ICU Management & Practice, Volume 19 - Issue 3, 2019
The fifth edition of the European Trauma Treatment Guidelines that have already been cited 1650 times and downloaded from the original home page nearly 600,000 times.
The European trauma treatment guidelines have significantly changed the treatment modalities of trauma patients around the world. The guidelines have also been endorsed by major European professional societies including European Society of Anaesthesiology (ESA), European Society of Intensive Care Medicine (ESICM), European Shock Society (ESS), European Society for Trauma and Emergency Surgery (ESTES), European Society for Emergency Medicine (EuSEM), Network for the Advancement of Patient Blood Management, Haemostasis and Thrombosis (NATA). There is, therefore, profound consensus with respect to these guidelines.
This updated version of the guidelines considers all the scientific evidence that has been produced during the last three years as well as evidence from current clinical practice. The existing suggestions and recommendations were revised by a group of experts, mainly delegates of European professional societies.
In the fifth version, there is more elaboration on the pathophysiology of trauma-induced coagulopathy. The organisation of the guidelines reflects the decision-making process along the patient pathway and less the treatment modalities. There are now nine chapters which are comparatively more patient and problem-oriented. The former chapter on resuscitation measures has been reorganised into three separate chapters (Chapters VI, VII, VII). Table 1 outlines the major issues/topics discussed in the new chapters (Spahn et al. 2019).

Key Recommendations in the Revised Guidelines
Some of the key recommendations in the revised guidelines include the following (Spahn et al. 2019):
- Routine practice should include the early and repeated monitoring of haemostasis, using either a combined traditional laboratory determination [prothrombin time (PT), platelet counts and fibrinogen] and/or point-of-care (POC) PT/international normalised ratio (INR) and/or a viscoelastic method (VEM). As per the new addition, laboratory tests are graded equally to the VEM test, and the Activated Partial Thromboplastin Time (APTT) is deleted because it is unspecific and does not offer any interpretation in the context of major trauma. Also, early and repeated are both very important terms in this recommendation because it is important to get an idea about the problem early on in order to determine whether it has been treated or whether there is a need for a second round of treatment with the same or with other treatment modalities.
- Patients treated or suspected of being treated with anticoagulant agents should be screened.
- Tranexamic acid (TXA) should be administered to the trauma patient who is bleeding or at risk of significant haemorrhage as soon as possible and within 3h after injury at a loading dose of 1g infused over 10 minutes, followed by an IV infusion of 1g over 8 hours. This is still in place as the last version.
- Protocols for the management of bleeding patients should consider the administration of the first dose of TXA en-route to the hospital. The important thing is to give it as early as possible.
- The administration of TXA should not await results from a viscoelastic assessment. It should always be given and it should be given as early as possible.
- In the initial management of patients with expected massive haemorrhage, it is recommended that one of the two following strategies should be followed:
- FFP (fresh frozen plasma) or pathogen-inactivated FFP in an FFP:RBC (red blood cells) ratio of at least 1:2 as needed.
- Fibrinogen concentrate and RBC.
- As per the revised guidelines, both measures are graded equally and should be determined based on a goal-directed strategy.
- Resuscitation measures should be continued using a goal-directed strategy, guided by standard laboratory coagulation values and/or VEM.
- Treatment with fibrinogen concentrate or cryoprecipitate should be initiated if major bleeding is accompanied by hypofibrinogenaemia (viscoelastic signs of a functional fibrinogen deficit or a plasma Clauss fibrinogen level ≤1.5 g/L).
