Safe healthcare organisations need to anticipate and prevent harm to patients. In this article, a framework for measuring and monitoring healthcare safety is presented.
The framework, developed by the Health Foundation has potential uses in supporting healthcare organisations to understand how safe their servies are and in identifying the relative strengths and weaknesses of current safety measures. However, implementation of the framework requires regulatory and mangerial support, and staff need sufficient time and resources to address the questions in the framework.
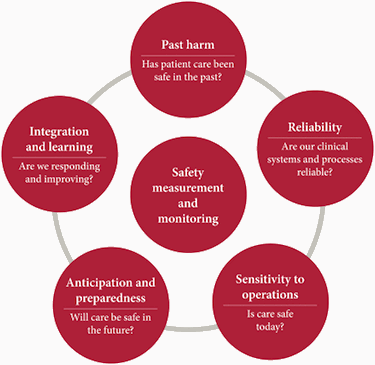
The Health Foundation has developed prompts for healthcare organisations to apply the framework in their own facility.
1. Past harm – has patient care been safe in the past?
Identify the different types of harm that can exist in your setting
Use a range of safety measures, while understanding their strengths and limitations
Ensure the measures are valid, reliable and specific
2. Reliability – are our clinical systems and processes reliable?
Specify the level of reliability you would expect in areas of standardised practice
Use local and national audits and initiatives to monitor reliability
Understand what contributes to poor reliability
3. Sensitivity to operations – is care safe today?
Select an appropriate mix of formal and informal safety monitoring mechanisms
Use the information to take action to avert safety issues
Reflect on whether current structures and committees enable timely action to be taken
4. Anticipation and preparedness – will care be safe in the future?
Don’t wait for things to go wrong before trying to improve safety
Explore new opportunities to develop systematic ways to anticipate future risks
Use a variety of tools and techniques to build an understanding of the factors that give rise to safety issues
5. Integration and learning – are we responding and improving?
Use the analysis of incidents to reveal the wider issues in the system
Place more emphasis on learning, feedback and action than simply on data collection
Integrate and tailor information to make it meaningful from the ward to the board
Illingworth notes that this framework "enabled people to think about stopping the collection of some measures that were not adding value, as well as suggesting new ones." It was effective when teams assessed honestly what their strengths and weaknesses were, and when teams thought about the questions in depth rather than as a checklist to 'tick off.' He recommends that users refger to the research report, which has more details and case studies to consider what the framework means in the particular clinical context.
Illingworth summarises:
"There was general agreement from healthcare leaders that a move to understanding and measuring factors that relate to future risk was critical to improving safety. However, this needs to be matched by an approach from regulators that is aligned and mature, rather than overlapping and prescriptive. This article concludes that the public, front line health professionals, managers and leaders alike should be meaningfully engaged in an open conversation about how to build a safer NHS."
Latest Articles
Guidelines, Healthcare, patient safety, patient care, healthcare management
Safe healthcare organisations need to anticipate and prevent harm to patients. In this article, a framework for measuring and monitoring healthcare safety...










