HealthManagement, Volume 20 - Issue 9, 2020
Why health governance and operations matter to implement interventions fast. Bavarian perspective
Key Points
- The COVID-19 pandemic heavily affects elderly population in long-term care facilities.
- Health governance priorities with clear protocols matter.
- Central support and operations are key to accelerating implementation and eliminating misinformation.
Background Situation
To date, the COVID-19 pandemic has heavily affected the elderly populations worldwide, leading to a significant number of deaths in people of 60 years and older. Long-term care (LTC) settings, especially care homes, have experienced large COVID-19 outbreaks associated with high fatality rates. International comparisons are still challenging due to different sources and incomplete datasets, as well as different definitions and aggregation levels. Nevertheless, recent studies have started to shed some light on COVID-19 fatalities linked to LTC settings (WHO 2020; BMSGPK 2020; Comas-Herrera et al. 2020a, 2020b).
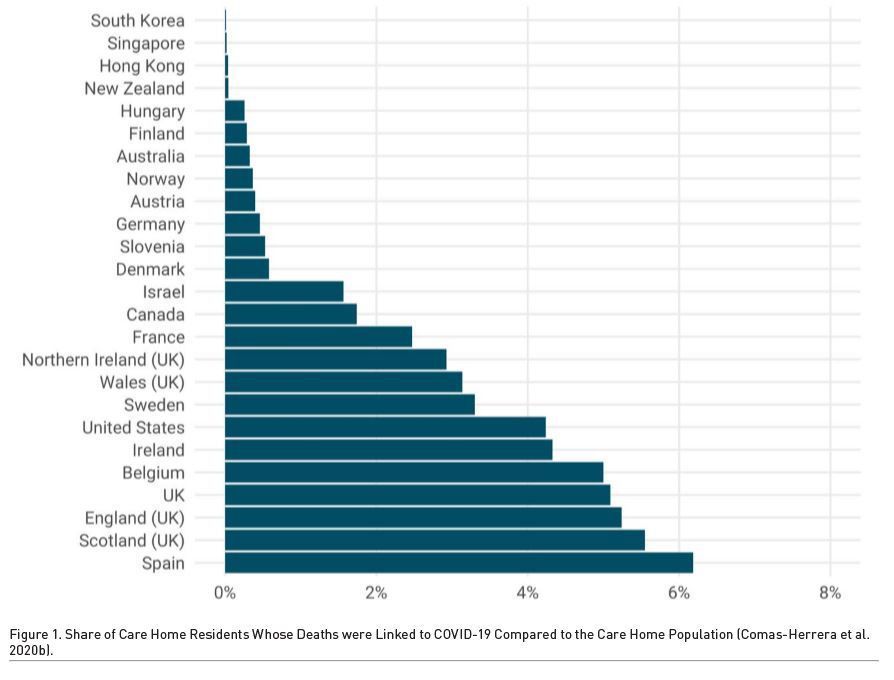
Fatality rates among elderly people are significantly higher than among total population in all countries, though the share of fatalities due to COVID-19 in care homes varies from country to country. Data show that in Germany, Austria or Denmark, the fatality rate is between 0.4% and 0.5% of the total population linked to care homes. In contrast, the share of care home residents dying due to COVID-19 amounts to 4.9% in Belgium, 5.3% in the UK and 6.1% in Spain (Comas-Herrera et al. 2020b).
Even more alarming is the fact that in several European countries more than 35% of all COVID-19 related deaths were linked to LTC facilities. In Germany, for example, 35% of COVID-19 deaths have been reported in such facilities; in the US, 45%; in Belgium, 64% (Comas-Herrera et al. 2020b).
The severe impact of the SARS-CoV-2 spread in LTC settings has led to the World Health Organization (WHO) issuing a policy paper, which flags the severe weaknesses in emergency response with regard to LTC services worldwide and outlines key policy objectives to help mitigate the risk of the COVID-19 spread across LTC facilities (WHO 2020).