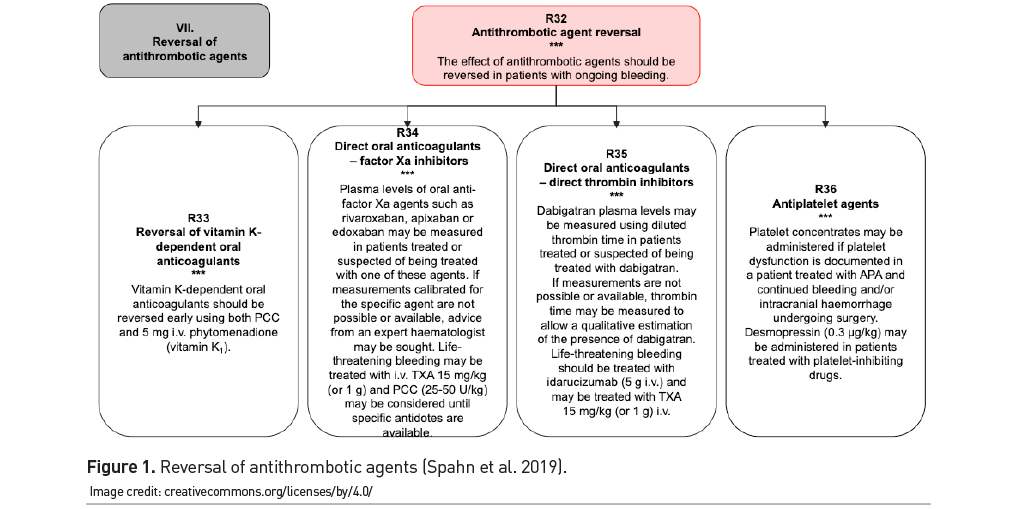
- Reversal of the effect of antithrombotic agents in patients with ongoing bleeding is recommended. The need for reversal should be weighed against the prothrombic state of the patient. This is because patients taking antithrombotic medications have an underlying thrombotic risk. Full reversal of the anticoagulant is only justified if there is life-threatening bleeding (ema.europa.eu/en/medicines/human/summaries-opinion/ondexxya). This is a new chapter in the guidelines, details of which are outlined in Figure 1 (Spahn et al. 2019).
- Appropriate thromboprophylaxis should be initiated as soon as possible after bleeding has been controlled.
- In the bleeding trauma patient, the emergency reversal of vitamin K-dependent oral anticoagulants is recommended with the early use of both prothrombin complex concentrates (PCC) and 5mg IV phytomenadione (vitamin K1).
- Measurement of plasma levels of oral direct anti-factor Xa agents such as apixaban, edoxaban, or rivaroxaban should be done in patients treated or suspected of being treated with one of these agents.
- Measurement of anti-Xa activity should be calibrated for the specific agent. If measurement is not possible or available, advice from an expert haematologist should be sought.
- If bleeding is life-threatening, TXA 15 mg/kg (or 1g) should be administered intravenously, and the use of PCC (25-50 U/kg) be considered until specific antidotes are available.
- Dabigatran plasma levels should be measured using diluted thrombin time in patients treated or suspected of being treated with dabigatran.
- If measurement is not possible or available, standard thrombin time should be measured to allow a qualitative estimation of the presence of dabigatran.
- If bleeding is life-threatening in those receiving dabigatran, patients should be treated with idarucizumab (5g intravenously) and with TXA 15 mg/kg (or 1 g) intravenously.
Key Points
- Injured patients should be transported quickly and treated by a specialised trauma centre whenever possible.
- Measures to monitor and support coagulation should be initiated as early as possible and used to guide a goal-directed treatment strategy.
- A damage control approach to surgical intervention should guide patient management.
- Coagulation support and thromboprophylactic strategies should consider trauma patients who have been pre-treated with anticoagulants or platelet inhibitors.
- Local adherence to a multidisciplinary, evidence-based treatment protocol should serve as the basis of patient management and undergo regular quality assessment.
Abbreviations
APTT activated partial thromboplastin time
FFP fresh frozen plasma
INR international normalised ratio
PCC prothrombin complex concentrates
POC point-of-care
PT prothrombin time
RCB red blood cells
TXA tranexamic acid
VEM viscoelastic method
References:
Spahn DR, Bouillon B, Cerny V, Duranteau J, Filipescu D, Hunt BJ, Komadina R, Maegele M, Nardi G, Riddez L, Samama C, Vincent JL, Rossaint R (2019) The European guideline on management of major bleeding and coagulopathy following trauma: fifth edition. Critical Care 23:98.
European Medicines Agency. Ondexxya for reversal of anticoagulation. Available from ema.europa.eu/en/medicines/human/summaries-opinion/ondexxya







