The novel coronavirus COVID-19 continues its spread globally. Public authorities are implementing various measures to contain or delay it, from complete or partial territorial lockdowns to closing schools to banning larger public gatherings. In this situation healthcare systems are on the front line, and hospitals and healthcare leadership must take necessary steps to ensure the safety of their staff, patients and the wider community.
You may also like: COVID-19 Clinical Guidance for Cardiovascular Care
Current Situation
According to the latest World Health Organization’s situation report (12 March 2020), there are over 125,000 confirmed COVID-19 cases in the world, with 4,613 deaths, of which China accounts for 3,173. Since late February, the majority of cases reported are from outside China, with an increasing majority of these reported from EU/EEA countries and the UK.Italy represents 58% of the cases and 88% of the fatalities. The WHO declared the outbreak a pandemic on 11 March.
The evidence so far suggests that about 80% of cases are mild (including subclinical). Most cases recover, 13-15% develop moderate to severe disease requiring oxygen supplementation and hospitalisation, and 5-6% experience critical illness requiring ICU support. The elderly and those with other chronic underlying conditions account for the majority of severe disease and fatalities to date (WHO 2020a).
The European Centre for Disease Prevention and Control (ECDC 2020a) estimates the pattern of increase in COVID-19 cases in EU/EEA as very similar to that of Hubei province in mid- and late-January 2020. The majority of European countries would reach the Hubei scenario by end of March and all countries by mid-April 2020.
Despite the increased efforts from all stakeholders, the report by the ECDC (2020a) point out that many unknowns remain regarding the virulence/pathogenicity, the effectiveness of different modes of transmission, the proportion of mild and asymptomatic cases, the infectivity during the incubation period and during recovery, the impact of individual or population-based preventive measures, the risk factors for severe illness besides age, and the effectiveness of treatment regimes. So far, detailed epidemiological data available are still limited, which complicates the efficient crisis management in healthcare.
Complications for Healthcare
The spread of the disease could result in increased hospital admissions, and already stretched capacity would be further exacerbated if substantial numbers of healthcare workers become infected or need to be isolated. In the event of a disruption of healthcare services, the impact could be very high, both in terms of public health/overall healthcare system and economic and societal disruptions. The ECDC considers the risk of transmission of COVID-19 in health and social institutions with large vulnerable populations to be high. Therefore, hospital preparednessand activation of contingency plans is an absolute priority at this moment, underscores the ECDC. Additional precautions are required by healthcare staff, in terms of very early detection and highly effective infection control, to protect themselves and prevent transmission in the healthcare setting.
Healthcare organisations should prepare to address the high demand for care of increased numbers of patients with moderate or severe respiratory distress (Murthy et al. 2020), focusing on the availability of ventilator equipment and personal protective equipment (PPE).
Based on the evidence from China, South Korea and Italy, hospitals need to:
- Discourage symptomatic patients from personal visits to any facility without prior instructions.
- Designate treatment facilities for both mild and severe COVID-19 cases with critical care capabilities, including cancellation of nonurgent procedures, redeployment of staff, creating temporary treatment facilities among others.
- Ban access to hospitals to visitors.
- Decrease the administrative workload for personnel to free up resources.
- Prepare/adapt business continuity plans for healthcare facilities.
Checklist for Hospitals
To support hospital preparedness for the management of COVID-19 patients, ECDC has developed a checklist (2020b) covering the following areas:
- Establishment of a core team and key internal and external contact points
- Human, material and facility capacity
- Communication and data protection
- Hand hygiene, personal protective equipment (PPE), and waste management
- Triage, first contact and prioritisation
- Patient placement, moving of the patients in the facility, and visitor access
- Environmental cleaning
Detailed information on each of the areas can be found here.
It is noted that the recommendations may vary
depending on the
specific characteristics of the hospital and other factors.
Infection prevention and control (IPC)
The WHO recommends the following controls in healthcare settings for epidemics and pandemics (WHO 2014).
- Administrative: appropriate infrastructure, clear policies, laboratory testing, appropriate triage and placement of patients, adequate staff-to-patient ratios and training of staff.
- Environmental and engineering: space to allow social distance of at least 1 m, well-ventilated isolation rooms, availability and proper use of PPE.
The ECDC technical report (ECDC 2020c)for administrators and healthcare professionals provides guidance for preparedness; triage, initial contact and assessment in primary and emergency care; patient transport; environmental cleaning; and waste management. Some of the recommended measures include:
- Designation of a full-time staff member as the lead for IPC and preparedness for COVID-19, responsible for the relevant education and training of staff.
- Respiratory hygiene measures (covering mouth/nose with a tissue or elbow when coughing or sneezing, wearing medical masks in certain cases, performing hand hygiene, staff self-isolating if suspected of being infected).
- Allocating additional facilities to cohort cases with mild symptoms.
- Availability of isolation rooms, appropriate PPEs (ECDC 2020d), adequate laboratory support, etc.
- Appropriate use of PPEs.
- Regular cleaning followed by disinfection.