As it is still very early to make a systematic assessment of the attainment of all objectives, individual case studies can help shed light on different societal conditions and different approaches and strategies of emergency response. Case study examples can particularly help further identify and specify effective approaches that have been proven successful in mitigating the risk of the spread among residents of LTC such as the elderly or people with disabilities. For instance, countries such as Germany put very thorough measures in place early on in the pandemic to protect the elderly. Bavaria in particular, as one of the most affected federal states of Germany, took a coordinated approach early on to protect the elderly and people with disabilities living in LTC facilities.
As these measures were followed by a substantial drop in the infection and mortality rates in the subsequent weeks of the outbreak, an analysis of the Bavarian example might provide some indications as to which measures to implement the policy objectives identified by WHO have proven effective in mitigating the risk of COVID-19 in a coordinated and timely manner.
This article thus presents the Bavarian COVID-19 strategy towards LTC, focussing on factors that might offer insights into its effectiveness, such as identification and prioritisation of coordinated policy objectives to mitigate the COVID-19 impact on the elderly through effective implementation structure of interventions.
As the second wave of the pandemic is on the rise worldwide, the purpose of this article is to share the lessons of the timely measures taken in Bavaria so that others could learn from this experience. To this end, the paper relies on a descriptive case study methodology instead of a comparative study at this stage.
Strategies Against COVID-19 Spread in Care Homes
After the initial rise of case fatalities due to COVID-19 among the elderly worldwide, different institutions started releasing guidelines as early as in February 2020 to provide guidance on how to mitigate the risk of outbreaks in LTC settings. While the initial focus was on the health sector in general, many guidelines subsequently embraced strategies of protecting the vulnerable population in LTC facilities.
For instance, the European Centre for Disease Control (ECDC) has been publishing guidelines for 2019-nCoV-2 infection control and prevention in healthcare settings from February 2020 onwards. This has been complemented by a technical report for EU/EEA Member States planning to implement monitoring systems at LTC facilities (ECDC 2020).
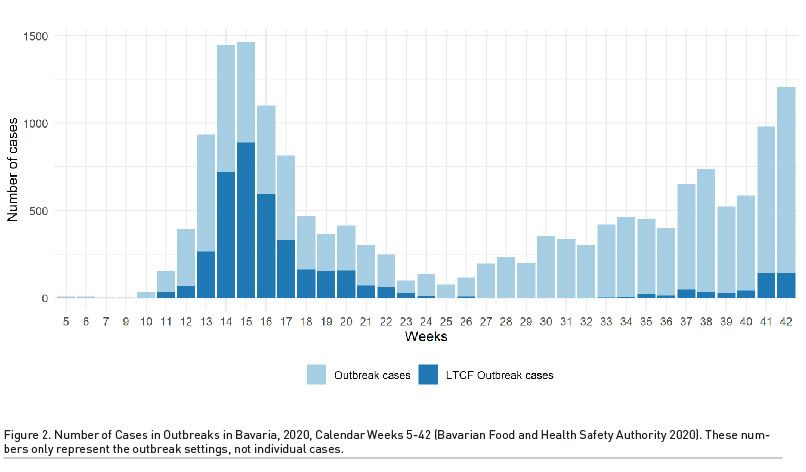
Similarly, many countries developed individual guidelines for their respective health systems, e.g. in Germany, the Robert Koch Institute (RKI) issued the first version of its ‘Notes on prevention and management of COVID-19 diseases in inpatient and outpatient care for the elderly’ on 23 March 2020 (RKI 2020). After the first heavy outbreaks in the UK in April, Ladhani et al. (2020) outlined potential strategies for prevention of COVID-19 in LTC in addition to immediate and wider testing, isolation and quarantine for care home workers to avoid the rapid growth of infections. Comas-Herrera (2020a) and colleagues from the International Long-Term Care Policy Network (LTCCOVID) elaborated on these thoughts and introduced the need for COVID-19 response coordination in care homes, highlighting the fast and unanimous response as crucial.
