Diagnosis of chronic obstructive pulmonary disease could be improved by the use of parametric response mapping (PRM), report investigators from the University of Michigan (U-M). In a study published in Nature Medicine, they report on the use of PRM to study computed tomography (CT) scans of the lungs of patients with COPD, who took part in a COPDGene study funded by the US National Heart, Lung and Blood Institute.
The study found that the PRM technique for evaluating CT scans could differentiate better between early-stage damage to the small airways of the lungs and more severe damage known as emphysema. The results also demonstrated that the overall severity of a patient’s disease measured with PRM correlates closely with the patient’s performance on existing tests based on breathing ability.
“Essentially, with the PRM technique, we’ve been able to tell subtypes of COPD apart, distinguishing functional small airway disease, or fSAD, from emphysema and normal lung function,” said Brian Ross, PhD, a research professor of radiology, professor of biological chemistry and senior author of the paper. “We believe this offers a new path to more precise diagnosis and treatment planning, and a useful tool for precisely assessing the impact of new medications and other treatments.”
Originally developed to show the response of brain tumours to treatment, the PRM technique allows researchers to identify COPD specific changes in three-dimensional (3D) lung regions over time. A U-M spinoff company, Imbio, has licensed U-M’s patents on the PRM technique, and is developing the technology for use in early prediction of treatment response of brain tumors and other cancers. Imbio has now begun developing PRM for COPD subtype diagnosis and tracking.
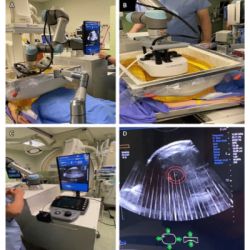
With the PRM technique, the researchers use computer techniques to overlay the CT scan taken during a full inhalation with an image captured during a full exhalation. The overlaid (registered) CT images share the same geometric space; therefore, the lung tissue in the inflated and deflated lungs aligns. Healthy lung tissue’s density will change more between the two images than the density of diseased lung, allowing researchers to create a 3D “map” of the patient’s lungs.
PRM assign colours to each small 3D area, called a voxel, according to the difference in signal changes within each of the areas between the two scans. Green means healthy, yellow means a reduced ability to push air out of the small sacs, and red means severely reduced ability.
“PRM can also help to track COPD progression or response to treatment over time,” remarked lead author Dr. Craig Gabán, assistant professor of radiology. Although the current study typically looked at a “snapshot” of CT scans taken a one time, it also includes data on two U-M COPD patients who were imaged over more than two years. More longitudinal data are needed to determine that PRM works well for long-term monitoring and studies are ongoing.
Whereas a simple breathing test called spirometry is still considered the best way to diagnose the disease, spirometry is limited in its ability to differentiate between diverse types of lung injury that COPD patients experience.
Source: University of Michigan Health System