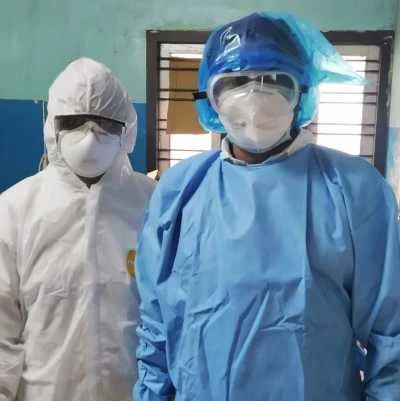
Personal Protective Equipment
As of March 2020, there is reduced access to PPE and hand hygiene materials across the globe, therefore, rational use of PPE and hand hygiene materials for the care and management of COVID-19 is encouraged (WHO 2020b). For staff this involves selecting the proper PPE and being trained in how to put on, remove and dispose of it.
Optimal PPE availability can be achieved through the following steps:
- Minimising the need for PPE by means of telemedicine, using physical barriers (glass or plastic windows) to reduce exposure, restricting staff’s presence in the rooms of COVID-19 patients (also consider bundling activities), restricting visitors’ access to facilities, and providing clear instructions regarding PPE use and hand hygiene.
- Ensuring rational and appropriate use of PPE (staff using specific PPE for various types of care, efficient allocation of masks, coordinated PPE supply chain management mechanisms).
If PPE stocks are insufficient, staff should be allocated to perform a procedure, or set of procedures in designated areas.
Other recommendations for hospitals include developing a strategy for patient volume and complexity including provisions for geographical cohorting and supplies conservation; readjusting staff’s schedules with appropriate compensation strategies; monitoring staff for signs or symptoms of infection; ensuring transparent communication and providing moral support (Chopra et al. 2020). Bolstering the general approach to routine respiratory viruses is another recommended direction as it will simultaneously improve care for current patients, make work safer for clinicians and help to prevent nosocomical transmission of COVID-19 (Klompas 2020).
References
Chopra V et al. How Should U.S. Hospitals Prepare for Coronavirus Disease 2019 (COVID-19)?. Ann Intern Med. 2020; [Epub ahead of print 11 March 2020]. Available from: https://doi.org/10.7326/M20-0907
European Centre for Disease Prevention and Control (2020a) Rapid Risk Assessment: Novel coronavirus disease 2019 (COVID- 2019) pandemic: increased transmission in the EU/EEA – sixth update. ECDC: Stockholm. Available from: https://www.ecdc.europa.eu/sites/default/files/documents/RRA-sixth-update-Outbreak-of-novel-coronavirus-disease-2019-COVID-19.pdf
European Centre for Disease Prevention and Control (2020b). Checklist for hospitals preparing for the reception and care of coronavirus 2019 (COVID-19) patients. ECDC: Stockholm. Available from: https://www.ecdc.europa.eu/sites/default/files/documents/covid-19-checklist-hospitals-preparing-reception-care-coronavirus-patients.pdf
European Centre for Disease Prevention and Control (2020c). Interim guidance for environmental cleaning in non-healthcare facilities exposed to SARS-CoV-2 2020. Available from: https://www.ecdc.europa.eu/sites/default/files/documents/coronavirus-SARS-CoV-2-guidance-environmental-cleaning-non-healthcare-facilities.pdf
European
Centre for Disease Prevention and Control (2020d). Guidance for wearing and
removing personal protective equipment in healthcare settings for the care of
patients with suspected or confirmed COVID-19 2020. Available from: https://www.ecdc.europa.eu/en/publications-data/guidance-wearing-and-removing-personal-protective-equipment-healthcare-settings
Klompas M (2020) Coronavirus Disease 2019
(COVID-19): Protecting Hospitals From the Invisible. Ann Intern Med [Epub ahead
of print 11 March 2020]. Available from: https://doi.org/10.7326/M20-0751
Murthy S et al. Care for Critically Ill Patients With COVID-19. JAMA. Published online 11 March 2020. https://jamanetwork.com/journals/jama/fullarticle/2762996
World Health Organization (2020a). Report of the WHO-China Joint Mission on Coronavirus Disease 2019 (COVID-19) 2020. Available from: https://www.who.int/docs/default-source/coronaviruse/who-china-joint-mission-on-covid-19-final-report.pdf.
World Health Organisation (2020b). Rational use of personal protective equipment for coronavirus disease 2019 (COVID-19) 2020 [updated 27 February 2020]. Available from: https://apps.who.int/iris/bitstream/handle/10665/331215/WHO-2019-nCov-IPCPPE_use-2020.1-eng.pdf
World Health Organisation (2014) Infection prevention and control of epidemic-and pandemic-prone acute respiratory infections in health care. Geneva: World Health Organization. Available from:
https://apps.who.int/iris/bitstream/handle/10665/112656/9789241507134_eng.pdf
Image credit: By Javed Anees - District Hospital, Tirur, CC0, Wikimedia Commons


![Tuberculosis Diagnostics: The Promise of [18F]FDT PET Imaging Tuberculosis Diagnostics: The Promise of [18F]FDT PET Imaging](https://res.cloudinary.com/healthmanagement-org/image/upload/c_thumb,f_auto,fl_lossy,h_184,q_90,w_500/v1721132076/cw/00127782_cw_image_wi_88cc5f34b1423cec414436d2748b40ce.webp)