A letter by UCSF researchers published in JAMA Internal Medicine provides evidence that a quarter of all atrial fibrillation (AF) patients at the lowest risk for stroke receive unnecessary blood thinners from cardiology specialists.
According to senior author Gregory Marcus, MD, MAS, director of clinical research in the UCSF Division of Cardiology, there is a push to get providers to prescribe these drugs but these drugs end up being under-prescribed among those who actually need them. The study by these researchers suggests that people are trying to do the right thing but because there is a lack of understanding of some critical nuances, they end up prescribing these drugs unnecessarily to low-risk patients.
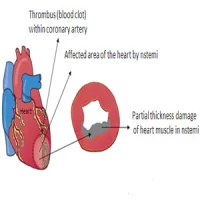
AF patients who are at risk for thromboembolism are prescribed anticoagulation therapies with warfarin or other drugs in order to reduce morbidity and mortality. However, since the use of these drugs carries a bleeding risk, they are not recommended for patients at low risk for stroke. Current guidelines do not recommend the use of oral anticoagulation therapies in patients under the age of 60 without heart disease or other known risk factors for thromboembolism or in AF patients without any proven risk factor for stroke.
Marcus and his colleagues reviewed 11,000 patients nationwide age 60 and under. They examined the prevalence of non-guideline adhering oral anticoagulant prescription in young and healthy patients at the lowest risk of thromboembolism.
The findings show that approximately 25 percent of patients were prescribed oral anticoagulant therapy contrary to guidelines. They also found that males with AF at the lowest risk of stroke were more likely to be prescribed these drugs as compared to females. The same was true for older and overweight patients without stroke risk factors.
"Practitioners who prescribe blood thinners need to be diligent about weighing the risks and benefits of these medications," said lead author Jonathan C. Hsu, MD, MAS, of the UC San Diego Division of Cardiology and recent UCSF cardiology and electrophysiology graduate. "In those patients with no risk factors for stroke, the risk of bleeding likely outweighs the benefit of stroke reduction. The fact that blood thinners were prescribed to so many patients with no risk factors for stroke is a wake-up call that we need to do better for our patients."
Source: University of California - San Francisco
Image Credit: Wikimedia Commons
References:
Marcus, Gregory. (2015). Oral Anticoagulant Prescription in Patients with Atrial Fibrillation and a Low Risk of Thromboembolism: Insights from the NCDR PINNACLE Registry. JAMA Internal Medicine. DOI:10.1001/jamainternmed.2015.0920