About 1.6 million people die of lung cancer each year, making it the leading cause of cancer-related deaths in the world. The poor outcomes of treatment in lung cancer resulting from the fact that most cases are diagnosed in the advanced stage of the disease justify the implementation of an optimal lung cancer prevention in the form of smoking cessation and screening programmes that would offer a chance to detect early stages of the disease, while fitting within specific economic constraints, according to a review article in the journal Advances in Medical Sciences.
Due to late diagnosis of lung cancer and, in some cases, the high aggressiveness of the tumour, overall 5-year survival rates are low – 12% among men and 7% among women. The article explains:
"Five-year survival rates decrease with increasing disease stage. In stages I, II, III and IV, the rates are 60–80%, 20–30%, 16% and less than 10%, respectively. Surgery is the most effective treatment with curative intent. The cure is most likely in early-stage disease."
However, as the article notes, the proportion of patients treated for stage I disease does not exceed 50% in the majority of thoracic surgical centres worldwide.
The paper highlights the importance of implementing lung cancer screening and smoking cessation programmes in high-risk group in order to reduce the mortality rate. The National Lung Screening Trial (NLST) – the largest and most expensive randomised, clinical trial in the United States demonstrated a 20% mortality rate reduction in patients who had undergone chest low-dose computed tomography (LDCT) screening, as compared to patients screened with a conventional chest x-ray. This finding supported the position of those who were pushing for the implementation of LDCT screening into everyday clinical practice.
Results of the NLST enabled the implementation of lung cancer screening programme among high-risk patients in the U.S. and parts of China. In 2017, recommendations of the European Society of Thoracic Surgeons also strongly recommend an implementation of a screening programme in the EU.
Lung cancer screening programmes are useful in the promotion of smoking cessation, as shown by the Dutch-Belgian NELSON study and other trials. Cessation rate in the NELSON study reached 16% versus 6% in the general population.
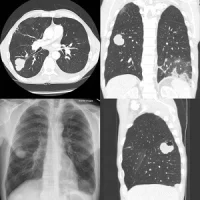
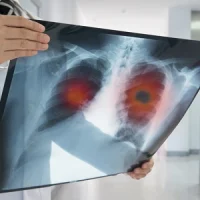
Although lung cancer screening does reduce lung cancer-related mortality, it has a low impact on the detection of malignant tumours itself. This is because, the article says, many small nodules of less than 2 mm in diameter are detected on LDCT and "it is very difficult to determine whether they are malignant or benign." This leads to many false positive results, which decreases the specificity and positive predictive value (PPV) on the one hand and expose the patients to unnecessary and expensive diagnostic procedures on the other.
"The diagnostic accuracy of screening may be potentially increased by improving the selection criteria and/or adding other early detection tools, such as radiomics or molecular testing," the article points out. Trials looking into these possibilities are well underway in the United States, UK, Poland and Italy. The goal is to better select patients at a significantly higher risk of lung cancer and, in patients with detected nodules on LDCT, to differentiate benign from malignant tumours detected on CT. These studies also aim to increase cost-effectiveness of the screening.
In addition, detection of markers in body fluids seems "very promising" but requires further studies, the article says.
Source: Advances in Medical Sciences
Image Credit: Pixabay
Lung cancer screening programmes are useful in the promotion of smoking cessation, as shown by the Dutch-Belgian NELSON study and other trials. Cessation rate in the NELSON study reached 16% versus 6% in the general population.
Although lung cancer screening does reduce lung cancer-related mortality, it has a low impact on the detection of malignant tumours itself. This is because, the article says, many small nodules of less than 2 mm in diameter are detected on LDCT and "it is very difficult to determine whether they are malignant or benign." This leads to many false positive results, which decreases the specificity and positive predictive value (PPV) on the one hand and expose the patients to unnecessary and expensive diagnostic procedures on the other.
"The diagnostic accuracy of screening may be potentially increased by improving the selection criteria and/or adding other early detection tools, such as radiomics or molecular testing," the article points out. Trials looking into these possibilities are well underway in the United States, UK, Poland and Italy. The goal is to better select patients at a significantly higher risk of lung cancer and, in patients with detected nodules on LDCT, to differentiate benign from malignant tumours detected on CT. These studies also aim to increase cost-effectiveness of the screening.
In addition, detection of markers in body fluids seems "very promising" but requires further studies, the article says.
Source: Advances in Medical Sciences
Image Credit: Pixabay
References:
Ostrowski M, Marjański T, Rzyman W (2018) Low-dose computed tomography screening reduces lung cancer mortality. Advances in Medical Sciences 63 (2018) 230–236 https://doi.org/10.1016/j.advms.2017.12.002
Latest Articles
lung cancer, CT screening, smoking cessation, lung cancer prevention
Poor outcomes of treatment in lung cancer resulting from the fact that most cases are diagnosed in the advanced stage of the disease justify the implementation of an optimal lung cancer prevention in the form of smoking cessation and screening programmes