ICU Management & Practice, Volume 23 - Issue 3, 2023
Critical care must move to a way of working that recognises climate change is a medical emergency, necessitating us all to put sustainability at the forefront of our actions as a multidisciplinary team working together in the best interests of our patients, our environment and our resources.
Planetary Health and Public Health
People’s health depends on the health of the planet. The ever-escalating climate crisis negatively impacts public health, from the direct impact of extreme weather events, including heatwaves, wildfires, droughts, hurricanes, rising sea levels and flooding (Romanello et al. 2022) to the indirect impacts of climate-change-instigated migration and conflict. The United Nations (UN) recognises the urgent need to resolve human-induced climate change in their Framework Convention on Climate Change (UNFCCC), Intergovernmental Panel on Climate Change (IPCC), and annual Conference of the Parties (COP) (UN Climate Change 2023). The COP26 Health Programme included five priority initiatives for improving the climate crisis: 1) building climate resilient health systems; 2) developing low carbon sustainable health systems; 3) adaption research for health; 4) inclusion of health priorities in Nationally Determined Contributions; and 5) raising the voice of health professionals as advocates for stronger ambition on climate change (WHO Climate Change and Health 2021).
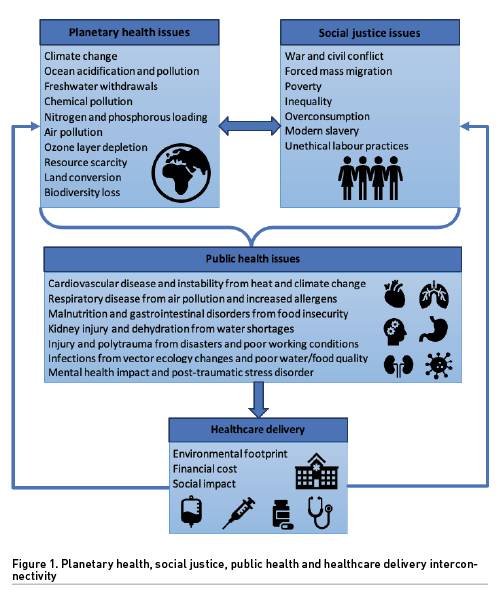
We are in a critical decade, with the IPCC (2023) highlighting that despite challenges thus far, it is not too late to restrict global warming to 1.5°C by 2030 through “rapid and deep emissions reductions across all sectors of the global economy” (Stiell 2023). Otherwise, the human health issues resulting from the climate crisis will worsen, leading to both an environmental catastrophe and a global public health medical emergency (Howard et al. 2023). However, climate change is not the only interlinked planetary and public health concern. To avoid ‘carbon tunnel vision’, a holistic approach to environmental sustainability should also address ecosystem issues related to water, land, atmosphere, biosphere and resource availability (Deivanayagam and Osborne 2023; Fang et al. 2022). Furthermore, social justice issues can be both a cause and an effect of ecological problems with interrelated public health implications (Figure 1). It is also unethical how people in low-income countries often experience the worst impacts of climate change, and yet they contribute minimally to planetary damage (Chapman and Ahmed 2021).
Environmental Sustainability and Intensive Care
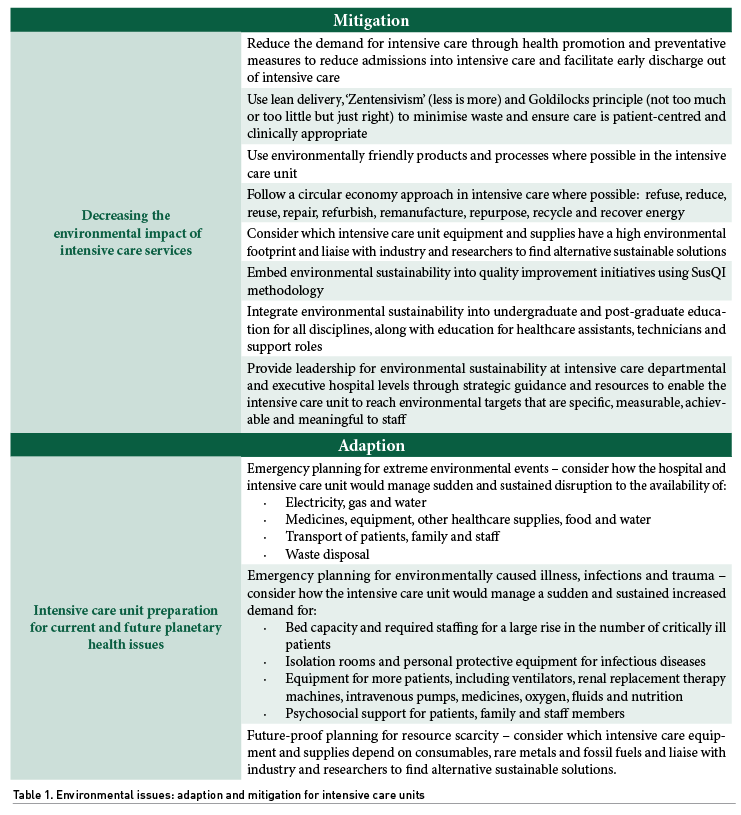
Intensive care clinicians and managers must become more aware of the intrinsically linked planetary and public health problems in Figure 1 to understand better how they can actively participate in both mitigation by reducing healthcare’s environmental footprint (ANZICS 2022) and adaptation by adjusting to current and future ecological issues (Bein et al. 2020), as outlined in Table 1.
