Critical illness reduces normal sleep
Most critically ill ICU patients report, recall, or are observed to have disordered sleep. Specifically, the number of awakenings per hour is higher than in health (Elliott et al. 2013; Roche-Campo et al. 2013, Drouot et al. 2014), daytime somnolence is increased to as much as 50% of total sleep (White et al. 1983; Cordoba-Izquierdo et al. 2013), and patients report sleep quality as worse than baseline (Elliott et al. 2013; Freedman et al. 1999; Little et al. 2012). EEG recordings show a higher than normal proportion of light to deep sleep and that sedating drugs are primarily responsible for an “atypical sleep” pattern characterised by disorganised delta waves and the absence of k complexes and sleep spindles [summarised in Devlin et al. (2018)]. There are many possible reasons for disordered sleep, and as the importance of each will vary in different patients (Figure 1), so will the optimal approach to management.
Sedation is a poor substitute for sleep
Virtually every ICU clinician has at some stage asked: “My patient didn’t sleep, could we give a sedative?” The single most important goal of this paper is to explain why this question is analogous to the request “My patient keeps coughing, could we give a muscle relaxant?” Cough is distressing to patients and staff, but a muscle relaxant is a temporary solution that would make many underlying problems worse, while also causing psychological distress. It is much better to make a diagnosis, address underlying causes, and use symptomatic temporising treatments that do not create adverse effects worse than the problem they are designed to treat.
Sleep is a physiological state of cognitive and sensory disengagement from the environment (Kamdar et al. 2012) required in some form by all mammals. Various cardiovascular, respiratory, gastrointestinal and thermoregulatory effects are observed, the importance of which is not fully understood. However, acute sleep deprivation experiments are simple to conduct, revealing perceptual distortions within 24-48 hours, followed by delusions then hallucinations and psychosis (Waters et al. 2018). Physical performance (Kirschen et al. 2018) and immune function (Mullington et al. 2010) are also degraded by inadequate sleep.
Despite their ability to produce the outward appearance of sleep, GABA-ergic sedatives used to facilitate tolerance of an endotracheal tube can have the opposite effect. Benzodiazepines increase N2 (light) but reduce N3 (deep—thought to be the most restorative) sleep (Achermann and Borbely 1987; Borbely et al. 1985), as does propofol (Herregods et al. 1989). Similarly, opioids also reduce N3 and REM sleep (Kamdar et al. 2012). Benzodiazepines in particular have been associated with delirium in the ICU (Pandharipande et al. 2006; 2008), and delirium itself is an independent risk for disordered sleep (Devlin et al. 2018). Therefore, commencing or increasing the rate of a sedative infusion is not a rational strategy to treat insomnia in most ICU patients. Rather, specific treatments such as those listed below should be tried first. The pain, agitation/sedation, delirium, immobility, and sleep (PADIS) guidelines recommend against propofol as a strategy to improve the sleep of critically ill patients, and against benzodiazepines in general (Devlin et al. 2018). Of course, there remain many specific indications for opioids or GABA-ergic sedatives in the ICU other than sleep.
Measuring sleep
If specific treatments for sleep are to be used, it would be logical to measure their effect using a validated instrument. Regrettably, sleep is more difficult to identify than most other physiological variables, and current tools are so imperfect that recent consensus guidelines (Devlin et al. 2018) recommend against routine clinical use. Nonetheless, technology is advancing rapidly in this area. Polysomnography (electroencephalogram, electromyogram and electrooculogram), the gold standard, is too complex to acquire and interpret for anything but research use. Actigraphy, using motion-sensors on the wrist, while sufficiently accurate in routine sleep studies, over-estimates sleep in critically ill patients who can be immobile for reasons other than sleep (Kamdar et al. 2012). Compressed EEG signals (primarily Bispectral Index, BIS) can estimate sleep depth, but poorly define different stages in sleep architecture and are difficult to use over many hours. Subjective assessment using the Richards-Campbell Sleep Questionnaire (RCSQ) has been validated in ICU patients and correlates well with polysomnography (Richards et al. 2000), and appears better than any technological device at present. An observational study formally comparing all of these measurement approaches is in progress (Delaney et al. 2018).
