days intubation and ventilation in critical care – an observational study using ultrasound. BMC Anesthesiol. 16.
Vallabhajosyula S, Ahmed AM, Sundaragiri PR (2020) Role of echocardiography in sepsis and septic shock. Ann Transl Med. 8(5):150.
Vieillard-Baron A, Slama M, Cholley B et al. (2008) Echocardiography in the intensive care unit: from evolution to revolution? Intensive Care Med. 34(2):243-9.
Vezzani A, Manca T, Brusasco C et al. (2017) A randomized clinical trial of ultrasound-guided infra-clavicular cannulation of the subclavian vein in cardiac surgical patients: short-axis versus long-axis approach. Intensive Care Med. 43:1594-601.
Vezzani A, Manca T, Brusasco C et al. (2014) Diagnostic value of chest ultrasound after cardiac surgery: a comparison with chest X-ray and auscultation. J Cardiothorac Vasc Anesth. 28:1527-32.
Volpicelli G, Gargani L, Perlini S et al. (2021) Lung ultrasound for the early diagnosis of COVID-19 pneumonia: an international multicenter study. Intensive Care Med. 47(4):444-54.
Walker FO (2004) Neuromuscular ultrasound. Neurol Clin. 22(3):563-90, vi.
Weitzel WF, Hamilton J, Wang X et al. (2015) Quantitative lung ultrasound comet measurement: method and initial clinical results. Blood Purif. 39(1-3):37-44.
Wong A, Galarza L, Forni L et al. (2020) Recommendations for core critical care ultrasound competencies as a part of specialist training in multidisciplinary intensive care: a framework proposed by the European Society of Intensive Care Medicine (ESICM). Crit Care. 24(1):393.
Wu C, Zheng Z, Jiang L et al. (2018) The predictive value of bedside ultrasound to restore spontaneous circulation in patients with pulseless electrical activity: A systematic review and meta-analysis. PLoS One. 13(1):e0191636.
Yamamoto T (2014) Critical care echocardiography. Masui. 63(9):954-61.