The ‘People, Planet and Profit’ model recognises the interconnectivity of financial, social and ecological systems, with sustainable resourcing of one element impacting and being co-dependent on the others (Elkington 2002; Oung 2022). The true success of all sectors, including healthcare, requires this triple-bottom-line philosophy. Still, clinicians and healthcare managers have not yet widely normalised addressing environmental sustainability, despite healthcare causing 4.4% of the total greenhouse gas emissions globally (Karliner et al. 2019) and intensive care generating a significantly high environmental footprint (McGain et al. 2018; McGain et al. 2020). We must urgently move environmental sustainability from the fringe to the centre ground in intensive care. This means a new way of thinking to prioritise sustainability in all aspects of clinical care, including purchasing and using drugs and equipment, using energy efficiently (with renewable sources where possible) and dealing with waste. Healthcare should not be resting on its laurels, believing it already does enough good on behalf of others; in relation to environmental sustainability, we need less tokenism and more implementation. What was viewed previously as "hippy green" activism should now rapidly transition into mainstream realism.
Placing sustainability into the centre ground in how we work, think, and approach healthcare cannot be restricted solely to interested individuals; instead, it needs to involve the entire multidisciplinary team. Managers and non-clinical facing staff are at least as necessary, if not more important, than nurses, pharmacists, allied health professionals, assistant roles and doctors. It is incorrect to view sustainability as more expensive than continuing as we are – far from it. If done well, sustainable healthcare can deliver better patient care, save resources and money, add social value, and generate less waste (Mortimer et al. 2018).
Operationalising Intensive Care Sustainability
What does putting sustainability into the centre ground mean, though? Operationalising sustainability by changing platitudes into actions requires leadership and teamwork between directorate management, estates, waste, pharmacy, procurement and all roles working in an intensive care unit (Trent et al. 2023). A multi-disciplinary intensive care sustainability team can be set up and linked with other directorates and an overarching hospital sustainability team. Before absolving individual responsibility by assuming sustainability teams cover everything, it is essential to remember that responsibility is simultaneously individual and collective and that agreed intensive care sustainability actions should be coordinated to be most effective (Stamps et al. 2020). For example, the critical care unit at the University Hospital of Wales has a carbon footprint of approximately 1% of the Health Board’s total carbon footprint. This hospital’s intensive care unit can and has made efficiencies, including turning computers off overnight, using light-emitting diode bulbs, and not fully charging unnecessary electrical equipment at all times. Without coordination with other directorates and wide rollout across a hospital site, the efficiencies made in intensive care will be very small but still important as part of a whole system approach.
Another example of operationalising healthcare sustainability is the ‘gloves off’ campaign initiated by nurses in Great Ormond Street Hospital, London who demonstrated that decreasing unnecessary non-sterile glove use saves money and reduces waste (Greener NHS 2020; NHS England 2018). The critical care team in the University Hospital of Wales spends in excess of £100,000 on non-sterile gloves. Reducing inappropriate gloves use by 20% could save £20,000 without impacting patient care and decreasing the critical care unit's environmental footprint. Rolling out a 'gloves off' campaign in intensive care units across a region, network or country would significantly improve environmental sustainability and achieve significant financial savings without impacting patient care. To do so requires education for glove users, coordination within teams, good role models and clear leadership.
