ICU Management & Practice, Volume 17 - Issue 1, 2017
The ICU-Hear project delivered by the charity Music in Hospitals™ provides specialised live music sessions for critically ill patients. The initiative started after Helen Ashley Taylor (a former ICU patient) met Sister Natalie Mason, Adult Critical Care Follow up Lead at Manchester Royal Infirmary at a regional support group for former ICU patients. Helen had volunteered for the charity Music in Hospitals ™ for over 7 years. After Natalie and Helen discussed the potential patient benefits of live music on the ICU, a pilot project was set up. A working group now plans to research the positive impact on patient health.
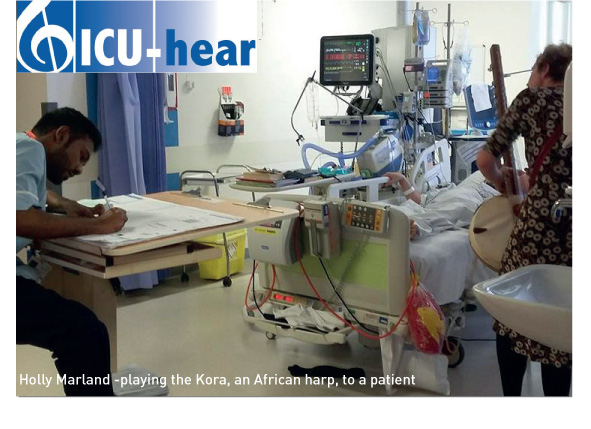
Soothing melodic music regularly meanders through and above the environmental soundscape of the critical care unit at Manchester Royal Infirmary (MRI). From the tranquillity of an acoustic guitar or a gentle African harp accompanied by beautiful soft singing to the flowing, mellow rich tones of a clarinet, professional musicians from the long-established charity, Music in HospitalsTM, have been playing live music to critically ill patients since July 2016. The initial pilot project attracted significant attention, including national press and local television coverage (Ashley Taylor 2016; Granada News 2016). In January 2017 the UK Prime Minister acknowledged the work with a Points of Light award, recognising the initiative borne out of patient experience that has resulted in a successful patient and staff collaboration (Prime Minister’s Office 2017).
Setting the Scene
It has taken two years for the idea to evolve to this stage of development and recognition, having begun when I experienced being an ICU patient in February 2015. Considerable planning and preparation was involved before the first music session took place, and since then the compelling positive results and patient feedback have continued to inform the evolution and expansion of this project. “Absolutely brilliant”, “wonderful”, “soothing”, “calming”, “fantastic”, “uplifting”, “enjoyable”, “relaxing” “amazing”, “beautiful”, “therapeutic”, “pleasant”, “peaceful”, and “welcome” are words regularly used by patients to describe the experience. These are not ordinarily adjectives chosen by patients to describe any part of the ICU experience. Relatives also express gratitude for being able to smile and relax on the ICU during what is an exceptionally difficult time in their lives. Indications from feedback and data collected suggest the music may be beneficial to patients’ clinical outcomes, relatives and caregivers and the working atmosphere more generally.
Transforming an Anxious Time
These positive self-reports made by patients after hearing live music on the ICU are significant. Many published accounts focus on harrowing ICU patient experiences (particularly of delirium), which remain in former patients’ memories for a considerable time. Both qualitative and quantitative data collections have been used during this project, and to date all patients have confirmed feeling relaxed whilst hearing the music. Adult Critical Care Matron Donna Cummings at MRI reports that the relaxing effects of the music on patients continue long after the musicians leave the ward. She describes the musical intervention as “overwhelmingly moving to see and participate in”.
