According to UT Southwestern Medical Center researchers, a real-time radiation monitor that alerts staff by beeping in response to radiation exposure during cardiac-catheterisation procedures markedly reduces the amount of exposure that medical workers receive. Results of the RadiCure study are published in the journal Circulation: Cardiovascular Interventions.
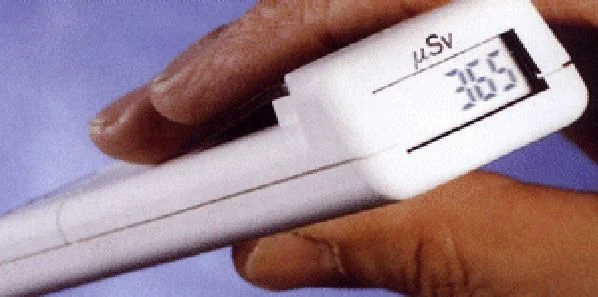
The device, Bleeper Sv, which is worn by medical workers, will beep approximately once every 15 minutes in response to low background radiation. It beeps more frequently — once every 20 seconds — when exposure is higher, or continuously if it is very high. The device is simple, robust and the display is positioned so that it is easy to read when the unit is in a breast pocket.
“Radiation is invisible,” said senior author Dr. Emmanouil Brilakis, Associate Professor of Internal Medicine at UT Southwestern Medical Center (Dallas, TX, USA). “Use of a radiation detection device can provide real-time ‘visualisation’ of radiation exposure, enabling operators to take actions to reduce radiation exposure.”
In this randomised study, Dr. Brilakis and colleagues divided 505 patients undergoing either diagnostic coronary angiography or percutaneous coronary intervention (such as stent placement) into two groups. In half the procedures, medical workers used the current gold standard for radiation monitoring, which is a “dosimetry” badge that is worn by a medical worker for a month and then sent off for the cumulative radiation dose to be read. In the other half, medical personnel wore the Bleeper Sv to monitor their exposure to radiation.
In settings where the medical workers wore the device that gives the real-time auditory feedback, radiation exposure was consistently decreased by approximately one-third, the research team reported.
“Using devices that provide real-time radiation-exposure feedback can help the operator adopt safer radiation practices,” explained Dr. Brilakis, who is also Director of the Cardiac Catheterization Laboratories at the VA North Texas Health Care System. “In our study, this was achieved in a real-life setting among unselected patients using a low-cost device that can be used with any x-ray system.”
Some actions that medical staff can take to reduce radiation exposure are:
Physicians and other medical workers on cardiac-catheterisation teams will likely participate in hundreds of procedures a year. The dose limit for occupational exposure is 20 mSv per year for five years, Dr. Brilakis' team noted. However, no dose is safe and all doses are considered to contribute to cancer risk.
“It has been shown that people who are chronically exposed to radiation in cardiac catheterisation labs are more likely to develop left-sided brain tumours,” Dr. Brilakis added. “The reduction in operator exposure observed in our study is likely to translate into a decreased risk for long-term adverse clinical events.”
Other UT Southwestern researchers involved in the RadiCure study are Dr. Anna Kotsia, Postdoctoral Researcher; Bavana V. Rangan, Research Scientist; Michele Roesle, RN; Dr. Atif Mohammad, Senior Research Associate; and Dr. Subhash Banerjee, Associate Professor of Internal Medicine.
This study is supported by the Department of Veterans Affairs and the Dallas VA Research Corp.
Source: Newswise
Image Credit: Vertec Scientific Ltd
The device, Bleeper Sv, which is worn by medical workers, will beep approximately once every 15 minutes in response to low background radiation. It beeps more frequently — once every 20 seconds — when exposure is higher, or continuously if it is very high. The device is simple, robust and the display is positioned so that it is easy to read when the unit is in a breast pocket.
“Radiation is invisible,” said senior author Dr. Emmanouil Brilakis, Associate Professor of Internal Medicine at UT Southwestern Medical Center (Dallas, TX, USA). “Use of a radiation detection device can provide real-time ‘visualisation’ of radiation exposure, enabling operators to take actions to reduce radiation exposure.”
In this randomised study, Dr. Brilakis and colleagues divided 505 patients undergoing either diagnostic coronary angiography or percutaneous coronary intervention (such as stent placement) into two groups. In half the procedures, medical workers used the current gold standard for radiation monitoring, which is a “dosimetry” badge that is worn by a medical worker for a month and then sent off for the cumulative radiation dose to be read. In the other half, medical personnel wore the Bleeper Sv to monitor their exposure to radiation.
In settings where the medical workers wore the device that gives the real-time auditory feedback, radiation exposure was consistently decreased by approximately one-third, the research team reported.
“Using devices that provide real-time radiation-exposure feedback can help the operator adopt safer radiation practices,” explained Dr. Brilakis, who is also Director of the Cardiac Catheterization Laboratories at the VA North Texas Health Care System. “In our study, this was achieved in a real-life setting among unselected patients using a low-cost device that can be used with any x-ray system.”
Some actions that medical staff can take to reduce radiation exposure are:
- Reducing the frame rate (the number of x-ray images taken per second to create a “movie” of the coronary arteries);
- Decreasing fluoroscopy time;
- Repositioning the patient;
- Repositioning the medical worker;
- Adjusting the position of the radiation shield; and
- Using additional shielding.
Physicians and other medical workers on cardiac-catheterisation teams will likely participate in hundreds of procedures a year. The dose limit for occupational exposure is 20 mSv per year for five years, Dr. Brilakis' team noted. However, no dose is safe and all doses are considered to contribute to cancer risk.
“It has been shown that people who are chronically exposed to radiation in cardiac catheterisation labs are more likely to develop left-sided brain tumours,” Dr. Brilakis added. “The reduction in operator exposure observed in our study is likely to translate into a decreased risk for long-term adverse clinical events.”
Other UT Southwestern researchers involved in the RadiCure study are Dr. Anna Kotsia, Postdoctoral Researcher; Bavana V. Rangan, Research Scientist; Michele Roesle, RN; Dr. Atif Mohammad, Senior Research Associate; and Dr. Subhash Banerjee, Associate Professor of Internal Medicine.
This study is supported by the Department of Veterans Affairs and the Dallas VA Research Corp.
Source: Newswise
Image Credit: Vertec Scientific Ltd
Latest Articles
X-ray, Cardiac, radiation dose, brain tumours, cathetherisation
According to UT Southwestern Medical Center researchers, a real-time radiation monitor that alerts staff by beeping in response to radiation exposure durin...