HealthManagement, Volume 21 - Issue 3, 2021
Recent paradigmatic shifts in society as a whole and healthcare in particular demand organisations to change how they approach, devise and implement their management strategies. In this context, people management is one of the priority areas, and a team of experts suggest a management model underpinning the New Health Staff 2030 context.
Key Points
Lately the environment for organisations, particularly in healthcare, has been changing dramatically, especially since the start of the pandemic. Leaders need to focus on adapting to these new volatile circumstances.
- COVID-19 exacerbated the tendencies of the Fourth Industrial Revolution/Health 4.0 in terms of both healthcare context, strategic development, health service management models and people management.
- The Strategic Management of People (SMP 4.0) model brings forward the principles of equity, sustainability, accountability and responsibility through a number of integrated practices.
- With the human dimension at its epicentre, the SMP 4.0 model comprises three structuring vectors, i.e. the structure, the processes and the strategy respectively aligned with the domains of resourcing, developing and engaging.
- For the above, values and organisational structure, communication as well as leadership are the three determinants of success.
- By 2030, efficient people management would mean the alignment of its perspective with the principles of the Super Smart Society.
The context of health service delivery has come under pressure and has been confronted with challenges unthinkable a few years ago. Management models, taken for granted in their processes and results, are now questioned about their suitability, flexibility, adjustment and responsiveness.
Health professionals who are decisive for the effectiveness and excellence of these organisations are now faced with new demands and challenges to which they feel sometimes helpless or unable to respond.
Leaders, from organisations to politicians, are now confronted with other ways of being in society. They are now committed not only to responding to present needs, but above all to the preparation to respond to the challenges that the future may pose.
In line with the theme of this volume, ‘New Health Staff 2030’ a reflection on the most recent changes is important in the context of managing people in health services, main threats and challenges that are identified and the way of endowing these services with excellent professionals prepared for the action in the future.
Heading into Healthcare 4.0
The management of health services has particularities inherent to the characteristics specific to this type of organisation. Oriented towards the provision of preventive, curative and rehabilitation healthcare for patients using advanced technology, there are also places for teaching-learning, research and innovation. They are marked by the high autonomy and degree of technical-scientific specialisation of its multidisciplinary teams. Due to the complexity of its mission and structure, the definition of policies, strategies, people and process management require a deep level of knowledge and professionalisation.
Over the last few years, due to the phenomena of globalisation, the accelerated technological evolution, demographic and environmental changes, and the search for knowledge and its dissemination, among others, have propelled organisations towards strategies for customer/patient focus, resource optimisation, and new models of collaboration, innovation and flexibility. These organisational contexts were until recently called VUCA contexts (volatility, uncertainty, complexity and ambiguity).
Inevitably, also in the organisation of health and health care provision, these effects had an impact. There was a transformation in the way health was understood and a consequent adjustment in the way of guaranteeing it. Technology and evolution of information systems has brought new opportunities to the context of health.
We are facing the emergence of Health 4.0 (Thuemmler and Bai 2017). The act of health provision is largely supported by the evolution that technology provides in terms of automation, big data and even virtualisation. These new processes allow to overcome failures and inefficiencies, optimising human action, streamlining processes and globalising action (for example, digital health). The relationship itself between providers and users undergoes significant changes and is guided by the optimisation of tasks and processes, and increased efficiency and quality of provision of services.
However, if in the last few years it was considered that the management of health services suffered huge pressure arising from the VUCA context and technological advances, now we are faced with even more significant changes.
The COVID-19 pandemic and the associated socioeconomic changes have given rise to contexts sharply marked by frailty, anxiety, non-linearity and incomprehensibility (BANI contexts – Brittle, Anxious, Non-linear, Incomprehensible). The arrival of the current pandemic has shaken the world.
No scenario foresaw this magnitude. Although there are expected changes, the unpredictability of its emergence and its breadth has become an urgent challenge that waits for an answer. It is in this environment marked by instability and adaptability that organisations in general, and health organisations in particular, must achieve answers, sometimes totally new, and anticipate the action for the post-COVID-19.
Leaders must ensure the organisation’s effectiveness at present, while guaranteeing resources and competencies that differentiate them in the future. For this sustainability it is necessary that they promote efficiency and organisational reliability, innovation and adaptation to the external context, always valuing human capital (people) (Yukl 2008).
The COVID-19 pandemic has placed the leadership of organisations in front of complex threats and challenges. It has shown extreme weaknesses, incomprehensible, some of them unimaginable, and generators of ‘fears’. The future is unknown.
