“Cardiovascular diseases (CVDs) affect mainly the elderly, but for many years an increase in incidence has been observed in young people as well, regardless of gender,” said Professor Hanna Szwed, last author and head of the 2nd Department of Coronary Artery Disease, Institute of Cardiology in Warsaw, Poland. “The World Health Organization estimates that CVDs cause more than 52% of all deaths in women and the number continues to rise. Up to 1% of all heart attacks are in young women.”
This study in 7 386 women assessed the effect of risk factors on MI incidence in young women and assessed differences related to age. The epidemiological profile of 1 941 young women (aged ≤45 years) with MI was retrospectively compared with two control groups: 4 275 women aged 63-64 years with MI and 1 170 healthy women (no MI history) aged ≤45 years.
The study used data from three national registries. Data on women with MI came from the Polish Registry of Acute Coronary Syndromes (PL-ACS).2 Information on healthy women was from the Multicentre Study of State National Population Health (WOBASZ)3 and National Survey of Risk Factors for Cardiovascular Diseases (NATPOL).4
The average age among young MI patients in the study was 42 years (range 21-45 years). Multivariate analysis showed that four out of five classic risk factors were independent predictors of MI in young women. The strongest was diabetes which increased MI risk by six-fold. Arterial hypertension increased risk by four times while hypercholesterolemia tripled risk and current smoking increased risk by 1.6 times. There was no statistical significance for obesity expressed by body mass index (BMI).5
Professor Szwed said: “The lack of a correlation with obesity could be because of the overwhelming influence of diabetes in this population. We also found that the risk of MI in young women increased with the number of coexisting factors (Figure 1).”
The researchers found that young healthy women had an average of 1.1 risk factors, while young MI patients had 1.7 and older women with MI had 2.0. Compared to young healthy women, young women with MI more often had arterial hypertension, hypercholesterolemia and diabetes and were current or past smokers (Figure 2).6
In the population of older women with MI, the prevalence of nearly all individual risk factors was even greater than in young women with MI.7 Smoking was the only risk factor with a greater prevalence in the younger group (48.7% vs.22.2% p<0.0001 forcurrentsmoking, and 65.5% vs.45.1% p<0.0001 for pastsmoking) (Figure 2). “We found that therisk factor profile in young women with MI was similar to the older population apart from the greater occurrence of tobacco smoking in young women,” said Professor Szwed.“This finding correlates with other research which shows that smoking is a growing problem in young women.This is clearly an area where prevention efforts are needed.” Interestingly, youngwomenwith MI were morelikely thanolder women to have none of the above-mentionedrisk factors(16.5%vs.8.2% p <0.0001).The most frequent risk factor inthis subgroupof patients(bothfor youngerand older women)wasa familyhistoryof coronary artery disease,with a higher rate in younger compared to older women (11.9%vs5.5% p=0.0035).
Professor Szwed concluded: “At present there are not enough global scientific reports focused on the problem of coronary heart disease in young populations, particularly in women. More research is needed into this growing problem to deepen our knowledge, improve prevention efforts and reduce mortality.”
Figure 1: Relationship between average number of risk factors and rate of heart attacks in young women according to age
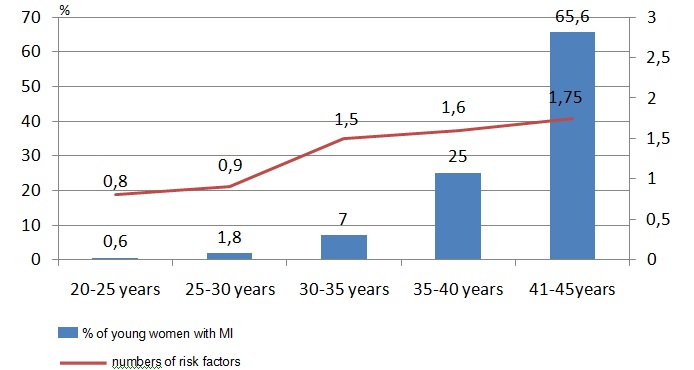
Figure 2: Prevalence of risk factors by age and history of myocardial infarction
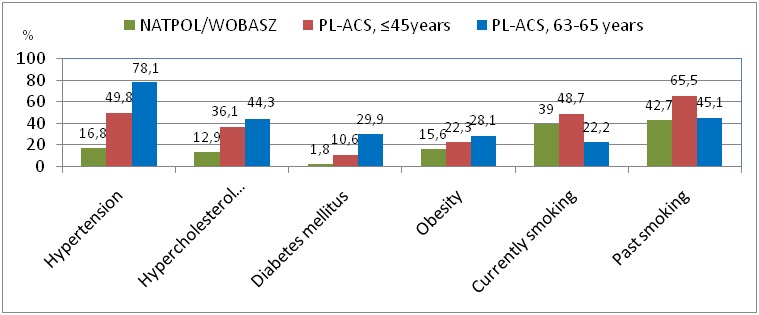
NATPOL/WOBASZ: healthy women aged <45 years; PL-ACS: women with history of MI
Source: ESC
Image Credit: Wikimedia Commons