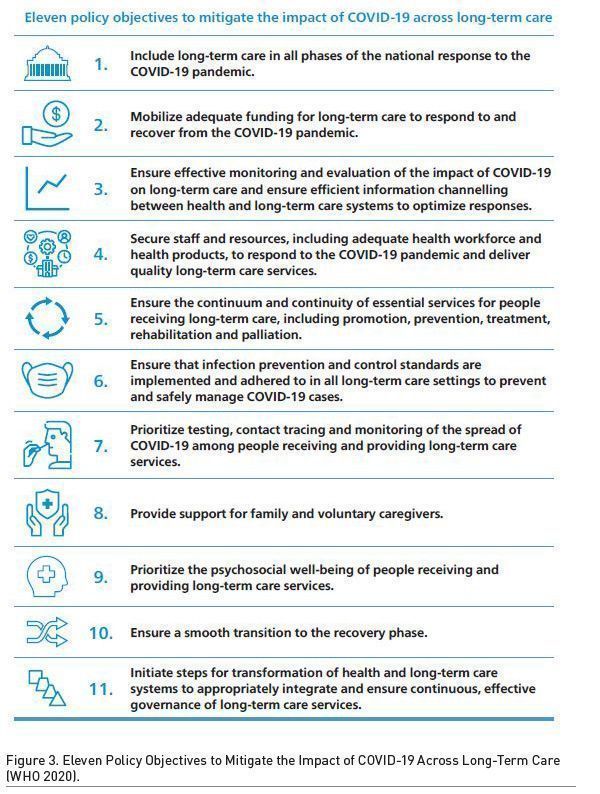
In June, WHO further built on the LTCCOVID work and issued a comprehensive policy paper with 11 policy objectives to mitigate the impact of COVID-19 across LTC, including infectious disease monitoring and prevention but also health governance and health systems resilience (WHO 2020).
Factors of Timely Response; Health Systems Differences
Although the guidance and recommendations are published by multilateral and supranational health bodies such as WHO or ECDC, the implementation of health measures is always the country or even federal state responsibility, therefore the determining factors for a successful intervention are country and federal state specific.
While there are many similarities across different health systems for what to do in terms of protecting the elderly from COVID-19, the WHO policy paper (2020) indicates that there have been significant differences on how to implement the measures most effectively within the necessary timeframe.
At the very least, a proper approach would require a collaborative commitment to prioritise timely and focussed implementation, and then a setup of governance structures and implementation measurements, to ensure that priority focus is met in a timely manner.
In the LTC context, the implementation challenges are very demanding. Care homes operate in a multistakeholder setting that involves multiple sectors, different ministries at different levels, as also pointed out by WHO (2020). These are conditions that usually work against timely intervention. Furthermore, care home residents are especially vulnerable to isolation measures, bearing the risk of social and psychological side effects exacerbated by the constraints of external visits and other isolation measures (Sporket 2020).
The following paragraphs outline the Bavarian approach during the crisis. Bavaria was able to overcome part of the implementation challenges mentioned above by introducing several policy objectives that were also recommended by the WHO and thus focussed on both the what and the how.
Regulation on COVID-19 in Care Homes in Bavaria
Bavarian policies regarding care homes include both stationary care homes for the elderly and care homes for people with disabilities. Bavaria has a population of 126,000 residents and approximately 106,000 personnel in stationary care homes for the elderly. Together with those living and working in care homes for people with disabilities, this adds up to a population of about 150,000 residents and 140,000 personnel (these data exclude the elderly and people with disabilities who are receiving ambulatory care). After the first wave of infections in LTC facilities and with local health authorities overwhelmed by the pandemic burden, the Bavarian government identified a need for special protection of the elderly and disabled people living in LTC facilities. As such, Bavaria opted for a coordinated and concerted approach and set up a governance and implementation structure with a focus on immediate outbreaks and prevention alike, thus overcoming the disparity of decentralised management during the outbreak peak.
Bavaria did so by announcing Katastrophenfall – the ‘State of Emergency’ (SoE) on 16 March 2020 (Bayerische Staatsregierung 2020), which allowed for centralisation of the main executive authority for COVID-19 related matters. On 25 March 2020 the Bavarian Infection Protection Act (BayIFSG) was issued, among others (Bayerische Staatskanzlei 2020), complementing the federal Infection Protection Act (IFSG) with specific regulations and guidelines on LTC facilities. For instance, regulations included a complete prohibition of external visits from March to May 2020 and restricted visits until the end of June 2020 to prevent the virus from entering these facilities. Further measures included compulsory preparation and implementation of extended SARS-CoV-2 specific hygiene measures in every LTC facility, such as introducing basic hygiene measures, keeping distancing measures, setting up pandemic zones, and ensuring wearing of protection gear.