It is more and more imperative to keep in mind the importance and the need to prepare real experts for the future.
A Changing World
The changes, associated in 2017 by Schwab (2017) with the Fourth Industrial Revolution, had an impact on health as well. The digital revolution was characterised by a more ubiquitous and mobile internet, artificial intelligence and machine learning, the use of more advanced and sophisticated technologies which are more integrated and allow interaction between the physical, digital and biological domains. This revolution brought about changes not only in the ‘what’ and the ‘how’ we do things, but also in the ‘who we are’. It had systemic impacts and led to global transformations that also impacted health systems, with Health 4.0 considered as a paradigmatic shift and not just a stage of technological development. Schwab announced a “transformation fundamentally in the way in which we live, work and relate”. But he also warned about the need to shape this revolution 4.0 so that it became empowering and more people-centred.
It is, however, in 2020, with the pandemic context that this reflection and also the impact on human dimension becomes more relevant. COVID-19 and its effects brought to the management of health services a sense of relevance and urgency that goes beyond the mere effects of technological evolution. It has become a revolution of thought and action that originates and reinforces a set of changes that should be considered in the future.
In terms of health context, there are two main changes/movements:
i. From the segmentation of sectors and markets to anchored management models, reinforcing the complementarity and interdependence of services and sectors – integrative ‘competition’ movement instead of uncritical competition.
ii. From the user/patient view, in a logic of a sick person with complaints and needs, to the notion of customer/market as a stakeholder with rights, opinion and interests – movement of centring on the individual as an active partner in the health care relationship.
In strategic terms, the most impactful changes for the future of the health services are centred on:
i. Moving the focus from the disease and the sick, to the specificity of each situation and the active, responsible and participating citizen – movement to integrate new technologies, big data and intelligence of things oriented towards the wellbeing and quality of life.
ii. Reinforcement of responses oriented towards virtualisation and anticipation in detriment of the traditional model of proximity and presence – movement of full integration of models supported by the evolution of automation and digitalisation, in addition to their operation in networks and in the cloud.
iii. Alignment between the need for specialised communication but with a focus and a sense of purpose – aiming at the reinforcement of the health services user’s integration as an active partner, with literacy and understanding that allows them to act and choose consciously.
In terms of health service management models, the main challenges exist in the alignment between traditional modes of operation and those that emerge from learning resulting from the pandemic context:
i. Evolution of an integrated management logic that respects options for ‘just in time’ without ignoring the importance of ‘ just in case’ – an anticipatory management perspective that allows to respond in a timely and logically consistent way to potential challenges or threats in the future.
ii. Rethinking the purpose of organisations allowing to align the logic of efficiency, currently prevalent, with the logic of effectiveness in opportunity and response – the challenge of understanding earnings as future bets, often deferred in the form of value to the community.
iii. Betting on strategies focused on viability, but as well integrating the values underlying sustainability – a management model in which the notion of organisational success is anchored in the responsibility and in the creation of a shared value (community/society).
In terms of people management, recent movements allow for the anticipation and the defence of the need for an increased concern with the type and the way the values and competencies are integrated into health organisations.
i. Technical specialisation (specific, acquired and updated knowledge) has to be accompanied by a deep plasticity in its use – a movement of dynamic multidisciplinarity with functional polyvalence in different contexts and with differentiated structures.
ii. Recognition and reinforcement of the complementarity of Power Skills (soft skills, thinking skills and digital skills) as a condition for individual and organisational success in contexts of unforeseen or unknown challenges and threats.
iii. Reinforcement of equity, liability, accountability and sustainability values in a logic of ethical transversality between sectors, contexts and situations.
The trends and challenges set out allow to justify the perspective of Health 4.0 and to anticipate a new future of greater demands and requirements, compatible with a leap in terms of individual responsibility and wellbeing, all underlying a Super Smart Society (Society 5.0).

Managing Future Health Professionals
Regarding this reflection on the preparation/management of the future professionals, a set of questions comes out, for which we will have to find answers. How to attract and retain talent for these organisations? How to manage the quality of the relationship and the quality of work context? How to foster cognitive creativity and flexibility? How to implement complex problem-solving strategies that are customer-oriented, where the customer has become increasingly informed and involved (in terms of higher intervention)? How to promote inclusion, equality and non-discrimination? How to monetise and profit from people, structures and models that would allow the expected results?