This ability to focus on live music is noteworthy considering the prevalence of delirium among ICU patients. There is evidence too that relatives can suffer with anxiety and be at risk of developing post-traumatic stress disorder (PTSD) after witnessing loved ones suffering from critical illness and delirium (Jones et al. 2012). Published reports state that delirium is common and can result in a longer ICU stay, longer duration of mechanical ventilation and is associated with higher mortality rates (Ely 2001). Recognition and early intervention of the management of delirium is important, including the most commonly missed subtype, hypoactive delirium (Meagher 2000)—often called ‘quiet’ delirium. Sister Natalie Mason and Matron Donna Cummings report that the MRI uses a combination of pharmacological and non-pharmacological strategies to both prevent and manage delirium in patients on the ICU, and the unit has seen dramatic reductions in incidences of delirium over the past 18 months.
Patient Experience of the ICU Sound Environment
I documented my own patient experience after discharge, then my post ICU recovery period 13 months later. Re-reading that first contemporaneous account one year on, after a challenging recovery period and after hearing the experiences of other former ICU patients, I started considering further the potential benefits of offering live music to ICU patients. My own account frequently refers to the noise I experienced 24/7 on the ICU, and the distressing effect it had on me. I couldn’t stop the unpleasant cacophony of sounds reaching me. I couldn’t lift my arms to put my hands over my ears, and I couldn’t always communicate to tell anyone how upsetting I was finding the sound environment. I couldn’t sleep. I couldn’t escape. My acute sense of hearing became a curse rather than a blessing.
 |  |
 |  |

A Brief Musical Encounter
I recalled hearing a few minutes of music
towards the end of my stay on the high dependency unit (HDU) after leaving the
ICU. This provided the initial stimulus for the ICU-hear project. After leaving
hospital I wrote:
“I recall trying to hold a TV remote in my hands on the high dependency unit and struggling to press the buttons. I couldn’t follow TV programmes—the noise was upsetting. My husband turned it on at one point and there was some choral singing. It was wonderful—my only happy moment of that whole hospital stay. The music, the singing—it brought me back into the present moment temporarily. The music gave me both hope and comfort. The noise throughout my hospital stay had been a source of stress—so to hear some lovely music was a small but memorable bit of therapy”.
After my second hospital discharge
(following an emergency re-admission), I sent a message to the Chair of the
volunteer committee for Music in HospitalsTM North (who had previously worked
as an ICU sister for 20 years), a charity I had volunteered with for many
years. In it I wrote:
“There was a cheery moment right in the middle
of the most serious low point. It [the music] transformed a horrible situation
for me into one where I was instantly brought back to my former inner self”.
See Also: Music Therapy Has a Role in the ICU
Effects
of a Musical Awakening
The beauty and quality of the soothing music were a welcome respite, providing an awakening from the state of passive consciousness and displacement I had endured for numerous days and nights. I experienced feeling alert, focused and connected to the world again. Apathy, isolation and discomfort were forgotten. My mind cleared; I felt calm and organised. I was engaged and energised by lovely sounds. It transformed a disorientating, frightening experience, and that memorable impact stayed with me.
I subsequently wondered if that impact could have been even greater if I’d experienced music earlier—before being moved off the ICU and on to the HDU. Having volunteered with Music in HospitalsTM for several years I also wondered about the potential impact of receiving live music that was personalised and delivered under clinical supervision, where the music evolves to match the patient’s condition.
Shared
Patient Experiences
I wasn’t aware initially that my personal experience resonated with many former ICU patients. After meeting others and sharing accounts of the ongoing effects following harrowing experiences of prolonged anxiety and delirium on the ICU, I realised the long-term ramifications an ICU stay can have. Despite immense gratitude for the devoted staff who ensured their survival, many former ICU patients struggled with daily life after discharge. Awareness of this fact is sometimes poor amongst friends, families, some GPs and many employers. Recovering pre-illness life and/or livelihood can be enormously challenging.
Practicalities of Launching ICU-Hear
When I met Sister Natalie Mason, critical care follow up lead at MRI ICU, at a regional patient support group, I spoke about my own patient experiences of intrusive noise, the impact of hearing music and my volunteering work with Music in HospitalsTM. Natalie described a specific project addressing noise levels at night at the MRI. She had also researched the potential merits of live music. After talking together about the benefits that live music might provide for patients and realising that we both were keen for it to happen, a pilot project was discussed with Music in HospitalsTM. The ICU-hear project was subsequently pioneered at the MRI.
