ICU Management & Practice, Volume 22 - Issue 2, 2022
Introduction
In 2017, an international group of intensivists with a particular interest for geriatric intensive care published a statement paper (Flaatten et al. 2017). This paper discussed the status of research in the very old critical ill patients, and what should be the priorities for such research in the coming years (Table 1). In this overview we seek to find out where this area of research stands five years later. Are any of the suggested topics better described and have new and important issues emerged?
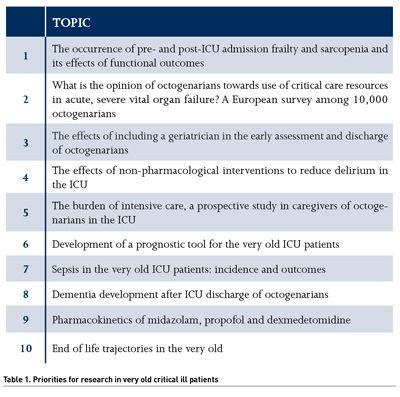

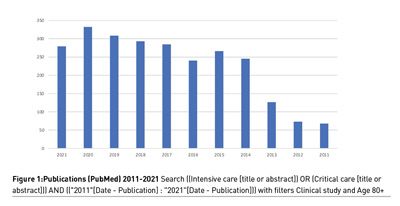
If we look at the absolute numbers of related clinical research in this group, we see a considerable increase from 2011 until today, in total 2124 publications, but the number of publications has stabilised the last five years around 300 publications per year (Figure 1). Hence publications on the very old ICU patients measured as published paper seems still to attain a high interest.
The topics of the publications are more diverse. With the same research string but adding 11 specific topics found either in the title or the abstract, we found a more diverse picture. The topics of interest spread from low interest like severity score (n=20) to high interest like outcome (n=485) (Figure 2). One topic occurred and peaked in 2020 and 2021 - COVID-19. We found this despite only covering two years to be overall the third most popular topic over the 5-year period and was by far the highest in 2021 with 142 papers. The topics within the COVID-19 subgroup naturally varied to cover a broad spectrum.
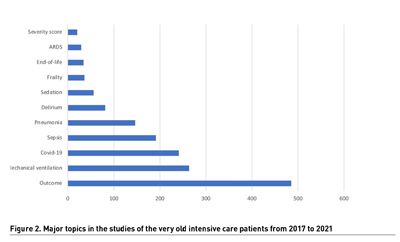
Comparing these findings with Table 1 reveals that several items found to be important in 2017 are poorly covered. This goes for the more soft items like the study of opinions among elderly about intensive care, end-of life issues, frailty and sedation. These are all important topics that merit more focus.
COVID-19 and the Elderly Group of ICU Patients
Old patients have paid a severe tribute to COVID with a disproportionate number needing admission to an intensive care and a large proportion succumbing from the disease. In the beginning of the pandemic, several countries issued recommendations for admission and treatment of the most severe cases. However, little was known about the validity and applicability of such recommendations for the group of old critically ill patients. Since most of the interventional studies excluded old patients or included only a small number, there is doubt for extrapolating data to an old population.
Our VIP network has been active since 2017 and it was straightforward to adapt our CRF to the COVID surges and to motivate centres to participate. As a result, the COVID-19 in very old ICU patients (COVIP) study recruited 3140 patients older than 70 years from 19 March 2020 to 4 February 2021 in more than 150 ICUs across 15 European countries. COVIP is a prospective observational study looking at patient demographics, treatment modalities in ICU and outcomes included health related quality of life up to three months after admission to the ICU.
We confirmed the poor prognosis in this old population with only 39% of the patients surviving up to 90-days (Jung et al. 2021a). Further, we documented that the effect of crude age is less important that the degree of frailty in this group. Outcome in patients above 70 in the presence of frailty was not influenced by age. In our quality analysis of outcome within the group of surviving patients 48% (n = 592) experienced ‘severe problems’ or ‘extreme problems’ in at least one of the five domains of the EQ-5D-5L questionnaire (Soliman et al. 2022). ‘Severe problems’ were mentioned by 41% (n = 496), and ‘extreme problems’ on one of the five domains in 30% (n = 371).
