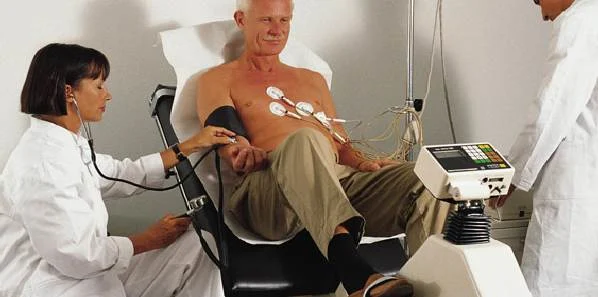
The American College of Physicians has issued new guidance stating that adults without symptoms and who are at low risk of developing coronary artery disease should not be screened for heart disease with resting or stress electrocardiography, stress echocardiography, or stress myocardial perfusion imaging.1
“Cardiac screening in adults at low risk for coronary heart disease is low value care because it does not improve patient outcomes and it can lead to potential harms,” ACP President David Fleming said in a statement released with the guidelines. “Physicians should instead focus on strategies for improving cardiovascular health by treating modifiable risk factors such as smoking, diabetes, hypertension, high cholesterol, and obesity and encouraging healthy levels of exercise.”
Based on the guidance, asymptomatic, low risk patients are those who are determined to have a 10-year risk of coronary heart disease events of less than 10 percent, estimated from published risk calculators such as the Framingham risk score. To establish risk, these calculators take into account such factors as age, sex, hypertension, low HDL cholesterol concentration, family history of premature coronary heart disease, and history of smoking.
The evidence for the new guidelines came from several sources, including a systematic review,2 the recommendations of the US Preventive Services Task Force,3 several guidelines developed by the American College of Cardiology in partnership with other organisations, and articles on the benefits and harms of cardiac screening. “A search for primary care, cardiology, or radiology guidelines that recommend cardiac screening in low risk adults found none,” the article noted.
One reason that cardiac screening in low risk patients might be ineffective was that there was no proved, effective treatment for many of the abnormalities found, such as left ventricular hypertrophy, asymptomatic bundle branch block, or non-specific depolarisation abnormalities, according to the report. “Conversely, interventions for modifiable CHD [coronary heart disease] risk factors, such as smoking, hypertension, diabetes, and overweight, are generally indicated regardless of cardiac screening test findings,” the report said.
The risks of screening included those inherent in testing, such as complications as the result of exercise electrocardiography or the use of drugs used to induce stress and, in the case of myocardial perfusion imaging, radiation exposure, and in the interventions that might follow, the report said. Angiography, for example, is associated with a risk of about 1.7 percent of serious adverse events, including death, myocardial infarction, stroke, and arrhythmia, the report noted.
False positive test results were also common in low risk groups, the report warned, noting that up to 75 percent of asymptomatic men with exercise induced ST segment depression on electrocardiography will prove to have no significant angiographic coronary artery disease.
“In patients in the low-risk category, cardiac screening is not indicated. Rather, strategies should focus on treating modifiable risk factors (such as smoking, diabetes, hypertension, hyperlipidaemia, and overweight) and encouraging healthy levels of exercise,” the report concluded.
References
1. Chou R; High Value Care Task Force of the American College of Physicians. Cardiac screening with electrocardiography, stress echocardiography, or myocardial perfusion imaging: advice for high-value care from the American College of Physicians. Ann Intern Med 2015;162:438-47.
2. Chou R, Arora B, Dana T, Fu R, Walker M, Humphrey L. Screening asymptomatic adults with resting or exercise electrocardiography: a review of the evidence for the US Preventive Services Task Force. Ann Intern Med 2011;155:375-85.
3. Moyer VA; US Preventive Services Task Force. Screening for coronary heart disease with electrocardiography: US Preventive Services Task Force recommendation statement. Ann Intern Med 2012;157:512-8.
Source: BMJ 2015;350:h1607
Image Credit: Illinois Department of Public Health
“Cardiac screening in adults at low risk for coronary heart disease is low value care because it does not improve patient outcomes and it can lead to potential harms,” ACP President David Fleming said in a statement released with the guidelines. “Physicians should instead focus on strategies for improving cardiovascular health by treating modifiable risk factors such as smoking, diabetes, hypertension, high cholesterol, and obesity and encouraging healthy levels of exercise.”
Based on the guidance, asymptomatic, low risk patients are those who are determined to have a 10-year risk of coronary heart disease events of less than 10 percent, estimated from published risk calculators such as the Framingham risk score. To establish risk, these calculators take into account such factors as age, sex, hypertension, low HDL cholesterol concentration, family history of premature coronary heart disease, and history of smoking.
The evidence for the new guidelines came from several sources, including a systematic review,2 the recommendations of the US Preventive Services Task Force,3 several guidelines developed by the American College of Cardiology in partnership with other organisations, and articles on the benefits and harms of cardiac screening. “A search for primary care, cardiology, or radiology guidelines that recommend cardiac screening in low risk adults found none,” the article noted.
One reason that cardiac screening in low risk patients might be ineffective was that there was no proved, effective treatment for many of the abnormalities found, such as left ventricular hypertrophy, asymptomatic bundle branch block, or non-specific depolarisation abnormalities, according to the report. “Conversely, interventions for modifiable CHD [coronary heart disease] risk factors, such as smoking, hypertension, diabetes, and overweight, are generally indicated regardless of cardiac screening test findings,” the report said.
The risks of screening included those inherent in testing, such as complications as the result of exercise electrocardiography or the use of drugs used to induce stress and, in the case of myocardial perfusion imaging, radiation exposure, and in the interventions that might follow, the report said. Angiography, for example, is associated with a risk of about 1.7 percent of serious adverse events, including death, myocardial infarction, stroke, and arrhythmia, the report noted.
False positive test results were also common in low risk groups, the report warned, noting that up to 75 percent of asymptomatic men with exercise induced ST segment depression on electrocardiography will prove to have no significant angiographic coronary artery disease.
“In patients in the low-risk category, cardiac screening is not indicated. Rather, strategies should focus on treating modifiable risk factors (such as smoking, diabetes, hypertension, hyperlipidaemia, and overweight) and encouraging healthy levels of exercise,” the report concluded.
References
1. Chou R; High Value Care Task Force of the American College of Physicians. Cardiac screening with electrocardiography, stress echocardiography, or myocardial perfusion imaging: advice for high-value care from the American College of Physicians. Ann Intern Med 2015;162:438-47.
2. Chou R, Arora B, Dana T, Fu R, Walker M, Humphrey L. Screening asymptomatic adults with resting or exercise electrocardiography: a review of the evidence for the US Preventive Services Task Force. Ann Intern Med 2011;155:375-85.
3. Moyer VA; US Preventive Services Task Force. Screening for coronary heart disease with electrocardiography: US Preventive Services Task Force recommendation statement. Ann Intern Med 2012;157:512-8.
Source: BMJ 2015;350:h1607
Image Credit: Illinois Department of Public Health
Latest Articles
echocardiography, coronary artery disease, asymptomatic CAD, American College of Physicians, cardiac screening, electrocardiography
The American College of Physicians has issued new guidance stating that adults without symptoms and who are at low risk of developing coronary artery disea...