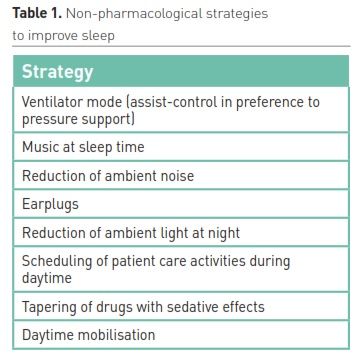
Non-pharmacological methods to improve sleep
Ventilator mode
The 2018 PADIS guidelines recommended assist-control ventilation over pressure-support ventilation, based on three comparative studies in which sleep had been measured as an outcome (Devlin et al. 2018). All three trials (which together comprised only 61 patients) found a significant benefit in sleep efficiency (proportion of time meant to be asleep actually spent asleep)(18.3% greater, 95% CI 7.9%-28.8%), and also a small but significant increase in the proportion of total sleep time spent in REM sleep. Whether this would also be true for synchronised intermittent mandatory ventilation + pressure support ventilation (SIMV+PSV) (in countries and ICUs where it is the default mode in preference to assist control) was not studied. No recommendation was made on whether adaptive modes of ventilation are beneficial. It is likely that this question is suitable for an “n of 1” trial design—that is, in a patient with insomnia, trial of a night on assist control or SIMV+PSV seems likely to lose little.
Music
One small randomised trial has tested the effect of music on sleep (Su et al. 2013). Participants listened to 45 minutes of classical-type music written specifically for the purpose, or no music. Those played music had significantly lower heart rate, blood pressure, respiratory rate, and spent significantly longer in stage N3 sleep and had significantly better subjective sleep scores.
Reduction of ambient noise
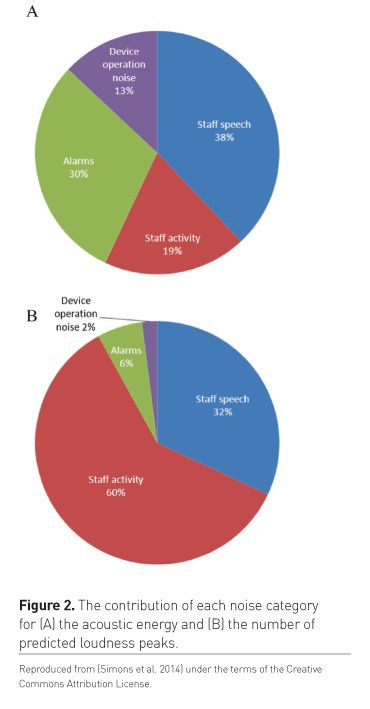
Ambient noise levels in the ICU are approximately double that recommended by the World Health Organization (Darbyshire and Young, 2013). However, background noise is probably less important for sleep disruption than the frequency and magnitude of peak levels, which were above 85dBA up to 16 times an hour. That this is not the inevitable consequence of electronic devices, mechanical ventilators, etc. was shown by a 2014 Dutch observational study (Simons et al. 2014) that found the loudness peaks (part B of Figure 2) were 60% due to staff activity and 32% due to staff speech. Only 6% were due to equipment alarms.
Earplugs
If encouraging clinical staff to be quiet is impossible, another approach could be to use patient earplugs. This is surprisingly effective, as shown by a 2017 meta-analysis of nine studies/1,455 patients (Litton et al. 2016) that found an overall relative risk of delirium of 0.59 (95% CI 0.44-0.78), although not all of the included studies measured sleep. Of those that did, two found earplugs did indeed improve self-reported sleep quality, while one did not observe any significant difference.
Light
Five studies (summarised in Bion et al. 2018) have assessed the effect of reducing environmental light at night. However, each has done this as part of a multi-component intervention that also reduced noise and other disruptions to patient sleep, and all used subjective sleep assessments. The reviewers concluded that this, combined with the different patient populations studied (from non-ventilated neuro ICU patients to mechanically ventilated ICU patients), made it difficult to reach any conclusion about the utility of this intervention alone. Nonetheless, it is difficult to argue against such a low-cost, low risk intervention as turning down the intensity of the lighting at night.
Scheduling of patient care activities
When asked, patients reported that having their vital signs assessed and having blood taken were more disruptive to sleep than any noise (Freedman et al. 1999). Critical care is a 24-hour activity, but whether medication administration, radiographs, wound care, and bathing need to interrupt sleep up to 40-60 times per night (Gabor et al. 2003; Tamburri et al. 2004) really should be questioned. Often these activities are not done for staff convenience but because of the realities of staff rostering; taking this into account at a departmental level might alleviate this major problem.
Tapering of drugs with sedative effects
Many drugs used in critical care have sedating effects, and abrupt withdrawal after a period of habituation leads to a withdrawal state characterised by hyper-alertness and insomnia. Unless there is a good reason, it is usually better to slowly reduce doses of opioids and other sedating medications over several days (Brown et al. 2000) Doing so can avoid the need to simply replace one type of sedative with another.
Mobilisation to restore day-night rhythm
Early mobilisation is to date the non-pharmacological intervention associated with the greatest observed reduction in delirium (Schweickert et al. 2009). While there are many possible mechanisms for this effect, one must be the likelihood that patients were less likely to be able to sleep during the day, and hence re-established their day-night circadian rhythm earlier than might otherwise have been the case. The cognitive and sleep effects of enhancing other daytime activities are yet to be assessed in critically ill patients.
