ICU Management & Practice, Volume 20 - Issue 4, 2020
Designing the Dream PICU
The construction of the new PICU was a challenge in terms of space and process design. The application of simulation to construct this new unit was a collaboration between the PICU, the HSJD Simulation Program, and the Boston Children’s Hospital Simulator Program (SIMPeds), Boston MA. Since 2014, HSJD and SIMPeds have maintained a collaboration agreement where SIMPeds provides support and mentorship to accelerate the development of the HSJD Simulation Program among four service lines focused on systems analysis (SIMTest), team performance (SIMTrain), scaling of training (SIMNetwork) and production of novel simulators and training devices (SIMEgineering). The SIMTest line, consists of evaluating spaces, processes and equipment using highly realistic clinical simulation.
Why Did We Use Simtest Simulation to Design the New PICU?
It is readily understandable how useful it is to test a product before putting it on the market. Nevertheless, this practice is common in other industries but rare in healthcare. SIMtest consists of bringing together professionals, simulators, actors, real medical equipment and even patients and families, in a real or pre-built facility, to understand the work in depth and resolve questions about work spaces and processes. The SIMTest methodology has a several conceptual foundations that are important to emphasise
The first is the model of different perspectives of work, as described by Shorrock: -- namely "work as imagined", "work as prescribed", "work as disclosed" and ultimately and most precisely "work as done." In practice, these four perspectives never completely overlap. Through SIMTest, we attempt to bridge the gap between work-as-imagined and and most closely approximate work-as-done. And we do it in a physically and psychologically safe environment, where an error or a design deficiency has no consequence for patients and professionals.
The second is Argyris' double-loop reflection model – referring to the finding that humans have deeply held mental models or “frames” (Eg. assumptions, culture, unwritten rules, personal factors) that drive their decisions and actions. Through SIMtest debriefings we are able to reveal those mental frames and better understand how people tend to prefer to perform work in a certain way. This information is essential to designing ergonomic and intuitive work environments and processes for greatest safety and efficiency.
The third pillar relates to “Safety Model” – namely “Safety 1 and Safety 2." According to Hollnagel, preoccupation with traditional primary focus on error and risks (“Safety 1”) often leads to an underappreciation of an equally important safety force – namely inherent human resilience and prevention measures (“Safety 2), understanding things that go well in daily work. Fostering an appreciation for both Safety 1 and 2 is the key to creating the largest impact on quality, efficiency and patient safety. SIMTest offers opportunities to elucidate and illuminate Safety 2 activities within the system.
How Did We Implement SIMtest?
The planning and execution of a SIMTest activity is a process with several stages, which are specified in Figure 1.
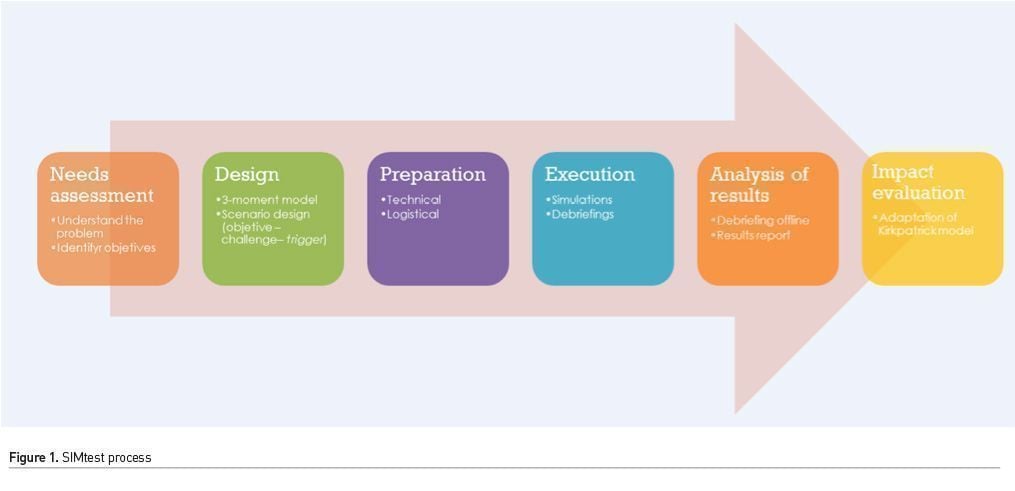
Firstly, conducting an accurate needs assessment is critical to the entire process. We carried out working sessions with a multidisciplinary group of professionals, months before the simulations took place. In the case of the new PICU, the main goal was to analyse key aspects of the transition to individual, enclosed treatment cubicles. Three specific sets of concerns were identified: one related to space (room size, internal distribution, visibility), one related to work processes (adaptation of current processes and new ways of working), and one related to the families’ experience (comfort, balance between privacy and safety).