Zentensivism is a concept used to delineate a different way of practising intensive care; with less intervention and more compassion (Ahrens 2021; Siuba et al. 2020). Fewer tests do not mean less care. Tests should be considered in terms of ‘is this test justified’ and ‘will the result of this test change my management’ or will watching and waiting provide better holistic patient and family-centred care? Zentensivism was not initially connected to sustainability, but there is a clear link between sustainability and fewer tests, better recognition of when further interventional care will not improve the patient’s outcome and earlier initiation of end-of-life care as the most appropriate course of action. Patients in intensive care have a proportionately high mortality rate (Detsky et al. 2017). If those most at risk of dying can be identified more clearly and earlier, we can deliver better, more sustainable care. This principle also applies to whether intensive care should play a role at the outset of critical illness; nearly all of us will be critically ill before we die, but that does not mean nearly all of us should receive critical care as the best care option. Medicine and wider society need to engage better about what is possible and, in a broader sense, what is most appropriate and sustainable at the end of life.
Tools and Resources for Sustainable Intensive Care
There are resources now available to clinicians, managers, researchers and educators which explicitly relate to environmental sustainability. The following is a list of intensive care-specific resources to help guide planning, implementing and evaluating environmental sustainability initiatives for intensive care units:
- A Beginner’s Guide to Sustainability in the ICU (ANZICS 2022).
- Critical Care Susnet – sustainability network hosted by the Centre for Sustainable Healthcare and endorsed by the Intensive Care Society and British Association of Critical Care Nurses (CSH Networks 2023).
- My Green ICU collection for the European Society of Intensive Care Medicine’s Intensive Care Medicine journal (Bein and McGain 2023).
Those wanting to improve the environmental sustainability of their local unit should also consider indirectly relevant resources which fit the ethos of stewardship, ‘less is more’, the Goldilocks Principle (not too much, not too little and just the right amount of intervention) and complication prevention. For instance, the ICU Liberation bundle (Society of Critical Care Medicine 2020), ventilator-associated pneumonia bundle (Mastrogianni et al. 2023), antimicrobial stewardship (Murphy et al. 2022) and fluid stewardship (Hawkins et al. 2020) all promote a speedier recovery for the critically ill with fewer complications and less resource use, thereby lowering the environmental footprint of an intensive care unit stay. Initiatives to reduce inappropriate intensive care unit admissions and enhance timely discharge can also be developed using a sustainability lens.
There are a variety of environmental sustainability resources, organisations and events that are relevant to all healthcare areas, including intensive care, such as:
- SusQI Framework – model to embed sustainability within quality improvement to address environmental sustainability, reduce financial cost and add social value while improving healthcare quality with free resources and templates.
- Centre for Sustainable Healthcare – engages healthcare professionals, service users and the wider community to understand better the interconnectivity between health and the environment and work towards reducing healthcare’s resource footprint.
- Health Care Without Harm – an international organisation with regional sections for América Latina (Spanish and Portuguese versions), Asia, Europe and US-Canada and publications and resources translated into multiple languages.
- Centre for Sustainable Health Systems – supports research, education, communities of practice, strategic initiatives and events related to promoting sustainable healthcare.
- Nordic Centre for Sustainable Healthcare – brings together stakeholders, organisations and projects to provide a network and platform for promoting ecologically sustainable healthcare.
- Healthcare Ocean – provides advocacy, education and collaboration to reduce the unintentional oceanic damage caused by the procurement and delivery of healthcare.
- WHO Health-care waste – World Health Organization guidance on ensuring safe and sustainable healthcare waste management.
Conclusion
Intensive care units use proportionately excess amounts of energy, consumables, medicines and staff in our care processes, and we generate large amounts of waste. We must recognise how intensive care’s environmental footprint contributes to poor planetary health. It is time for environmental sustainability to become an urgent central focus in delivering intensive care services to minimise the damage caused to our environment whilst also providing the best and most appropriate care for the critically ill.
Conflict of interest
There are no conflicts of interest for Dr Jack Parry-Jones. Dr Heather Baid has received grants related to healthcare environmental sustainability from the University of Brighton Rising Stars award, and the British Association of Critical Care Nurses and Research England.
References:
Ahrens I (2021) Patient-centred intensive care medicine using a holistic approach: #zentensivist—an interview with Dr Matthew Siuba. Eur Heart J Acute Cardiovasc Care. 10(7):823-824.
Bein T, Karagiannidis C, Quintel M (2020) Climate change, global warming, and intensive care. Intensive Care Med. 46(3):485-487.
Bein T, McGain F eds. (2023) Collection: My Green ICU. Intensive Care Med. Available at link.springer.com/collections/aefebhegjj
Chapman AR, Ahmed AK (2021) Climate justice, human rights, and the case for reparations. Health Hum Rights. 23(2):81-94.