To answer these questions, it is fundamental that health service management is anchored in a strong and aligned management of people. We present a model of Strategic Management of People (SMP 4.0)(Duarte et al. 2019) in which the principles of equity, sustainability, accountability and responsibility dominate through a set of integrated practices of:
- Strengthening investment in skills development (lifelong learning) by the use of new models of knowledge sharing and development. Models based on the reinforcement of collaborative and multidisciplinary networks and on heutagogic strategies, where the protagonism is on the learners.
- Diminishing the importance of educational models for training/employment resulting from the traditional STEAM approaches (Sciences, Technology, Engineering, Arts and Mathematics). And making such models transversal and integrated in a World Web Learning logic (WWL).
- Adding to the competencies 4.0 (technical, social and personal skills) the domains of Design Thinking and Critical Thinking, which are more oriented towards the development of Power Skills (soft skills, thinking skills and digital skills).
- Giving more weight and value to the ‘mixed workforce’ – people and robots/technology working together: workers always connected, in multiple contexts in an anytime, anywhere model.
- Expanding artificial intelligence (AI) to HR processes (recruitment, remunerations, etc.).
- Using and promoting AI in a conscious, ethical and responsible way.
- Promoting a culture of safety and high performance.
- Making an employee’s experience and happiness a top priority, and creating sustainable environments (quality of life and wellbeing, diversity, inclusion and collaborative networks).
- Offering both organisations and people a sense of purpose added to their work/function, while taking into account the social/environmental/family and organisational factors.
- Understanding and welcoming the ‘Digital Protean Worker’ (highly qualified, with high digital and soft skills, with an interest for geographic and organisational mobility, and mobilised by values of achievement and social commitment).
SPM 4.0: A Model for Strategic Management of People
To respond to the identified challenges in health services, the Strategic People Management Model integrates the main changes and concerns presented, and also constitutes a guiding framework for action in the future.
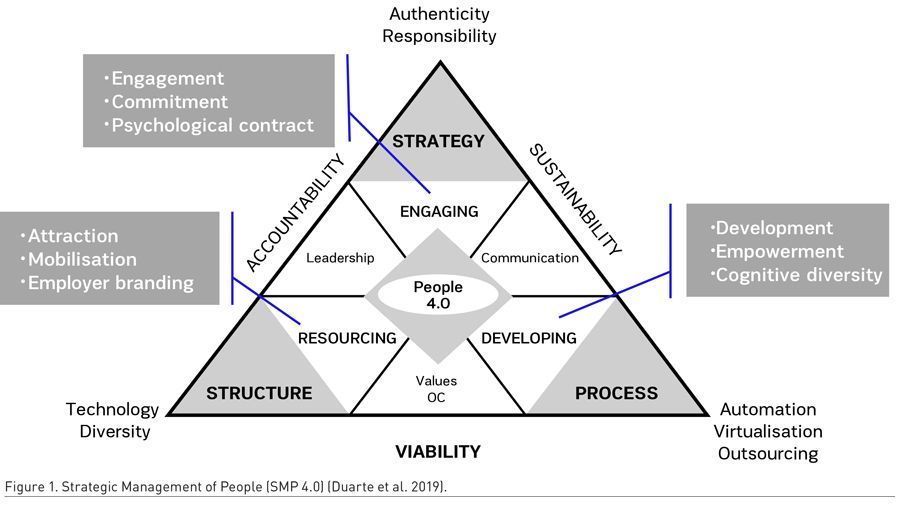
The model (Figure 1) is synergistically articulated around three structuring vectors, having as its epicentre the human dimension (people and their experiences). The structuring vectors are:
i. The structure is understood as the organisational design and results from the identification, analysis, ordering and grouping of the activities and resources of the organisations. It contains all the essential resources for being functional (material, relational, capital, informational, etc.), and their interactions. The structure should be agile and flexible enough to be able to respond to rapid and uncertain changes. It should also increment new collaborative models and partnerships with the stakeholders (internal and external) developed in a logic of responsibility and confidence, enhancing organisational results and predictability of the action.
ii. The processes include the set of activities, methods and routines specific to health organisations, which are aiming at maximising the value in health and wellbeing.
iii. The strategy is defined as the mediating force between organisations and their environment, characterised by a pattern or a plan that integrates the main goals, policies and tactics of an organisation for the pursuit of its objectives and goals. Anchored in a vision of the future, it allows the allocation of resources (structure) and the assimilation of processes that guarantee in advance a differentiation in the face of contextual premises. It is the strategy that ensures viability and sustainability conditions of the organisation.