The aim of the pilot project was to make the critical care unit less clinical, altering the ambience by using soothing music. The staff recognise, understand and appreciate that the ICU can be a daunting experience. Care is taken to ensure that patients and/or relatives give permission for music to be played to them. Musicians ensure they are never in the way; they sensitively step aside should a patient need urgent medical attention. Staff have not been distracted by the musicians, and have welcomed the calming ambience on the unit that has been introduced by the music.
Selecting the Right Professional Musicians
It was paramount that the musicians selected for this work were sensitive, skilled, experienced professionals who could individualise delivery of live music at the bedside according to the changing needs of patients, families and the critical care staff. The musicians must be sensitive, empathetic and able to provide a gentle musical repertoire. They must be well versed in intensive care protocol, in addition to having a gentle, approachable personality and the resilience to adapt to any difficult situations they may witness. Music in HospitalsTM supports musicians with this and provides continuing professional development to enable the identification and development of effective common working practices.
The Importance of Live Music
Live performance (in contrast to recorded music) enables the musicians to observe and monitor any small changes in the patient, so that they may alter the tone and pace of the music accordingly.
The instruments played during the pilot study were chosen for their suitability for the environment and noisy bedside machinery—providing sounds that were engaging yet unobtrusive in this noise-polluted space. It is only more recently that I realised Florence Nightingale had recommended the beneficial healing effects of stringed instruments, the human voice and wind instruments, which she believed were “capable of having a continuous sound” (Nightingale 1860). These are precisely the instruments we have used so far for this work.
Music at the Hospital Bedside
Florence Nightingale introduced music as a beneficial nursing intervention for wounded soldiers during the Crimean War. Music in HospitalsTM started its work after World War Two, when it began playing live music to wounded servicemen in military hospitals. The charity maintains strong links with veterans in its work today. Some problems encountered by veterans, including PTSD, are also complications some ICU patients experience. Music in HospitalsTM has worked across the entire healthcare spectrum for decades, yet live music has rarely been requested for adult ICUs in the UK. After first playing in military hospitals 70 years ago, the charity’s specialist musicians are once again playing live at the bedsides of seriously ill patients.
Next
Phase
The multidisciplinary team involved throughout this venture has reviewed existing research studies alongside the pilot project outcomes. This is informing the next work phase, enabling consideration of targeted ways to introduce music as a non-pharmacological intervention. Insights gained over two years—before, during and after the pilot project—have provided an evidence base of data for further research. Whilst live music is utilised on neonatal ICUs, there is limited research on a sufficiently large scale involving live (rather than recorded) music on adult ICUs. It is recognised that music is a safe, relatively inexpensive intervention, and there is a pool of published research supporting the impact of music on health and body physiology (Harris 2014). One recent study concluded that live harp music in a critical care unit reduced pain by 27% (Chaisson et al. 2013). Another study found that listening to music improved patients’ tolerance of mechanical ventilation. They also experienced less anxiety and required less sedation (Chan et al. 2013). Sedation in mechanically ventilated patients is a contributing factor to the onset of delirium (Ely 2004). Live music in neonatal ICUs is associated with infants’ reduced heart rates and deeper sleep, potentially reducing time needed in hospital (Arnon et al. 2006).
There is clearly a place for live musical intervention in the care of critically ill people. Using live music for the alleviation of several aspects of the patient ICU experience may improve patient outcomes both on the ICU and also after discharge. The music can also potentially change the way relatives, staff and patients interact, making it easier to care for patients if patients and relatives are more relaxed.
Research design and preparation for
furthering this project is at an advanced stage, and the pioneering work at MRI
continues on a regular basis. Sid Richards, regional director for Music in
Hospitals North, confirmed that following phenomenal feedback from patients,
relatives and staff, more musicians are being carefully selected and trained
for the ICU environment and the charity is working hard to expand the work
across more UK hospitals to benefit ICU patients.