We performed two separate operations: one before building the unit (pre-construction simulations) and another after building it but before admitting patients (post-construction simulations).
Each involved the design of highly challenging simulation scenarios for specific concerns, which were prepared with the relevant technical and logistical aspects in mind. It is important to note that the "worst case" scenario generally allows for a greater number of safety risks and successful adaptations to be identified and for participants' mental frames to emerge more clearly. The SIMTests pose a considerable technical challenge, so having an experienced simulation engineering team is critical.
Each simulation session consisted of an initial briefing (to review objectives, clarify operational roles and rules, and create a psychologically safe environment) and several consecutive scenarios, with their corresponding debriefings. These structured debriefing sessions were conducted by experienced facilitators. In the ensuing discussions, the views of participants and observers were collected and a logical "observation-cause-effect-solution" workflow was followed.
After the simulations, the team conducted a post-process information analysis and wrote a final report on the findings relevant to the design of the new PICU. Sometimes, possible solutions emerged during the debriefings and were included in the report. In other cases, the collected findings allowed the PICU and hospital managers to subsequently identify the most successful solution for each challenge.
What Simulations Did We Use to Get the Most Information?
Pre-construction simulations
Objectives: To address aspects related to room size, internal layout, and the family experience. Additionally, the details of particular work processes that could affect architectural decisions were explored.
Logistics/Implementation: A full-scale part of the future PICU was built in an unused area of the hospital, following the official draft architectural plan. The walls were made of drywall and high-fidelity patient simulators and real medical equipment were placed inside (Images 1 and 2). The participants were in-house teams of physicians, nurses, and nurse assistants from the PICU, as well as non-PICU staff when required by the scenario. Actors were incorporated to play the role of families, in order to allow teams to decide their location in complex situations and also to incorporate their experiences. Observers from different disciplines (leading physicians and nurses, engineers, architects, safety and patient experience experts, etc.) were placed at specific viewing points that did not interfere with the scenarios. A total of 62 people were involved in the execution of the 6 scenarios: 35 professionals and actors, 17 observers, and 10 members of the SIMTest team.

During the 3-day SIMTest operation, 6 scenarios were run in the full-scale PICU mock-up. The scenarios were situations that stressed the system and were focused on:
• Assessing the suitability of the planned room size in different situations (e.g., the standard 24 m2 cubicle in cannulation of ECMO patients).
• Identifying elements of the rooms that contribute to or hinder efficient and safe care delivery during critical
events.
• Identifying concerns and potential solutions related to transitioning from an open layout to enclosed cubicles.
• Determining the optimal location for the preparation of urgent medications.
• Identifying equipment solutions for families to promote parental presence in closed cubicles (striking a balance between comfort and safety).
After-action review/Debriefings: The structure of the debriefing sessions was determined by the test objectives, although elements related to patient safety, the viability of different processes, and the participants' experiences were always considered. In some cases a rapid simulation-debriefing cycle was used, in which modifications were made to the working environment based on observer feedback during the initial debriefing and parts of the simulations were repeated to test the effectiveness of the proposed changes.
Results: The simulations contributed to decisions about important aspects of the new PICU project. The final report compiled 49 sets of relevant observations and possible solutions identified during the debriefings. In a post-processing stage, the data were analysed in depth, risks and causes were assessed, and final solutions were proposed.
