Heart failure is a common disorder affecting millions of people globally. Over the past three decades, the prevalence of heart failurehas been increasing primarily because of the advancing age of the population and advances in medicine, which is allowing patients with hypertension, myocardial infarction, end-stage renal disease, and diabetes to live longer and eventually develop heart failure.
The management of heart failure is complex and involves changes in lifestyle, medical treatment, an evaluation of genetic factors and sometimes the use of medical devices. In the last few years, many new drugs have been developed that not only reduce symptoms of heart failure but also prolong survival. For patients who do not respond to traditional drug therapies, there are several types of vascular and electrical interventions that can be combined with drug therapy to reduce morbidity and mortality. The management of heart failure has become so complex that there are cardiologists who specialise in the management of just this one cardiac disorder and need to continually stay up to date to get the best outcomes.
You might also like: Top Heart Disease, Stroke Research Advances in 2019
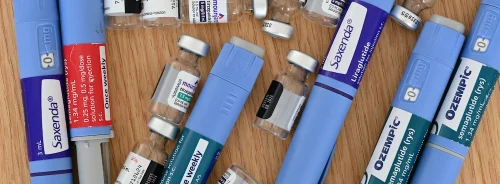
At the latest heart failure conference in Lebanon that was attended by the leading experts in the world, all landmark trials involving drug therapy starting with the angiotensin-converting enzyme inhibitors, angiotensin receptor blockers, beta-blockers, aldosterone antagonists and angiotensin receptor neprilysin inhibitor (sacubitril/valsartan) were reviewed. In addition, the outcomes from the most recent DAPA-HF trial were also discussed. Experts predict that these agents (inhibitors of sodium-glucose cotransporters 2) will play a vital role in the management of heart failure in the near future.
The heart failure meeting also focused on non-invasive structural interventions that may improve survival and outcomes in patients with heart failure. Results from the COAPT study regarding the evidence supporting the use of transcatheter mitral valve repair were also discussed. Currently, the transcatheter mitral valve repair is sometimes used to manage patients with heart failure and in patients with primary/secondary mitral regurgitation. Experts discussed the designs and outcomes between the COAPT and MITRA-FR3 studies and identified criteria for selecting patients for these therapies.
Dr. Nassir Marrouche from Tulane University also reviewed the new findings from the CASTLE AF trial which proved for the first time that catheter-based ablation of atrial fibrillation can improve survival in patients with heart failure. The meeting also reviewed devices used to manage heart failure like resynchronisation therapy and the use of defibrillators.
There was also a review of assist devices for the management of patients with heart failure. All experts agreed that they would not like to see their patients reach this stage but unfortunately when everything else fails, use of assistive devices is the last option. The overall conclusion was that assist devices can improve the quality of life or they can be used as a bridge to transplant.
Source: European Heart Journal
Image Credit: iStock
References:
Azar R, Abdelmassih T (2020) Innovation in Heart Failure: from Pills to Devices: Report from the second annual meeting of the Division of Cardiology of Hotel Dieu de France, Beirut, Lebanon on 6–7 September 2019. European Heart Journal, 41(8):906-907.
Latest Articles
heart failure
An overview of major innovations in heart failure presented at a recent cardiology meeting in Beirut, Lebanon.