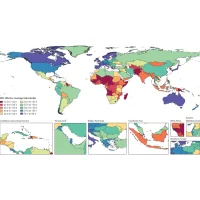
Over 100 countries from five regions participated in the World Health Organization (WHO) survey on the impact of COVID-19 on health systems. The results show that in the overwhelming majority of countries, especially low- and middle-income ones, experienced disruption to their health services, including both routine and elective services as well as critical care.
You might also like:COVID-19 Technology Access Pool is Launched
With this project, conducted
over the period from March to June 2020, WHO aimed to understand how the COVID-19 pandemic impacted up
to 25 essential health services and how countries approached the challenges and
maintained essential services. Despite some limitations to the survey, it is
claimed to be comprehensive and providing comparable data from different
countries. Ultimately, 105 countries responded to the survey.
The key findings include the following.
- On average, countries experienced disruptions in 50% of 25 tracer services. It included severe/complete disruptions (i.e. service provision or use changed by over 50%) in routine immunisation, non-communicable diseases diagnosis and treatment, family planning and contraception, treatment for mental health disorders and cancer diagnosis and treatment. The majority of service disruptions were partial (i.e. service provision or use changed by 5–50%), e.g. in the case of malaria and tuberculosis diagnosis and treatment. Emergency services were the least disrupted, but the disruptions were still reported by almost a quarter of responding countries.
- Among the 105 countries, 80% had had packages of essential health services in place prior to the pandemic and 66% had already identified a core set of services, which are essential during the pandemic.
- A combination of supply and demand factors caused the disruptions. On the demand side, over three quarters of responding countries saw outpatient care attendance reduced, lockdowns mitigating access and increased financial challenges. On the supply side, two thirds reported cancellation of elective services as the most evident factor, followed by insufficient personal protective equipment provision, staff redeployment, unavailability of some services and interruptions in the supply of medical equipment and health products.
- The strategies to maintain essential health services varied across the responding countries. The most common approaches included triage of health services, telemedicine deployment, changes to prescribing practices and supply chain and public health information strategies. Notably, only 14% eliminated user fees as recommended by WHO.
Based on the results of the
survey, WHO stresses that it is necessary to
improve real-time monitoring of changes in service delivery and utilisation and
use this information to inform public health strategies. Understanding the need
for assistance reported by many countries, WHO is developing the COVID19:
Health Services Learning Hub, a web-based platform that will allow sharing
of experiences and learning from innovative country practices.
The full text of the ‘Pulse survey on continuity of essential health services during the COVID-19 pandemic’ is available here.
Source and image credit: WHO