The pre-construction SIMTest allowed some hypotheses regarding the practical use of spaces to be validated. It was found that it was possible to cannulate ECMO on a patient in a standard-size room, as an alternative to larger treatment cubicles planned for more complex patients. It was also possible to perform CPR safely in the smaller rooms.
The analysis of spaces suggested the appropriateness of incorporating specific elements into the structure of the new PICU cubicles. Examples include the decision to make the parent beds collapsible and wall-mounted to increase work space if needed or positioning a nursing station every 2 rooms to improve safety.
Post-construction simulations
Once built and before admitting real patients, the new PICU was "opened" for 3 days with 6 simulated patients.
Objectives: Focus on the adaptation of work processes to the new environment: it was no longer a question of "where" to work, but rather "how" to do it. It aimed to explore processes that involved intense multi-professional interaction and that were highly dependent on the physical environment: preparation of medications, requests for mutual support between nurses in different situations, organisation of people and resources during a critical event, and the transfer of complex patients between treatment cubicles inside the PICU.
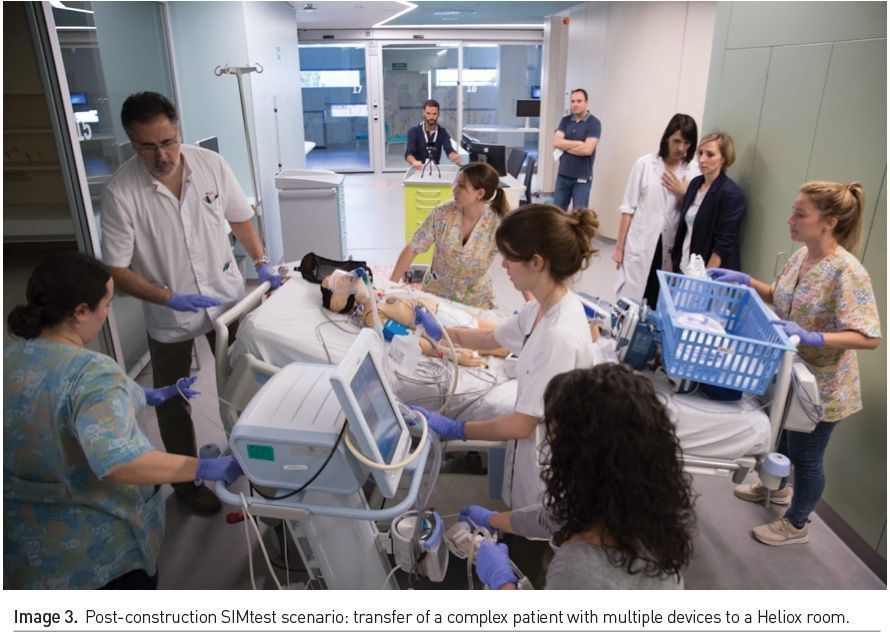
Logistics/Implementation: Seven different scenarios were run in real time with the 6 simulated patients. They involved teams of in-house PICU staff and actors (Image 3).
The medication preparation and administration process was tested by performing a rapid-cycle analysis of 3 scenarios: a complete preparation procedure in the central nurse control area, a complete procedure in the nursing station by the cubicle door, and a mixed model combining actions at both locations. Several safety risks were identified, as well as successful spontaneous adaptations of the professionals to this process. The protocol was modified to make it more robust and efficient.

The other objectives were tested in four different scenarios: a non-critical incident in a patient requiring support from another nurse and the reorganisation of care for the remaining patients, an invasive procedure involving several professionals, a patient with cardiorespiratory arrest, and the transfer of a complex patient with multiple devices to a Heliox room.
Results: The observations of these scenarios made it possible to validate protocols. The simulations led to a very important global change: the hospital approved the creation of a new position with no patients assigned on each nursing shift in order to have someone to maintain situational awareness of the unit's status, monitor the need for resources, and support the other nurses when necessary.
After-action review/Debriefings: As in the pre-construction simulations, the structure of the debriefing was defined by the objectives and also a rapid simulation-debriefing cycle was used in some scenarios.