Deivanayagam TA, Osborne RE (2023) Breaking free from tunnel vision for climate change and health. PLOS Global Public Health. 3(3):e0001684.
Detsky ME, Harhay MO, Bayard DF, Delman et al. (2017) Six-month morbidity and mortality among intensive care unit patients receiving life-sustaining therapy. A prospective cohort study. Ann Am Thorac Soc. 14(10):1562-1570.
Elkington J (2002) Cannibals with forks: the triple bottom line of 21st-century business. Oxford, Capstone.
Fang L, Hixson R, Shelton C (2022) Sustainability in anaesthesia and critical care: beyond carbon. BJA Educ. 22(12):456-465.
Greener NHS (2020) Great Ormond Street Hospital – reducing single-use plastics case study. Available at england.nhs.uk/greenernhs/whats-already-happening/great-ormond-street-hospital-reducing-single-use-plastics-case-study/
Hawkins WA, Smith SE, Newsome AS et al. (2020) Fluid stewardship during critical illness: A call to action. J Pharm Pract. 33(6):863-873.
Howard C, MacNeill AJ, Hughes F et al. (2023) Learning to treat the climate emergency together: social tipping interventions by the health community. Lancet Planet Health. 7(3):e251-e264.
IPCC (2023) AR6 Synthesis Report: Climate Change 2023. Available at ipcc.ch/report/sixth-assessment-report-cycle/
Karliner J, Slotterback S, Boyd R et al. (2019) Health care’s climate footprint. How the health sector contributes to the global climate crisis and opportunities for action. Health Care Without Harm and ARUP. Available at noharm-global.org/sites/default/files/documents-files/5961/HealthCaresClimateFootprint_092319.pdf
Mastrogianni M, Katsoulas T, Galanis P et al. (2023) The impact of care bundles on ventilator-associated pneumonia (VAP) prevention in adult ICUs: A systematic review. Antibiotics. 12(2):227.
McGain F, Burnham JP, Lau R et al. (2018) The carbon footprint of treating patients with septic shock in the intensive care unit. Crit Care Resusc. 20(4):304-312.
McGain F, Muret J, Lawson C et al. (2020) Environmental sustainability in anaesthesia and critical care. Br J Anaesth. 125(5):680-692.
Mortimer F, Isherwood J, Wilkinson A et al. (2018) Sustainability in quality improvement: redefining value. Future Healthc J. 5(2):88–93.
Murphy CV, Reed EE, Herman DD et al. (2022) Antimicrobial stewardship in the ICU. Semin Respir Crit Care Med. 43(1):131-140.
NHS England (2018) ‘The gloves off’ campaign. The Atlas of Shared Learning. Available at england.nhs.uk/atlas_case_study/the-gloves-are-off-campaign/
Oung K (2022) People, planet, profit: environmentally and socially sustainable business strategies. New York, Business Expert Press.
Pichler P-P, Jaccard IS, Weisz U et al. (2019) International comparison of health care carbon footprints. Environ Res Lett. 14(6):064004.
Romanello M, Di Napoli C, Drummond P et al. (2022) The 2022 report of the Lancet Countdown on health and climate change: health at the mercy of fossil fuels. Lancet. 400(10363):1619-1654.
Siuba MT, Carroll CL, Farkas JD et al. (2020) The zentensivist manifesto. Defining the art of critical care. ATS Sch. 1(3):225-232.
Society of Critical Care Medicine (2020) ICU Liberation Bundle A-F. Available at sccm.org/Clinical-Resources/ICULiberation-Home/ABCDEF-Bundles
Stamps DC, Waller MG, Foley SM et al. (2020) Chief Nursing Officer Council partners with sustainability department to develop a model of success for reducing the organization’s carbon footprint. Nurse Lead. 18(6):586-591.
Stiell S (2023) Statement by Simon Stiell, UN Climate Change Executive Secretary, on the IPCC’s Synthesis Report of the Sixth Assessment Report. United Nations Climate Change. Available at unfccc.int/news/statement-by-simon-stiell-un-climate-change-executive-secretary-on-the-ipcc-s-synthesis-report-of
Trent L, Law J, Grimaldi D (2023) Create intensive care green teams, there is no time to waste. Intensive Care Med.
United Nations Climate Change (2023) UN Climate Change. Available at unfccc.int/
WHO Climate Change and Health (2021) Health at COP26. Available at who.int/teams/environment-climate-change-and-health/climate-change-and-health/advocacy-partnerships/talks/cop26