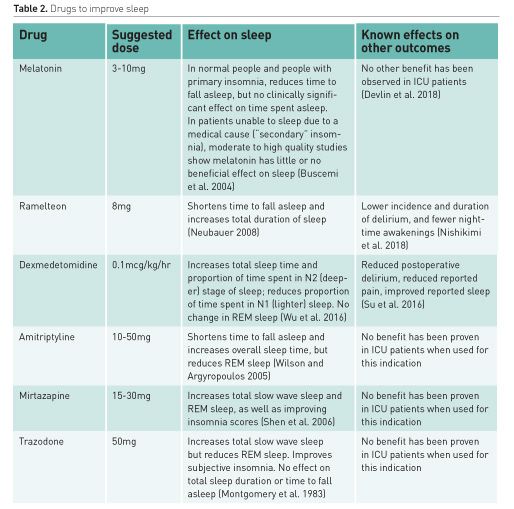
Drugs to improve sleep
Noting the adverse effects of GABA-ergic drugs when used as sedatives in critical illness, it would seem unwise to choose benzodiazepines as nocturnal sedatives in patients with or recovering from critical illness. While all of the non-pharmacological measures listed above should be considered first, some patients are so distressed by insomnia or so refractory to non-pharmacological treatment that treatment with medication should be at least attempted.
Melatonin
The 2018 PADIS guidelines make no recommendation regarding melatonin and sleep, based on three identified trials they class of low quality that enrolled a total of only 60 patients (Devlin et al. 2018). At least three more trials are planned or already recruiting in ICU populations (Prevention of Delirium in Intensive Care by Melatonin (DEMEL) [clinicaltrials.gov/ct2/show/NCT03524937], Melatonin Use in the Intensive Care Elderly Population (MICE) [clinicaltrials.gov/ct2/show/NCT03013790], and Melatonin for Prevention of Delirium in Critically Ill Patients (MELLOW-1) [clinicaltrials.gov/ct2/show/NCT02615340].
Ramelteon
One small randomised controlled trial of the melatonin-receptor agonist ramelteon was published in 2018, and two larger trials (Melatonin for Prevention of Delirium in Critically Ill Patients (MELLOW-1) [clinicaltrials.gov/ct2/show/NCT02615340] and Pro-phylactic administration of Melatonin for the prevention of Delirium in Intensive Care units – a randomized placebo controlled trial (Pro-MEDIC study) ACTRN12616000436471 [anzctr.org.au/Trial/Registration/TrialReview.aspx?id=369434] are currently underway. In the published single-centre study of 88 patients, the 45 who received 8mg/d ramelteon had nearly half the incidence of delirium (24.4% vs. 46.5%, p=0.04) of nearly half the duration (0.78 vs 1.40 days, p=0.048), and the nonintubated patients had fewer night-time awakenings (Nishikimi et al. 2018), all suggesting this is a promising intervention, apparently without substantial CNS or other adverse effects. Lack of availability in some countries currently limits utility.
Dexmedetomidine
Dexmedetomidine, an alpha-2 agonist, produces sedation in critically ill patients by a mechanism distinct from propofol and benzodiazepines. Unlike these drugs, it increases the proportion of N3 sleep (Akeju et al. 2018). In a study of 76 postoperative non-ventilated non-cardiac surgery high dependency unit (HDU) patients aged ≥ 65 years, very low dose dexmedetomidine (0.1 mcg/kg/hr) increased the proportion of N2 sleep from 15.8% (IQR 1.3-62.8%) with placebo to 43.5% (16.6%-80.2%), prolonged total sleep time, and improved subjective sleep quality (Wu et al. 2016). In a larger subsequent trial, the same investigators found the same protocol associated with significantly improved subjective sleep quality, along with less than half the incidence of postoperative delirium (9% vs. 23%; odds ratio 0.35, 95% CI 0.22-0.54; p<0.0001) (Su et al. 2016). Survival rates were higher initially with dexmedetomidine at six months, one year, and 2 years (rate difference 5.2%, 5.3%, and 6.7%, respectively; p<0.05), but after three years the difference was not significant (32.6% vs. 34.9% mortality; hazard ratio 0.87, 95% CI 0.68-1.13; p=0.303) (Zhang et al. 2018). In contrast, a study of 100 initially delirium-free critically-ill patients randomised to 0.2-0.7 mcg/kg/hr dexmedetomidine at night vs. placebo found dexmedetomidine associated with less delirium (relative risk, 0.44; 95% CI, 0.23-0.82; p=0.006), but no observable difference in sleep quality on a subjective sleep questionnaire (Skrobik et al. 2018). This led the PADIS guideline authors to be circumspect in their recommendation, stopping short of recommending dexmedetomidine for sleep alone but noting its potential benefit on sleep could be considered when choosing a sedative if one was indicated (Devlin et al. 2018).
