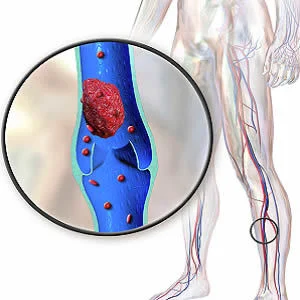
Although pulmonary CT angiography (CTA) is increasingly used to evaluate patients believed to suffer from pulmonary embolism (PE), the diagnostic yield remains low, according to a review published in American Journal of Roentgenology. The finding suggests a potential benefit to the use of clinical decision tools in the diagnostic work-up of suspected PE patients.
“Validated clinical decision rules and integrated clinical decision support (CDS) systems can influence the appropriate use of pulmonary CTA, but further investigation is required to define the most successful means of integration into clinical practice,” said the study's co-author Dr. Jadranka Stojanovska, from University of Michigan Health Systems, Ann Arbor.
PE is a frequently suspected diagnosis, especially in patients appearing in emergency departments with cardiopulmonary symptoms. The study suggests that CTA is overused as a screening rather than a diagnostic examination, which increases financial costs and medical consequences from radiation exposure and the use of contrast media.
Unfortunately, the moderate impact of CDS on pulmonary CTA use and yield is related to physician nonadherence, according to researchers. Factors hindering successful implementation of CDS systems include:
- Electronic clinical decision rules or support systems are cumbersome and require added input by the ordering clinician.
- Physician's distrust of standardised rules, fear of legal retribution if a morbid or fatal PE is missed, and unfamiliarity with radiation exposure and iodinated contrast risks.
Patient input also factors into nonadherence, the researchers note, as some patients with particular symptoms may request CT for evaluation. Clinicians may assume that in the absence of PE an alternative diagnosis will be established with pulmonary CTA, despite evidence that different etiologic factors are supported in only one-third of cases.
A one-time or limited educational intervention is not as likely to help overcome these obstacles as repetitive educational efforts up to five years, according to the study.
Dr. William M. Sherk, also from University of Michigan Health Systems, Ann Arbor, is co-author of the study.
Source: American Roentgen Ray Society (ARRS)
Image Credit:
References:
Latest Articles
CT angiography, Pulmonary embolism, Clinical Decision Tools, diagnostic yield
Although pulmonary CT angiography (CTA) is increasingly used to evaluate patients believed to suffer from pulmonary embolism (PE), the diagnostic yield remains low.