In addition, the regulations set out a clear protocol for dealing with outbreaks, such as on introducing protection measures and on testing, tracing and isolating to curb the outbreaks. The authorities updated these on a regular basis (current version: 7. BaylfSMV), taking into account new information.
Power of Mobile Teams
What makes the Bavarian approach worthy of further examination is its focus on the coordinated implementation of the regulations. After the first reported outbreaks in care homes that involved striking fatalities, the authorities deployed the Bavarian ‘Task Force Care Homes’ to take action against the outbreaks. It was active from 6 April 2020 until 15 September 2020 and consisted of 75 highly qualified staff seconded by the Health Reporting, Epidemiology and Social Medicine unit of the Bavarian Health and Food Safety Authority (15 staff) and the Medical Service of Health Insurance in Bavaria (MDK) (60 staff). The MDK staff in their regular work are responsible for the quality control in LTC, but that was put on hold due to the pandemic. As such, the two organisations agreed to set up this Task Force.
Compared to other parts of Germany, where MDK staff was also supporting local public health authorities, the Bavarian approach stood out due to its centralised nature. One of the reasons for this centralisation was the insufficient number of health personnel at the local public health authorities to deal with the pandemic.
Overall, the professional background of the team included areas such as Public Health, Medicine, Nursing, Care Home Management, Health Management and Prevention.
The mandate of the Task Force was to protect care homes against further outbreaks and COVID-19 related deaths in cooperation with the local health authorities. For this, it offered telephone and email support to care homes and health authorities, but most importantly, this new unit was able to rapidly put together and send mobile teams to help local health authorities effectively manage outbreaks locally.
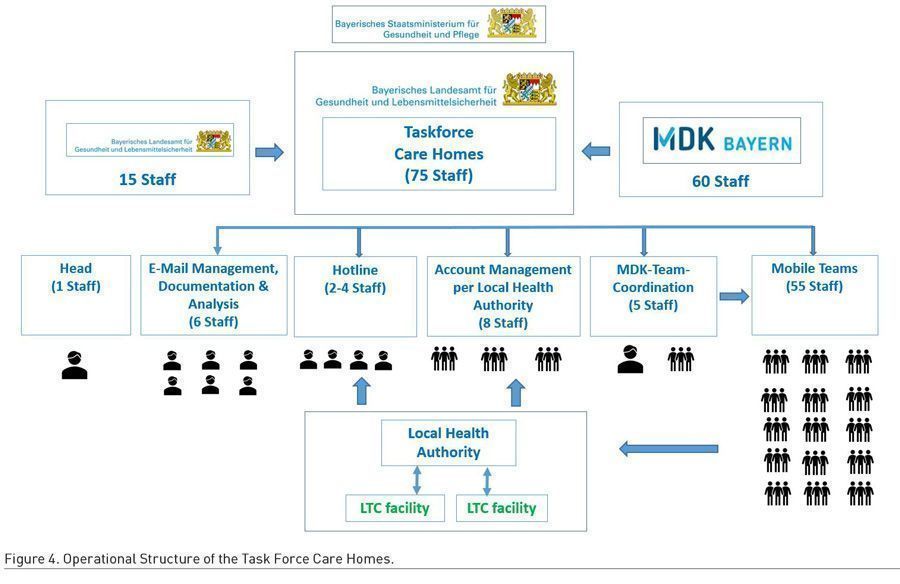
When the Task Force was set up, it compiled a list of 2,199 LTC facilities in Bavaria from different sources. For 1,491 care homes out of this total population, a risk assessment with regards to the severity of SARS CoV-2 outbreaks was conducted, clustering LTC facilities into high-, medium- and low-risk categories. Assessing criteria such as the age of the building or caring for residents with dementia, 759 care homes were considered high-risk, 506 medium-risk and 226 low-risk.
The Task Force offered support to all facilities classified as high- and medium-risk through a telephone survey, but all facilities could also proactively request support.