Zolpidem, zopiclone, zaleplon, eszopiclone
Conveniently grouped as “z-drugs”, zolpidem (an imidazopyridine), zopiclone and eszopiclone (cyclopyrrolones) and zaleplon (a pyrazolopyrimidine) are non-benzodiazepine agonists of the GABAA receptor. They are claimed to have fewer adverse effects than the commonly-used sedative-hypnotic benzodiazepines (typically temazepam, diazepam and lorazepam), although there is little evidence for this. Perhaps for this reason, there has been almost no research on these drugs as ICU sedatives, and they rarely appear in critical care guidelines, including the 2018 PADIS guidelines (Devlin et al. 2018). Perhaps their only indication is to continue chronic use (in preference to abrupt withdrawal) in a patient planned to stay only briefly in the ICU.
Amitriptyline
Amitriptyline is not covered in the 2018 PADIS guideline (Devlin et al. 2018) and is recommended against by some authors on the grounds that it has “not been studied for use in insomnia and has important potential side effects including hypotension, arrhythmias, and anticholinergic syndrome. Use … to promote sleep has been discouraged by an NIH consensus panel on chronic insomnia” (Kamdar et al. 2012). However, chronic insomnia is quite different to brief treatment in ICU, and the doses usually prescribed (10-50mg nocte) are most unlikely to cause the listed complications, especially when patient weight and metabolic function are considered. Amitriptyline, the tricyclic antidepressant most commonly used as a nocturnal sedative, is generally recognised to reduce REM sleep, but to reduce sleep latency and to increase overall sleep time (Wilson and Argyropoulos 2005). Whether this provides benefit in an individual patient is readily appreciated after only 1-2 nights’ treatment. While non-pharmacological treatments are always better first-line options, given the known adverse effects of benzodiazepines and the absence of other good options, some argue that amitriptyline is a reasonable alternative.
Mirtazapine
Mirtazapine, an atypical antidepressant with a mechanism that includes presynaptic alpha-2 negative feedback blockade, postsynaptic serotonergic (5HT2 and 5HT3) blockade, and enhanced noradrenergic and 5HT1 neurotransmission, also causes somnolence as a side effect that has been used as a primary indication in some patients. Its effect on sleep in patients with major depression is more encouraging than what is known of amitriptyline: it increases total slow wave sleep and REM sleep, as well as improving insomnia scores (Shen et al. 2006). As for amitriptyline, its use in critical illness is essentially not studied, but doses of 15-30mg should be safe, and n-of-1 trials in individual patients would appear to be a reasonable strategy in the absence of large randomised trials.
Trazodone
Trazodone, a tetracyclic antidepressant, is commonly prescribed to outpatients as a treatment for insomnia as an alternative to benzodiazepines. This practice was recently supported by a systematic review of 45 studies (Jaffer et al. 2017). Its off-label use (at 50mg nocte for at most 7 days) was recommended in a 2006 guideline from the UK Intensive Care Society as an alternative to benzodiazepines, although there are no trials in this context (Borthwick et al. 2006).
Antihistamines (diphenhydramine, doxylamine)
Diphenhydramine (25-50mg nocte) and doxylamine (25mg nocte) both reduce sleep latency and increase total sleep time (Koski 2011). However, a quoted 70% increased risk of cognitive decline in a cohort study comparing hospitalised patients receiving diphenhydramine to those not receiving it, along with more behavioural disturbances (Agostini et al. 2001), have led to recommendations against the use of sedating antihistamines as nocturnal sedatives in hospitalised patients. While this is not trial evidence and these adverse effects could be the result of many cofounding influences, availability of the alternatives listed above argue against using antihistamines as first-line options in adults.
Conclusion
Facilitating sleep at night is likely to have outcome benefit in many patients, and is also likely to address the insomnia that many commonly recall as a particularly distressing memory of their ICU stay. The non-pharmacological approaches to insomnia are almost always preferable first-line alternatives in critically ill patients. There is evidence that achieving the outward manifestations of sleep through use of benzodiazepines or other GABA-ergic drugs has a net detrimental effect. There are several non-GABA-ergic alternatives that show promise, but none has convincingly shown benefit in randomised controlled trials. In part, this is due to the practical difficulties of objectively measuring sleep in critically ill patients. “N of 1” trials of certain agents until the optimal approach is found for each individual might be the best strategy, in anticipation of future definitive trials.