Another important issue included in the COVIP study was an analysis of the use of steroids. It was commonly acknowledged that systemic steroids were beneficial for hospitalised patients with COVID-19, but with insufficient documentation to conclude in the very old patient group. In a comparison of patients receiving steroids or not during the first and second surge in Europe, we found an independent association of steroids with increased mortality from 14 days after ICU admission (Jung et al. 2021b).
Early tracheostomy was not found to be of benefit, and we documented huge variability in the use of this procedure across European countries (Polok et al. 2021). We were expecting improved prognosis from severe COVID-19 from the first to the second surge in parallel with optimisation of oxygenation therapy, avoidance of early invasive mechanical ventilation and use of steroids. In fact, we found treatments to differ during the second wave with less invasive mechanical ventilation and more use of steroids. However, these differences did not translate into better outcomes since the mortality was significantly higher in the second wave compared to the first one (Jung et al. 2021c). This higher mortality could be related to different admission policy and pressure on ICU beds (Jung et al. 2021c) and to the above mentioned use of steroid treatment that was detrimental in old patients.
We have further shown that pressure on ICU beds increased the number of decisions to limit life-sustaining treatment (LST) (Jung et al. 2022). We will claim that information on withholding and withdrawing LST is crucial to interpret survival curves and have been missing in most outcome papers including critical ill elderly patients (Flaatten et al. 2022).
We also took advantage of information from a previous cohort in patients without COVID (VIP2 study) to compare patient characteristics, treatment and outcome between COVID and non-COVID patients older than 80 years admitted for acute respiratory failure (Guidet et al. 2022). This was obtained with matching the propensity score and regression analysis patients from the two cohorts. In this study we found elderly COVIP patients to be less sick (lower SOFA score), less frail (lower CFS) but with more decision to forgo LST and with a higher one-month mortality.
Conclusions
This overview reveals an increase in publications about critically ill ICU patients during the last five years. However, the topics of interest for publications follows traditional patterns with outcome, sepsis, and mechanical ventilation as the most popular issues. An exception is the large number of publications following the COVID-19 pandemic. Specific age-related issues like frailty, end-of life issues and prognostications (severity score) are less frequently published. We could not find any publications related to the wishes of elderly persons or their family with regards to receiving intensive care.
We hope our VIP network will continue to reveal new knowledge about the very old ICU patients also in the future. More knowledge of this group is crucial if we want to overcome the challenge of the rapid increase in the population of elderly across the globe, and concomitant huge increase in very old ICU patients. We should not stop to treat elderly critical ill patients, but we need to know more about those who will not profit from such intervention for the benefit of the elderly themselves and their families.
Conflict of interest
None.
References:
Flaatten H et al. (2017) The status of intensive care medicine research and a future agenda for very old patients in the ICU. Int Care Med. 43 1–10.
Flaatten H et al. (2022) The importance of revealing data on limitation of life sustaining therapy in critical ill elderly COVID-19 patients. J Crit Care. 67:147-148
Guidet B et al. (2022) Increased 30-day mortality in very old ICU patients with COVID-19 compared to patients with respiratory failure without COVID-19. Int Care Med. 1-13. Epub ahead of print.
Jung C et al. (2021a) The impact of frailty on survival in elderly intensive care patients with COVID-19: the COVIP study. Critical care. 25, 149.
Jung C et al. (2021b) Steroid use in elderly critically ill COVID-19 patients. Eur Respir J. 58(4):2100979.
Jung C et al. (2021c) Differences in mortality in critically ill elderly patients during the second COVID-19 surge in Europe. Crit Care. 25:344.
Jung C et al. (2022) The relationship between treatment limitations and pressure on intensive care units in elderly patients. Intensive Care Med. 48(1):124-25.
Polok K et al.(2022) Association between tracheostomy timing and outcomes for critically ill COVID-19 patients aged ≥70 years: Prospective observational study in European intensive care units. Brit J Anaesth. 128(3):482-90
Soliman IW et al. (2022) Health-related quality of life in older patients surviving ICU treatment for COVID-19: results from an international observational study of patients older than 70 years. Age Ageing. 51:afab278.