Based on the risk assessment and the incoming requests, the Task Force supported 1,454 care homes out of 2,199 LTC Facilities (66,1%) within 1,591 missions. Of the 1,591 missions, 561 care homes received telephone consultations, and 634 received an onsite visit only, which included consultations on the proper measures implementation both in relation to an outbreak or as a preventative measure. Residents and personnel of 257 care homes were tested. Within 141 care homes several missions took place.
As the pandemic brought about dynamic needs, the Task Force responded with the following support:
1) SARS-CoV-2 Outbreak Support. In case of an acute outbreak, a mobile team went onsite to support the LTC personnel and local health authorities, making sure tests were conducted in a timely manner and hygiene protocols were introduced accordingly. For this type of support, the Task Force was in touch with 250 care homes that had a SARS-CoV-2 outbreak, and sent a mobile team to 245 care homes for onsite support. As some care homes had quite severe outbreaks, the mobile teams visited those facilities several times to monitor, advise on and adjust hygiene standards, as well as to conduct several follow-up tests on residents and staff.
2) Prevention. As the first wave of the outbreak subsided, the Task Force started offering preventative consulting services to LTC facilities with a high and medium risk score, to increase preparedness in case of a potential outbreak. During this phase, 1,245 care homes were contacted by phone, to prepare them for a potential outbreak. This offer was taken up by 950 care homes that either received telephone consultations or onsite visits.
The main measures taken through the Task Force to deliver support included:
1. Initiating immediate testing of all residents and personnel so that the local health authorities could pursue contract tracing and monitor the spread of COVID-19 within and around LTC facilities.
2. Ensuring the implementation of hygiene and infection control standards according to the RKI and the Bavarian guidelines (i.e. setting up pandemic zones, ensuring protection gear use, etc.).
3. Securing staff and resources in care homes to deliver quality LTC service, even in cases of staff shortages due to infection among personnel.
4. Prevention: (a) from April 2020 onwards, additional focus on preventative phone calls using a standardised protocol; (b) preventative visits to LTC facilities where indicated or requested.
Due to the pandemic dynamic development, the focus of consultations varied over time. At the beginning of the pandemic, in April and May 2020, care homes mainly requested support to implement infection control measures, such as isolation zones, and social distancing measures as well as to train staff and residents to properly use personal protection equipment (PPE). When the lockdown was eased and admissions of new residents, including those who were discharged from hospital, and external visits were allowed again, there was increased demand for consultations on the latest regulations on admissions, visits, etc.
Critical Measures to Mitigate COVID-19 Impact Across LTC
An internal assessment of the Task Force Care Homes highlights the importance of onsite visits, which made the main difference in tackling the pandemic, particularly because of implementing three measures:
- Rapid testing. As the mobile teams were duly qualified and equipped, tests could be conducted rapidly, allowing for proper diagnostics, contact tracing, infection monitoring and breaking the infection chain by local authorities
- Immediate onsite advice and enforcement of infection control measures and hygiene standards to curb further spread
- Supporting preventive measures onsite and strengthening the homes’ preparedness for a potential second wave.
These measures are closely interlinked with the WHO policy objectives that have been identified as key factors to protect the elderly (WHO 2020). Specifically, this case study demonstrates that Bavaria was able to introduce the first seven policy objectives out of eleven. In addition to rapid testing, implementing infection control measures and providing preventative measures, the Task Force provided adequate resources including material; it monitored the risk for the care homes and provided immediate and preventative support. This was complemented by measures taken by the federal authorities, such as including emergency response in the federal regulations, or committing indirect funding to staff running the Task Force.
Although our case study cannot claim a causal relationship, this initial analysis seems to indicate that the outlined principles indeed have an impact on the extent and risks of outbreaks in care homes. It should be noted that Bavaria did not systematically build in Policy 8 (support to families and informal care givers) and Policy 9 (prioritise psychosocial support of people receiving and providing care) within the overall care settings during this immediate response. As Sporket (2020) has indicated, mental health challenges can go along with lockdowns and isolation measures following strict infectious disease management measures.
Concerted Governance and Implementation
Considering the above-mentioned success of delivering relevant policy objectives identified to tackle the COVID-19 pandemic, it is worth exploring the key factors that allowed the rapid setup of such an initiative in such a timely manner in the multi-sectoral LTC setting, which would otherwise have taken much longer to implement. Furthermore, what made it possible to efficiently contain the spread of COVID-19 in care homes?
