According to a new observational study, the use of fractional flow reserve (FFR) or intravascular ultrasound (IVUS) during PCI does not improve long-term mortality when compared with standard angiography-guided PCI.
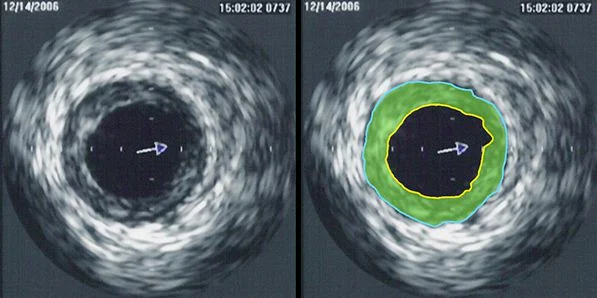
The study findings are based on the analysis of 41,688 patients that were included in the Pan-London (UK) PCI Registry with stable angina and non-ST-segment-elevation MI (NSTEMI). 2,767 patients underwent FFR-guided PCI and IVUS was used in 1,831 patients. Results showed that the FFR-guided mortality rate after 3.3 years was not significantly different from angiography-guided PCI. IVUS-guided PCI also did not demonstrate a mortality benefit when compared with angiography-guided PCI.
Patients in the FFR group received fewer implanted stents as compared to those in the IVUS and conventional PCI group. Thus, while findings indicate that FFR guided PCI may have a stent-sparing effect, no significant mortality benefit was derived.
The findings have been published in the Journal of American Medical Association: Internal Medicine. Dr. Georg Frohlich of University College London Hospital, UK says, "It is perhaps too optimistic to expect a survival advantage from the use of a purely diagnostic procedure."
Dr. Sanjit Jolly of McMaster University, Hamilton ON has echoed the sentiment that there is no real benefit that can derived from FFR-guided procedures and that it does not offer any survival advantage over conventional angiographic PCI.
During the St. Jude Medical sponsored FAME II Trial, the FFR approach did not show a survival benefit. FAME showed the benefit of FFR on the primary end point of major adverse cardiovascular events.
The American Heart Association (AHA) recommends the use of FFR in patients with stable angina only if the coronary lesion is considered of intermediate severity. AHA also recommends the use of IVUS to assess intermediate lesions in the left main artery.
While the findings are similar to those observed in the FAME studies, Dr. Aseem Malhotra from Croydon University Hospital, London, UK, highlights that this new study provides additional real-world information about the use of FFR and IVUS and can help avoid the unnecessary use of diagnostic modalities and the overtreatment of certain lesions. According to Malhotra, even lesions that appear to be more than 80 percent stenosed might not be functionally significant.
Over-diagnosis and overtreatment contributes to an increase in the overall healthcare costs of a nation. Having this knowledge that coronary stenting in patients with stable angina does not lead to better clinical outcomes can hopefully reduce the overenthusiastic use of new technologies that show no superior benefit.
These techniques are better used in patients who have a larger burden of ischemia or limiting angina despite the use of optimal medical therapy. Accurate selection of the right patients can help reduce healthcare costs as well as better clinical outcomes overall.
Source: Medscape
Image credit: Wikimedia Commons
The study findings are based on the analysis of 41,688 patients that were included in the Pan-London (UK) PCI Registry with stable angina and non-ST-segment-elevation MI (NSTEMI). 2,767 patients underwent FFR-guided PCI and IVUS was used in 1,831 patients. Results showed that the FFR-guided mortality rate after 3.3 years was not significantly different from angiography-guided PCI. IVUS-guided PCI also did not demonstrate a mortality benefit when compared with angiography-guided PCI.
Patients in the FFR group received fewer implanted stents as compared to those in the IVUS and conventional PCI group. Thus, while findings indicate that FFR guided PCI may have a stent-sparing effect, no significant mortality benefit was derived.
The findings have been published in the Journal of American Medical Association: Internal Medicine. Dr. Georg Frohlich of University College London Hospital, UK says, "It is perhaps too optimistic to expect a survival advantage from the use of a purely diagnostic procedure."
Dr. Sanjit Jolly of McMaster University, Hamilton ON has echoed the sentiment that there is no real benefit that can derived from FFR-guided procedures and that it does not offer any survival advantage over conventional angiographic PCI.
During the St. Jude Medical sponsored FAME II Trial, the FFR approach did not show a survival benefit. FAME showed the benefit of FFR on the primary end point of major adverse cardiovascular events.
The American Heart Association (AHA) recommends the use of FFR in patients with stable angina only if the coronary lesion is considered of intermediate severity. AHA also recommends the use of IVUS to assess intermediate lesions in the left main artery.
While the findings are similar to those observed in the FAME studies, Dr. Aseem Malhotra from Croydon University Hospital, London, UK, highlights that this new study provides additional real-world information about the use of FFR and IVUS and can help avoid the unnecessary use of diagnostic modalities and the overtreatment of certain lesions. According to Malhotra, even lesions that appear to be more than 80 percent stenosed might not be functionally significant.
Over-diagnosis and overtreatment contributes to an increase in the overall healthcare costs of a nation. Having this knowledge that coronary stenting in patients with stable angina does not lead to better clinical outcomes can hopefully reduce the overenthusiastic use of new technologies that show no superior benefit.
These techniques are better used in patients who have a larger burden of ischemia or limiting angina despite the use of optimal medical therapy. Accurate selection of the right patients can help reduce healthcare costs as well as better clinical outcomes overall.
Source: Medscape
Image credit: Wikimedia Commons
Latest Articles
PCI, Cardiac, Angiography, AHA, angina, FFR, IVUS
According to a new observational study, the use of fractional flow reserve (FFR) or intravascular ultrasound (IVUS) during PCI does not improve long-term m...