In articulation with the three structuring vectors of organisations, there are three key domains of people management that deserve to be highlighted. These three areas are:
i. Resourcing – aligned with the Structure vector, its purpose is planning and prospecting, and the attraction, identification and selection of talents that are essential to the provision of health services. It supports employer branding dimensions, recruitment and selection, and management of talent mobility.
ii. Developing – aligned with the Processes vector, it aims at the development and empowerment of people and the creation and diffusion of knowledge. The characteristics of this new digital-knowledge workers demand a paradigm of continuous learning and reinforcement of life experience. The acquisition and dissemination of knowledge, the management and evaluation of performance all have requirements for personalisation and sharing, and come with expectations of a quick and permanent feedback. It should have a purpose of improvement, recognition and motivation and provide an attractive experience. It is no longer enough for people management to incorporate technologies to facilitate managerial process and traditional administrative procedures. A new form of self-regulation of learning and assessment, which is personalised and self-managed, encourages taking advantage of opportunities arising from social, mobile and cloud technologies, and the virtualisation of numerous processes and procedures.
iii. Engaging – aligned with the Strategy vector, this domain has the purpose of fostering and managing workers’ commitment to the organisations. Committed workers not only contribute more strongly to the organisational success but also manage to benefit from and make use of, more effectively, their capacities and competencies and abilities. It is important that People Management 4.0 takes into account the drivers of organisational engagement and integrates them into its policies. The importance of meaningful work, the opportunity to participate and develop rewarding relationships, and the emergence of inclusive policies, associated with a culture of trust and empowerment, will have to be allied with remuneration policies and attractive careers.
To guarantee the alignment between the structuring vectors (structure, processes and strategy) and the key domains of intervention of people management (Resourcing, Developing and Engaging), it is important to consider the three determinants of success:
i. Values and organisational culture – mediating the structure and the processes, it is characterised by two distinct and inseparable perspectives: the individual and the organisational. Regarding individual terms, it is important to put the emphasis on ethical concerns and societal commitment (social and environmental), all consolidated in patterns and standards of autonomy, responsibility and development. The sharing of these values fosters, in organisations, new ways of being. The organisations, in their turn, integrate these values and develop cultures of flexibility, inclusion and innovation, all anchored in principles of trust and commitment. This combination results in what is the ultimate motive of the organisation and its contribution to society – the sustainability.
ii. Communication – determined by strategy and processes, it assumes and takes on a determinant role in people management and in the success and consolidation of the organisation’s identity. Thus, concern and increased care for internal communication (both formal and informal), as well as for external communication, becomes essential and extremely important.
iii. Leadership – it is a hinge between the strategy and the structure. Leadership has to derive and assimilate change towards the development of strategies that encourage innovation and active learning across the organisation, with the focus on people’s engagement. This challenge calls for new leadership competencies and skills that are structured in relational terms (e.g. development of a culture of trust, authentic communication, promotion of individual and team development, and ensuring the inclusion of individual interests and values). Regarding technical terms, leadership must be able to challenge the status quo and promote creativity and innovation, as well as develop benchmarking and networking initiatives that ensure the updating and the ability of responsiveness, in a context that is permanently and rapidly changing. The 21st century leader will assert themselves by their adaptive and disruptive practices, by their integration of values and implementation of growth strategies and also by value creation for society.
In Summary
With the challenge of managing people in 2030, we believe that the core will be effectively in a perspective aligned with the vision of Society 5.0 (Super Smart Society). A society with solid values of equity, responsibility, accountability and sustainability. A society in which it will be fundamental to (re)think and (re)position the technologies to improve humanity’s quality of life.
Based on the learning resulting from the management of people in the turbulent context of the COVID-19 pandemic, we believe that, more than ever, human and social capital will be the determinant of organisational success, and a competitive advantage for organisations, in general, and for health, in particular.
We must guarantee a society of values, in which technologies are not an end in themselves but rather a means for a better life.
We need the world to remain Human and health professionals who assure that!
Conflict of Interest
No conflict of interest declared. 
References:
Duarte A et al. (2019) Gestão de pessoas 4.0 [People management 4.0]. In Machado C, Davim JP (Eds.), Organização e Políticas Empresariais [Business Organization and Policies] (1st ed., pp. 15–53). Lisbon: Actual Editora.
Schwab K (2017) The Fourth Industrial Revolution. London, England: Portfolio Penguin.
Thuemmler C, Bai C (Eds.) (2017) Health 4.0: How Virtualization and Big Data are Revolutionizing Healthcare. New York, NY: Springer Publishing.
Yukl G (2008) How leaders influence organizational effectiveness. The Leadership Quarterly, 19(6):708-722.