The analysis of the Bavarian case identifies three relevant factors contributing to the impact of the interventions:(1) SoE as legal precondition, (2) free capacity of specialists, (3) highly effective management operations.
(1) Legal precondition. With the introduction of SoE, Bavaria put in place a legal mechanism that allowed for coordinated cooperation across otherwise independent administrative units such as ministries, local councils and alike, and thus enabled cooperation with MDK that was otherwise not possible. According to this law, “(an) Emergency in the sense...(is) an event in which the life or health of a large number of people or the natural foundations of life or significant property is endangered or damaged to an unusual extent and the danger can only be averted or the disturbance can only be prevented and eliminated if, under the leadership of the Civil Protection Authority, the authorities, services, organisations and forces deployed cooperate” (Bayerische Staatsregierung 2020). This mechanism enabled the authorities to initiate a cooperation between the Bavarian State Ministry of Interior, Sport and Integration and the Bavarian State Ministry of Health and Care in general, and the Bavarian Health and Food Safety Authority and MDK in particular, all to provide priority support to LTC facilities.
(2) Free capacity of specialists. This new unit, the Task Force Care Homes, was comprised of 75 specialists, 60 of them MDK auditors of care homes. Such rapid setup was possible only because of the free capacity of MDK’s highly specialised auditors and the flexibility of the Health Reporting, Epidemiology and Social Medicine unit. The work of MDK in care homes was suspended due to the pandemic so that they could be redeployed for new duties, and they were highly motivated to participate and act quickly within their highly specialised niche. Also, the State Office for Health and Food Safety (LGL) unit reduced or suspended their regular duties while the Task Force was active and could provide management, technical and other medical support.
(3) Highly effective health management operations. The Task Force could only be so effective through the dedication of each contributing individual, as well as through the management structures and operations that were put in place for immediate decision-making and operational excellence that allowed rapid updates. For instance, the Task Force operations included clear responsibilities, holiday covers and key contact points for the local health authorities. Besides, the unit set up clear areas of operations, such as documentation and analysis, mission coordination, mobile team coordination, mobile team missions, and a hotline. These were supported by regular information meetings, an information management system with daily updates, and a process to provide the mobile teams with PPE. Moreover, the Task Force’s mobile teams were organised in such a way that they could react fast and be at a care home the next day the latest, supporting the facility with PPE where needed and helping with implementing relevant hygiene measures.
Future Protection of Vulnerable Groups
The COVID-19 pandemic has once again highlighted that elderly and people with disabilities living in LTC facilities are a vulnerable population in need of protection. Public health services worldwide are in charge of protecting people against infectious diseases including COVID-19. While there is a global understanding on the necessary objectives, the views on their timely implementation vary greatly. This case study exemplified the Bavarian approach to tackle the pandemic, which included creating an interim specialist unit to protect a vulnerable group following a specific protocol. The most important factors to win time in order to interrupt the infection chain were the ability of rapid testing, immediate onsite advice and preventative measures onsite support.
Even though the results are dependent on the German health system structure, they shed some light on how effective measures can help protect the elderly and people with disabilities.
Moving forward, it needs to be emphasised that the Task Force Care Homes was established as an interim solution on the way to more sustainable support for the elderly and people with disabilities living in LTC settings. To ensure transition to more resilient health systems, more systematic research is necessary, such as a comparative analysis of what measures different countries took, what went well and what went wrong.
Future research could look into the situation in care homes, both in Bavaria and in other parts of the country, that did not get this concerted support. Also, more international research and policy action is recommended to ensure both short-term and long-term response to the virus. Specifically, the study recommends focussing on the following three aspects:
1) WHO has recommended to also prioritise the psychosocial well-being of LTC residents and their families. This was not taken into account by the Bavarian authorities in the beginning, however, as it is outlined in the text, first observations indicate that mental health challenges may be caused by lockdowns and isolation measures following strict infectious disease management measures (Sporket 2020). To ensure keeping vulnerable groups mentally healthy, mental health risks have to be better researched to empower policymakers with the right ways to ensure that the elderly are not put under additional psychosocial pressure.