Additional applications: Before the opening of the new PICU, all the professionals had the opportunity to participate in simulation-based workshops to experience the new spaces and familiarise themselves with the work processes. This helped to improve the experience of transitioning to a new PICU. A specific simulation room was included in the architectural project, with the same monitoring equipment as a standard treatment cubicle. In this space professionals hone their skills and improve teamwork, training on a weekly basis to increase the day-to-day integration between simulation and patient care.
What Have We Learned From the Experience?
The US Agency for Healthcare Research and Quality defines five characteristics of high reliability organisations. One of them is “deference to expertise: ” – that people closest to the work are often the most knowledgeable about the work and their relationship to it”. One of the strengths of SIMTest is that frontline professionals are deeply involved in the process from start to finish, including design of the space where they will work and in the validation of processes in these new areas. Perhaps not surprisingly, their response to the SIMTest work has been outstanding with common expressions of satisfaction emphasising the relevancy to improving their everyday workflow (Eg. “It has been extremely useful to address our concerns during the construction of our dream PICU…”, “For me, it was crucial to experience the problems we’ll have in the new PICU and learn how to solve them before we move there”).
All contributions during the debriefings are based on experiences provided by the simulation, in a safe environment. People's opinions are not only based on evocations of one's own work (“work-as-imagined”). The simulation provides a perspective ("work-as-simulated") that helps enormously to bridge the gap with the real work (“work-as-done”).
As an added value, we have observed that it is much easier to achieve consensus among different professionals during a SIMTest than in a traditional meeting. This makes it easier to empathise with other people's points of view and find realistic solutions that everyone can agree on.
An important issue is the costs vs. benefits of SIMTest activities. We did not carry out an exhaustive analysis comparing the costs of the simulations and the cost of the consequences of not having made the proposed modifications. However, we calculated that the SIMTest represented around 0.4% of the total cost of the construction project for the new PICU. The cost of modifying already-built structures or changing already-acquired equipment would have been enormously higher. Furthermore, many measures were adopted to prevent risks that the simulation brought to light. In terms of safety, this benefit is incalculable and enormously valuable to both the patients and the organisation.
Conclusion
In conclusion, SIMTest applied to the new PICU helped us to build a new, safer PICU to provide excellent care in a child and family centered model. This was the first application of simulation to facility design and construction for our hospital and represented a starting point for a line of work that has since grown steadily. Since the PICU SIMTest, about 20 other applications of SIMTests have been organised at HSJD, providing unique tools to improve the design and work processes related to new spaces in the Neonatology Unit and Cancer Center to name a few. As another example, recent SIMTest-based work has contributed to the design of processes related to MRI-guided intracranial tumor ablation, as well as the its timely application to optimising safe care within the COVID-19 pandemic.
SIMTest provides us with a controlled and safe parallel reality and allows us to reflect and learn from experience. This learning translates into better workspaces and safer processes.
Conflict of Interest
Catherine Allan obtained a grant through AHRQ (R18: Advances in Patient Safety through Simulation Research).The other authors state no conflict of interest related to this article 
Abbreviations
HSJD: Hospital Sant Joan de Déu
PICU: Paediatric Intensive Care Unit
ECMO: Extracorporeal memebrane oxigenation
CPR: Cardiopulmonary Resuscitation
References:
Argyris C (1991) Teaching Smart People How to Learn. Harvard Business Review . Reflections, 4(6).
Hollnagel E, Leonhardt, J, Licu T Shorrock S (2013) From Safety-I to Safety-II: A White Paper. Brussels, Belgium: EUROCONTROL. Available from skybrary.aero/bookshelf/books/2437.pdf
Hollnagel E (2014). Safety-I and Safety-II: The past and future of safety management. Farnham, England: Ashgate.
Shorrock S (2016) The varieties oh human work. Available from https://humanisticsystems.com/2016/12/05/the-varieties-of-human-work/
Shorrock S, Leonhardt J, Licu T, Peters C (2014). Systems thinking for safety: Ten principles. A white paper. Brussels: EUROCONTROL. Available from bit.ly/ST4SAFETY
US Agency for Healthcare Research and Quality: high reliability organizations. Available from psnet.ahrq.gov/primer/high-reliability
EA20












