The current pandemic has led to increased use of telemedicine, allowing delivery of care with no person-to-person contact, in line with physical distancing measures to prevent further spread of coronavirus.
You might also like:Bright Ideas
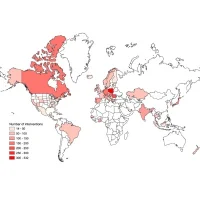
A new survey study (Scott et al. 2020) zeroed in on telemedicine use among people living with type 1 diabetes, whose access to their healthcare providers or critical medical supplies (e.g. insulin) might have been restricted by the pandemic. Of 7,477 respondents from 89 countries, 30% reported that the pandemic actually had forced cancellation of appointments with their doctors.
As regards use of telehealth services, 28% of respondents reported receiving remote care primarily through telephone (72%), followed by video consultation (28%). Notably, these virtual appointments/visits were considered to be "useful" by the majority (86%) of those who received remote care, and 75% plan to have remote appointments beyond the pandemic.
The study made use of an anonymous questionnaire distributed via social media – Facebook, Twitter and Instagram – between 24 March and 5 May 2020. The online survey covered questions relating to the use and perception of telemedicine, diabetes treatment and control, and medical supply during the pandemic.
Other key findings of the survey study are:
- 32% of respondents reported no fundamental change in their medical follow‐up, with 9% stating that no personal contact was made with their doctors over the duration of the study.
- Glucose control, indicated by HbA1c, was positively associated with positive perception of telemedicine.
- In males, 45% of respondents with an HbA1c > 9% rated telemedicine not useful compared to those with lower HbA1c, while among females this proportion stood at 20%.
The results of this worldwide survey show that a large percentage of respondents with type 1 diabetes either have had or plan to have remote/virtual consultations in view of the COVID-19 pandemic.
Type 1 diabetes may be particularly well suited to telemedicine since consultations are mostly based around a review of glucose data and discussions about therapy, according to study authors.
Furthermore, the increasing use of continuous glucose monitoring (CGM), insulin pumps and smart insulin pens, alongside cloud/screen-based data sharing and greater access to webcams, lends support towards greater use of telemedicine – allowing both the patient and provider to view the data without being together physically.
"Interestingly, age and level of education do not appear to influence peoples’ perceptions of telemedicine so far, whereas poor glucose control seems to negatively affect the perception on usefulness of telemedicine, particularly in males," the authors wrote. "Beyond the pandemic, telemedicine may offer an alternative means to improve efficiency and cost effectiveness of care for people with diabetes."
Aside from cost and time savings, remote care can be beneficial for people living far from their healthcare providers or those with mobility issues that make in-person visits difficult.
Source: Wiley
Image credit: AndreyPopov
via iStock