2) One of the reasons for setting up the Task Force Care Homes was the inability of several local health authorities to cope with the massive spread of infection due to staff shortages. To ensure long-term coping capacity of the local authorities, ways have to be explored to strengthen the public health services in the long run, for them to be able to fulfil their duties (Kuhn and Wildner 2020).
3) Similarly, the entire LTC sector has been exposed to this risk because of its many shortcomings (staff shortage, low wages, etc.). As with the public health services, there is a need to explore the care sector pathways, to strengthen the system – if we want to build long-term resilient health systems.
Independent of this research outlook, the future mitigation of the spread of COVID-19 in LTC will depend on the consequent implementation of thorough hygiene concepts on the local level.
Conflict of Interest
None. 
Contributors
Bavarian Health and Food Safety Authority: Johannes Brettner, MPH; Dr Inken Brockow, MPH; Anna Lena Frank, MSc; Alexandra Hachmeister; Marianne Hanauer; Judith Hausmann, BSc; Dr Gabriele Hölscher, MPH; Dr Anja Lüders, MPH; Dr Carola Marzi, MPH; Dr Durdica V. Marosevic; Dr Birgit Odenwald, MPH; Dr Veronika Reisig, MPH; Thomas Schneider.
Medical Service of Health Insurance in Bavaria: Markus Fischer; Dominique Labouvie.
References:
Bayerische Staatskanzlei (2020) Bayerisches Infektions-schutzgesetz (BayIFSG) vom 25. März 2020 [Bavarian Infection Protection Act (BayIfSG) of March 25, 2020] (GVBl. P. 174, BayRS 212-3-G). Available from iii.hm/15pp
7th Bavarian Infection Protection Measures Regulation (7 BayIfSMV), 1 October 2020 (BayMBl. No. 562, BayRS 2126-1-11-G), last amended by Section 1 of the Regulation from 22 October, 2020 (BayMBl. No. 601). Available from iii.hm/15pq
Bayerische Staatsregierung (2020) Bericht aus der Kabinettssitzung vom 17. März 2020 [Report from the cabinet meeting on March 17, 2020]. Published 17 March. Available from iii.hm/15pr
BMSGPK (Hg.) (2020). COVID-19 in Alten- und Pflegeheimen [COVID-19 in elderly care and nursing homes]. Available from iii.hm/15ps
Comas-Herrera A et al. (2020a). International examples of measures to prevent and manage COVID-19 outbreaks in residential care and nursing. Report in LTCcovid.org, International Long-Term Care Policy Network, CPEC-LSE, 11 May 2020. Available from iii.hm/15pt
Comas-Herrera A et al. (2020b), Mortality associated with COVID-19 outbreaks in care homes: early international evidence. LTCcovid.org, last updated 14 October. Available from iii.hm/15pu
European Centre for Disease Prevention and Control (2020) Surveillance of COVID-19 in long-term care facilities in the EU/EEA, 19 May 2020. Stockholm: ECDC. Available from iii.hm/15pv
Kuhn J, Wildner M (2020) Corona-Krise und öffentlicher Gesundheitsdienst [Corona crisis and the Public Health Service]. GGW, 20(4):15-22.
Ladhani SN et al. (2020) Investigation of SARS-CoV-2 outbreaks in six care homes in London. EClinical Medicine (26):1-8.
Landesamt für Gesundheit und Lebensmittelsicherheit (2020) Epidemiologischer SARS-CoV-2 Situationsbericht [Epidemiological SARS-CoV-2 situation report] (internal report).
Robert Koch-Institut (2020) Prävention und Management von COVID-19 in Alten- und Pflegeeinrichtungen und Einrichtungen für Menschen mit Beeinträchtigungen und Behinderungen [Notes on prevention and management of COVID-19 diseases in inpatient and outpatient care for the elderly]. Available from iii.hm/15pw
Sporket M (2020) Befragung zur Situation von Bewohner*innen in Pflegeeinrichtungen im Rahmen der Corona-Pandemie [Survey on the situation of residents in care facilities in the context of the corona pandemic]. Available from iii.hm/15px
WHO (2020) Preventing and managing COVID-19 across long-term care services. Policy Brief, 24 July. Available from iii.hm/15py





